Abstract
Objectives
This study aimed to investigate the regulatory roles of lncRNA MALAT1, miR-124-3p, and IGF2BP1 in osteogenic differentiation of periodontal ligament stem cells (PDLSCs).
Materials and methods
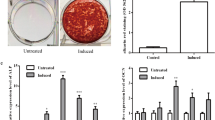
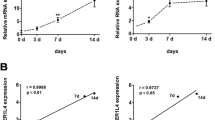
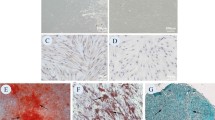
We characterized PDLSCs by employing quantitative real-time polymerase chain reaction (qRT-PCR) and Western blot analyses to evaluate the expression of key osteogenic markers including ALPL, SPP1, and RUNX2. Manipulation of lncRNA MALAT1 and miR-124-3p expression levels was achieved through transfection techniques. In addition, early osteogenic differentiation was assessed via Alkaline phosphatase (ALP) staining, and mineral deposition was quantified using Alizarin Red S (ARS) staining. Cellular localization of lncRNA MALAT1 was determined through Fluorescence In Situ Hybridization (FISH). To elucidate the intricate regulatory network, we conducted dual-luciferase reporter assays to decipher the binding interactions between lncRNA MALAT1 and miR-124-3P as well as between miR-124-3P and IGF2BP1.
Results
Overexpression of lncRNA MALAT1 robustly promoted osteogenesis in PDLSCs, while its knockdown significantly inhibited the process. We confirmed the direct interaction between miR-124-3p and lncRNA MALAT1, underscoring its role in impeding osteogenic differentiation. Notably, IGF2BP1 was identified as a direct binding partner of lncRNA MALAT1, highlighting its pivotal role within this intricate network. Moreover, we determined the optimal IGF2BP1 concentration (50 ng/ml) as a potent enhancer of osteogenesis, effectively countering the inhibition induced by si-MALAT1. Furthermore, in vivo experiments utilizing rat calvarial defects provided compelling evidence, solidifying lncRNA MALAT1’s crucial role in bone formation.
Conclusions
Our study reveals the regulatory network involving lncRNA MALAT1, miR-124-3p, and IGF2BP1 in PDLSCs’ osteogenic differentiation.
Clinical relevance
These findings enhance our understanding of lncRNA-mediated osteogenesis, offering potential therapeutic implications for periodontal tissue regeneration and the treatment of bone defects.








Similar content being viewed by others
Data availability
No datasets were generated or analysed during the current study.
References
Monsarrat P, Vergnes JN, Nabet C, Sixou M, Snead ML, Planat-Bénard V, Casteilla L, Kémoun P (2014) Concise review: mesenchymal stromal cells used for periodontal regeneration: a systematic review. Stem Cells Transl Med 3:768–774. https://doi.org/10.5966/sctm.2013-0183
Qi L, Zhang Y (2014) The microRNA 132 regulates fluid shear stress-induced differentiation in periodontal ligament cells through mTOR signaling pathway. Cell Physiol Biochem 33:433–445. https://doi.org/10.1159/000358624
Ha SH, Choung PH (2020) MSM promotes human periodontal ligament stem cells differentiation to osteoblast and bone regeneration. Biochem Biophys Res Commun 528:160–167. https://doi.org/10.1016/j.bbrc.2020.05.097
Kinane DF, Stathopoulou PG, Papapanou PN (2017) Periodontal diseases. Nat Rev Dis Prim 3:17038. https://doi.org/10.1038/nrdp.2017.38
Menicanin D, Mrozik KM, Wada N, Marino V, Shi S, Bartold PM, Gronthos S (2014) Periodontal-ligament-derived stem cells exhibit the capacity for long-term survival, self-renewal, and regeneration of multiple tissue types in vivo. Stem Cells Dev 23:1001–1011. https://doi.org/10.1089/scd.2013.0490
