Abstract
Background
Prior research and experience has increased physician understanding of infant skull fracture prediction. However, patterns related to fracture length, nonlinearity, and features of complexity remain poorly understood, and differences across infant age groups have not been previously explored.
Methods
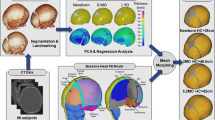
To determine how infant and low-height fall characteristics influence fracture patterns, we collected data from 231 head CT 3D reconstructions and quantified length and nonlinearity using a custom image processing code. Regression analysis was used to determine the effects of age and fall characteristics on nonlinearity, length, and features of fracture complexity.
Results
While impact surface had an important role in the number of cracks present in a fracture, younger infants and greater fall heights significantly affected most features of fracture complexity, including suture-to-suture spanning and biparietal involvement. In addition, increasing fracture length with increasing fall height supports trends identified by prior finite-element modeling. Finally, this study yielded results supporting the presence of soft tissue swelling as a function of fracture location rather than impact site.
Conclusions
Age-related properties of the infant skull confer unique fracture patterns following head impact. Further characterization of these properties, particularly in infants <4 months of age, will improve our understanding of the infant skull’s response to trauma.
Impact
-
Younger infant age and greater fall heights have significant effects on many features of fracture complexity resulting from low-height falls.
-
Incorporating multiple crack formation and multiple bone involvement into computational models of young infant skull fractures may result in increased biofidelity.
-
Drivers of skull fracture complexity are not well understood, and skull fracture patterns in real-world data across infant age groups have not been previously described.
-
Understanding fracture complexity relative to age in accidental falls will improve the understanding of accidental and abusive head trauma.
Similar content being viewed by others
Introduction
Skull fractures are relatively common in infancy, identified in up to 10% of infants presenting for minor head trauma.1,2,3 While isolated infant skull fractures often result from low-height falls, they have been associated with sentinel and occult injuries increasing concern for child maltreatment.4,5,6 Alternatively, when skull fractures are inadequately understood, an abundance of caution may lead to extensive evaluations and interventions by child welfare agencies.7 Head computed tomography (CT) and three-dimensional (3D) reconstruction has refined our detection and characterization of both linear and complex fractures. While fracture complexity once played a significant role in the assessment of infant skull fractures and a clinician’s level of concern for inflicted injury, research has shown that fracture complexity on its own should not guide abuse determinations.8,9,10,11
Several age-dependent skull characteristics influence fracture susceptibility. Trabecular fibers radiating outward from ossifying centers located at bony prominences in the infant skull result in an anisotropic bone, which has directionally-dependent material behavior.12,13 As the infant skull grows and strengthens, the trabecular fiber network incorporates into the bone, disappearing during childhood, altering the skull’s architecture and impact response. Varying skull thickness across skull bones,14 as well as the presence and geometry of sutures and fontanelles,12 further influences infant skull fractures.
Computational modeling offers some insight into age-dependent features that lead to skull fracture initiation,15,16,17,18 but very few studies predict fracture patterns, limiting our understanding of how fall parameters and infant characteristics contribute to infant skull fracture complexity. Recently, He et al.19 incorporated fracture mechanics theory into the Coats et al’s16 1.5-month-old FE model, successfully predicting the length and orientation of skull fractures in three infant cadavers between 2 and 5 months of age. Yan et al.20 used this adapted FE model framework to investigate the effect of impact angle and fall height on resulting skull fracture patterns. The authors found that the impact angle influenced the fracture initiation site and fracture orientation, while fall height increased final fracture length and nonlinearity. Although age-related differences have been previously noted, differences specifically within the infant age category have not been explored.
We sought to determine how infant and low-height fall characteristics influence fracture patterns in a large clinical dataset. We hypothesized that decreasing infant age would increase features of skull fracture complexity, increasing fall height would increase fracture length and nonlinearity, and impact surfaces with less energy absorption would increase fracture length, nonlinearity, and features of complexity. To our knowledge, this is the first study to investigate skull fracture patterns qualitatively and quantitatively in a large real-world dataset. These data will bolster biofidelity and accuracy of developing head trauma computational models and provide context and support for previously identified fall-related variables.
