Abstract
Aim
Preclinical studies suggested that insulin, incretin and thiazolidinediones had effect on regulation of bone metabolism. But clinical evidence is limited. We assessed the effects of these antihyperglycemic agents on bone metabolism in patients with newly diagnosed type 2 diabetes.
Methods
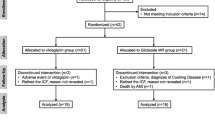
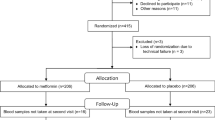
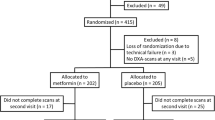
The present study was a two-center, randomized, parallel-group clinical trial. Sixty-two newly diagnosed and drug-naïve patients with type 2 diabetes were randomized to exenatide (EXE, n = 20), mixed protamine zinc recombinant human insulin lispro injection (25R; INS, n = 21) or pioglitazone (PIO, n = 21) group for a 24-week treatment. Glycosylated hemoglobin A1c (HbA1c), body weight, body mineral density (BMD) and fasting serum concentration of bone turnover markers including osteocalcin (OC), C-telopeptide of type I collagen (CTX) and tartrate-resistant alkaline phosphatase 5b (TRAcP5b) were assessed at baseline and week 24.
Results
Baseline characteristics were similar among groups. At week 24, HbA1c improved in all patients (EXE:−2.4 ± 0.3 %, INS:−2.4 ± 0.3 %, PIO:−2.0 ± 0.2 %; p > 0.05 among groups). Patients treated with exenatide lost body weight remarkably (−4.7 ± 0.8 kg). In spite of the amelioration of glucose control, no significant improvement of OC, CTX or TRAcP5b was observed at week 24 (EXE: OC −0.619 ± 0.728 ng/ml, CTX 0.147 ± 0.046 ng/ml, TRAcP5b 0.302 ± 0.149 U/L;INS: OC 0.637 ± 0.787 ng/ml, CTX −0.012 ± 0.074 ng/ml, TRAcP5b 0.124 ± 0.395 U/L; PIO: OC −0.150 ± 0.691 ng/ml, CTX 0.073 ± 0.094 ng/ml, TRAcP5b 0.586 ± 0.183 U/L; p > 0.05), as well as BMD measurement, regardless of the treatments.
Conclusions
Twenty-four-week treatment with exenatide, insulin and pioglitazone improved glucose control in patients with newly diagnosed type 2 diabetes, but had no impact on bone turnover markers or BMD.
Similar content being viewed by others
References
de Liefde II, van der Klift M, de Laet CE, van Daele PL, Hofman A, Pols HA (2005) Bone mineral density and fracture risk in type-2 diabetes mellitus: the Rotterdam study. Osteoporos Int 16:1713–1720
Vestergaard P (2007) Discrepancies in bone mineral density and fracture risk in patients with type 1 and type 2 diabetes—a meta-analysis. Osteoporos Int 18:427–444
Hamilton EJ, Rakic V, Davis WA, Paul Chubb SA, Kamber N, Prince RL, Davis TME (2012) A five-year prospective study of bone mineral density in men and women with diabetes: the fremantle diabetes study. Acta Diabetol 49:153–158
Saller A, Maggi S, Romanato G, Tonin P, Crepaldi G (2008) Diabetes and osteoporosis. Aging Clin Exp Res 20:280–289
Maggi S, Siviero P, Brocco E, Albertin M, Romanato G, Crepaldi G (2014) Vitamin D deficiency, serum leptin and osteoprotegerin levels in older diabetic patients: an input to new research avenues. Acta Diabetol 51:461–469
Khazai NB, Beck GR Jr, Umpierrez GE (2009) Diabetes and fractures: an overshadowed association. Curr Opin Endocrinol Diabetes Obes 16:435–445
Clowes JA, Allen HC, Prentis DM, Eastell R, Blumsohn A (2003) Octreotide abolishes the acute decrease in bone turnover in response to oral glucose. J Clin Endocrinol Metab 88:4867–4873