Yu B, Hu J, Li Q, Wang F (2021) CircMAP3K11 contributes to proliferation, apoptosis and migration of human periodontal ligament stem cells in inflammatory microenvironment by regulating TLR4 via miR-511 sponging. Front Pharmacol 12:633353. https://doi.org/10.3389/fphar.2021.633353
Li X, Zhang B, Wang H, Zhao X, Zhang Z, Ding G, Wei F (2020) The effect of aging on the biological and immunological characteristics of periodontal ligament stem cells. Stem Cell Res Ther 11:326. https://doi.org/10.1186/s13287-020-01846-w
Zhou Y, Fan W, Xiao Y (2014) The effect of hypoxia on the stemness and differentiation capacity of PDLC and DPC. Biomed Res Int 2014:890675. https://doi.org/10.1155/2014/890675
ENCODE Project Consortium (2012) An integrated encyclopedia of DNA elements in the human genome. Nature 489:57–74. https://doi.org/10.1038/nature11247
Chen LL (2016) Linking long noncoding RNA localization and function. Trends Biochem Sci 41:761–772. https://doi.org/10.1016/j.tibs.2016.07.003
Lin C, Yang L (2018) Long noncoding RNA in cancer: wiring signaling circuitry. Trends Cell Biol 28:287–301. https://doi.org/10.1016/j.tcb.2017.11.008
Quinn JJ, Chang HY (2016) Unique features of long non-coding RNA biogenesis and function. Nat Rev Genet 17:47–62. https://doi.org/10.1038/nrg.2015.10
Struhl K (2007) Transcriptional noise and the fidelity of initiation by RNA polymerase II. Nat Struct Mol Biol 14:103–105. https://doi.org/10.1038/nsmb0207-103
Fatica A, Bozzoni I (2014) Long non-coding RNAs: new players in cell differentiation and development. Nat Rev Genet 15:7–21. https://doi.org/10.1038/nrg3606
Hung T, Wang Y, Lin MF, Koegel AK, Kotake Y, Grant GD, Horlings HM, Shah N, Umbricht C, Wang P, Wang Y, Kong B, Langerød A, Børresen-Dale AL, Kim SK, van de Vijver M, Sukumar S, Whitfield ML, Kellis M, Xiong Y, Wong DJ, Chang HY (2011) Extensive and coordinated transcription of noncoding RNAs within cell-cycle promoters. Nat Genet 43:621–629. https://doi.org/10.1038/ng.848
Yang Y, Yujiao W, Fang W, Linhui Y, Ziqi G, Zhichen W, Zirui W, Shengwang W (2020) The roles of miRNA, lncRNA and circRNA in the development of osteoporosis. Biol Res 53:40. https://doi.org/10.1186/s40659-020-00309-z
Bellavia D, Salamanna F, Raimondi L, De Luca A, Carina V, Costa V, Alessandro R, Fini M, Giavaresi G (2019) Deregulated miRNAs in osteoporosis: effects in bone metastasis. Cell Mol Life Sci 76:3723–3744. https://doi.org/10.1007/s00018-019-03162-w
Pu M, Chen J, Tao Z, Miao L, Qi X, Wang Y, Ren J (2019) Regulatory network of miRNA on its target: coordination between transcriptional and post-transcriptional regulation of gene expression. Cell Mol Life Sci 76:441–451. https://doi.org/10.1007/s00018-018-2940-7
Zheng Y, Li X, Huang Y, Jia L, Li W (2018) Time series clustering of mRNA and lncRNA expression during osteogenic differentiation of periodontal ligament stem cells. PeerJ 6:e5214. https://doi.org/10.7717/peerj.5214
Chen J, Wang Y, Wang C, Hu JF, Li W (2020) LncRNA functions as a new emerging epigenetic factor in determining the fate of stem cells. Front Genet 11:277. https://doi.org/10.3389/fgene.2020.00277