Methods
Retrospective chart review
Subjects were identified by Primary Children’s Hospital (PCH; Salt Lake City, UT) searches based on International Classification of Disease, Tenth Revision codes (S02.0, S02.1) of evaluations performed between 2014 and 2019. Patients were included if ≤12 months old at the time of their evaluation and had undergone a non-contrast head CT with 3D reconstruction revealing a skull fracture after a reported history of a household or caregiver-related fall. Patients with fractures only involving facial bones, resulting from window falls, or with underlying bone disease were excluded. Given poorly understood skull fracture healing patterns,21 we excluded cases with ≥10-day delay to imaging. Cases were compared to PCH Center for Safe & Healthy Families’ internal database for consultations with child abuse pediatrics (CAP).
We collected information regarding child physical abuse evaluations, including the treating physician’s assessment in the medical notes, whether the patient had undergone a skeletal survey, whether the patient’s reported fall had been witnessed, and the degree of relationship between the witness and the infant. A first-degree witness would be a single caregiver present to witness the fall; a second-degree witness would include a second caregiver who also reported witnessing the fall; a third-degree witness would include multiple witnesses or independent third parties who witnessed the event, such as if the fall had occurred in a public place. Falls only heard by a caregiver were counted as first-degree. CAP determinations resulted from multidisciplinary team review of the patient’s presenting history, physical and radiological findings, and at times, supplemental information from scene investigation by child welfare and law enforcement agencies. PCH standard trauma protocol recommends that all infants ≤6 months old presenting with traumatic injury undergo a skeletal survey since approximately 2016, resulting in some skeletal surveys that would have otherwise been routine to not have been performed. In addition, CAP may have been contacted over the telephone, which not always resulted in chart documentation during the initial years of the study’s timeframe. Nonetheless, if a case had any documented concern for inflicted injury, it was not included in our population. Charts were independently reviewed by the first author, T.M.R.-M. This study was reviewed and approved by the University of Utah Institutional Review Board and deemed exempt research.
Data collection for descriptive statistics
We collected patient demographics, fall characteristics, and head CT findings. Fall characteristics refer to fall height, fall mechanism, and impact surface. We sought to include typical household, community, and caregiver-related falls, which we anticipated would generally range between 0.3 and 2.0 m, consistent with prior low-height falls descriptions.22 We reviewed the reported estimated fall height and compared them with available standard measurements. In addition, several real-life measurements were taken and compared to the reported and standard height measurements. Standard height measurements appeared most consistent with the real-life measurements, and therefore, were used in all cases to estimate object heights. When applicable, patient sitting or standing heights were included in the fall height estimate using 50th percentile measurements on Center for Disease Control and Prevention growth charts minus 5 cm to approximate impact locations to the side of the head rather than vertex. Each author estimated fall height independently and the consensus between the three authors was used as the final fall height reference.
Fall mechanisms were defined by the initiation site of the fall, broadly including falls from a person’s arms, falls from a table or countertop, falls from a chair, falls from a bed, stair falls, postural falls during standing or sitting, and carrier-related falls. Impact surface was defined as the surface the infant’s head struck upon falling. We grouped surfaces based on their relative coefficient of restitution (COR)—a measure of a particular surface’s ability to absorb energy. Our surface COR group definitions were based on previously published literature,23,24 as well as in-house testing (Table 1).
Head CT findings refer to features of fracture complexity and include the number of fractures, the number of cracks that made up the fracture, the number of branches a crack developed, whether the crack appeared to cross a suture, and the skull bones involved with their laterality. We collected data regarding associated intracranial hemorrhage or injury (ICH/ICI) and the location of soft tissue swelling (STS) when present. Head CTs were performed according to PCH protocols, and reports were rendered by senior pediatric radiologists. Clarifications were sought through PCH pediatric radiologists and neuroradiologists when appropriate.
Image analysis
Upon head impact, a localized region of the infant skull experiences enough stress to damage the bone and initiate fracture. Single or multiple cracks may propagate from a single initiation site, or may propagate from different initiation sites on the same, or separate, skull bone. As cracks propagate, energy is released, driving the crack front, or the front of the crack, away from the crack initiation site. Cracks can initiate at the edge of a suture or can propagate towards and connect with a suture. A crack may appear to contact and cross a suture to an adjacent bone, which we defined as suture crossing (Fig. 1a), and may span a bone in between sutures, which we defined as suture-to-suture spanning (Fig. 1b). Crack branching may also occur, appearing as small fragments arising, or branching off, from a larger crack (Fig. 1c). In our study, we considered branches as any crack <15 mm stemming from a larger crack.
a “Suture crossing”—fracture crack appears to cross the left lambdoid suture into the occipital bone (thick black arrow). b “Suture-to-suture spanning”—fracture spans the left parietal bone, extending between the left coronal and left lambdoid suture (thin black arrows). c “Branching” illustrates small branch off main fracture (*).
