Abstract
Objectives
Given the increasing prevalence of osteoporosis and the important role dynamic balanced plays in the assessment of muscle function, we aimed to examine the joint and separate effects of osteoporosis and poor dynamic balance on the incidence of sarcopenia in Chinese elderly individuals.
Design
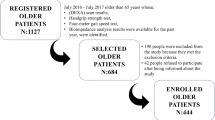
This study was conducted on 658 (44.4% male) Chinese suburban-dwelling participants with a mean age of 68.42 ± 5.43 years who initially had no sarcopenia and were aged >60 years. A quantitative ultrasound scan of each participant’s calcaneus with a T score less than −2.5 was used to identify the prevalence of osteoporosis. Sarcopenia was diagnosed according to the Asian Working Group for Sarcopenia criteria. We assessed dynamic balance using the Timed Up and Go Test (TUGT). Participants who scored in the top 20% on the TUGT were defined as having poor dynamic balance.
Results
After a follow-up of three years, the incidence of sarcopenia in the general population was 8.1% (9.6% in males, 6.8% in females). The incidence of sarcopenia was progressively greater in people suffering from both osteoporosis and poor dynamic balance (OR=2.416, 95%CI=1.124–5.195) compared to those who only had osteoporosis (OR=0.797, 95%CI=0.378–1.682) or poor dynamic balance (OR=1.226, 95%CI=0.447–3.363) in models without adjustments. Even after adjusting for potential confounders, the result still held true (OR=2.431, 95%CI=1.053–5.614).
Conclusions
In our study, we found individuals who suffered from both osteoporosis and poor dynamic balance simultaneously had a significantly higher incidence of sarcopenia than those who suffered from either one or the other.

Similar content being viewed by others
References
China. State Statistical B. Communique of the major statistics from the first national population census as released by the State Statistical Bureau of the People’s Republic of China (November 1, 1954). Chin Sociol Anthropol. 1984; 16:62–5.
Lauretani F, Bautmans I, De Vita F, Nardelli A, Ceda GP, Maggio M. Identification and treatment of older persons with sarcopenia. Aging Male. 2014; 17:199–204.
Evans WJ, Campbell WW. Sarcopenia and age-related changes in body composition and functional capacity. J Nutr. 1993; 123:465–8.
Cawthon PM, Marshall LM, Michael Y, Dam TT, Ensrud KE, Barrett-Connor E, et al. Frailty in older men: prevalence, progression, and relationship with mortality. J Am Geriatr Soc. 2007; 55:1216–23.
Goodpaster BH, Park SW, Harris TB, Kritchevsky SB, Nevitt M, Schwartz AV, et al. The loss of skeletal muscle strength, mass, and quality in older adults: the health, aging and body composition study. J Gerontol A Biol Sci Med Sci. 2006; 61:1059–64.
Riis BJ, Hansen MA, Jensen AM, Overgaard K, Christiansen C. Low bone mass and fast rate of bone loss at menopause: equal risk factors for future fracture: a 15-year follow-up study. Bone. 1996; 19:9–12.
Chen P, Li Z, Hu Y. Prevalence of osteoporosis in China: a meta-analysis and systematic review. BMC Public Health. 2016; 16:1039.
Sjoblom S, Suuronen J, Rikkonen T, Honkanen R, Kroger H, Sirola J. Relationship between postmenopausal osteoporosis and the components of clinical sarcopenia. Maturitas. 2013; 75:175–80.
Yoshimura N, Muraki S, Oka H, Iidaka T, Kodama R, Kawaguchi H, et al. Is osteoporosis a predictor for future sarcopenia or vice versa? Four-year observations between the second and third ROAD study surveys. Osteoporos Int. 2017; 28:189–99.
da Silva AP, Matos A, Ribeiro R, Gil A, Valente A, Bicho M, et al. Sarcopenia and osteoporosis in Portuguese centenarians. Eur J Clin Nutr. 2017; 71:56–63.
