Abstract
Supportive care and pharmacological treatment can improve the quality of life of people with end-stage chronic obstructive pulmonary disease (COPD) who cope on a daily basis with substantial physical, psychological, social and spiritual morbidity. Smoking cessation is the only intervention that reduces the rate of progression of COPD, but evidence-based drug treatments and non-pharmacological strategies can relieve symptoms and reduce the impact of exacerbations. People with severe COPD live with increasingly troublesome breathlessness and other symptoms such as fatigue, pain, sputum production and weight loss. As breathlessness increases, treatment is stepped up from short-acting to long-acting bronchodilators supplemented by non-pharmacological interventions such as pulmonary rehabilitation. Opiates relieve breathlessness, and referral to a multidisciplinary breathlessness service is an option for those with intractable symptoms. Other smoking-related conditions, such as coronary heart disease and lung cancer as well as depression and anxiety are common and should be treated with conventional pharmacotherapy. Acute exacerbations become more frequent and more severe as the disease reaches end-stage. Inhaled corticosteroids in combination with long-acting bronchodilators can reduce the frequency of exacerbations, and supported self-management aims to facilitate timely treatment of deterioration. Palliative care services have traditionally been predicated on identifying people with end-stage disease—a model that does not resonate with the unpredictable, relapsing trajectory of COPD. Approaches to care that promote a flexible approach to palliation alongside curative care could do much to improve the burden of living with severe COPD.

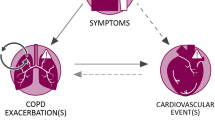
Adapted from Rocker et al. [8]
Similar content being viewed by others
References
Global Initiative for Chronic Obstructive Lung Disease. Global strategy for the diagnosis, management, and prevention of chronic obstructive pulmonary disease (2016). http://www.goldcopd.org. Accessed Oct 2016.
Salvi SS, Barnes PJ. Chronic obstructive pulmonary disease in non-smokers. Lancet. 2009;374:733–43.
van Gemert F, Kirenga B, Chavannes N, Kamya M, Luzige S, Musinguzi P, et al. Prevalence of chronic obstructive pulmonary disease and associated risk factors in Uganda (FRESH AIR Uganda): a prospective cross-sectional observational study. Lancet Global Health. 2015;3:e44–51.
van Gemert F, Chavannes N, Kirenga B, Jones R, Williams S, Tsiligianni I, et al. Socio-economic factors, gender and smoking as determinants of COPD in a low-income country of sub-Saharan Africa: FRESH AIR Uganda. NPJ Prim Care Respir Med. 2016;26:16050.
Murray CJL, Vos T, Lozano R, Naghavi M, Flaxman AD, Michaud C, et al. Disability-adjusted life years (DALYs) for 291 diseases and injuries in 21 regions, 1990–2010: a systematic analysis for the Global Burden of Disease Study 2010. Lancet. 2012;380:2197–223.
Habraken JM, Willems DL, de Kort SJ, Bindels PJE. Health care needs in end-stage COPD: a structured literature review. Patient Educ Couns. 2007;68:121–30.
Seamark DA, Seamark CJ, Halpin D. Palliative care in chronic obstructive pulmonary disease: a review for clinicians. J R Soc Med. 2007;100:225–33.
Rocker GM, Sinuff T, Horton R, Hernandez P. Advanced chronic obstructive pulmonary disease: innovative approaches to palliation. J Palliat Med. 2007;10:783–96.
Janssen DJ, Spruit MA, Wouters EF, Schols JM. Daily symptom burden in end-stage chronic organ failure: a systematic review. Palliat Med. 2008;22:938–48.
Giacomini M, DeJean D, Simeonov D, Smith A. Experiences of living and dying with COPD: a systematic review and synthesis of the qualitative empirical literature. Ont Health Technol Assess Ser. 2012;12:1–47.
Buckingham S, Kendall M, Ferguson S, MacNee W, Sheikh A, White P, et al. HELPing older people with very severe chronic obstructive pulmonary disease (HELP-COPD): piloting a practical intervention. NPJ Prim Care Respir Med. 2015;25:15020.
