Abstract
Background
A previous study has demonstrated that symptoms suggestive of dumping syndrome appear after a provocation test early after laparoscopic sleeve gastrectomy (LSG) in 45 % of patients, and these are mainly related to early dumping. The aim of this study is to evaluate the evolution of dumping symptoms during the first postoperative year.
Methods
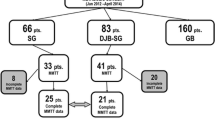
Twenty-five non-diabetic morbidly obese patients (6 male, 19 female) were evaluated with an oral glucose tolerance test (OGTT) preoperatively, at 6 weeks and at 6 months postoperatively. In addition, 12 of them repeated the OGTT at 12 months after LSG. Sigstad score was used to separate dumpers from non-dumpers and Arts’ questionnaire to differentiate between early and late dumping. Insulin and glucose levels were also measured.
Results
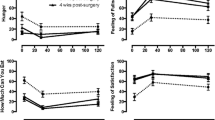
Sigstad score remained significantly elevated at 6 and 12 months postoperatively compared to preoperative values. Symptoms suggestive of dumping syndrome were recorded in 40 % of patients at 6 months and in 33 % at 12 months postoperatively. Arts’ questionnaire demonstrated that early dumping score remained higher compared to baseline at 6 and 12 months postoperatively. Late dumping scores increased gradually during the time and that difference was statistically significant at 12 months after LSG. Hypoglycaemia occurred at 33 % of patients both at 6 and 12 months postoperatively.
Conclusions
Symptoms suggestive of dumping syndrome after provocation still exist at 6 and 12 months in a significant proportion of patients after LSG and include both early and late dumping. These findings are consistent with the high incidence of hypoglycaemia after OGTT at 6 and 12 months after LSG.


Similar content being viewed by others
References
Tack J, Arts J, Caenepeel P, et al. Pathophysiology, diagnosis and management of postoperative dumping syndrome. Nat Rev Gastroenterol Hepatol. 2009;6:583–90.
Vecht J, Masclee AAM, Lamers CBHW. The dumping syndrome. Current insights into pathophysiology, diagnosis and treatment. Scand J Gastroenterol Suppl. 1997;223:21–7.
Ukleja A. Dumping syndrome: pathophysiology and treatment. Nutr Clin Pract. 2005;20:517–25.
Olbers T, Björkman S, Lindroos A, et al. Body composition, dietary intake, and energy expenditure after laparoscopic Roux-en-Y gastric bypass and laparoscopic vertical banded gastroplasty: a randomized clinical trial. Ann Surg. 2006;244:715–22.
Kenler HA, Brolin RE, Cody RP. Changes in eating behavior after horizontal gastroplasty and Roux-en-Y gastric bypass. Am J Clin Nutr. 1990;52:87–92.
Zukin P, Weiner I. Psychological factors in the dumping syndrome. J Nerv Ment Dis. 1960;130:426–7.
Hobsley M. Dumping and diarrhoea. Br J Surg. 1981;68:681–4.
Melissas J, Koukouraki S, Askoxylakis J, et al. Sleeve gastrectomy: a restrictive procedure? Obes Surg. 2007;17:57–62.
Melissas J, Daskalakis M, Koukouraki S, et al. Sleeve gastrectomy—a “food limiting” operation. Obes Surg. 2008;18:1251–6.
Karamanakos SN, Vagenas K, Kalfarentzos F, et al. Weight loss, appetite suppression, and changes in fasting and postprandial ghrelin and peptide-YY levels after Roux-en-Y gastric bypass and sleeve gastrectomy: a prospective, double blind study. Ann Surg. 2008;247:401–7.
Peterli R, Wölnerhanssen B, Peters T, et al. Improvement in glucose metabolism after bariatric surgery: comparison of laparoscopic Rouxen-Y gastric bypass and laparoscopic sleeve gastrectomy: a prospective randomized trial. Ann Surg. 2009;250:234–41.
Valderas JP, Irribarra V, Boza C, et al. Medical and surgical treatments for obesity have opposite effects on peptide YY and appetite: a prospective study controlled for weight loss. J Clin Endocrinol Metab. 2010;95:1069–75.
Baumann T, Kuesters S, Grueneberger J, et al. Time-resolved MRI after ingestion of liquids reveals motility changes after laparoscopic sleeve gastrectomy—preliminary results. Obes Surg. 2011;21:95–101.
