Abstract
Background
The occurrence of incisional hernias after various types of abdominal procedures and incisions continues to be a problem. A number of studies conducted for diverse risk groups have identified a beneficial role for the prophylactic use of mesh augmentation. To what extent this affects the stability of a suture was tested in our biomechanical model.
Materials and methods
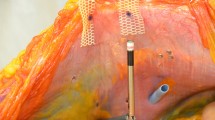
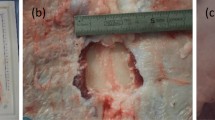
To that effect, we compared three groups, carrying out six measurements in each case: (1) single suture in a muscle specimen, (2) suture and additional reinforcement with fibrin glue, and (3) suture and additional reinforcement with a mesh fixed with fibrin glue (Tissucol, Tisseel; with an overlap of 2 cm to all sides).
Results
The single suture conferred a tensile strength, which in our model, was just above the prescribed maximum abdominal pressure of 32 N (37.3 N). The additional use of fibrin glue did not have any significant impact on this result (41.8 N). Only through mesh augmentation with fibrin glue was it possible to achieve a significantly greater tensile strength (64.5 N, p = 0.003).
Conclusions
The prophylactic use of meshes for stabilization of laparotomy closures appears to be effective. Adequate mesh fixation can be achieved with fibrin glue alone. Further experimental studies and in particular randomized clinical trials are needed to demonstrate proof of the long-term advantages of mesh augmentation in risk groups.


Similar content being viewed by others
References
Burger JW, van’t Riet M, Jeekel J (2002) Abdominal incisions: techniques and postoperative complications. Scand J Surg 91:315–321
Ellis H, Gajraj H, George CD (1983) Incisional hernias: when do they occur? Br J Surg 70:290–291
Höer J, Lawong G, Klinge U, Schumpelick V (2002) Influencing factors on the causes of incisional hernia. Chirurg 73:474–480
Mudge M, Hughes LE (1985) Incisional hernia: a 10 year prospective study of incidence and attitudes. Br J Surg 72:70–71
O’Dwyer PJ, Courtney CA (2003) Factors involved in abdominal wall closure and subsequent incisional hernia. Surgeon 1:17–22
Van’t Riet M, Steyerberg EW, Nellensteyn J, Bonjer HJ, Jeekel J (2002) Meta-analysis of techniques for closure of midline abdominal incisions. Br J Surg 89:1350–1356
Bucknall TE, Cox PJ, Ellis H (1982) Burst abdomen and incisional hernia: a prospective study of 1129 major laparotomies. Br Med J (Clin Res Ed) 284:931–933
Gislason H, Viste A (1999) Closure of burst abdomen after major gastrointestinal operations—comparison of different surgical techniques and later development of incisional hernia. Eur J Surg 165:958–961
Liapis CD, Dimitroulis DA, Kakisis JD, Nikolaou AN, Skandalakis P, Dakalopoulos M, Kostakis AG (2004) Incidence of incisional hernias in patients operated on for aneurysm or occlusive disease. Am Surg 70:550–552
Strzelczyk J, Czupryniak L, Loba J, Wasiak J (2002) The use of polypropylene mesh in midline incision closure following gastric-bypass surgery reduces the risk of postoperative hernia. Langenbecks Arch Surg 387:294–297
Sugerman HJ, Kellum JM, Reines HD, DeMaria EJ, Newsome HH, Lowry JW (1996) Greater risk of incisional hernia with morbidly obese than steroid-dependent patients and low recurrence with prefascial polypropylene mesh. Am J Surg 171:80–84
Van’t R, de vos van Steenwijk PJ, Bonjer HJ, Steyerberg EW, Jeekel J (2004) Incisional hernia after repair of wound dehiscence: incidence and risk factors. Am Surg 70:281–286
Grindflek E, Moc M, Taubert H, Simianer H, Lien S, Moen T (2006) Genome-wide linkage of inguinal hernia in pigs using affected sib pairs. BMC Genet 7:25–37
Jansen PL, Mertens P, Klinge U, Schumpelick V (2004) The biology of hernia formation. Surgery 136:1–4
Franz MG (2006) The biology of hernias and the abdominal wall. Hernia 10:462–471
Klinge U (2006) Are collagens the culprits in the development of incisional and inguinal hernia disease? Hernia 10:472–477
Capella RF, Iannace VA, Capella JF (2007) Reducing the incidence of incisional hernias following open gastric bypass surgery. Obes Surg 17:438–444
Fassiadis N, Roidl M, Hennig M, South LM, Andrews SM (2005) Randomized clinical trial of vertical or transverse laparotomy for abdominal aortic aneurysm repair. Br J Surg 92:1208–1211