Epiphaniou E, Shipman C, Harding R, Mason B, Murray SA, Higginson IJ, et al. Coordination of end-of-life care for patients with lung cancer and those with advanced COPD: are there transferable lessons? A longitudinal qualitative study. Prim Care Respir J. 2014;23:46–51.
Gore JM, Brophy CJ, Greenstone MA. How well do we care for patients with end stage chronic obstructive pulmonary disease (COPD)? A comparison of palliative care and quality of life in COPD and lung cancer. Thorax. 2000;55:1000–6.
Barnett K, Mercer SW, Norbury M, Watt G, Wyke S, Guthrie B. Epidemiology of multimorbidity and implications for health care, research, and medical education: a cross-sectional study. Lancet. 2012;380:37–43.
Lozano R, Naghavi M, Foreman K, Lim S, Shibuya K, Aboyans V, et al. Global and regional mortality from 235 causes of death for 20 age groups in 1990 and 2010: a systematic analysis for the Global Burden of Disease Study 2010. Lancet. 2012;380:37–43.
Connors AF, Dawson NV, Thomas C, Harrell FE, Desbiens N, Fulkerson WJ, et al. Outcomes following acute exacerbation of chronic obstructive lung disease. The SUPPORT investigators. Am J Respir Crit Care Med. 1996;154:959–67.
Almagro P, Calbo E, de Echagüen AO, Quintana BBS, Heredia JL, Garau J. Mortality after hospitalization for COPD. Chest. 2002;121:1441–8.
Calverley PMA, Anderson JA, Celli B, Ferguson GT, Jenkins C, Jones PW, et al. Salmeterol and fluticasone propionate and survival in chronic obstructive pulmonary disease. N Engl J Med. 2007;356:775–89.
Lynn J, Adamson D. Living well at the end of life. Adapting health care to serious chronic illness in old age. Santa Monica: RAND; 2003.
World Health Organization Europe. The solid facts: palliative care. Copenhagen: WHO; 2004.
House of Commons Health Committee. Palliative care. London: The Stationery Office; 2004.
National Institute for Health and Clinical Excellence. National clinical guideline management of chronic obstructive pulmonary disease in adults in primary and secondary care. Thorax. 2004;59(Suppl 1):S1–232.
Qaseem A, Wilt TJ, Weinberger SE, Hanania NA, Criner G, Van der Molen T, et al. Diagnosis and management of stable chronic obstructive pulmonary disease: a clinical practice guideline update from the American College of Physicians, American College of Chest Physicians, American Thoracic Society, and European Respiratory Society. Ann Intern Med. 2011;155:179–91.
Abramson M, Frith P, Yang I, McDonald C, Hancock K, Jenkins S, et al. COPD-X concise guide for primary care. Brisbane: Lung Foundation Australia; 2016.
Kendall M, Buckingham S, Ferguson S, Hewitt N, Pinnock H. We need to stop looking for something that is not there…. [letter]. NPJ Prim Care Respir Med. 2014;24:14031.
Murray SA, Kendall M, Boyd K, Sheikh A. Illness trajectories and palliative care. BMJ. 2005;330:1007–11.
Murray SA, Boyd K, Sheikh A. Palliative care in chronic illness. We need to move from prognostic paralysis to active total care. BMJ. 2005;330:611–2.
Lanken PN, Terry PB, DeLisser HM, Fahy BF, Hansen-Flaschen J, Heffner JE, on behalf of the ATS End-of-Life Care Task Force, et al. An Official American Thoracic Society clinical policy statement: palliative care for patients with respiratory diseases and critical illnesses. Am J Respir Crit Care Med. 2008;177:912–27.
Christakis NA, Lamont EB. Extent and determinants of error in doctor’s prognosis in terminally ill patients: prospective cohort study. BMJ. 2000;320:469–73.
Pinnock H, Kendall M, Murray SA, Worth A, Levack P, Porter M, et al. Living and dying with severe chronic obstructive pulmonary disease: multi-perspective longitudinal qualitative study. BMJ. 2011;342:d142.
