Abstract
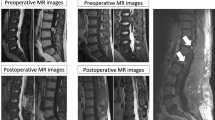
Spinal paragangliomas are extremely rare tumors, most frequently involving the cauda equina and the filum terminale. We aimed to investigate the clinical manifestations, radiological features, management, and follow-up data of primary spinal paraganglioma. We present the clinical data and long-term outcomes from a consecutive surgical series of 19 patients with pathologically diagnosed spinal paragangliomas. All of the patients had undergone surgical resection. Pre- and postoperative magnetic resonance imaging was performed and follow-up data and neurological functional assessment are presented and discussed. The mean age at diagnosis was 47.7 years, with a significant male predominance. The primary clinical symptoms were low back pain and sciatica. Magnetic resonance images (MRI) showed characteristic signs that help differentiate paragangliomas from other spinal tumors, including a “salt & pepper” sign, serpiginous flow void, and a peripheral hypointense rim. Also, a well-encapsulated appearance can be found intraoperatively. During a mean follow-up period of 62.1 months, remnant tumor progression was noted on MRI in three patients with incomplete resection. Pain symptoms were relieved immediately after surgical intervention, while motor and sphincter dysfunction were much slower to improve. Differential diagnosis of paraganglioma based on MR images alone is challenging, but the presence of specific characteristic features provides suggestive clues; however, accurate diagnosis depends on pathological criteria. Despite the benign course, gross total resection is ideal, given an increased risk of recurrence in situ. Timely recognition and surgical treatment should be emphasized to avoid progressive neurological deficits.



Similar content being viewed by others
References
Caruso R, Wierzbicki V, Marrocco L, Salvati M (2006) Paragangliomas of the cauda equina. Report of one case and review of the literature. J Exp Clin Cancer Res 25:269–275
Moran CA, Rush W, Mena H (1997) Primary spinal paragangliomas: a clinicopathological and immunohistochemical study of 30 cases. Histopathology 31:167–173
Yang SY, Jin YJ, Park SH, Jahng TA, Kim HJ, Chung CK (2005) Paragangliomas in the cauda equina region: clinicopathoradiologic findings in four cases. J Neurooncol 72:49–55
Conti P, Mouchaty H, Spacca B, Buccoliero AM, Conti R (2006) Thoracic extradural paragangliomas: a case report and review of the literature. Spinal Cord 44:120–125
Sundgren P, Annertz M, Englund E, Stromblad LG, Holtas S (1999) Paragangliomas of the spinal canal. Neuroradiology 41:788–794
Lerman RI, Kaplan ES, Daman L (1972) Ganglioneuroma-paraganglioma of the intradural filum terminale. Case report. J Neurosurg 36:652–658
Nakamura M, Miyamoto K, Shimizu K (2009) Difference in evaluation of patients with low back pain using the Japanese Orthopaedic Association Score for Back Pain and the Japanese Version of the Roland-Morris Disability Questionnaire. J Orthop Sci 14:367–373
Ohtori S, Ito T, Yamashita M et al (2010) Evaluation of low back pain using the Japanese Orthopaedic Association Back Pain Evaluation Questionnaire for lumbar spinal disease in a multicenter study: differences in scores based on age, sex, and type of disease. J Orthop Sci 15:86–91
Jeffs GJ, Lee GY, Wong GT (2003) Functioning paraganglioma of the thoracic spine: case report. Neurosurgery 53:992–994; discussion 994–995
Chen G, Luo Z, Liu T, Yang H (2011) Functioning paraganglioma of the cervical spine. Orthopedics 34:e700–e702
Destito D, Bucolo S, Florio A, Quattrocchi C (2012) Management of head and neck paragangliomas: a series of 9 cases and review of the literature. Ear Nose Throat J 91:366–375