Ferron M, Wei J, Yoshizawa T, Del Fattore A, DePinho RA, Teti A, Ducy P, Karsenty G (2010) Insulin signaling in o Guillermo E. Umpierrez, osteoblasts integrates bone remodeling and energy metabolism. Cell 142:296–308
Asmar M, Holst JJ (2010) Glucagon-like peptide 1 and glucose-dependent insulinotropic polypeptide: new advances. Curr Opin Endocrinol Diabetes Obes 17:57–62
Wei W, Wan Y (2011) Thiazolidinediones on PPARgamma: the roles in bone remodeling. PPAR Res 2011:867180
Xu W, Bi Y, Sun Z, Li J, Guo L, Yang T, Wu G, Shi L, Feng Z, Qiu L, Li Q, Guo X, Luo Z, Lu J, Shan Z, Yang W, Ji Q, Yan L, Li H, Yu X, Li S, Zhou Z, Lv X, Liang Z, Lin S, Zeng L, Yan J, Ji L, Weng J (2015) Comparison of the effects on glycaemic control and b-cell function in newly diagnosed type 2 diabetes patients of treatment with exenatide, insulin or pioglitazone: a multicenter randomized parallel-group trial (the confidence study). J Intern Med 277:137–150
Bunck MC, Diamant M, Cornér A, Eliasson B, Malloy JL, Shaginian RM, Deng W, Kendall DM, Taskinen MR, Smith U, Yki-Järvinen H, Heine RJ (2009) One-year treatment with exenatide improves beta-cell function, compared with insulin glargine, in metformin-treated type 2 diabetic patients: a randomized, controlled trial. Diabetes Care 32:762–768
Meloni AR, DeYoung MB, Han J, Best JH, Grimm M (2013) Treatment of patients with type 2 diabetes with exenatide once weekly versus oral glucose-lowering medications or insulin glargine: achievement of glycemic and cardiovascular goals. Cardiovasc Diabetol 12:48
Russell-Jones D, Cuddihy RM, Hanefeld M, Kumar A, González JG, Chan M, Wolka AM, Boardman MK, DURATION-4 Study Group (2012) Efficacy and safety of exenatide once weekly versus metformin, pioglitazone, and sitagliptin used as monotherapy in drug-naive patients with type 2 diabetes (DURATION-4): a 26-week double-blind study. Diabetes Care 35:252–258
Reyes-García R, Rozas-Moreno P, López-Gallardo G, García-Martín A, Varsavsky M, Avilés-Perez MD, Muñoz-Torres M (2013) Serum levels of bone resorption markers are decreased in patients with type 2 diabetes. Acta Diabetol 50:47–52
Gerdhem P, Isaksson A, Akesson K, Obrant KJ (2005) Increased bone density and decreased bone turnover, but no evident alteration of fracture susceptibility in elderly women with diabetes mellitus. Osteoporos Int 16:1506–1512
Rosato MT, Schneider SH, Shapses SA (1998) Bone turnover and insulin-like growth factor I levels increase after improved glycemic control in noninsulin-dependent diabetes mellitus. Calcif Tissue Int 63:107–111
Okazaki R, Totsuka Y, Hamano K, Ajima M, Miura M, Hirota Y, Hata K, Fukumoto S, Matsumoto T (1997) Metabolic improvement of poorly controlled noninsulin-dependent diabetes mellitus decreases bone turnover. J Clin Endocrinol Metab 82:2915–2920
Kanazawa I, Yamaguchi T, Yamauchi M, Yamamoto M, Kurioka S, Yano S, Sugimoto T (2009) Adiponectin is associated with changes in bone markers during glycemic control in type 2 diabetes mellitus. J Clin Endocrinol Metab 94:3031–3037
Kindblom JM, Ohlsson C, Ljunggren O, Karlsson MK, Tivesten A, Smith U, Mellstrom D (2009) Plasma osteocalcin is inversely related to fat mass and plasma glucose in elderly Swedish men. J Bone Miner Res 24:785–791
Im JA, Yu BP, Jeon JY, Kim SH (2008) Relationship between osteocalcin and glucose metabolism in postmenopausal women. Clin Chim Acta 396:66–69