We captured still images from head CT 3D reconstructions for image analysis. Images were deemed to be of good quality for analysis when the authors could clearly identify cracks with minimal background or movement artifacts. Most CTs were obtained on GE Healthcare RevolutionTM CT scanners. Toshiba AquilionTM, GE OptimaTM CT660, and GE LightSpeedTM scanners were also used. Scaled references were not included in most 3D reconstructions, and establishing retrospective measurements on the rendered study was not generally possible. To account for variations in CT scanner output while allowing for a measurement reference that was otherwise unavailable, a scale factor was established for GE and Toshiba-obtained 3D reconstructions by gathering measurements of universally present anatomical landmarks on two-dimensional CT slices with scaled references, such as the ear canal and nasal bridge, and comparing to measurements of the same structures on 3D reconstructions.
A custom image processing code was created (MATLAB 2022, The MathWorks, Natick, MA, 2022) to quantify fracture length and nonlinearity (Fig. 2). Length was calculated as the true distance of the crack path measured on the outer surface of the involved bone. Nonlinearity was calculated as the length of a crack divided by the straight-line distance between the crack endpoints, known as the Euclidean distance (Fig. 2b). Scores >1 indicate deviation from a straight-line configuration. The fracture length was the sum of the lengths for every crack and the fracture nonlinearity was the average of the nonlinearity for all the cracks.
Statistical analysis
A linear regression was performed to evaluate the significant effects of sex, age, fall height, and impact surface on nonlinearity, length, and the number of fractures, cracks, and branches. A logistic regression was performed to evaluate the same effects on suture crossing, suture-to-suture spanning, biparietal involvement, and the presence of ICH/ICI. Interaction effects for fall height and age, as well as fall height and impact surface, were included with the main effects for both regression models. The effect of race was not evaluated given the insufficient distribution in the sample population. Cases for which fall height estimates and image scale factors had not been possible to establish were excluded from these statistical analyses, including stair falls.
Age was treated as a continuous variable in the regression models but was also binned into three developmental groups (0–4, 4–8, and 8–12 months) to evaluate significant differences between the individual age groups using Tukey–Kramer comparison tests and Pearson’s χ2 tests. One-way ANOVA and χ2 tests were also used to evaluate the effect of fall mechanisms and witness degree on the dependent variables. Statistical significance for all analyses was defined as p value <0.05. Analysis was executed on JMP® Statistical Software (JMP® Version 16.1. SAS Institute Inc., Cary, NC, 1989–2021).
Results
Descriptive results
A total of 231 cases met the inclusion criteria. Our study population was predominantly white, with a male-to-female ratio of 1.5, consistent with previously published epidemiological skull fracture data,25 and a mean age of 5.5 months (Table 2). Results regarding fall characteristics, fall heights, and impact surfaces are detailed in Tables 3, 4, and 5, respectively. A total of 274 fractures were identified, the majority of which involved the parietal bone, as typically expected (Table 6). Most fractures involving multiple bones were found in the oldest age group, except for biparietal fractures, which were most common in the youngest. Statistical evaluation of multiple bone involvement excluded the biparietal fractures, which were evaluated separately. Most cases involved a single fracture, and most fractures had a single crack (Table 7). It is notable that approximately 27% of fractures had three or more cracks, mostly present in the younger age group. Branching, suture crossing, and biparietal involvement were relatively uncommon (6.9%, 7.3%, and 6.9%, respectively), while suture-to-suture spanning was more frequent, seen in just over one-fourth of cases. STS was overwhelmingly common, present in 97.8% of cases. Notably, STS was overlying all but two biparietal skull fractures (Table 8 and Fig. 3).
No prior concern for head injury. STS developed bilaterally shortly after fall, prompting imaging: a CT axial image revealing bilateral STS (thick white arrows) overlying biparietal fractures; b CT bone window revealing biparietal skull fractures (thin black arrows); c right parietal fracture on CT 3D reconstruction (thick black arrow); and d left parietal fracture on CT 3D reconstruction (thick black arrow).