Coventry PA, Grande GE, Richards DA, Todd CJ. Prediction of appropriate timing of palliative care for older adults with non-malignant life-threatening disease: a systematic review. Age Ageing. 2005;34:218–27.
Murray S, Pinnock H, Sheikh A. Palliative care for people with COPD: we need to meet the challenge. Prim Care Respir J. 2006;15:362–4.
Habraken JM, Pols J, Bindels PJE, Willems DL. The silence of patients with end-stage COPD: a qualitative study. Br J Gen Pract. 2008;58:844–9.
Kendall M, Buckingham S, Ferguson S, MacNee W, Sheikh A, White P, et al. Exploring the concept of need in people with very severe chronic obstructive pulmonary disease: a qualitative study BMJ Support Palliat Care. 2015. doi:10.1136/bmjspcare-2015-000904.
Tashkin DP, Rennard S, Hays JT, Lawrence D, Marton JP, Lee TC. Lung function and respiratory symptoms in a 1-year randomised smoking cessation trial of varenicline in COPD patients. Respir Med. 2011;105:1682–90.
Anthonisen NR, Connett JE, Kiley JP, Altose MD, Bailey WC, Buist AS, et al. Effects of smoking intervention and the use of an inhaled anticholinergic bronchodilator on the rate of decline of FEV1. The Lung Health Study. JAMA. 1994;272:1497–505.
Stead LF, Koilpillai P, Fanshawe TR, Lancaster T. Combined pharmacotherapy and behavioural interventions for smoking cessation. Cochrane Database Syst Rev. 2016;3:CD008286. doi:10.1002/14651858.CD008286.pub3.
van Eerd EAM, van der Meer RM, van Schayck OCP, Kotz D. Smoking cessation for people with chronic obstructive pulmonary disease. Cochrane Database Syst Rev. 2016;8:CD010744. doi:10.1002/14651858.CD010744.pub2.
Cahill K, Stevens S, Perera R, Lancaster T. Pharmacological interventions for smoking cessation: an overview and network meta-analysis. Cochrane Database Syst Rev. 2013;5:CD009329. doi:10.1002/14651858.CD009329.pub2.
Stead LF, Perera R, Bullen C, Mant D, Hartmann-Boyce J, Cahill K, et al. Nicotine replacement therapy for smoking cessation. Cochrane Database Syst Rev. 2012;11:CD000146. doi:10.1002/14651858.CD000146.pub4.
Rigotti NA, Clair C, Munafò MR, Stead LF. Interventions for smoking cessation in hospitalised patients. Cochrane Database Syst Rev. 2012;5:CD001837. doi:10.1002/14651858.CD001837.pub3.
Cahill K, Lindson-Hawley N, Thomas KH, Fanshawe TR, Lancaster T. Nicotine receptor partial agonists for smoking cessation. Cochrane Database Syst Rev. 2016;5:CD006103. doi:10.1002/14651858.CD006103.pub7.
Nocturnal Oxygen Therapy Trial Group. Continuous or nocturnal oxygen therapy in hypoxemic chronic obstructive lung disease: a clinical trial. Ann Intern Med. 1980;93:391–8.
Cooper CB, Waterhouse J, Howard P. Twelve year clinical study of patients with hypoxic cor pulmonale given long term domiciliary oxygen therapy. Thorax. 1987;42:105–10.
Gulbas G, Gunen H, In E, Kilic T. Long-term follow-up of chronic obstructive pulmonary disease patients on long-term oxygen treatment. Int J Clin Pract. 2012;66:152–7.
British Thoracic Society. BTS guideline for home oxygen use in adults. Thorax. 2015;70(Suppl 1):i1–43.
Goodridge D. People with chronic obstructive pulmonary disease at the end of life: a review of the literature. Int J Palliat Nurs. 2006;12:390–6.
Spathis A, Booth S. End of life care in chronic obstructive pulmonary disease: in search of a good death. Int J COPD. 2008;3:11–29.