Braghetto I, Davanzo C, Korn O, et al. Scintigraphic evaluation of gastric emptying in obese patients submitted to sleeve gastrectomy compared to normal subjects. Obes Surg. 2009;19:1515–21.
Tzovaras G, Papamargaritis D, Sioka E, et al. Symptoms suggestive of dumping syndrome after provocation in patients after laparoscopic sleeve gastrectomy. Obes Surg. 2012;22:23–8.
Triantafyllidis G, Lazoura O, Sioka E, et al. Anatomy and complications following laparoscopic sleeve gastrectomy: radiological evaluation and imaging pitfalls. Obes Surg. 2011;21:473–8.
Sigstad H. A clinical diagnostic index in the diagnosis of the dumping syndrome. Changes in plasma volume and blood sugar after a test meal. Acta Med Scand. 1970;188:479–86.
Arts J, Caenepeel P, Bisschops R, et al. Efficacy of the long-acting repeatable formulation of the somatostatin analogue octreotide in postoperative dumping. Clin Gastroenterol Hepatol. 2009;7:432–7.
[No authors listed]. 1983 metropolitan height and weight tables. Stat Bull Metrop Life Found. 1983;64:3–9.
Deitel M. The change in the dumping syndrome concept. Obes Surg. 2008;18:1622–4.
Himpens J, Dapri G, Cadière GB. A prospective randomized study between laparoscopic gastric banding and laparoscopic isolated sleeve gastrectomy: results after 1 and 3 years. Obes Surg. 2011;16:1450–6.
Kafri N, Valfer R, Nativ O, et al. Hazzan D Health behavior, food tolerance, and satisfaction after laparoscopic sleeve gastrectomy. Surg Obes Relat Dis. 2011;7:82–8.
Wilson-Pérez HE, Chambers AP, Sandoval DA, Stefater MA, Woods SC, Benoit SC, Seeley RJ. The effect of vertical sleeve gastrectomy on food choice in rats. Int J Obes (Lond). 2012. doi:10.1038/ijo.2012.18.
Yehoshua RT, Eidelman LA, Stein M, et al. Laparoscopic sleeve gastrectomy—volume and pressure assessment. Obes Surg. 2008;18:1083–8.
Yamashita Y, Toge T, Adrian TE. Gastrointestinal hormone in dumping syndrome and reflux esophagitis after gastric surgery. J Smooth Muscle Res. 1997;33:37–48.
Valderas JP, Irribarra V, Rubio L, et al. Effects of sleeve gastrectomy and medical treatment for obesity on glucagon-like peptide 1 levels and glucose homeostasis in non-diabetic subjects. Obes Surg. 2011;21:902–9.
Peterli R, Steinert RE, Woelnerhanssen B, et al. Metabolic and hormonal changes after laparoscopic Roux-en-Y gastric bypass and sleeve gastrectomy: a randomized, prospective trial. Obes Surg. 2012;22:740–8.
Kim SH, Liu TC, Abbasi F, et al. Plasma glucose and insulin regulation is abnormal following gastric bypass surgery with or without neuroglycopenia. Obes Surg. 2009;19:1550–6.
Goldfine AB, Mun EC, Devine E, et al. Patients with neuroglycopenia after gastric bypass surgery have exaggerated incretin and insulin secretory responses to a mixed meal. J Clin Endocrinol Metab. 2007;92:4678–85.
Scavini M, Pontiroli AE, Folli F. Asymptomatic hyperinsulinemic hypoglycaemia after gastric banding. N Engl J Med. 2005;353:2822–3.
Baggio LL, Drucker DJ. Biology of incretins: GLP-1 and GIP (review). Gastroenterology. 2007;132:2131–57.
Vincent RP, le Roux CW. Changes in gut hormones after bariatric surgery (review). Clin Endocrinol (Oxf). 2008;69:173–9.
Guldstrand M, Ahrén B, Adamson U. Improved beta-cell function after standardized weight reduction in severely obese subjects. Am J Physiol Endocrinol Metab. 2003;284:E557–65.
Utzschneider KM, Carr DB, Barsness SM, et al. Diet-induced weight loss is associated with an improvement in beta-cell function in older men. J Clin Endocrinol Metab. 2004;89:2704–10.
Conflict of Interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Papamargaritis, D., Koukoulis, G., Sioka, E. et al. Dumping Symptoms and Incidence of Hypoglycaemia After Provocation Test at 6 and 12 Months After Laparoscopic Sleeve Gastrectomy. OBES SURG 22, 1600–1606 (2012). https://doi.org/10.1007/s11695-012-0711-3
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-012-0711-3