Abstract
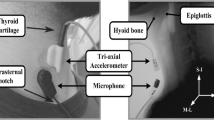
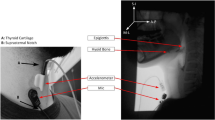
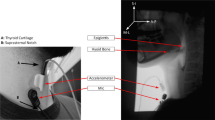
Spontaneous swallowing is considered a reflexive, pharyngeal clearance mechanism. Reductions in spontaneous swallow frequency may be a sensitive index for dysphagia and related morbidities. This study evaluated an acoustic recording technique as a measure to estimate spontaneous swallow frequency. Initially, a multichannel physiologic (surface electromyography, swallow apnea, cervical auscultation) recording technique was validated and subsequently compared to an isolated acoustic (microphone) recording technique on a sample of younger (25 ± 2.8 years) and older (68 ± 5.3 years) healthy adult participants. Sensitivity (94 %), specificity (99 %), and classification accuracy (98 %) were high for swallow identification from the multichannel physiologic recording technique. Interjudge reliability was high (k = 0.94, 95 % CI = 0.92–0.96). No significant differences in spontaneous swallow frequency were observed between the multichannel physiologic recordings and the acoustic recordings (0.85 vs. 0.81 swallows per minute). Furthermore, these two techniques were highly correlated (r = 0.95). Interjudge reliability for swallow identification via acoustic recordings was high (k = 0.96, 95 % CI = 0.94–0.99). Preliminary evaluation of the temporal stability of spontaneous swallow frequency measured from acoustic recordings indicated that time samples as short as 5 min produce viable results. Age differences were identified in spontaneous swallow frequency rates, with older participants swallowing less frequently than younger participants (0.47 vs. 1.02 swallows per minute). Collectively, these results indicate that an isolated acoustic recording technique is a valid approach to estimate spontaneous swallow frequency.



Similar content being viewed by others
References
Dua K, Surapaneni SN, Kuribayashi S, Hafeezullah M, Shaker R. Pharyngeal airway protective reflexes are triggered before the maximum of volume of fluid that the hypopharynx can safely hold is exceeded. Am J Physiol Gastrointest Liver Physiol. 2001;301:G197–202.
Dua K, Surapaneni SN, Kuribayashi S, Haffeezullah M, Shaker R. Protective role of aerodigestive reflexes against aspiration: study on subjects with impaired and preserved reflexes. Gastroenterology. 2011;140:1927–33.
Shaker R, Ren J, Bardan E, Easterline C, Dua K, Xie P, Kern M. Pharyngoglottal closure reflex: characterization in healthy young, elderly and dysphagic patients with predeglutitive aspiration. Gerontology. 2003;49:12–20.
Shaker R, Hogan WJ. Reflex-mediated enhancement of airway protective mechanisms. Am J Med. 2000;108(Suppl 4a):8s–14s.
Shaker R. Airway protective mechanisms: current concepts. Dysphagia. 1995;10:16–27.
Murray J, Langmore SE, Ginsberg S, Dostie A. The significance of accumulated oropharyngeal secretions and swallowing frequency in predicting aspiration. Dysphagia. 1996;11:99–103.
Bredenoord AJ, Weusten BL, Samsom M, Smout AJ. Air swallowing, belching and reflux in patients with gastroesohageal reflux disease. Am J Gastroenterol. 2006;101:1721–6.
Conchillo JM, Selimah M, Bredenoord AJ, Timmer R, Smout AJ. Air swallowing, belching, acid and non-acid reflux in patients with functional dyspepsia. Aliment Pharmacol Ther. 2007;25:965–71.
Hemmink GJ, Weusten BL, Bredenoord AJ, Samsom M, Smout AJ. Increased swallowing frequency in GORD is likely to be caused by perception of reflux episodes. Neurogastroenterol Motil. 2009;21:143–8.
Pehlivan M, Yüceyar N, Ertekin C, et al. An electronic device measuring the frequency of spontaneous swallowing; digital phagometer. Dysphagia. 1996;11:259–64.
Leslie P, Drinnan MJ, Ford GA, Wilson JA. Swallowing respiratory patterns and aging: presbyphagia or dysphagia. J Gerontol A Biol Sci Med Sci. 2005;60:391–5.
Hinchey JA, Shephard T, Furie K, Smith D, Wang D. Stroke Practice Improvement Network Investigators. Formal dysphagia screening protocols prevent pneumonia. Stroke. 2005;36:1972–6.
Carnaby G, Hankey GJ, Pizzi J. Behavioural intervention for dysphagia in acute stroke: a randomised controlled trial. Lancet Neurol. 2006;5:31–7.