Kanazawa I, Yamaguchi T, Yamamoto M, Yamauchi M, Kurioka S, Yano S, Sugimoto T (2009) Serum osteocalcin level is associated with glucose metabolism and atherosclerosis parameters in type 2 diabetes mellitus. J Clin Endocrinol Metab 94:45–49
Kanazawa I, Yamaguchi T, Yamauchi M, Yamamoto M, Kurioka S, Yano S, Sugimoto T (2010) Serum undercarboxylated osteocalcin was inversely associated with plasma glucose level and fat mass in type 2 diabetes mellitus. Osteoporos Int 22:187–194
Sayinalp S, Gedik O, Koray Z (1995) Increasing serum osteocalcin after glycemic control in diabetic men. Calcif Tissue Int 57:422–425
Gregorio F, Cristallini S, Santeusanio F, Filipponi P, Fumelli P (1994) Osteopenia associated with non-insulin-dependent diabetes mellitus: what are the causes? Diabetes Res Clin Pract 23:43–54
Hong SH, Koo JW, Hwang JK, Hwang YC, Jeong IK, Ahn KJ, Chung HY, Kim DY (2013) Changes in serum osteocalcin are not associated with changes in glucose or insulin for osteoporotic patients treated with bisphosphonate. J Bone Metab 20:37–41
Poomthavorn P, Nantarakchaikul P, Mahachoklertwattana P, Chailurkit LO, Khlairit P (2014) Effects of correction of vitamin D insufficiency on serum osteocalcin and glucose metabolism in obese children. Clin Endocrinol (Oxf) 80:516–523
Finkelstein JS, Sowers M, Greendale GA, Lee ML, Neer RM, Cauley JA, Ettinger B (2003) Ethnic variation in bone turnover in pre- and early perimenopausal women: effects of anthropometric and lifestyle factors. J Clin Endocrinol Metab 87:3051–3056
Nuche-Berenguer B, Portal-Núñez S, Moreno P, González N, Acitores A, López-Herradón A, Esbrit P, Valverde I, Villanueva-Peñacarrillo ML (2010) Presence of a functional receotpr for GLP-1 in osteoblastic cells, independent of the cAMP-linked GLP-1 receptor. J Cell Physiol 225:585–592
Ng KW (2011) Regulation of glucose metabolism and the skeleton. Clin Endocrinol (Oxford) 75:147–155
Nuche-Berenguer B, Moreno P, Esbrit P, Dapía S, Caeiro JR, Cancelas J, Haro-Mora JJ, Villanueva-Peñacarrillo ML (2009) Effect of GLP-1 treatment on bone turnover in normal, type 2 diabetic, and insulin-resistant states. Calcif Tissue Int 84:453–461
Nuche-Berenguer B, Moreno P, Portal-Nuñez S, Dapía S, Esbrit P, Villanueva-Peñacarrillo ML (2010) Exendin-4 exerts osteogenic actions in insulin-resistant and type 2 diabetic states. Regul Pept 159:61–66
Bunck MC, Eliasson B, Cornér A, Heine RJ, Shaginian RM, Taskinen MR, Yki-Järvinen H, Smith U, Diamant M (2011) Exenatide treatment did not affect bone mineral density despite body weight reduction in patients with type 2 diabetes. Diabetes Obes Metab 13:374–377
Bunck MC, Poelma M, Eekhoff EM, Schweizer A, Heine RJ, Nijpels G, Foley JE, Diamant M (2012) Effects of Vildagliptin on postprandial markers of bone resorption and calcium homeostasis in recently diagnosed, well-controlled, type 2 diabetes patients. J Diabetes 4:181–185
Garnero P (2008) Biomarkers for osteoporosis management: utility in diagnosis, fracture risk prediction and therapy monitoring. Mol Diagn Ther 12:157–170
Jensen LB, Kollerup G, Quaade F, Sørensen OH (2001) Bone mineral changes in obese women during a moderate weight loss with and without calcium supplementation. J Bone Miner Res 16:141–147
Riedt CS, Cifuentes M, Stahl T, Chowdhury HA, Schlussel Y, Shapses SA (2005) Overweight postmenopausal women lose bone with moderate weight eduction and 1 g/day calcium intake. J Bone Miner Res 20:455–463