Nout E, Lange JF, Salu NE, Wijsmuller AR, Hop WCJ, Goossens RHM, Snijdrs CJ, Jeekel J, Kleinrensink GJ (2007) Creep behaviour of commonly used suture materials in abdominal wall surgery. J Surg Res 138:51–55
Knaebel HP, Koch M, Sauerland S, Diener MK, Büchler MW, Seiler CM, INSECT Study Group of the Study Centre of the German Surgical Society (2005) Interrupted or continuous slowly absorbable sutures—design of a multi-centre randomised trial to evaluate abdominal closure techniques INSECT-trial. BMC Surg 5:3
Knaebel HP, Kirschner M, Reidel M, Büchler M, Seiler C (2006) Operative standardization of randomized controlled studies in surgery. Chirurg 77:267–272
Burger JW, Luijendijk RW, Hop WC, Halm JA, Verdaasdonk EG, Jeekel J (2004) Long-term follow-up of randomized controlled trial of suture versus mesh repair of incisional hernia. Ann Surg 240:578–583
Flum DR, Horvath K, Koepsell T (2003) Have outcomes of incisional hernia repair improved with time? A population-based analysis. Ann Surg 237:129–135
O’Hare JL, Ward J, Earnshaw JJ (2007) Late results of mesh wound closure after elective open aortic aneurysm repair. Eur J Vasc Endovasc Surg 33:412–413
Rogers M, McCarthy R, Earnshaw JJ (2003) Prevention of incisional hernia after aortic aneurysm repair. Eur J Vasc Endovasc Surg 26:519–522
Strzelczyk JM, Szymanski D, Nowicki ME, Wilczynski W, Gaszynski T, Czupryniak L (2006) Randomized clinical trial of postoperative hernia prophylaxis in open bariatric surgery. Br J Surg 93:1347–1350
Gutierrez de la Pena C, Medina Achirica C, Dominguez-Adame E, Medina Diez J (2003) Primary closure of laparotomies with high risk of incisional hernia using prosthetic material: analysis of usefulness. Hernia 7:134–136
Israelsson LA (2005) Preventing and treating parastomal hernia. World J Surg 29:1086–1089
Berger D (2007) Prevention of parastomal hernias by prophylactic use of a specially designed intraperitoneal onlay mesh. Hernia 12:243–246 online first
Gögenur I, Mortensen J, Harvald T, Rosenberg J, Fischer A (2006) Prevention of parastomal hernia by placement of a polypropylene mesh at primary operation. Dis Colon Rectum 49:1131–1135
Jänes A, Cengiz Y, Israelsson LA (2004) Randomized clinical trial of the use of a prosthetic mesh to prevent parastomal hernia. Br J Surg 91:280–282
Marimuthu K, Vijayasekar C, Ghosh D, Mathew G (2006) Prevention of parastomal hernia using preperitoneal mesh: a prospective observational study. Colorectal Dis 8:672–675
Geisler DJ, Reilly JC, Vaughan SG, Glennon EJ, Kondylis PD (2003) Safety and outcome of use of nonabsorbable mesh for repair of fascial defect in the presence of open bowel. Dis Colon Rectum 46:1118–1123
Bellon JM, Lopez-Hervas P, Rodriguez M, Garcia-Honduvilla N, Pascual G, Bujan J (2006) Midline abdominal wall closure: a new prophylactic mesh concept. J Am Coll Surg 203:490–497
Petter-Puchner AH, Fortelny R, Mittermayr R, Öhlinger W, Redl H (2005) Fibrin sealing versus stapling of hernia meshes in an onlay model in the rat. Hernia 9:322–329
Schwab R, Schumacher O, Junge K, Binnebösel M, Klinge U, Becker HP, Schumpelick V (2008) Biomechanical analysis of mesh fixation in TAPP and TEP hernia repair. Surg Endosc 22:731–738
ten Hallers EJ, Jansen JA, Marres HA, Rakhorst G, Verkerke GJ (2007) Histological assessment of titanium and polypropylene fiber mesh implantation with and without fibrin tissue glue. J Biomed Mater Res A 80:372–380
Klinge U, Conze J, Limberg W, Brücker C, Ottinger AP, Schumpelick V (1996) Pathophysiology of the abdominal wall. Chirurg 67:229–233
Klinge U, Klosterhalfen B, Birkenhauer V, Junge K, Conze J (2002) Schumpelick V. Impact of polymer pore size on the interface scar formation in a rat model. J Surg Res 103:208–214
Scheidbach H, Tamme C, Tannapfel A, Lippert H, Köckerling F (2004) In vivo studies comparing the biocompatibility of various polypropylene meshes and their handling properties during endoscopic total extraperitoneal (TEP) patchplasty: an experimental study in pigs. Surg Endosc 18:211–220
Acknowledgment
We thank Mr. Heinlein from GfE-Medizintechnik GmbH for technical support in conducting and analyzing the experiments.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Schug-Pass, C., Lippert, H. & Köckerling, F. Primary mesh augmentation with fibrin glue for abdominal wall closure—investigations on a biomechanical model. Langenbecks Arch Surg 395, 151–156 (2010). https://doi.org/10.1007/s00423-008-0453-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00423-008-0453-9