Abstract
Purpose of Review
Importation of schistosomiasis by migrant populations is increasingly being recognized as a global health issue in non-endemic countries, with consequences for the infected individuals and for public health. The purpose of this review is to assess the extent of the problem and the possible ways to mitigate its impacts.
Recent Findings
Published studies on schistosomiasis in migrants to the main refugee-hosting countries were identified and reviewed. The use of sensitive tests for screening indicated that the prevalence of schistosomiasis among migrants to non-endemic countries was higher than previously recognized. The establishment of schistosomiasis transmission in southern Europe had also demonstrated the ease with which the disease could be spread to new areas by moving populations.
Summary
The high prevalence of schistosomiasis among refugees and migrant populations is documented by several reports from Europe, North America, Australia, and New Zealand. It is also clear that there are no uniform international protocols for screening and treatment of migrants with schistosomiasis. Moreover, the existing protocols are not being consistently implemented and may not be inclusive of all vulnerable migrants. There is a need for more research on the implementation, feasibility, cost-effectiveness, and efficacy of different protocols for screening and treatment of refugees and migrant populations from high-risk areas. There is also a need for development and evaluation of newer, more accurate diagnostic screening tests for this purpose.

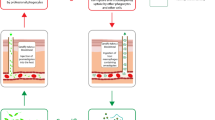
Similar content being viewed by others
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
WHO Media center, Schistosomiasis fact sheet, updated January 2017. Available from: http://www.who.int/mediacentre/factsheets/fs115/en/
WHO. Status of schistosomiasis endemic countries, 2015. Available from: http://apps.who.int/neglected_diseases/ntddata/sch/sch.html
Madinga J, Linsuke S, Mpabanzi L, Meurs L, Kanobana K, Speybroeck N, et al. Schistosomiasis in the Democratic Republic of Congo: a literature review. Parasites & Vectors. 2015;8:601. https://doi.org/10.1186/s13071-015-1206-6.
Cao C, Baoa Z, Lia S, Weib W, Yib P, Yua Q, et al. Schistosomiasis in a migrating population in the lake region of China and its potential impact on control operations. Acta Tropica. 2015;145:88–92.
Bian C-R, Lu D-B, Su J, Zhou X, Zhuge HX, PHL L. Serological prevalence of Schistosoma japonicum in mobile populations in previously endemic but now non-endemic regions of china : a systematic review and meta-analysis. PLoSONE. 2015;10(6):e0128896. https://doi.org/10.1371/journal. pone.0128896.
UNHCR, Global trends, forced displacement in 2016, trends at a glance, http://www.unhcr.org/globaltrends2016/
United Nations Department of Economic and Social Affairs, Population Division. Trends in international migration, 2015. December 2015. http://www.un.org/en/development/desa/population/migration/publications/migrationreport/docs/MigrationReport2015.pdf
McCarthy AE, Weld LH, Barnett ED, So H, Coyle C, Greenaway C, et al. Spectrum of illness in international migrants seen at GeoSentinel clinics in 1997-2009, part 2: migrants resettled internationally and evaluated for specific health concerns. Clin Infect Dis. 2013 Apr;56(7):925–33. https://doi.org/10.1093/cid/cis1016.
Montresor A, Crompton DWT, Hall A, Bundy DAP, Savioli L. Guidelines for the evaluation of soil-transmitted helminthiasis and schistosomiasis at community level. Geneva: World Health Organization; 1998. p. 1–49.
Katz N, Chaves A, Pellegrino J. A simple device for quantitative stool thick-smear technique in Schistosomiasis mansoni. Rev Inst Med Trop São Paulo. 1972;14:397–400.
WHO. Bench aids for the diagnosis of intestinal parasites. Geneva: World Health Organization; 1994. p. 1–20.
Peters PA, Mahmoud AA, Warren KS, Ouma JH, Siongok TK. Field studies of a rapid, accurate means of quantifying Schistosoma haematobium eggs in urine samples. Bull World Health Organ. 1976;54:159–62.
•• Hinz R, Schwarz NG, Hahn A, Frickmann H. Serological approaches for the diagnosis of schistosomiasis—a review. Mol Cell Probes. 2017;31:2–21. This review presents results of published studies on serological assays detecting antibodies against different Schistosoma species. It provides insights in the diagnostic performance and an overview on the availability of described assays and their suitability for case management and large-scale screening. It is helpful for understanding the value of the assays in screening for schistosomiasis
Kinkel H-F, Dittrich S, Bäumer B, Weitzel T. Evaluation of eight serological tests for diagnosis of imported schistosomiasis. Clin Vaccine Immunol. 2012;19:948–53.