Sonneland PR, Scheithauer BW, LeChago J, Crawford BG, Onofrio BM (1986) Paraganglioma of the cauda equina region. Clinicopathologic study of 31 cases with special reference to immunocytology and ultrastructure. Cancer 58:1720–1735
Lee KY, Oh YW, Noh HJ et al (2006) Extraadrenal paragangliomas of the body: imaging features. AJR Am J Roentgenol 187:492–504
Demircivi OF, Aydin M, Bezircioglu H, Oran I (2010) Paraganglioma of the cauda equina: a highly vascular tumour. J Clin Neurosci 17:1445–1447
Hong JY, Hur CY, Modi HN, Suh SW, Chang HY (2012) Paraganglioma in the cauda equina. A case report. Acta Orthop Belg 78:418–423
North CA, Zinreich ES, Christensen WN, North RB (1990) Multiple spinal metastases from paraganglioma. Cancer 66:2224–2228
Lau D, La Marca F, Camelo-Piragua S, Park P (2013) Metastatic paraganglioma of the spine: case report and review of the literature. Clin Neurol Neurosurg 115:1571–1574
Hamilton MA, Tait D (2000) Metastatic paraganglioma causing spinal cord compression. Br J Radiol 73:901–904
Lehmen JA, Babbel DM, Mikhitarian K, Choma TJ (2010) Paraganglioma presenting as metastatic lesion in a cervical vertebra: a case report and review of the literature. Spine (Phila Pa 1976) 35:E152–154
Makiese O, Chibbaro S, Marsella M, Tran BHP, George B (2012) Jugular foramen paragangliomas: management, outcome and avoidance of complications in a series of 75 cases. Neurosurg Rev 35:185–194; discussion 194
Fitzgerald LF, Cech DA, Goodman JC (1996) Paraganglioma of the thoracic spinal cord. Clin Neurol Neurosurg 98:183–185
Amato B, Bianco T, Compagna R et al (2014) Surgical resection of carotid body paragangliomas: 10 years of experience. Am J Surg 207:293–298
van Heerden JA, Roland CF, Carney JA, Sheps SG, Grant CS (1990) Long-term evaluation following resection of apparently benign pheochromocytoma(s)/paraganglioma(s). World J Surg 14:325–329
Tran BHP (2014) Radiotherapy for glomus jugulare paraganglioma. Eur Ann Otorhinolaryngol Head Neck Dis 131:223–226
Dupin C, Lang P, Dessard-Diana B et al (2014) Treatment of head and neck paragangliomas with external beam radiation therapy. Int J Radiat Oncol Biol Phys 89:353–359
Kiziltan HS, Ozucer B, Eris AH, Veyseller B (2014) Bilateral carotid paraganglioma: surgery and radiotherapy. Clin Med Insights Case Rep 7:53–57
Navarro MA, Maitz A, Grills IS et al (2010) Successful treatment of glomus jugulare tumours with gamma knife radiosurgery: clinical and physical aspects of management and review of the literature. Clin Transl Oncol 12:55–62
Niemeijer ND, Alblas G, van Hulsteijn LT, Dekkers OM, Corssmit EP (2014) Chemotherapy with cyclophosphamide, vincristine and dacarbazine for malignant paraganglioma and pheochromocytoma: systematic review and meta-analysis. Clin Endocrinol (Oxf) 81:642–651
Li ZJ, Lan XL, Hao FY et al (2014) Primary cerebellar paraganglioma: a pediatric case report and review of the literature. Pediatr Neurol 50:303–306
Suarez C, Rodrigo JP, Mendenhall WM et al (2014) Carotid body paragangliomas: a systematic study on management with surgery and radiotherapy. Eur Arch Otorhinolaryngol 271:23–34
Acknowledgments
We thank all of the patients who trusted us with their care, and all of the physicians and staff who helped in this study.
Compliance with Ethical Standards
The authors declare that they have no conflict of interest. All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. Informed consent was obtained from all individual participants included in the study.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Yang, C., Li, G., Fang, J. et al. Clinical characteristics and surgical outcomes of primary spinal paragangliomas. J Neurooncol 122, 539–547 (2015). https://doi.org/10.1007/s11060-015-1742-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11060-015-1742-0