Most ICH/ICI was focal and underlying, or small and scattered, with some contrecoup small hemorrhages not requiring neurosurgical intervention or extended clinical observation. In three cases, ICH was large and required operative drainage, all of which were epidural. Clinically, all 231 cases reported that the patient presented neurologically well, including those that required neurosurgical intervention. Patients were consistently reported by caregivers to have cried immediately or shortly after impact, without prolonged loss of consciousness, prolonged apnea, or seizures. Three cases reported brief (<60 s) alteration in mental status and unresponsiveness followed by return to baseline behavior with no further deterioration. Of note, these were not the cases that required neurosurgical intervention.
Most skeletal surveys (75%) were in children ≤6 months old. Only two skeletal surveys yielded additional injuries—each revealing an acute clavicular fracture deemed to be consistent with the reported fall by CAP. Both cases had presented to medical evaluation shortly after the reported fall, and both had a second-degree witness. Intraoral injury, scleral injury, and bruising was not reported in our population. Further details regarding CAP evaluation are outlined in Table 9. The treating provider specifically discussed how the constellation of findings yielded a low level of concern for abuse in all other cases not otherwise evaluated.
Statistical analysis results
A total of 218 cases were of sufficient quality for image analysis. Increasing fall height significantly increased the number of fractures (p = 0.020). The number of cracks was greater in falls involving younger infants (p = 0.011), greater fall heights (p = 0.034), and high COR surfaces (p = 0.015). In addition, the interaction between fall height and impact surface was significant (p = 0.034), as low COR surfaces had a greater number of cracks when paired with falls from greater heights. Similarly, multiple bone involvement was found to significantly increase at greater heights (p = 0.02) and with high COR surfaces (p = 0.03). Impact surface was not found to have a significant effect on either fracture nonlinearity or fracture length. Fracture length was found to decrease in older infant age groups (p = 0.004) and with lower fall heights (p = 0.043). No predictor variables were found to have any significant effect on nonlinearity.
Branching and suture crossing were rare, and neither fall height, impact surface, nor age was found to have a significant effect on their development. Of note, infant age showed a nearly significant effect (p = 0.066) with a greater number of branches per fracture in younger infant age groups. Suture-to-suture spanning was significantly associated to increasing fall height (p = 0.031) and younger infant age (p = 0.001). While biparietal involvement was not as commonly seen as suture-to-suture spanning, we did find it to be significantly associated with younger infants (p = 0.003). All biparietal fractures in our sample population were found in infants younger than 6 months old, and the majority (70.6%) were in the 0–4-month age group. Age was also found to significantly affect ICH/ICI, with ICH/ICI more frequently found in younger infants (p = 0.007). In addition, increasing fall height in younger infants significantly increased ICH/ICI (p = 0.005).
Among our predictor variables, infant age had a significant effect on many outcomes. Figure 4 relates to the prevalence of these outcomes, while Fig. 5 illustrates the trend of fracture nonlinearity and fracture length means by age groups. Note the lack of statistical significance in fracture nonlinearity despite a decreasing trend (p = 0.240). Height also had a significant effect on many outcomes such as fracture length, the number of fractures, the number of cracks, suture-to-suture spanning, and ICH/ICI. Our findings suggest that while impact surface has an important role in the development of cracks, infant age and height exert more significant effects on many features of fracture complexity. After binning age into three developmental groups, the effect of age on suture-to-suture spanning (p = 0.018) and biparietal fracture (p = 0.003) remained, but the age effect on the number of cracks and ICH/ICI disappeared, suggesting that the group definitions may not best represent the trends for those variables.
The diagonal line represents significant values from logistic regression models. The top bars represent significant differences in fracture length from one-way ANOVAs with post hoc Tukey–Kramer comparisons when age is binned (0–4, 4–8, and 8–12 months). No significant differences were found between age groups and nonlinearity. *p < 0.05; **p < 0.005; †p = 0.240.
When limiting our sample population to cases with only parietal bone involvement, we found a significant increase in nonlinearity with younger infants (p = 0.027) and the number of fractures was now significantly increased with younger ages (p = 0.023) rather than by increasing fall height. Many greater fall heights involved multiple bone fractures, so the reduction in the dataset to only parietal bone involvement eliminated many of the greater-height falls. Results for other variables were comparable to the larger dataset.