Tsang VC, Wilkins PP. Immunodiagnosis of schistosomiasis. Immunol Invest. 1997;26:175–88.
Bierman WF, Wetsteyn JC, van Gool T. Presentation and diagnosis of imported schistosomiasis: relevance of eosinophilia, microscopy for ova, and serology. J Travel Med. 2005;12:9–13.
•• Utzinger J, Becker SL, van Lieshout L, van Dam GJ, Knopp S. New diagnostic tools in schistosomiasis. Clin Microbiol Infect. 2015;21(6):529–42. This is a review on the latest developments in schistosomiasis diagnosis, including microscopic techniques, rapid diagnostic tests for antigen detection, polymerase chain reaction (PCR) assays, and proxy markers for morbidity assessments. This is relevant to understanding interpretation of screening tests used in migrants
van Dam GJ, Xu J, Bergquist R, de Dood CJ, Utzinger J, Qin ZQ, et al. An ultra-sensitive assay targeting the circulating anodic antigen for the diagnosis of Schistosoma japonicum in a low-endemic area, People’s Republic of China. Acta Trop. 2015;141:190–7.
Knopp S, Corstjens PLAM, Koukounari A, Cercamondi CI, Ame SM, de Dood CJ, et al. Sensitivity and specificity of a urine circulating anodic antigen test for the diagnosis of Schistosoma haematobium in low endemic settings. PLoS Negl Trop Dis. 2015;9:e0003752.
Ochodo EA, Gopalakrishna G, Spek B, et al. Circulating antigen tests and urine reagent strips for diagnosis of active schistosomiasis in endemic areas. Cochrane Database Syst Rev. 2015;3:CD009579.
Verweij JJ, Stensvold CR. Molecular testing for clinical diagnosis and epidemiological investigations of intestinal parasitic infections. Clin Microbiol Rev. 2014;27:371–418.
van Lieshout L, Roestenberg M. Clinical consequences of new diagnostic tools for intestinal parasites. Clin Microbiol Infect. 2015 Jun;21(6):520–8. https://doi.org/10.1016/j.cmi.2015.03.015.
Seybolt LM, Christiansen D, Barnett ED. Diagnostic evaluation of newly arrived asymptomatic refugees with eosinophilia. Clin Infect Dis. 2006;42:363–7.
Edwards A. 2015. UNHCR viewpoint: ‘refugee’ or ‘migrant’. Available from: http://www.unhcr.org/en-us/news/latest/2016/7/55df0e556/unhcr-viewpoint-refugee-migrant-right.html
UNHCR Convention and protocol relating to the status of refugees http://www.unhcr.org/3b66c2aa10.html
• Hvass AMF, Wejse C. Systematic health screening of refugees after resettlement in recipient countries: a scoping review. Annals of Human Biology. 2017;44(5):475–83. https://doi.org/10.1080/03014460.2017.1330897. This is a review of studies on health screening of refugees in North America, Australia/New Zealand, and Europe. Because of differences in country policies, the screenings were conducted differently in the various locations. The studies demonstrated great variation in who was targeted for screening and how screening was conducted.
Department of Homeland Security. Yearbook of immigration statistics 2015. Available from: https://www.dhs.gov/immigration-statistics/yearbook/2015
Domestic intestinal parasite guidelines. Available from: https://www.cdc.gov/immigrantrefugeehealth/guidelines/domestic/intestinal-parasites-domestic.html.
Guidelines for overseas presumptive treatment of strongyloidiasis, schistosomiasis, and soil-transmitted helminth infections. Available from: https://www.cdc.gov/immigrantrefugeehealth/guidelines/overseas/intestinal-parasites-overseas.html
•• Centers for Disease Control. Treatment schedules for presumptive parasitic infections. Available from: http://www.cdc.gov/immigrantrefugeehealth/guidelines/overseas/interventions/interventions.html .This site shows the US CDC intestinal parasite guidelines and an updated table for predeparture treatment. The guidelines address the parasitic infections most commonly encountered in refugees but focus on soil-transmitted helminthic infections ( Ascaris , Trichuris , hookworm), Strongyloides , and Schistosoma spp.
Geltman PL, Cochran J, Hedgecock C. Intestinal parasites among African refugees resettled in Massachusetts and the impact of an overseas pre-departure treatment program. Am J Trop Med Hyg. 2003;69(6):657–62.
Lifson AR, Thai D, O'Fallon A, Mills WA, Hang K. Prevalence of tuberculosis, hepatitis B virus, and intestinal parasitic infections among refugees to Minnesota. Public Health Reports. 2002;117(1):69–77.