Dean MM. End-of-life care for COPD patients. Prim Care Respir J. 2008;17:46–50.
Ambrosino N, Simonds A. The clinical management in extremely severe COPD. Respir Med. 2007;101:1613–24.
Elofsson LC, Ohlen J. Meanings of being old and living with chronic obstructive pulmonary disease. Palliat Med. 2004;18:611–8.
Skilbeck J, Mott L, Smith D, Page H, Clark D. Nursing care for people dying from chronic obstructive pulmonary disease. Int J Palliat Nurs. 1997;3:100–6.
Gysels M, Bausewein C, Higginson IJ. Experiences of breathlessness: a systematic review of the qualitative literature. Palliat Support Care. 2007;5:281–302.
Seamark DA, Blake SD, Seamark CJ. Living with severe chronic obstructive pulmonary disease (COPD): perceptions of patients and their carers. Palliative Med. 2004;18:619–25.
Jones PW, Harding G, Wiklund I, Berry P, Leidy NI. Improving the process and outcome of care in COPD: development of a standardised assessment tool. Prim Care Respir J. 2009;18:208–15.
Sestini P, Renzoni E, Robinson S, Poole P, Ram FSF. Short-acting beta2-agonists for stable chronic obstructive pulmonary disease. Cochrane Database Syst Rev. 2002. doi:10.1002/14651858.CD001495.
Appleton S, Jones T, Poole P, Pilotto L, Adams R, Lasserson TJ, et al. Ipratropium bromide versus short acting beta-2 agonists for stable chronic obstructive pulmonary disease. Cochrane Database Syst Rev. 2006. doi:10.1002/14651858.CD001387.pub2.
Kew KM, Mavergames C, Walters JA. Long-acting beta2-agonists for chronic obstructive pulmonary disease. Cochrane Database Syst Rev. 2013;10:CD010177. doi:10.1002/14651858.CD010177.pub2.
Barr RG, Bourbeau J, Camargo CA Jr. Tiotropium for stable chronic obstructive pulmonary disease. Cochrane Database Syst Rev. 2005;2:CD002876. doi:10.1002/14651858.CD002876.pub2.
Farne HA, Cates CJ. Long-acting beta2-agonist in addition to tiotropium versus either tiotropium or long-acting beta2-agonist alone for chronic obstructive pulmonary disease. Cochrane Database Syst Rev. 2015. doi:10.1002/14651858.CD008989.pub3.
Van Boven JF, Chavannes NH, van der Molen T, Rutten-van Mölken MP, Postma MJ, Vegter S. Clinical and economic impact of non-adherence in COPD: a systematic review. Respir Med. 2014;108:103–13.
Nannini LJ, Poole P, Milan SJ, Holmes R, Normansell R. Combined corticosteroid and long-acting beta2-agonist in one inhaler versus placebo for chronic obstructive pulmonary disease. Cochrane Database Syst Rev. 2013. doi:10.1002/14651858.CD003794.pub4.
Kew KM, Seniukovich A. Inhaled steroids and risk of pneumonia for chronic obstructive pulmonary disease. Cochrane Database Syst Rev. 2014. doi:10.1002/14651858.CD010115.pub2.
Rojas-Reyes MX, García Morales OM, Dennis RJ, Karner C. Combination inhaled steroid and long-acting beta2-agonist in addition to tiotropium versus tiotropium or combination alone for chronic obstructive pulmonary disease. Cochrane Database Syst Rev. 2016. doi:10.1002/14651858.CD008532.pub3.
Corhay J-L, Nguyen Dang D, Van Cauwenberge H, Louis R. Pulmonary rehabilitation and COPD: providing patients a good environment for optimising therapy. Int J Chron Obstruct Pulmon Dis. 2014;9:27–39.
McCarthy B, Casey D, Devane D, Murphy K, Murphy E, Lacasse Y. Pulmonary rehabilitation for chronic obstructive pulmonary disease. Cochrane Database Syst Rev. 2015. doi:10.1002/14651858.CD003793.pub3.