Finally, we looked at the effect of fall mechanism and witness degree on head CT fracture characteristics. Witness degree had no significant effect on any skull fracture feature or measurement. We found that the complexity of the fracture was generally greater when an infant fell from a person’s arms, which resulted in a significantly greater number of cracks (p = 0.005), branching (p = 0.024), suture-to-suture spanning (p = 0.004), biparietal involvement (p = 0.0283), and ICH/ICI (p = 0.010) compared to lower height mechanisms, such as chairs and beds. These findings support prior literature where the highest clinical burden resulted from fall mechanisms involving drops from adult caregivers’ arms and falls from the furniture.1 Stair falls in our study did not have any fracture features significantly different than other fall mechanisms. Fall mechanism did not significantly affect fracture nonlinearity and length.
Discussion
Our study revealed several key findings that enrich our current understanding of the infant skull’s response to common fall conditions. First, consistent with our hypothesis, infant age was found to have a strong influence on many fracture features, specifically, the number of crack fronts, suture-to-suture spanning, multiple bone involvement, and biparietal involvement, suggesting that skull fractures in younger infants develop more features of fracture complexity than older infants. This is not surprising given that cranial bone is thinner, weaker, and less stiff in younger infants.12,13,26
Increased complexity in younger infant ages compared to older children has been noted in the clinical literature. Ibrahim and Margulies27 reviewed 285 cases of falls from different heights in children ≤48 months old, and found that with heights <3 m, children ≤12 months old (infants) exhibited more skull fractures than children >12 months old (toddlers). Furthermore, they found that infants developed multiple skull fractures more frequently than toddlers across all heights. Multiple skull fractures in toddlers were only identified in falls >3 m. The authors focused on age-related differences between infants and toddlers, so head injuries within the infant age group were not compared. Our results suggest that differences not only exist across major pediatric developmental groups (i.e., infants and toddlers), but that significant differences exist within the infant age groups.
The vulnerability of the youngest age group (0–4-month-old) is particularly concerning because it corresponds with an age range of high rates of abuse. Research has shown that the incidence of abusive head trauma is highest in infants ≤12 months old, with a peak during early infancy in children ≤4 months old.28 The increased risk of abuse in this young age group understandably heightens clinicians’ concern when young infants present with a head injury. Specifically, multiple bone involvement and suture-to-suture spanning have been recently proposed as indicative of abuse.29,30,31 However, these studies’ conclusions do not consider the unique structural characteristics associated with young infant age. Our results highlight an overlap between a period of infant vulnerability to abusive injury and a structurally significant period where impact injury, accidental or inflicted, is more likely to result in increased features of fracture complexity when compared to older infants. Therefore, we discourage assigning high concern to isolated skull fractures based solely on features of fracture complexity at this time. Further research aimed at determining structural and material drivers of these age-related differences, and at examining specific features of fracture complexity within the youngest (0–4-month-old) age group should be pursued.
A second key outcome of our study was the comparison of fracture length and nonlinearity trends with those previously reported by the new computational fracture mechanics framework. Yan et al.20 posited that a greater height increased potential energy in the infant head resulting in longer fractures. Similarly, the authors suggested that increased potential energy at greater heights allowed more energy to drive fractures across trabecular fibers, increasing the resulting nonlinearity. Our results did reveal a significant increase in fracture length with increasing fall heights, supporting the model’s predictions. In addition, we found that longer fractures were found in younger infants, again suggesting intrinsic age-related properties of the infant skull. We did not find a significant effect on fracture nonlinearity, however. In fact, no age or fall characteristics were found to significantly affect nonlinearity. From our analysis, increases in fracture length, number of skull bones involved, number of crack fronts, and number of total fractures all increased with increasing fall height—each of these features is a venue for energy release. We hypothesize that the FE model predicted increased nonlinearity with increasing height because its current capabilities do not allow for some of those venues, such as >2 crack fronts or multiple bone involvement.19
An interesting finding that did not support our initial hypothesis was the lack of a significant effect by impact surface on features of fracture complexity, nonlinearity, and length. Clinical studies will often categorize surfaces based on general recollections of flooring material (i.e., wood, tile), while biomechanical studies may categorize the impact surface depending on its mechanical response to a load. Some research groups have aimed to categorize flooring material based on its ability to absorb energy transmitted upon the impact of a solid object. The COR provides a measure of the energy absorbed by the impacted surface or returned to the object impacting the surface. A surface with high COR, such as tile or concrete, absorbs less energy from a falling object. The unabsorbed energy is then available to drive the formation of a crack initiation site and the propagation of a resulting crack on the object. We found that while many features of skull fractures were not affected by the impact surface in our study population, the number of cracks and the number of skull bones involved did see a significant decrease with low COR impact surfaces and a significant increase with high COR impact surfaces. Furthermore, we found an increased number of cracks in impacts with a low COR surface from higher heights. These results suggest that impact surface does have a significant role in determining the initial avenue for energy release where the energy returned by the surface will be channeled into crack formation. Once the cracks are formed, however, the length of the fracture and additional features of complexity are more likely related to the existing skull architecture, which our results have suggested are strongly dependent on the infant’s age.
