Abstract
The extent and rate of bioavailability are fundamental measures to characterize the pharmacokinetics of drugs after oral administration. Together with bioavailability (F), the mean absorption time (MAT) can be used to define the rate of bioavailability, i.e., the rate of drug absorption. Previous results suggest that F may depend on MAT. Estimates of F and MAT were obtained from the input function (sum of two inverse Gaussian functions) used to model the oral absorption process. The estimation was performed by population analysis (nonlinear mixed-effects modeling) based on data from bioavailability studies in healthy volunteers. For trospium and ketamine, F decreased significantly with increasing MAT, while for propiverine, a significant increase was observed. Thus, the interindividual variability in F could be largely attributed to the interindividual variability in MAT. For trospium and propiverine, the relative dispersion (normalized variance) of the absorption time distribution increased significantly with MAT. For trospium and propiverine, the plot of F versus MAT provides information about the effect of gastrointestinal transit on drug absorption. In contrast, an increase in hepatic extraction with increasing MAT is responsible for the dependence of F on MAT. The F versus MAT plot is suggested as a simple diagnostic tool in evaluating the results of bioavailability studies.
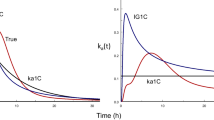
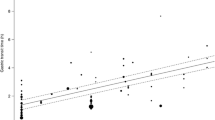
Graphical Abstract





Similar content being viewed by others
References
Cutler DJ. Theory of the mean absorption time, an adjunct to conventional bioavailability studies. J Pharm Pharmacol. 1978;30(8):476–8. https://doi.org/10.1111/j.2042-7158.1978.tb13296.x.
Weiss M. The relevance of residence time theory to pharmacokinetics. Eur J Clin Pharmacol. 1992;43(6):571–9. https://doi.org/10.1007/BF02284953.
Weiss M. Generalizations in linear pharmacokinetics using properties of certain classes of residence time distributions. II. Log-concave concentration-time curves following oral administration. J Pharmacokinet Biopharm. 1987;15(1):57–74. https://doi.org/10.1007/BF01062939.
May K, Giessmann T, Wegner D, Oertel R, Modess C, Oswald S, et al. Oral absorption of propiverine solution and of the immediate and extended release dosage forms: influence of regioselective intestinal elimination. Eur J Clin Pharmacol. 2008;64(11):1085–92. https://doi.org/10.1007/s00228-008-0528-0.
Weiss M, Sermsappasuk P, Siegmund W. Modeling the heterogeneous intestinal absorption of propiverine extended-release. Eur J Pharm Sci. 2015;76:133–7. https://doi.org/10.1016/j.ejps.2015.05.010.
Abebe BT, Weiss M, Modess C, Roustom T, Tadken T, Wegner D, et al. Effects of the P-glycoprotein inhibitor clarithromycin on the pharmacokinetics of intravenous and oral trospium chloride: a 4-way crossover drug-drug interaction study in healthy subjects. J Clin Pharmacol. 2019. https://doi.org/10.1002/jcph.1421.
Abebe BT, Weiss M, Modess C, Tadken T, Wegner D, Meyer MJ, et al. Pharmacokinetic drug-drug interactions between trospium chloride and ranitidine substrates of organic cation transporters in healthy human subjects. J Clin Pharmacol. 2020;60(3):312–23. https://doi.org/10.1002/jcph.1523.
Tadken T, Weiss M, Modess C, Wegner D, Roustom T, Neumeister C, et al. Trospium chloride is absorbed from two intestinal “absorption windows” with different permeability in healthy subjects. Int J Pharm. 2016;515(1–2):367-73 S0378-5173(16)30973-5. https://doi.org/10.1016/j.ijpharm.2016.10.030.
Weiss M, Siegmund W. Pharmacokinetic modeling of ketamine enantiomers and their metabolites after administration of prolonged-release ketamine with emphasis on 2,6-hydroxynorketamines. Clin Pharmacol Drug Dev. 2022;11(2):194–206. https://doi.org/10.1002/cpdd.993.
Dahan A, Miller JM, Amidon GL. Prediction of solubility and permeability class membership: provisional BCS classification of the world’s top oral drugs. AAPS J. 2009;11(4):740–6. https://doi.org/10.1208/s12248-009-9144-x.