Carrasco F, Ruz M, Rojas P, Csendes A, Rebolledo A, Codoceo J, Inostroza J, Basfi-Fer K, Papapietro K, Rojas J, Pizarro F, Olivares M (2009) Changes in bone mineral density, body composition and adiponectin levels in morbidly obese patients after bariatric surgery. Obes Surg 19:41–46
Holecki M, Zahorska-Markiewicz B, Chudek J, Wiecek A (2010) Changes in bone mineral density and bone turnover markers in obese women after short-term weight loss therapy during a 5-year follow-up. Pol Arch Med Wewn 120:248–254
Yamada C, Yamada Y, Tsukiyama K, Yamada K, Udagawa N, Takahashi N, Tanaka K, Drucker DJ, Seino Y, Inagaki N (2008) The murine glucagonlike peptide-1 receptor is essential for control of bone resorption. Endocrinology 149:574–579
Antonopoulou M, Bahtiyar G, Banerji MA, Sacerdote AS (2013) Diabetes and bone health. Maturitas 76:253–259
Waser B, Beetschen K, Pellegata NS, Reubi JC (2011) Incretin receptors in non-neoplastic and neoplastic thyroid C cells in rodents and humans: relevance for incretin-based diabetes therapy. Neuroendocrinology 94:291–301
Gier B, Butler PC, Lai CK, Kirakossian D, DeNicola MM, Yeh MW (2012) Glucagon like peptide-1 receptor expression in the human thyroid gland. J Clin Endocrinol Metab 97:121–131
Lecka-Czernik B (2010) Bone loss in diabetes: use of antidiabetic thiazolidinediones and secondary osteoporosis. Curr Osteoporos Rep 8:178–184
Dormuth CR, Carney G, Carleton B, Bassett K, Wright JM (2009) Thiazolidinediones and fractures in men and women [J]. Arch Intern Med 169:1395–1402
Meier C, Kraenzlin ME, Bodmer M, Jick SS, Jick H, Meier CR (2008) Use of thiazolidinediones and fracture risk. Arch Intern Med 168:820–825
Motyl KJ, McCabe LR, Schwartz AV (2010) Bone and glucose metabolism: a two-way street. Arch Biochem Bioph 503:2–10
Acknowledgments
The authors would like to thank all the participating patients in the study. This study was supported by the Key Clinical Project from the Ministry of Health of China and investigator-initiated trial research funds from Eli Lilly and Co. and Amylin Pharmaceuticals, Inc. The sponsors had no role in the study design, collection, analysis and interpretation of data, or writing the report.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All the authors declare that they have no conflict of interest.
Ethical standard
The study protocol has been reviewed by the ethics committee of the Third Affiliated Hospital of Sun Yat-sen University and Drum Tower Hospital Affiliated to Nanjing University Medical School, and have therefore been performed in accordance with the ethical standards laid down in an appropriate version of the 1964 Declaration of Helsinki.
Human and animal rights
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1975, as revised in 2008 (5).
Informed consent
Informed consent was obtained from all patients for being included in the study.
Additional information
Managed by Antonio Secchi.
Renyuan Li, Wen Xu and Sihui Luo have contributed equally to this work.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Li, R., Xu, W., Luo, S. et al. Effect of exenatide, insulin and pioglitazone on bone metabolism in patients with newly diagnosed type 2 diabetes. Acta Diabetol 52, 1083–1091 (2015). https://doi.org/10.1007/s00592-015-0792-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00592-015-0792-2