Of note, impact surface COR testing provides a range of values that will vary across experiments. Furthermore, surface values may vary within the same experiment given heterogeneity in the tested surface’s composition or attachment to subflooring. In this study, we have dichotomized COR values into high and low categories to allow for categorical impact surface grouping. This may challenge the classification of surfaces that, depending on the study design, can show relatively high or low COR. For example, carpet, a common impact surface across infant falls, has shown variable COR results across studies, likely related to the tested carpet’s textile composition and its underlaying surface.23,24 We found that plush carpeted surfaces, often located in bedrooms, have relatively low COR, while carpeted concrete surfaces yielded a higher COR. This is comparable with prior studies, although carpet remains a generally variable surface. This source of variability should be considered as anthropomorphic or computational fall simulations continue to be refined.
Finally, STS was notably common in our sample, consistent with prior skull fracture-related studies.32 Despite its frequency, skull fracture-associated STS is not completely understood, and literature remains limited. While STS has been previously thought of as solely an indicator of impact location, clinical research has increasingly suggested that this conjecture is unsupported. One skull fracture phenomenon providing support against this assumption is the development of biparietal fractures. Prior studies have shown that biparietal fractures can result from single impacts33,34,35 and STS has been found to commonly overlay both fractures in single-impact cases. This is consistent with our findings where STS was found to overlay both parietal fractures in all but 2 of 17 biparietal cases, all of which had a reported single-impact mechanism.
We believe the consistency across studies suggests that scalp STS commonly dictates the fracture location rather than the impact site. This supports a recent retrospective review of 234 cases of bilateral skull fractures in children ≤24 months of age.36 Interestingly, 70.6% of bilateral fractures in this study were identified in infants <6 months old with STS overlying bilateral fractures in just over 61% of total cases. While mechanism of injury was not specifically addressed, the authors posit that bilateral scalp hematomas may indicate focal impact or localized edema secondary to bone breakage regardless of an impact at the swelling’s specific location. They add that scalp hematomas may not necessarily indicate a double impact. Of note, neither study radiographically specified the content of the overlying swelling. It is reasonable, however, to assume that the terms can be used interchangeably when compared with our results. Further research evaluating soft tissue biomechanical responses to skull fractures should be pursued. In addition, evaluating specific impact scenarios and the likelihood of biparietal fractures will improve our understanding of biparietal fracture mechanics and its relationship to both inflicted and accidental injury.
Our study did have limitations. Its retrospective nature lends itself to the risk of incomplete data, seen primarily in our categorization of impact surfaces and their associated COR, resulting in 25 “unknown COR” cases. This raises the small but real possibility that surface may have had a larger impact in our results had the information been known. Despite an inherent risk of circular bias and missed inflicted trauma, we feel confident that evaluations were thorough and in accordance with protocols current at the time, eliciting a relatively low concern for any meaningful number of missed cases. Given the study’s design, we had to rely on numerous estimates, specifically surface COR and fall heights. As estimates, they remain imprecise, and although we do not have a significant concern for major deviations, if present, they may have an unrecognized effect on our results. While we evaluated multiple variables and skull fracture outcomes, other potentially influential factors are yet to be characterized and warrant further study.
In conclusion, intrinsic age-related properties of the infant skull confer unique and evolving responses to impact. Specifically, (1) age should be recognized as an influential factor in skull fracture propagation in addition to fall height, and younger infant age groups should be further studied; (2) biomechanical models should aim to incorporate multi-crack formation and multi-bone involvement to increase biofidelity, particularly in young infants; and (3) efforts to improve our biomechanical and clinical understanding of multiple fractures, such as biparietal fractures, and associated STS should be encouraged. Further characterization of these properties will improve our understanding of infant skull fractures and the infant skull’s response to accidental and inflicted mechanisms of trauma.