Weiss M, D’Argenio DZ, Siegmund W. Analysis of complex absorption after multiple dosing: application to the interaction between the P-glycoprotein substrate talinolol and rifampicin. Pharm Res. 2022;39(12):3293–300. https://doi.org/10.1007/s11095-022-03397-6.
Oswald S, Terhaag B, Siegmund W. In vivo probes of drug transport: commonly used probe drugs to assess function of intestinal P-glycoprotein (ABCB1) in humans. Handb Exp Pharmacol. 2011;201:403–47. https://doi.org/10.1007/978-3-642-14541-4_11.
Csajka C, Drover D, Verotta D. The use of a sum of inverse Gaussian functions to describe the absorption profile of drugs exhibiting complex absorption. Pharm Res. 2005;22(8):1227–35. https://doi.org/10.1007/s11095-005-5266-8.
Weiss M. A novel extravascular input function for the assessment of drug absorption in bioavailability studies. Pharm Res. 1996;13(10):1547–53.
Weiss M. Empirical models for fitting of oral concentration time curves with and without an intravenous reference. J Pharmacokinet Pharmacodyn. 2017;44(3):193–201. https://doi.org/10.1007/s10928-017-9507-3;10.1007/s10928-017-9507-3.
Riegelman S, Collier P. The application of statistical moment theory to the evaluation of in vivo dissolution time and absorption time. J Pharmacokinet Biopharm. 1980;8(5):509–34. https://doi.org/10.1007/BF01059549.
D’Argenio D, Schumitzky A, Wang X. User’s guide: pharmacokinetic/pharmacodynamic systems analysis software. Los Angeles, CA: Biomedical Simulations Resource; 2009.
Weiss M. Relationship between dissolution rate in vitro and absorption rate in vivo of ketamine prolonged-release tablets. Eur J Drug Metab Pharmacokinet. 2023. https://doi.org/10.1007/s13318-022-00812-6.
Bergstrand M, Soderlind E, Weitschies W, Karlsson MO. Mechanistic modeling of a magnetic marker monitoring study linking gastrointestinal tablet transit, in vivo drug release, and pharmacokinetics. Clin Pharmacol Ther. 2009;86(1):77–83. https://doi.org/10.1038/clpt.2009.43.
Cora LA, Romeiro FG, Americo MF, Oliveira RB, Baffa O, Stelzer M, et al. Gastrointestinal transit and disintegration of enteric coated magnetic tablets assessed by ac biosusceptometry. Eur J Pharm Sci. 2006;27(1):1–8. https://doi.org/10.1016/j.ejps.2005.08.009.
Kolbow J, Modess C, Wegner D, Oswald S, Maritz MA, Rey H, et al. Extended-release but not immediate-release and subcutaneous methylnaltrexone antagonizes the loperamide-induced delay of whole-gut transit time in healthy subjects. J Clin Pharmacol. 2015. https://doi.org/10.1002/jcph.624.
Abuhelwa AY, Foster DJR, Upton RN. A quantitative review and meta-models of the variability and factors affecting oral drug absorption-part I: gastrointestinal pH. AAPS J. 2016;18(5):1309–21. https://doi.org/10.1208/s12248-016-9952-8.
Keller F, Kunzendorf U, Walz G, Haller H, Offermann G. Saturable first-pass kinetics of propranolol. J Clin Pharmacol. 1989;29(3):240–5. https://doi.org/10.1002/j.1552-4604.1989.tb03320.x.
Mistry B, Leslie JL, Eddington ND. Influence of input rate on the stereospecific and nonstereospecific first pass metabolism and pharmacokinetics of metoprolol extended release formulations. Chirality. 2002;14(4):297–304. https://doi.org/10.1002/chir.10045.
Wagner JG. Propranolol: pooled Michaelis-Menten parameters and the effect of input rate on bioavailability. Clin Pharmacol Ther. 1985;37(5):481–7. https://doi.org/10.1038/clpt.1985.76.
Author information
Authors and Affiliations
Contributions
M. W. analyzed the data. M. W. and W. S. wrote the manuscript.
Ethics declarations
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Weiss, M., Siegmund, W. Dependence of Bioavailability on Mean Absorption Time: What Does It Tell Us?. AAPS J 25, 36 (2023). https://doi.org/10.1208/s12248-023-00803-8
Received:
Accepted:
Published:
DOI: https://doi.org/10.1208/s12248-023-00803-8