He H, Liu Y, Tian Q, Papasian CJ, Hu T, Deng HW. Relationship of sarcopenia and body composition with osteoporosis. Osteoporos Int. 2016; 27:473–82.
Tarantino U, Baldi J, Scimeca M, Piccirilli E, Piccioli A, Bonanno E, et al. The role of sarcopenia with and without fracture. Injury. 2016; 47 Suppl 4:S3–S10.
Cruz-Jentoft AJ, Baeyens JP, Bauer JM, Boirie Y, Cederholm T, Landi F, et al. Sarcopenia: European consensus on definition and diagnosis: Report of the European Working Group on Sarcopenia in Older People. Age Ageing. 2010; 39:412–23.
Kang L, Han P, Wang J, Ma Y, Jia L, Fu L, et al. Timed Up and Go Test can predict recurrent falls: a longitudinal study of the community-dwelling elderly in China. Clin Interv Aging. 2017; 12:2009–16.
Chen LK, Liu LK, Woo J, Assantachai P, Auyeung TW, Bahyah KS, et al. Sarcopenia in Asia: consensus report of the Asian Working Group for Sarcopenia. J Am Med Dir Assoc. 2014; 15:95–101.
Sim M, Prince RL, Scott D, Daly RM, Duque G, Inderjeeth CA, et al. Sarcopenia Definitions and Their Associations With Mortality in Older Australian Women. J Am Med Dir Assoc. 2019; 20:76–82 e2.
Zhang W, Shen S, Wang W, Zhou C, Xu L, Qiu J, et al. Poor lower extremity function was associated with pre-diabetes and diabetes in older chinese people. PLoS One. 2014; 9:e115883.
Ma Y, Fu L, Jia L, Han P, Kang L, Yu H, et al. Muscle strength rather than muscle mass is associated with osteoporosis in older Chinese adults. J Formos Med Assoc. 2018; 117:101–8.
Kanis JA. Assessment of fracture risk and its application to screening for postmenopausal osteoporosis: synopsis of a WHO report. WHO Study Group. Osteoporos Int. 1994; 4:368–81.
Han P, Kang L, Guo Q, Wang J, Zhang W, Shen S, et al. Prevalence and Factors Associated With Sarcopenia in Suburb-dwelling Older Chinese Using the Asian Working Group for Sarcopenia Definition. J Gerontol A Biol Sci Med Sci. 2016; 71:529–35.
Hwang HY, Choi JS, Kim HE. Masticatory efficiency contributing to the improved dynamic postural balance: A cross-sectional study. Gerodontology. 2018.
Cruz-Jentoft AJ, Landi F, Schneider SM, Zuniga C, Arai H, Boirie Y, et al. Prevalence of and interventions for sarcopenia in ageing adults: a systematic review. Report of the International Sarcopenia Initiative (EWGSOP and IWGS). Age Ageing. 2014; 43:748–59.
Lin CC, Lin WY, Meng NH, Li CI, Liu CS, Lin CH, et al. Sarcopenia prevalence and associated factors in an elderly Taiwanese metropolitan population. J Am Geriatr Soc. 2013; 61:459–62.
Aibar-Almazan A, Martinez-Amat A, Cruz-Diaz D, Jimenez-Garcia JD, Achalandabaso A, Sanchez-Montesinos I, et al. Sarcopenia and sarcopenic obesity in Spanish community-dwelling middle-aged and older women: Association with balance confidence, fear of falling and fall risk. Maturitas. 2018; 107:26–32.
Frisoli A, Jr., Chaves PH, Ingham SJ, Fried LP. Severe osteopenia and osteoporosis, sarcopenia, and frailty status in community-dwelling older women: results from the Women’s Health and Aging Study (WHAS) II. Bone. 2011; 48:952–7.
Doherty TJ. Invited review: Aging and sarcopenia. J Appl Physiol (1985). 2003; 95:1717–27.