Data availability
In accordance with Springer Nature’s Data Policy Type 3, all relevant raw data will be freely available to any researcher wishing to use them for non-commercial purposes, without breaching subject confidentiality. The datasets generated or analyzed during the current study are available from the corresponding author upon reasonable request.
References
Mulligan, C. S., Adams, S., Tzioumi, D. & Brown, J. Injury from falls in infants less than one year. J. Paediatr. Child Health 53, 754–760 (2017).
Wegmann, H. et al. The epidemiology of fractures in infants – which accidents are preventable? Injury 47, 188–191 (2016).
Reece, R. M. & Sege, R. Childhood head injuries: accident or abuse? Arch. Pediatr. Adolesc. Med. 154, 11–15 (2000).
Wood, J. N. et al. Use and utility of skeletal surveys to evaluate for occult fractures in young injured children. Acad. Pediatr. 19, 428–437 (2019).
Laskey, A. L., Stump, T. E., Hicks, R. A. & Smith, J. L. Yield of skeletal surveys in children ≤ 18 months of age presenting with isolated skull fractures. J. Pediatr. 162, 86–89 (2013).
Deye, K. P., Berger, R. P. & Lindberg, D. M., ExSTRA Investigators. Occult abusive injuries in infants with apparently isolated skull fractures. J. Trauma Acute Care Surg. 74, 1553–1558 (2013).
Kalichman, S. C. & Brosig, C. L. Mandatory child abuse reporting laws: issues and implications for policy. Law Policy 14, 153–168 (1992).
Hobbs, C. J. Skull fracture and the diagnosis of abuse. Arch. Dis. Child. 59, 246–252 (1984).
Leventhal, J. M., Thomas, S. A., Rosenfield, N. S. & Markowitz, R. I. Fracture in young children: distinguishing child abuse from unintentional injury. Am. J. Dis. Child. 147, 87–92 (1993).
Kemp, A. M. et al. Patterns of skeletal fractures in child abuse: systematic review. BMJ 337, a1518 (2008).
Metz, J. B. et al. Are complex skull fractures indicative of either child abuse or major trauma in the era of 3-dimensional computed tomography imaging? Pediatr. Emerg. Care. 38, e200–e204 (2022).
Coats, B., Ji, S. & Margulies, S. S. Material properties of human infant skull and suture at high rates. J. Neurotrauma 23, 1222–1232 (2006).
Metcalf, R. M., Comstock, J. M. & Coats, B. High-rate anisotropic properties in human infant parietal and occipital bone. J. Biomech. Eng. 143, 061010 (2021).
Weber, W. Biomechanical fragility of the infant skull. Z. Rechtsmed. 94, 93–101 (1985). German.
Li, Z. et al. A statistical skull geometry model for children 0-3 years old. PLoS ONE 10, e0127322 (2015).
Coats, B., Margulies, S. S. & Ji, S. Parametric study of head impact in the infant. Stapp Car Crash J. 51, 1–15 (2007).
Li, Z. et al. Development, validation, and application of a parametric pediatric head finite element model for impact simulation. Ann. Biomed. Eng. 39, 2984–2997 (2011).
Li, X., Sandler, H. & Kleiven, S. The importance of nonlinear tissue modelling in finite element simulations of infant head impacts. Biomech. Model Mechanobiol. 16, 823–840 (2017).
He, J., Yan, J., Margulies, S., Coats, B. & Spear, A. D. An adaptive-remeshing framework to predict impact-induced skull fracture in infants. Biomech. Model Mechanobiol. 19, 1595–1605 (2020).
Yan, J., He, J., Spear, A. & Coats, B. The effect of impact angle and fall height on skull fracture patterns in infants. J. Biomech. Eng. 143, 071004 (2021).
Kleinman, P. K., Coats, B. & Silvera V. M. Abusive head trauma: scalp, subscalp, and cranium. In: Diagnostic Imaging of Child Abuse (ed Kleinman, P. K.) 357–393 (Cambridge University Press, United Kingdom, 2015).
Chaudhary, S., et al. Pediatric falls ages 0–4: understanding demographics, mechanisms, and injury severities. Inj. Epidemiol. 5, 7 (2018).
Thompson, A. K., Bertocci, G. & Pierce, M. C. Assessment of head injury risk associated with feet-first free falls in 12-month-old children using an anthropomorphic test device. J. Trauma 66, 1019–1029 (2009).