Tello-Flores VA, Beltrán-Anaya FO, Ramírez-Vargas MA, Esteban-Casales BE, Navarro-Tito N, Alarcón-Romero LDC, Luciano-Villa CA, Ramírez M, Del Moral-Hernández Ó, Flores-Alfaro E (2021) Role of long non-coding RNAs and the molecular mechanisms involved in insulin resistance. Int J Mol Sci 22. https://doi.org/10.3390/ijms22147256
Yan C, Chen J, Chen N (2016) Long noncoding RNA MALAT1 promotes hepatic steatosis and insulin resistance by increasing nuclear SREBP-1c protein stability. Sci Rep 6:22640. https://doi.org/10.1038/srep22640
Vimalraj S, Subramanian R, Dhanasekaran A (2021) LncRNA MALAT1 promotes tumor angiogenesis by regulating microRNA-150-5p/VEGFA signaling in osteosarcoma: in-vitro and in-vivo analyses. Front Oncol 11:742789. https://doi.org/10.3389/fonc.2021.742789
Lu Y, Gong Z, Jin X, Zhao P, Zhang Y, Wang Z (2020) LncRNA MALAT1 targeting miR-124-3p regulates DAPK1 expression contributes to cell apoptosis in Parkinson’s Disease. J Cell Biochem 121:4838–4848. https://doi.org/10.1002/jcb.29711
Li X (2022) LncRNA metastasis-associated lung adenocarcinoma transcript-1 promotes osteogenic differentiation of bone marrow stem cells and inhibits osteoclastic differentiation of Mø in osteoporosis via the miR-124-3p/IGF2BP1/Wnt/β-catenin axis. J Tissue Eng Regen Med 16:311–329. https://doi.org/10.1002/term.3279
Younes N, Syed N, Yadav SK, Haris M, Abdallah AM, Abu-Madi M (2021) A whole-genome sequencing association study of low bone mineral density identifies new susceptibility loci in the Phase I Qatar Biobank Cohort. J Pers Med 11. https://doi.org/10.3390/jpm11010034
Song C, Guo Y, Chen F, Liu W (2022) lncRNA MALAT1 promotes osteogenic differentiation through the miR-217/AKT3 axis: a possible strategy to alleviate osteoporosis. J Gene Med 24:e3409. https://doi.org/10.1002/jgm.3409
Zhou Y, Xu Z, Wang Y, Song Q, Yin R (2022) LncRNA MALAT1 mediates osteogenic differentiation in osteoporosis by regulating the miR-485-5p/WNT7B axis. Front Endocrinol (Lausanne) 13:922560. https://doi.org/10.3389/fendo.2022.922560
Li J, Zhuang H, Wang Z, Cai J, Ma X, Chen W, Jiang X, Zhao D, Hou W, Tao Y (2022) lncRNAs MALAT1 and LINC00657 upstream to miR-214-3p/BMP2 regulate osteogenic differentiation of human mesenchymal stem cells. Mol Biol Rep 49:6847–6857. https://doi.org/10.1007/s11033-022-07136-3
Xiao X, Zhou T, Guo S, Guo C, Zhang Q, Dong N, Wang Y (2017) LncRNA MALAT1 sponges miR-204 to promote osteoblast differentiation of human aortic valve interstitial cells through up-regulating Smad4. Int J Cardiol 243:404–412. https://doi.org/10.1016/j.ijcard.2017.05.037
Bao M, Liu G, Song J, Gao Y (2020) Long non-coding RNA MALAT1 promotes odontogenic differentiation of human dental pulp stem cells by impairing microRNA-140-5p-dependent downregulation of GIT2. Cell Tissue Res 382:487–498. https://doi.org/10.1007/s00441-020-03246-1
Hua L, Zhang X (2021) MALAT1 regulates osteogenic differentiation of human periodontal ligament stem cells through mediating miR-155-5p/ETS1 axis. Tissue Cell 73:101619. https://doi.org/10.1016/j.tice.2021.101619
Zhang L, Sheng M, Cao H, Zhang L, Shao W (2023) Decoding the role of long non-coding RNAs in periodontitis: a comprehensive review. Biomed Pharmacother 166:115357. https://doi.org/10.1016/j.biopha.2023.115357
Xia F, Xu Y, Zhang X, Lyu J, Zhao P (2021) Competing endogenous RNA network associated with oxygen-induced retinopathy: expression of the network and identification of the MALAT1/miR-124-3p/EGR1 regulatory axis. Exp Cell Res 408:112783. https://doi.org/10.1016/j.yexcr.2021.112783