Walsh MC, Hunter GR, Livingstone MB. Sarcopenia in premenopausal and postmenopausal women with osteopenia, osteoporosis and normal bone mineral density. Osteoporos Int. 2006; 17:61–7.
Gillette-Guyonnet S, Nourhashemi F, Lauque S, Grandjean H, Vellas B. Body composition and osteoporosis in elderly women. Gerontology. 2000; 46:189–93.
Demontiero O, Boersma D, Suriyaarachchi P, Duque G. Clinical Outcomes of Impaired Muscle and Bone Interactions. Clinical Reviews in Bone and Mineral Metabolism. 2014; 12:86–92.
Salarian A, Zampieri C, Horak FB, Carlson-Kuhta P, Nutt JG, Aminian K. Analyzing 180 degrees turns using an inertial system reveals early signs of progression of Parkinson’s disease. Conf Proc IEEE Eng Med Biol Soc. 2009; 2009:224–7.
Bonnyaud C, Pradon D, Bensmail D, Roche N. Dynamic Stability and Risk of Tripping during the Timed Up and Go Test in Hemiparetic and Healthy Subjects. PLoS One. 2015; 10:e0140317.
Sim M, Prince RL, Scott D, Daly RM, Duque G, Inderjeeth CA, et al. Utility of four sarcopenia criteria for the prediction of falls-related hospitalization in older Australian women. Osteoporos Int. 2019; 30:167–76.
Waters DL, Qualls CR, Cesari M, Rolland Y, Vlietstra L, Vellas B. Relationship of Incident Falls with Balance Deficits and Body Composition in Male and Female Community-Dwelling Elders. J Nutr Health Aging. 2019; 23:9–13.
Szulc P, Beck TJ, Marchand F, Delmas PD. Low skeletal muscle mass is associated with poor structural parameters of bone and impaired balance in elderly men—the MINOS study. J Bone Miner Res. 2005; 20:721–9.
Guerrero N, Bunout D, Hirsch S, Barrera G, Leiva L, Henriquez S, et al. Premature loss of muscle mass and function in type 2 diabetes. Diabetes Res Clin Pract. 2016; 117:32–8.
Han P, Zhao J, Guo Q, Wang J, Zhang W, Shen S, et al. Incidence, Risk Factors, and the Protective Effect of High Body Mass Index against Sarcopenia in Suburb-Dwelling Elderly Chinese Populations. J Nutr Health Aging. 2016; 20:1056–60.
Cheung AS, Gray H, Schache AG, Hoermann R, Lim Joon D, Zajac JD, et al. Androgen deprivation causes selective deficits in the biomechanical leg muscle function of men during walking: a prospective case-control study. J Cachexia Sarcopenia Muscle. 2017; 8:102–12.
Acknowledgements
The authors thank Guiyan Shao from the Chadian public health center and Xiaofang Ren from Hangu welfare house for providing place and organization.
Funding
Funding: This work was supported by grant from National Natural Science Foundation of China (81601952) and Tianjin Municipal Science and Technology Commission (16ZXMJSY00070, Tianjin, China), and Health and Family Planning Commission of Binhai New Area (2017BWKZ005).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics approval and consent to participate: This research was approved by the Ethics Committee at Tianjin Medical University. The methodological sessions were carried out in accordance with the approved guidelines and regulations. The participants were fully informed of the nature of research and signed an informed consent to participate.
Competing interests: The authors declare that they have no competing interests in this section.
Rights and permissions
About this article
Cite this article
Yu, X., Hou, L., Guo, J. et al. Combined Effect of Osteoporosis and Poor Dynamic Balance on the Incidence of Sarcopenia in Elderly Chinese Community Suburban-Dwelling Individuals. J Nutr Health Aging 24, 71–77 (2020). https://doi.org/10.1007/s12603-019-1295-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12603-019-1295-6