Bertocci, G. et al. Influence of fall height and impact surface on biomechanics of feet-first free falls in children. Injury 35, 417–424 (2004).
Pinto, P. S., Poretti, A., Meoded, A., Tekes, A. & Huisman, T. A. G. M. The unique features of traumatic brain injury in children: Review of the characteristics of the pediatrics skull and brain, mechanisms of trauma, patterns of injury, complications and their imaging findings – part 1. J. Neuroimaging 22, e1–e17 (2012).
Margulies, S. S. & Thibault, K. L. Infant skull and suture properties: measurements and implications for mechanisms of pediatric brain injury. J. Biomech. Eng. 122, 364–371 (2000).
Ibrahim, N. & Margulies, S. S. Biomechanics of the toddler head during low-height falls: an anthropomorphic dummy analysis. J. Neurosurg. Pediatr. 6, 57–68 (2010).
Parks, S., Annest, J., Hill, H. & Karch, D. Pediatric Abusive Head Trauma: Recommended Definitions for Public Health Surveillance and Research (Centers for Disease Control and Prevention, Atlanta, GA, 2012).
Kriss, S., Morris, J. & Martich, V. Cranial suture evaluation in pediatric head trauma: Importance in differentiating abusive from accidental injury. Pediatr. Emerg. Care. 38, e703–e708 (2022).
Kriss, S., Morris, J. & Martich, V. Pediatric skull fractures contacting sutures: relevance in abusive head trauma. AJR Am. J. Roentgenol. 217, 218–222 (2021).
Uçan, B., Tokur, O. & Aydin, S. Pediatric skull fractures: could suture contact be a sign of abuse? Emerg. Radiol. 29, 403–408 (2022).
Metz, J. B. et al. Fracture-associated bruising and soft tissue swelling in young children with skull fractures: how sensitive are they to fracture presence? Pediatr. Emerg. Care. 37, e1392–e1396 (2021).
O’Hara, M. A. The infant with bilateral skull fractures: diagnostic considerations in consultation with a child abuse pediatrician. J. Inj. Violence Res. 11, 15–20 (2019).
Arnholz, D., Hymel, K. P., Hay, T. C. & Jenny, C. Bilateral pediatric skull fractures: accident or abuse? J. Trauma. 45, 172–174 (1998).
Aysha, A., Morantz, G., Lacroix, C., Saint-Martin, C. & Dudley, R. W. R. Bilateral parietal skull fractures in infants attributable to accidental falls. Pediatr. Neurosurg. 56, 424–431 (2021).
O’Hara, M. A. et al. Understanding bilateral skull fractures in infancy: a retrospective multicenter case review. Pediatr. Emerg. Care. Epub ahead of print (2022).
Acknowledgements
Statistical support was provided by the National Center for Advancing Translational Sciences of the National Institutes of Health under Award Number UL1TR002538. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health. In addition, the authors would like to acknowledge Primary Children Hospital’s Pediatric Radiology Department for guidance and assistance with a radiological review.
Funding
This work was supported by Award No. 2016-DN-BX-0160 and 2020-75-CX-0014, provided by the National Institute of Justice, Office of Justice Programs, U.S. Department of Justice. The opinions, findings, and conclusions or recommendations expressed in this publication are those of the authors and do not necessarily reflect those of the Department of Justice.
Author information
Authors and Affiliations
Contributions
T.M.R.-M. has substantially contributed to the conception and design of this study; has collected, analyzed, and interpreted data; and has written the manuscript. Y.A. performed image analysis and collected data. B.C. designed this study, analyzed and interpreted the data, and also wrote the manuscript. All three authors read, critically revised, and approved the final manuscript.
Corresponding author
Ethics declarations
Competing interests
T.M.R.-M. has provided medicolegal consultation and expert testimony on cases of suspected child abuse and neglect. No other competing interests were noted by the authors.
Ethics approval and consent to participate
This study was reviewed and approved by the University of Utah Institutional Review Board (IRB) and was deemed to be exempt research. Therefore, consent was not required for this study.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Ruiz-Maldonado, T.M., Alsanea, Y. & Coats, B. Age-related skull fracture patterns in infants after low-height falls. Pediatr Res 93, 1990–1998 (2023). https://doi.org/10.1038/s41390-022-02345-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41390-022-02345-9
- Springer Nature America, Inc.