Abstract
Background
Muscle function and its correlation with body composition and weight loss have not been studied deeply in pancreas and gastrointestinal cancers. This research aims to determine the skeletal muscle function and its relationship with body compartments, significant weight loss, and performance status (ECOG) 0-2 in a population with advanced digestive cancers.
Methods
A cross-sectional study was designed to determine the relationship between muscular function, weight loss, and body composition. Patients with advanced digestive adenocarcinomas were evaluated. Muscle strength was examined by hand grip technique and body composition by bioimpedance analysis. Values of hemoglobin and albumin were measured in plasma.
Results
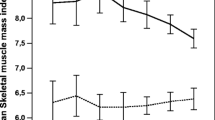
A sample of 81 patients was included. They had adenocarcinoma of stomach (n = 9), pancreas (n = 28), or colorectum (n = 44). With regard to skeletal muscle function, sub-maximal strength increased when percentage of weight loss decreased (p = 0.002) or when any of the following variables increased: skeletal muscle (p < 0.001), waist-hip ratio (p < 0.001), body surface area (p < 0.001), and body mass index (p = 0.001). According to multivariate analysis of these variables, only percentage of weight loss and skeletal muscle remained statistically significant. Endurance had no correlation with any of the variables. Higher weight loss was found in tumors of the upper tract (stomach and pancreas) in comparison with those of the lower tract (colorectal) (p = 0.005).
Conclusions
In advanced digestive cancer, sub-maximal strength correlated inversely with weight loss and directly with skeletal muscle such as in lung and head and neck cancers. On the other hand, endurance had no correlation with any of the variables considered.

Similar content being viewed by others
References
Siegel RL, Miller KD, Jemal A (2016) Cancer statistics. CA Cancer J Clin 66:7–30
Libutti SK, Saltz LB, Wollet C, Levine RA (2015) Cancer of the colon. In: De Vita H, Rosenberg (eds) Cancer: principles & practice of oncology, vol 57, 10th edn. Wolters Kluwer, pp 768–812
Zheng P, Zhou Z (2015) Human cancer immunotherapy with PD-1/PD-L1 blockade. Biomark Cancer 7:15–18
Matrisian L, Berlin J (2016) The past, present and future of pancreatic cancer clinical trials. Am Soc Clin Oncol Educ Book:e205-e215
Dry GK, Adjei A (2013) Understanding, recognizing, and managing toxicities of target anticancer therapies. CA Cancer J Clin 63:249–279
Verger E, Salamero M, Comil C (1992) Can Karnofsky perfomance status be transformed to the Eastern Cooperative Oncology Group scoring scale and vice versa? Eur J Cancer 28A:1328–1330
Kilgour RD, Vigano A, Trutschingg B, Lucar E et al (2013) Handgrip strength predicts survival and is associated with markers of clinical and functional outcomes in advanced cancer patients. Support Care Cancer 21:3261–3270
Donohoe CL, Ryan AM, Reynolds JV (2011) Cancer cachexia: mechanisms and clinical implications. Gastroenterol Res Pract 2011:601434. https://doi.org/10.1155/2011/601434
Dewys WD, Begg C, Lavin PT, Band PR, Bennett JM, Bertino JR, Cohen MH, Douglass HO Jr, Engstrom PF, Ezdinli EZ, Horton J, Johnson GJ, Moertel CG, Oken MM, Perlia C, Rosenbaum C, Silverstein MN, Skeel RT, Sponzo RW, Tormey DC (1980) Prognostic effect of weight loss prior to chemotherapy in cancer patients. Eastern Cooperative Oncology Group. Am J Med 69:491–497
Dy S, Lorenz K, Naeim A, Homayoon S et al (2008) Evidence-based recommendations for cancer fatigue, depression and dyspnea. J Clin Oncol 26:3886–3895
Cerchietti L, Navigante A, Peluffo G, Diament M et al (2004) Effects of celecoxib, medroxyprogesterone, and dietary intervention on systemic syndromes in patients with advanced lung adenocarcinoma. J Pain Symptom Manag 27:85–95
Hauser K, Rybicki L, Walsh D (2010) What’s in a name? Word descriptors of cancer-related fatigue. Palliat Med 24(7):724–730
Richardson A (1995) Fatigue in cancer patients: a review of the literature. Eur J Cancer Care 4:20–32
Luthy C, Cedraschi C, Pugliesi A, Di Silvestro K et al (2011) Patients ‘views about causes and preferences for the management of cancer-related fatigue-a case for non congruent with physicians? Support Care Cancer 19:363–370