Lowther SA, Johnson G, Hendel-Paterson B, Nelson K, Mamo B, Krohn K, et al. HIV/AIDS and associated conditions among hiv-infected refugees in Minnesota, 2000–2007. Int J Environ Res Public Health. 2012;9:4197–209. https://doi.org/10.3390/ijerph9114197.
Garg PK, Perry S, Dorn M, Hardcastle L, Parsonnet J. Risk of intestinal helminth and protozoan infection in a refugee population. Am J Trop Med Hyg. 2005;73(2):38691.
Posey D, Blackburn B, Weinberg M, Flagg E, Ortega L, Wilson M, et al. High prevalence and presumptive treatment of schistosomiasis and strongyloidiasis among African refugees. Clin Infect Dis. 2007;45:1310–5.
Franco-Paredes C, Dismukes R, Nicolls D, Hidron A, Workowski K, Rodriguez-Morales A, et al. Persistent and untreated tropical infectious diseases among Sudanese refugees in the United States. Am J Trop Med Hyg. 2007;77:633–5.
Quandelacy TM, Riefkohl A, Franco PC. Prevalence of untreated schistosomiasis among Sudanese refugees: “the lost boys of Sudan” in the United States. Bol Med Hosp Infant Mex. 503Vol. 67, Noviembre-Diciembre 2010. Boletin medico del Hospital Infantil de Mexico
Brodine SK, Thomas A, Huang R, et al. Community based parasitic screening and treatment of Sudanese refugees: application and assessment of Centers for Disease Control guidelines. Am J Trop Med Hyg. 2009;80:425–30.
Chang AH, Perry S, Du JN, Agunbiade A, Polesky A, Parsonnet J. Decreasing intestinal parasites in recent northern California refugees. Am. J. Trop. Med. Hyg. 2013;88(1):191–7. https://doi.org/10.4269/ajtmh.2012.12-0349.
Rapoport AB, McCormick D, Cohen PA. Screening for Schistosoma mansoni and Strongyloides stercoralis infection among Brazilian immigrants in the United States. Open Forum Infect Dis. 2015;2(1):ofv003. Published online 2015 Jan 8. https://doi.org/10.1093/ofid/ofv003. PMCID: PMC4438884.
Khan K, Heidebrecht C, Sears J, Chan A, Rashid M, Greenaway C, Stauffer W, Narasiah L, Pottie K; Canadian Collaboration for Immigrant and Refugee Health, guidelines for immigrant health, Appendix 8: intestinal parasites—Strongyloides and Schistosoma: evidence review for newly arriving immigrants and refugees http://www.cmaj.ca/content/suppl/2010/06/07/cmaj.090313.DC1/imm-para-8-at.pdf. This document reviews evidence on parasitic infection in refugee populations, the value of serologic testing and treatment of strongyloidiasis and schistosomiasis, and the use of ivermectin and praziquantel for treating strongyloidiasis and schistosomiasis.
Redditt VJ, Janakiram P, Graziano D, Rashid M. Health status of newly arrived refugees in Toronto, Ont: part 1: infectious diseases. Can Fam Physician. 2015;61(7):e303–9. PMCID: PMC4501620
CDC-DPDx-schistosomiasis infection—laboratory diagnosis. Available from: https://www.cdc.gov/dpdx/schistosomiasis/dx.html
Illinois Refugee Health Program. 2015 Annual screening summary report. Available from: http://www.dph.illinois.gov/sites/default/files/publications/publicationscmh2015-refugee-program-ar.pdf
• Citizenship and Immigration Canada. Statistics and open data. Available from: www.cic.gc.ca/english/resources/statistics/
López-Vélez R, Huerga H, Turrientes MC. Infectious diseases in immigrants from the perspective of a tropical medicine referral unit. Am J Trop Med Hyg. 2003;69(1):115–21.
Monge-Maillo B, Jiménez BC, Pérez-Molina JA, Norman F, Navarro M, Pérez-Ayala A, et al. Imported infectious diseases in mobile populations, Spain. Emerg Infect Dis. 2009;15:1745–52.
Monge-Maillo B, López-Vélez R, Norman FF, Ferrere-González F, Martínez-Pérez Á, Pérez-Molina JA. Screening of imported infectious diseases among asymptomatic sub-Saharan African and Latin American immigrants: a public health challenge. Am J Trop Med Hyg. 2015;92:848–56.
Bocanegra C, Salvador F, Sulleiro E, Sánchez-Montalvá A, Pahissa A, Molina I. Screening for imported diseases in an immigrant population: experience from a teaching hospital in Barcelona, Spain. Am J Trop Med Hyg. 2014;91:1277–81.