Gan L, Leng Y, Min J, Luo XM, Wang F, Zhao J (2022) Kaempferol promotes the osteogenesis in rBMSCs via mediation of SOX2/miR-124-3p/PI3K/Akt/mTOR axis. Eur J Pharmacol 927:174954. https://doi.org/10.1016/j.ejphar.2022.174954
Qadir AS, Um S, Lee H, Baek K, Seo BM, Lee G, Kim GS, Woo KM, Ryoo HM, Baek JH (2015) miR-124 negatively regulates osteogenic differentiation and in vivo bone formation of mesenchymal stem cells. J Cell Biochem 116:730–742. https://doi.org/10.1002/jcb.25026
Cao Y, Lv Q, Li Y (2021) Astragaloside IV improves tibial defect in rats and promotes proliferation and osteogenic differentiation of hBMSCs through MiR-124-3p.1/STAT3 Axis. J Nat Prod 84:287–297. https://doi.org/10.1021/acs.jnatprod.0c00975
Scalia P, Williams SJ, Fujita-Yamaguchi Y (2023) Human IGF2 gene epigenetic and transcriptional regulation: at the core of developmental growth and tumorigenic behavior. Biomedicines 11. https://doi.org/10.3390/biomedicines11061655
Wang P, Zhang L, Zhang J, Xu G (2022) MicroRNA-124-3p inhibits cell growth and metastasis in cervical cancer by targeting IGF2BP1. Exp Ther Med 23:233. https://doi.org/10.3892/etm.2022.11157
Chen W, Chen M, Xu Y, Chen X, Zhou P, Zhao X, Pang F, Liang W (2018) Long non-coding RNA THOR promotes human osteosarcoma cell growth in vitro and in vivo. Biochem Biophys Res Commun 499:913–919. https://doi.org/10.1016/j.bbrc.2018.04.019
Qu Y, Pan S, Kang M, Dong R, Zhao J (2016) MicroRNA-150 functions as a tumor suppressor in osteosarcoma by targeting IGF2BP1. Tumour Biol 37:5275–5284. https://doi.org/10.1007/s13277-015-4389-8
Kang H, Sung J, Jung HM, Woo KM, Hong SD, Roh S (2012) Insulin-like growth factor 2 promotes osteogenic cell differentiation in the parthenogenetic murine embryonic stem cells. Tissue Eng A 18:331–341. https://doi.org/10.1089/ten.TEA.2011.0074
Hardouin SN, Guo R, Romeo PH, Nagy A, Aubin JE (2011) Impaired mesenchymal stem cell differentiation and osteoclastogenesis in mice deficient for Igf2-P2 transcripts. Development 138:203–213. https://doi.org/10.1242/dev.054916
Yakar S, Werner H, Rosen CJ (2018) Insulin-like growth factors: actions on the skeleton. J Mol Endocrinol 61:T115–T137. https://doi.org/10.1530/jme-17-0298
Diao S, Yang H, Cao Y, Yang D, Fan Z (2020) IGF2 enhanced the osteo-/dentinogenic and neurogenic differentiation potentials of stem cells from apical papilla. J Oral Rehabil 47(Suppl 1):55–65. https://doi.org/10.1111/joor.12859
Zheng Y, Li X, Huang Y, Jia L, Li W (2017) The circular RNA landscape of periodontal ligament stem cells during osteogenesis. J Periodontol 88:906–914. https://doi.org/10.1902/jop.2017.170078
Livak KJ, Schmittgen TD (2001) Analysis of relative gene expression data using real-time quantitative PCR and the 2(-Delta Delta C(T)) method. Methods 25:402–408. https://doi.org/10.1006/meth.2001.1262
Wang Y, Li J, Tang M, Peng C, Wang G, Wang J, Wang X, Chang X, Guo J, Gui S (2023) Smart stimuli-responsive hydrogels for drug delivery in periodontitis treatment. Biomed Pharmacother 162:114688. https://doi.org/10.1016/j.biopha.2023.114688
Sedghi LM, Bacino M, Kapila YL (2021) Periodontal disease: the good, the bad, and the unknown. Front Cell Infect Microbiol 11:766944. https://doi.org/10.3389/fcimb.2021.766944