Navigante A, Cresta Morgado P, Casbarien O, López Delgado N et al (2013) Relationship between weakness and phase angle in advanced cancer patients with fatigue. Support Care Cancer 21:1685–1690
Bautmans I, Gorus E, Njemini R, Mets T (2007) Handgrip performance in relation to self-perceived fatigue, physical functioning and circulating IL-6 in elderly persons without inflammation. BMC Geriatr 7:5
Cresta Morgado P, Giorlando A, Castro M, Navigante A (2016) Relationship between weight loss and parameters of skeletal muscle function in patients with advanced cancer and fatigue. Support Care Cancer 24:3961–3966. https://doi.org/10.1007/s00520-016-3236-9
Lenk K, Schuler G, Adams V (2010) Skeletal muscle wasting in cachexia and sarcopenia: molecular pathophysiology and impact of exercise training. J Cachexia Sarcopenia Muscle 1:9–21. https://doi.org/10.1007/s13539-010-0007-1
Nedergaard A, Karsdal M, Sun S, Henriksen K (2013) Serological muscle loss biomarkers: an overview of current concepts and future possibilities. J Cachexia Sarcopenia Muscle 4:1–17. https://doi.org/10.1007/s13539-012-0086-2
Ebner N, von Haeling S (2017) Highlights from the 9th cachexia conference. J Cachexia Sarcopenia Muscle 8:508–511. https://doi.org/10.1002/jcsm.12217
Clark B, Manini T (2012) What is dynapenia? Nutrition 28:495–503
Lucia A, Ramírez M (2016) Muscling in cancer. N Engl J Med 375(9):892–894
Lieffers JR, Bathe OF, Fassbender K, Winget M, Baracos VE (2012) Sarcopenia is associated with postoperative infection and delayed recovery from colorectal cancer resection surgery. BJC 107:931–936
Lieffers JR, Moutzakis M, Hall K, Mc Cargar L et al (2009) A viscerally driven cachexia syndrome in patients with advanced colorectal cancer: contributions of organ and tumor mass to whole-body energy demands. Am J Clin Nutr 89:1173–1179
Parsons H, Baracos V, Dhillon N, Hong D, Kurzrock R (2012) Body composition, symptoms, and survival in advanced cancer patients referred to a phase I service. PLoS One 7(1):e29330: 1–7. https://doi.org/10.1371/journal.pone.0029330
Bachmann J, Heiligensetzer M, Krakowski-Roosen H, Buchler M et al (2008) Cachexia worsen prognosis in patients with resectable pancreatic cancer. J Gastrointest Surg 12:1193–1201
Fogelman DR, Morris J, Xiao L, Hassan M, Vadhan S, Overman M, Javle S, Shroff R, Varadhachary G, Wolff R, Vence L, Maitra A, Cleeland C, Wang XS (2017) A predictive model of inflammatory markers and patient-reported symptoms for cachexia in newly diagnosed pancreatic cancer patients. Support Care Cancer 25(6):1809–1817
Fisher D, Tish KM, Durivage H, Beaulieu N (2003) The cancer chemotherapy handbook. Mosby 11:486–497
Blanchard E, Hesketh P (2015) Nausea and vomiting. In: De Vita H, Rosenberg’s (eds) Cancer: principles & practice of oncology, vol 135, 10th edn. Lippincott Williams & Wilkins, pp 1976–1983
Tilignac T, Temparis S, Combaret L, Taillandier D, Pouch MN, Cervek M, Cardenas DM, le Bricon T, Debiton E, Samuels SE, Madelmont JC, Attaix D (2002) Chemotherapy inhibits skeletal muscle ubiquitin-proteasome-dependent proteolysis. Cancer Res 62:2771–2777
Prado C (2013) Body composition in chemotherapy: the promising role of CT scans. Curr Opin Clin Nutr Metab Care 16:525–533. https://doi.org/10.1097/MCO.0b013e328363bcfb
Acknowledgments
The authors thank the National Cancer Institute of Argentina for making this study possible. We also thank Vera Wassermann for her valuable help.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
The study protocol was approved by the Ethics Committee of the Bonorino Udaondo Gastroenerology Hospital of the city of Buenos Aires and met the recommendations stated in Helsinki Declaration. All the patients signed informed consent.
Conflict of interest
The authors declare that they have conflict of interest.
Rights and permissions
About this article
Cite this article
Cresta Morgado, P., Daud, M., Carballido, M. et al. Relationship between skeletal muscle function, body composition, and weight loss in patients with advanced pancreatic and gastrointestinal cancers. Support Care Cancer 27, 1181–1186 (2019). https://doi.org/10.1007/s00520-018-4421-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-018-4421-9