•• Delcor N, Maruri B, Arandes A, Guiu I, Essadik H, Soley M, et al. Infectious diseases in sub-Saharan immigrants to Spain. Am. J. Trop. Med. Hyg. 2016;94(4):750–6. https://doi.org/10.4269/ajtmh.15-0583. This paper describes infectious diseases in newly arrived sub-Saharan immigrants after standardized health visits at an international health center in Barcelona, Spain.
Salvador F, Molina I, Sulleiro E, Burgos J, Curran A, Van den Eynde E, et al. Tropical diseases screening in immigrant patients with human immunodeficiency virus infection in Spain. Am. J. Trop. Med. Hyg. 2013;88(6):1196–202. https://doi.org/10.4269/ajtmh.12-0714.
•• Herbinger K, Alberer M, Berens-Riha N, Schunk M, Bretzel G, von Sonnenburg F, et al. Spectrum of imported infectious diseases: a comparative prevalence study of 16,817 German travelers and 977 immigrants from the tropics and subtropics. Am. J. Trop. Med. Hyg. 2016;94(4):757–66. https://doi.org/10.4269/ajtmh.15-0731. This retrospective analysis shows a large spectrum of imported IDs among returning German travelers and immigrants, which varies greatly based not only on travel destination and origin of immigrants, but also on type of travel
Mockenhaupt F, Barbre K, Jensenius M, Larsen C, Barnett E, Stauffer W, Rothe C, Asgeirsson H, Hamer D, Esposito D, Gautret P, Schlagenhauf P. Profile of illness in Syrian refugees: a GeoSentinel analysis, 2013 to 2015. Euro Surveill. 2016;21(10). doi: https://doi.org/10.2807/1560-7917.ES.2016.21.10.30160
Maaßen W, Wiemer D, Frey 1C, Kreuzberg C, Tannich E, Hinz R, et al. Microbiological screenings for infection control in unaccompanied minor refugees: the German Armed Forces Medical Service’s experience. Military Medical Research. 2017;4:13. https://doi.org/10.1186/s40779-017-0123-8. PMCID: PMC5402321
• Deniaud F, Rouessé C, Collignon A, Domingo A, Rigal L. Failure to offer parasitology screening to vulnerable migrants in France: epidemiology and consequences. Sante. 2010;20(4):201–8.
Monpierre O, Baudino P, Rio-Rene P, Maurice S, Malvy D, Receveur MC. Global health of unaccompanied refugee minors in Gironde (France) between 2011 and 2013. Bull Soc Pathol Exot. 2016;109:99–106. https://doi.org/10.1007/s13149-016-0476-3. PMID: 26860845
Pierre Baudino. Etat de sant´e des mineurs isol´es ´etrangers accueillis en Gironde entre 2011 et ´ 2013. Masters Thesis, Université de Bordeaux, Medecine humaine et pathologie. 2015. HAL Id: dumas-01157256 https://dumas.ccsd.cnrs.fr/dumas-01157256
Chernet A, Kling K, Sydow V, Kuenzli E, Hatz C, Utzinger J, et al. Accuracy of diagnostic tests for Schistosoma mansoni infection in asymptomatic Eritrean refugees: serology and POC-CCA against stool microscopy. Clin Infect Dis. 2017; https://doi.org/10.1093/cid/cix366. This study was to evaluate the accuracy of a combination of microscopy, different serological tests, and POC-CCA tests for the screening of Eritrean refugees in Switzerland for schistosomiasis
• Beltrame A, Guerriero M, AnghebenA GF, Requena-Mendez A, Zammarchi L, et al. Accuracy of parasitological and immunological tests for the screening of human schistosomiasis in immigrants and refugees from African countries: an approach with latent class analysis. PLoS Negl Trop Dis. 2017;11(6):e0005593. https://doi.org/10.1371/journal.pntd.0005593. This study was to evaluate the accuracy of different tests for the screening of schistosomiasis in African migrants in Italy
Riccardi N, Nosenzo F, Peraldo F, Sarocchi F, Taramasso L, Traverso P, et al. Increasing prevalence of genitourinary schistosomiasis in Europe in the migrant era: neglected no more? PLOS Neglected Tropical Diseases. 2017; https://doi.org/10.1371/journal.pntd.0005237.
