Abstract
Background
For people with dementia, moving into a nursing home is usually considered at some point in time. Currently available information on predictors of institutionalization is often based on small sample sizes, not taking competing risks into account, and with inconclusive results for sex.
Aims
We aimed to carry out an analysis stratified by sex and using a competing risk approach.
Methods
We carried out an analysis of a survey linked with administrative data including 652 people with dementia, aged 60 years and older. The follow-up was up to 4.5 years. We used the cumulative incidence function for examining time until institutionalization and survival time and the sub-distribution hazard model for estimating hazard ratios.
Results
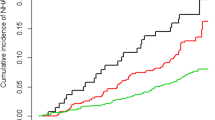
The participants were on average 81 years old, about 51% were female. At the end of the follow-up, 282 people had been institutionalized and 273 had died. The regression models show that the risk of institutionalization is higher in women than in men and when cared for by a care service in comparison to an informal caregiver. Inhibiting factors are Care Level (II, III) and positive evaluation of caregiving by caregivers. Stratified analysis by sex revealed that the risk of institutionalization in men is influenced by their relationship to their caregiver, in women by duration of care at baseline.
Discussion
Sex seems to play a role in predicting institutionalization.
Conclusion
Future research should focus on stratified analysis by sex. Knowing the predictors of institutionalization for men and women could influence long-term care management remarkably.



Similar content being viewed by others
References
Cepoiu-Martin M, Tam-Tham H, Patten S et al (2016) Predictors of long-term care placement in persons with dementia: a systematic review and meta-analysis. Int J Geriatr Psychiatry. doi:10.1002/gps.4449
Berry SD, Ngo L, Samelson EJ et al (2010) Competing risk of death: an important consideration in studies of older adults. J Am Geriatr Soc 58:783–787. doi:10.1111/j.1532-5415.2010.02767.x
Castora-Binkley M, Meng H, Hyer K (2014) Predictors of long-term nursing home placement under competing risk: evidence from the Health and Retirement Study. J Am Geriatr Soc 62:913–918. doi:10.1111/jgs.12781
Eska K, Graessel E, Donath C et al. (2013) Predictors of institutionalization of dementia patients in mild and moderate stages: a 4-year prospective analysis. Dement Geriatr Cogn Dis Extra 3:426–445. doi:10.1159/000355079
Gaugler JE, Yu F, Krichbaum K et al (2009) Predictors of nursing home admission for persons with dementia. Med Care 47:191–198. doi:10.1097/MLR.0b013e31818457ce
Luppa M, Riedel-Heller SG, Stein J et al (2012) Predictors of institutionalisation in incident dementia: results of the German Study on Ageing, Cognition and Dementia in Primary Care Patients (AgeCoDe study). Dement Geriatr Cogn Disord 33:282–288. doi:10.1159/000339729
Schulze J, van den Bussche H, Kaduszkiewicz H et al (2015) Institutionalization in incident dementia cases in comparison to age- and sex-matched controls: a 5-year follow-up from Germany. Soc Psychiatry Psychiatr Epidemiol 50:143–151. doi:10.1007/s00127-014-0911-3
Luppa M, Gentzsch K, Angermeyer MC et al (2011) Gender-specific predictors of institutionalisation in the elderly: results of the Leipzig longitudinal study of the aged (LEILA 75+) (Geschlechtsspezifische Pradiktoren von Institutionalisierung im Alter - Ergebnisse der Leipziger Langsschnittstudie in der Altenbevolkerung (LEILA 75+)). Psychiatr Prax 38:185–189. doi:10.1055/s-0030-1248496
Meinck M, Lubke N (2013) Geriatric multimorbidity in claims data: part 3: prevalence and predictive power of geriatric conditions in an age-specific systematic sample (Geriatrietypische Multimorbiditat im Spiegel von Routinedaten: Teil 3: Pravalenz und pradiktiver Wert geriatrietypischer Merkmalskomplexe in einer systematischen Altersstichprobe). Z Gerontol Geriatr 46:645–657. doi:10.1007/s00391-012-0462-8
Beekmann M, van den Bussche H, Glaeske G et al (2012) Geriatric morbidity patterns and need for long-term care in patients with dementia (Geriatrietypische Morbiditatsmuster und Pflegebedurftigkeit bei Patienten mit Demenz). Psychiatr Prax 39:222–227. doi:10.1055/s-0032-1305010
Busse R, Blumel M (2014) Germany: health system review. Health Syst Transit 16:1–296xxi
Prosiegel M, Böttger S, Schenk T et al (1996) Der Erweiterte Barthel-Index (EBI): eine neue Skala zur Erfassung von Fähigkeitsstörungen bei neurologischen Patienten. Neurologie und Rehabilit 2:7–13
Lawton MP, Brody EM (1969) Assessment of older people: self-maintaining and instrumental activities of daily living. Gerontologist 9:179–186
Balducci C, Mnich E, McKee KJ et al (2008) Negative impact and positive value in caregiving: validation of the COPE index in a six-country sample of carers. Gerontologist 48:276–286
Ware JE, Kosinski M, Turner-Bowker DM et al (2002) How to score version 2 of the SF-12 health survey. Quality Metric Incorporated, Lincoln
Gondara L (2015) Competing risk survival analysis using SAS: when, why and how. http://support.sas.com/resources/papers/proceedings15/1424-2015.pdf. Accessed 05 Aug 2016
Fine JP, Gray RJ (1999) A proportional hazards model for the subdistribution of a competing risk. J Am Stat Assoc 94:496–509. doi:10.1080/01621459.1999.10474144
Prince M, Ali G-C, Guerchet M et al (2016) Recent global trends in the prevalence and incidence of dementia, and survival with dementia. Alzheimers Res Ther 8:23. doi:10.1186/s13195-016-0188-8
Wimo A, Jonsson L, Bond J et al (2013) The worldwide economic impact of dementia 2010. Alzheimers Dement 9:1–11.e3. doi:10.1016/j.jalz.2012.11.006
Luppa M, Luck T, Weyerer S et al (2010) Prediction of institutionalization in the elderly. A systematic review. Age Ageing 39:31–38. doi:10.1093/ageing/afp202
Andel R, Hyer K, Slack A (2007) Risk factors for nursing home placement in older adults with and without dementia. J Aging Health 19:213–228. doi:10.1177/0898264307299359
Schoenmakers B, Buntinx F, Devroey D et al (2009) The process of definitive institutionalization of community dwelling demented vs non demented elderly: data obtained from a network of sentinel general practitioners. Int J Geriatr Psychiatry 24:523–531. doi:10.1002/gps.2147
Neumann PJ, Araki SS, Gutterman EM (2000) The use of proxy respondents in studies of older adults: lessons, challenges, and opportunities. J Am Geriatr Soc 48:1646–1654
Acknowledgements
We thank the German health insurance fund BARMER GEK for providing the data analysed in our study and for their support while conducting the survey. The survey was conducted in the context of a project funded by the BARMER GEK.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
There is no conflict of interest.
Informed consent
By returning the questionnaire participants gave their consent.
Research including human participants
All procedures performed in studies involving human participants were in accordance with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Appendix
Rights and permissions
About this article
Cite this article
Runte, R. Predictors of institutionalization in people with dementia: a survey linked with administrative data. Aging Clin Exp Res 30, 35–43 (2018). https://doi.org/10.1007/s40520-017-0737-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40520-017-0737-4