Evans RA, Singh SJ, Collier R, Williams JE, Morgan MD. Pulmonary rehabilitation is successful for COPD irrespective of MRC dyspnoea grade. Respir Med. 2009;103:1070–5.
Spruit MA, Singh SJ, Garvey C, ZuWallack R, Nici L, Rochester C, et al. An official American Thoracic Society/European Respiratory Society statement: key concepts and advances in pulmonary rehabilitation. Am J Respir Crit Care Med. 2013;188:e13–64.
Murphy L, Harrington P, Taylor SJC, Teljour C, Smith SM, Pinnock H, et al. The clinical-effectiveness of self-management support interventions in chronic obstructive pulmonary disease: an overview of reviews. Chron Respir Dis (in press).
Lewis A, Cave P, Stern M, Welch L, Taylor K, Russell J, et al. Singing for Lung Health—a systematic review of the literature and consensus statement. NPJ Prim Care Respir Med. 2016;1(26):16080.
Jennings AL, Davies AN, Higgins JP, Gibbs JS, Broadley KE. A systematic review of the use of opioids in the management of dyspnoea. Thorax. 2002;57:939–44.
Abernethy AP, Currow DC, Frith P, Fazekas BS, McHugh A, Bui C. Randomised, double blind, placebo controlled crossover trial of sustained release morphine for the management of refractory dyspnoea. BMJ. 2003;327:523–8.
British Medical Association/Royal Pharmaceutical Society. British National Formulary. No. 72. London: British Medical Association/Royal Pharmaceutical Society; 2016. p. 421.
Hardy J, Randall C, Pinkerton E, Flatley C, Gibbons K, Allan S. A randomised, double-blind controlled trial of intranasal midazolam for the palliation of dyspnoea in patients with life-limiting disease. Support Care Cancer. 2016;24:3069–76.
Simon ST, Higginson IJ, Booth S, Harding R, Bausewein C. Benzodiazepines for the relief of breathlessness in advanced malignant and non-malignant diseases in adults. Cochrane Database Syst Rev. 2010. doi:10.1002/14651858.CD007354.pub2.
Johnson MJ, Barbetta C, Currow DC, Maddocks M, McDonald V, Mahadeva R, et al. Management of chronic breathlessness. In: Bausewein C, Currow DC, Johnson MJ, editors. Palliative care in respiratory disease. ERS Monograph, vol. 73. Sheffield: European Respiratory Society; 2016. p. 111–33.
Currow DC, Agar M, Smith J, Abernethy AP. Does palliative home oxygen improve dyspnoea? A consecutive cohort study. Palliative Med. 2009;23:309–16.
Booth S, Anderson H, Swannick M, Wade R, Kite S, Johnson M. The use of oxygen in the palliation of breathlessness. A report of the expert working group of the scientific committee of the association of palliative medicine. Respir Med. 2004;98:66–77.
Struik FM, Lacasse Y, Goldstein RS, Kerstjens HA, Wijkstra PJ. Nocturnal noninvasive positive pressure ventilation in stable COPD: a systematic review and individual patient data meta-analysis. Respir Med. 2014;108:329–37.
Higginson IJ, Bausewein C, Reilly CC, Gao W, Gysels M, Dzingina M, et al. An integrated palliative and respiratory care service for patients with advanced disease and refractory breathlessness: a randomised controlled trial. Lancet Respir Med. 2014;2:979–87.
HajGhanbari B, Holsti L, Road JD, Reid WD. Pain in people with chronic obstructive pulmonary disease. Resp Med. 2012;106:998–1005.
World Health Organization. WHO's cancer pain ladder for adults. http://www.who.int/cancer/palliative/painladder/en. Accessed Oct 2016.
Ferreira I, Brooks D, Lacasse Y, Goldstein R, White J. Nutritional supplementation for stable chronic obstructive pulmonary disease. Cochrane Database Syst Rev. 2005. doi:10.1002/14651858.CD000998.pub.
Osadnik CR, McDonald CF, Jones AP, Holland AE. Airway clearance techniques for chronic obstructive pulmonary disease. Cochrane Database Syst Rev. 2012. doi:10.1002/14651858.CD008328.pub2.