Chen Q, Liu X, Wang D, Zheng J, Chen L, Xie Q, Liu X, Niu S, Qu G, Lan J, Li J, Yang C, Zou D (2021) Periodontal inflammation-triggered by periodontal ligament stem cell pyroptosis exacerbates periodontitis. Front Cell Dev Biol 9:663037. https://doi.org/10.3389/fcell.2021.663037
Chen L, Zhu S, Guo S, Tian W (2023) Mechanisms and clinical application potential of mesenchymal stem cells-derived extracellular vesicles in periodontal regeneration. Stem Cell Res Ther 14:26. https://doi.org/10.1186/s13287-023-03242-6
Jiang Z, Hua Y (2016) Hydrogen sulfide promotes osteogenic differentiation of human periodontal ligament cells via p38-MAPK signaling pathway under proper tension stimulation. Arch Oral Biol 72:8–13. https://doi.org/10.1016/j.archoralbio.2016.08.008
Singh A, Gill G, Kaur H, Amhmed M, Jakhu H (2018) Role of osteopontin in bone remodeling and orthodontic tooth movement: a review. Prog Orthod 19:18. https://doi.org/10.1186/s40510-018-0216-2
Komori T (2018) Runx2, an inducer of osteoblast and chondrocyte differentiation. Histochem Cell Biol 149:313–323. https://doi.org/10.1007/s00418-018-1640-6
Liu JL, Liu YS, Zheng MJ, He HY (2022) The management of bone defect using long non-coding RNA as a potential biomarker for regulating the osteogenic differentiation process. Mol Biol Rep 49:2443–2453. https://doi.org/10.1007/s11033-021-07013-5
Musolino C, Oteri G, Allegra A, Mania M, D’Ascola A, Avenoso A, Innao V, Allegra AG, Campo S (2018) Altered microRNA expression profile in the peripheral lymphoid compartment of multiple myeloma patients with bisphosphonate-induced osteonecrosis of the jaw. Ann Hematol 97:1259–1269. https://doi.org/10.1007/s00277-018-3296-7
Funding
This study was financially supported by grants from the National Natural Science Foundation of China, Changchun, China (No.82370934).
Author information
Authors and Affiliations
Contributions
Nan Gu: Conducted Experiments and Data Analysis.
Yao Wang: Conducted Literature Review and Manuscript Writing.
Lingfeng Li: Picture Production.
Xin Sui:Formal Analysis.
Zhihui Liu: Oversaw Project Design and Supervision.
Corresponding author
Ethics declarations
Ethics approval
The experiment was conducted under the supervision of the Institutional Animal care and Use Committee of Jilin University. The number of permit was SY202104016.
Consent to participate
Not applicable.
Conflict of interest
The authors declare that there is no conflict of interest.
Competing interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Highlights
1. MALAT1 Enhances Osteogenesis: lncRNA MALAT1 positively regulates osteogenic differentiation in PDLSCs, highlighting its role in bone regeneration.
2. Unveiling the Regulatory Axis: miR-124-3p targets IGF2BP1 to modulate osteogenic potential, unveiling a novel regulatory axis in periodontal tissue repair.
3. Therapeutic Insights for Bone Defects: Insights into lncRNA-mediated osteogenesis provide potential avenues for innovative therapies in periodontal regeneration and bone defect management.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Gu, N., Wang, Y., Li, L. et al. The mechanism of lncRNA MALAT1 targeting the miR-124-3p/IGF2BP1 axis to regulate osteogenic differentiation of periodontal ligament stem cells. Clin Oral Invest 28, 219 (2024). https://doi.org/10.1007/s00784-024-05616-3
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00784-024-05616-3