Elmstahl S, Bulow M, Ekberg O, Peterson M, Tegner H. Treatment of dysphagia improves nutritional conditions in stroke patients. Dysphagia. 1999;14:61–6.
Teasell R, Foley N, Martino R, Bhogal S, Speechley M. Dysphagia and aspiration after stroke: evidence-based review of stroke rehabilitation (EBRSR). Updated Aug 2010. www.ebsr.com. Accessed 6 Sept 2011.
Crary MA, Carnaby (Mann) GD, Groher ME. Biomechanical correlates of sEMG signals obtained during swallowing by healthy adults. J Speech Lang Hear Res. 2006;49:1–8.
Takahashi K, Groher ME, Michi K. Methodology for detecting swallowing sounds. Dysphagia. 1994;9:54–62.
Takahashi K, Groher ME, Michi K. Symmetry and reproducibility of swallowing sounds. Dysphagia. 1994;9:168–73.
Moriniére S, Boiron M, Alison D, Makris P, Beutter P. Origin of the sound components during pharyngeal swallowing in normal subjects. Dysphagia. 2008;23:267–73.
Cichero JA, Murdoch BE. Acoustic signature of the normal swallow: characterization by age, gender, and bolus volume. Ann Otol Rhinol Laryngol. 2002;111:623–32.
Youmans SR, Stierwalt JA. An acoustic profile of normal swallowing. Dysphagia. 2005;20:195–209.
Afkari S. Measuring frequency of spontaneous swallowing. Australas Phys Eng Sci Med. 2007;30:313–7.
Aboofazeli M, Moussavi Z. Automated classification of swallowing and breath sounds. Conf Proc IEEE Eng Med Biol Soc. 2004;5:3816–9.
Lazareck LJ, Moussavi ZM. Classification of normal and dysphagia swallows by acoustical means. IEEE Trans Biomed Eng. 2004;51:2103–12.
Santamato A, Panza F, Solfrizzi V, Russo A, Frisardi V, Megna M, Ranieri M, Fiore P. Acoustic analysis of swallowing sounds: a new technique for assessing dysphagia. J Rehabil Med. 2009;41:639–45.
Cichero J, Murdoch B. Detection of swallowing sounds: methodology revisited. Dysphagia. 2002;17:40–9.
Reynolds E, Vice F, Gewolb I. Variability of swallow-associated sounds in adults and infants. Dysphagia. 2009;24:13–9.
Aboofazeli M, Moussavi Z. Analysis of swallowing sounds using hidden Markov models. Med Biol Eng Comput. 2008;46:307–14.
South A, Somers SM, Jog MS. Gum chewing improves swallow frequency and latency in Parkinson patients: a preliminary study. Neurology. 2010;74:1198–202.
Crary MA, Carnaby-Mann GD, Groher ME. Identification of swallowing events from sEMG signals obtained from healthy adults. Dysphagia. 2007;22:94–9.
Lear CSC, Flanagan JB, Moorrees CFA. The frequency of deglutition in man. Arch Oral Biol. 1965;10:83–99.
Theurer J, Czachorowski KA, Martin LP, Martin RE. Effects of oropharyngeal air-pulse stimulation on swallowing in healthy older adults. Dysphagia. 2009;24:302–13.
Kapila YV, Dodds WJ, Helm JF, Hogan WJ. Relationship between swallow rate and salivary flow. Dig Dis Sci. 1984;29:528–33.
Theurer JA, Bihari F, Barr AM, Martin RE. Oropharyngeal stimulation with air-pulse trains increases swallow frequency in healthy adults. Dysphagia. 2005;20:254–60.
Cabre M, Serra-Prat M, Palomera E, Almirall J, Pallares R, Clavé P. Prevalence and prognostic implications of dysphagia in elderly patients with pneumonia. Age Ageing. 2010;39:39–45.
Rudney JD, Ji Z, Larson CJ. The prediction of saliva swallowing frequency in humans from estimates of salivary flow rate and the volume of saliva swallowed. Arch Oral Biol. 1995;40:507–12.
Vaiman M, Nahlieli O, Segal S, Eviatar E. Electromyography monitoring of patients with salivary gland diseases. Otolaryngol Head Neck Surg. 2005;133:869–73.
Conflict of interest
M. Crary, L. Sura, and G. D. Carnaby have no conflicts of interest to disclose.
Author information
Authors and Affiliations
Corresponding author
Additional information
Data collection and analysis at the Swallowing Research Laboratory, University of Florida Health Science Center.
Rights and permissions
About this article
Cite this article
Crary, M.A., Sura, L. & Carnaby, G. Validation and Demonstration of an Isolated Acoustic Recording Technique to Estimate Spontaneous Swallow Frequency. Dysphagia 28, 86–94 (2013). https://doi.org/10.1007/s00455-012-9416-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00455-012-9416-y