Poole P, Chong J, Cates CJ. Mucolytic agents versus placebo for chronic bronchitis or chronic obstructive pulmonary disease. Cochrane Database Syst Rev. 2015. doi:10.1002/14651858.CD001287.pub5.
National Institute for Health and Clinical Excellence. Multimorbidity: clinical assessment and management. NICE guidance 56. https://www.nice.org.uk/guidance/ng56. Accessed Dec 2016.
Feinstein AR. The pre-therapeutic classification of co-morbidity in chronic disease. J Chronic Dis. 1970;23:455–68.
Gallagher P, Ryan C, Byrne S, Kennedy J, O’Mahony D. STOPP (Screening Tool of Older Person’s Prescriptions) and START (Screening Tool to Alert doctors to Right Treatment). Consensus validation. Int J Clin Pharmacol Ther. 2008;46:72–83.
O’Mahony D, O’Sullivan D, Byrne S, O’Connor MN, Ryan C, Gallagher P. STOPP/START criteria for potentially inappropriate prescribing in older people: version 2. Age Ageing. 2015;44:213–8.
Van Manen JG, Bindels PJE, Dekker FW, IJzermans CJ, Van der Zee JS, Schade E. Risk of depression in patients with chronic obstructive pulmonary disease and its determinants. Thorax. 2002;57:412–6.
Mikkelsen RL, Middelboe T, Pisinger C, Stage KB. Anxiety and depression in patients with chronic obstructive pulmonary disease (COPD). A review. Nord J Psychiatry. 2004;58:65–70.
Maurer J, Rebbapragada V, Borson S, Goldstein R, Kunik ME, Yohannes AM, et al. Anxiety and depression in COPD. Current understanding, unanswered questions and research needs. Chest. 2008;134:435–565.
Brenes G. Anxiety and chronic pulmonary obstructive disease: prevalence, impact and treatment. Psychosom Med. 2003;65:963–70.
Fan VS, Ramsey SD, Giardino ND, Make BJ, Emery CF, Diaz PT, et al. Sex, depression, and risk of hospitalization and mortality in chronic obstructive pulmonary disease. Arch Intern Med. 2007;167:2345–53.
Usmani ZA, Carson KV, Cheng JN, Esterman AJ, Smith BJ. Pharmacological interventions for the treatment of anxiety disorders in chronic obstructive pulmonary disease. Cochrane Database Syst Rev. 2011. doi:10.1002/14651858.CD008483.pub2.
Yohannes AM, Alexopoulos GS. Pharmacological treatment of depression in older patients with chronic obstructive pulmonary disease: impact on the course of the disease and health outcomes. Drugs Aging. 2014;31:483.
Tselebis A, Pachi A, Ilias I, Kosmas E, Bratis D, Moussas G, et al. Strategies to improve anxiety and depression in patients with COPD: a mental health perspective. Neuropsychiatr Dis Treat. 2016;12:297.
Baraniak A, Sheffield D. The efficacy of psychologically based interventions to improve anxiety, depression and quality of life in COPD: a systematic review and meta-analysis. Patient Educ Couns. 2011;83:29–36.
Heslop K, Newton J, Baker C, Burns G, Carrick-Sen D, De Soyza A. Effectiveness of cognitive behavioural therapy (CBT) interventions for anxiety in patients with chronic obstructive pulmonary disease (COPD) undertaken by respiratory nurses: the COPD CBT CARE study: (ISRCTN55206395). BMC Pulm Med. 2013;13:62.
Coventry PA, Bower P, Keyworth C, Kenning C, Knopp J, Garrett C, et al. The effect of complex interventions on depression and anxiety in chronic obstructive pulmonary disease: systematic review and meta-analysis. PLoS One. 2013;8:e60532.
Guthrie E, Palmer L, Lelliott P, Agulnik D, Dupin M. No health without mental health – the supporting evidence. London: Royal College of Psychiatrists, Academy of Medical Royal Colleges; 2010.
Global Initiative for Asthma and Global Initiative for Chronic Obstructive Lung Disease. Asthma, COPD and Asthma-COPD Overlap Syndrome (ACOS). 2015. http://ginasthma.org/asthma-copd-and-asthma-copd-overlap-syndrome-acos. Accessed Oct 2016.
Suissa S, Dell’Aniello S. Ernst P Long-term natural history of chronic obstructive pulmonary disease: severe exacerbations and mortality. Thorax. 2012;67:957–63.
Calverley PM, Rabe KF, Goehring UM, Kristiansen S, Fabbri LM, Martinez FJ. Roflumilast in symptomatic chronic obstructive pulmonary disease: two randomised clinical trials. Lancet. 2009;374:685–94.
Rabe KF. Update on roflumilast, a phosphodiesterase 4 inhibitor for the treatment of chronic obstructive pulmonary disease. Br J Pharmacol. 2011;163:53–67.
Herath SC, Poole P. Prophylactic antibiotic therapy for chronic obstructive pulmonary disease (COPD). Cochrane Database Syst Rev. 2013. doi:10.1002/14651858.CD009764.pub2.
Varkey JB, Varkey AB, Varkey B. Prophylactic vaccinations in chronic obstructive pulmonary disease: current status. Curr Opinion Pulm Med. 2009;15:90–9.
Zwerink M, Brusse-Keizer M, van der Valk PD, Zielhuis GA, Monninkhof EM, van der Palen J, et al. Self management for patients with chronic obstructive pulmonary disease. Cochrane Database Syst Rev. 2014. doi:10.1002/14651858.CD002990.pub3.
Ure J, Hanley J, Pinnock H, Kidd G, McCall Smith E, Tarling A, et al. Piloting tele-monitoring in Chronic Obstructive Pulmonary Disease: a mixed methods exploration of issues in design and implementation. Prim Care Respir J. 2012;21:57–64.
Bolton CE, Waters CS, Peirce S, Elwyn G, on behalf of EPSRC and MRC Grand Challenge Team. Insufficient evidence of benefit: a systematic review of home telemonitoring for COPD. J Eval Clin Pract. 2011;17:1216–22.
Steventon A, Bardsley M, Billings J, Dixon J, Doll H, Hirani S, for the Whole System Demonstrator Evaluation Team, et al. Effect of telehealth on use of secondary care and mortality: findings from the Whole System Demonstrator cluster randomised trial. BMJ. 2012;344:e3874.
Pinnock H, Hanley J, McCloughan L, Todd A, Krishan A, Lewis S, et al. Effectiveness of telemonitoring integrated into existing clinical services on hospital admission for exacerbation of chronic obstructive pulmonary disease: researcher blind, multicentre, randomised controlled trial. BMJ. 2013;347:f6070.
Ek K, Ternestedt B-M. Living with chronic obstructive pulmonary disease at the end of life: a phenomenological study. J Adv Nurs. 2008;62:470–8.
Steinhauser KE, Voils CI, Clipp EC, Bosworth HB, Christakis NA, Tulsky JA. Are you at peace? One item to probe spiritual concerns at the end of life. Arch Intern Med. 2006;166:101–5.
Curtis JR. Palliative and end-of-life care for patients with severe COPD. Eur Respir J. 2008;32:796–803.
Knauft E, Nielsen EL, Engelberg RA, Patrick DL, Curtis JR. Barriers and facilitators to end-of-life care communication for patients with COPD. Chest. 2005;127:2188–96.
Back AL, Arnold RM, Quill TE. Hope for the best, and prepare for the worst. Ann Intern Med. 2003;138:439–43.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
VD and HP declare that they have no conflicts of interest.
Funding
No funding was received for this review.
Rights and permissions
About this article
Cite this article
Dalgliesh, V., Pinnock, H. Pharmacological Management of People Living with End-Stage Chronic Obstructive Pulmonary Disease. Drugs Aging 34, 241–253 (2017). https://doi.org/10.1007/s40266-017-0440-3
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40266-017-0440-3