Poddighe D, Castelli L, Pulcrano G, Grosini A, Balzaretti M, Spadaro S, et al. Urinary schistosomiasis in an adolescent refugee from Africa: an uncommon cause of hematuria and an emerging infectious disease in Europe. J Immigr Minor Health. 2016;18:1237–40. https://doi.org/10.1007/s10903-015-0272-3. PMID: 26335551
Manzardo C, Treviño B, Gómez i Prat J, Cabezos J, Monguí E, Clavería I, et al. Communicable diseases in the immigrant population attended to in a tropical medicine unit: epidemiological aspects and public health issues. Travel Med Infect Dis. 2008 Jan-Mar;6(1-2):4–11. https://doi.org/10.1016/j.tmaid.2007.11.002.
European Centre for Disease Prevention and Control. Rapid risk assessment: local transmission of Schistosoma haematobium in Corsica, France. Stockholm: The Centre; 2015. http://ecdc.europa.eu/en/publications/Publications/risk-assessment-Schistosoma%20haematobium-Corsica-update_TOR1N6.pdf
•• Boissier J, Grech-Angelini S, Webster BL, Allienne JF, Huyse T, Mas-Coma S, et al. Outbreak of urogenital schistosomiasis in Corsica (France): an epidemiological case study. Lancet Infect Dis. 2016;16:971–9. https://doi.org/10.1016/S1473-3099(16)00175-4. This paper presents an updated account of the epidemiological studies investigating the outbreak of urogenital schistosomiasis in Corsica (France)
Berry A, Fillaux J, Martin-Blondel G, Boissier J, Iriart X, Marchou B, et al. Evidence for a permanent presence of schistosomiasis in Corsica, France, 2015. Euro Surveill. 2016; 21(1).
Australian Government, Department of Immigration and Border Protection. Australia’s offshore humanitarian programme: 2015–16 http://www.border.gov.au/ReportsandPublications/Documents/statistics/australia-offshore-humanitarian-programme-2015-16.pdf
The Royal Australasian College of Physicians policy on refugee and asylum seeker health, Royal Australasian College of Physicians, May 2015 https://www.racp.edu.au/docs/default-source/advocacy-library/policy-on-refugee-and-asylum-seeker-health.pdf
• Chaves NJ, Paxton G, Biggs BA, Thambiran A, Smith M, Williams J, Gardiner J, Davis JS; On behalf of the Australasian Society for Infectious Diseases and Refugee Health Network of Australia Guidelines writing group. Recommendations for comprehensive post-arrival health assessment for people from refugee-like backgrounds. https://www.asid.net.au/documents/item/1225. These are the Australian guidelines for post-arrival health assessment in refugee-like populations. It provides detail on 39 studies including more than 30,000 people from refugee-like backgrounds from primary care, primary, and tertiary care refugee and asylum seeker health services and detention centers around Australia, presented by age and region of origin.
Caruana SR, Kelly HA, Ngeow JY, Ryan NJ, Bennett CM, Chea L, et al. Undiagnosed and potentially lethal parasite infections among immigrants and refugees in Australia. J Travel Med. 2006;13(4):233–9.
Rice JE, Skull SA, Pearce C, Mulholland N, Davie G, Carapetis JR. Screening for intestinal parasites in recently arrived children from East Africa. J Paediatr Child Health. 2003;39(6):456–9.
Martin JA, Mak DB. Changing faces: a review of infectious disease screening of refugees by the Migrant Health Unit, Western Australia in 2003 and 2004. Med J Aust. 2006;185(11–12):607–10.
Raman S, Wood N, Webber M, Taylor K, Isaacs D. Matching health needs of refugee children with services: how big is the gap? Aust N Z J Public Health. 2009;33(5):466–70.
Davis J, Weber M. A prospective audit of 215 newly arrived African refugees. J Paediatr Child Health. 2007;42(A13).
Tiong ACD, Patel MS, Gardiner J, Ryan R, Linton KS, Walker K a, et al. Health issues in newly arrived African refugees attending general practice clinics in Melbourne. Med J Aust. 2006;185(11):602–6.
Gibney KB, Mihrshahi S, Torresi J, Marshall C, Leder K, Biggs BA. The profile of health problems in African immigrants attending an infectious disease unit in Melbourne, Australia. Am J Trop Med Hyg. 2009;80(5):805–11.
Sheikh M, Pal A, Wang S, MacIntyre CR, Wood NJ, Isaacs D, et al. The epidemiology of health conditions of newly arrived refugee children: a review of patients attending a specialist health clinic in Sydney. J Paediatr Child Health. 2009 Sep;45(9):509–13.
Mutch RC, Cherian S, Nemba K, Geddes JS, Rutherford DM, Chaney GM, et al. Tertiary paediatric refugee health clinic in Western Australia: analysis of the first 1026 children. J Paediatr Child Health. 2012;48(7):582–7.
Johnston V, Smith L, Roydhouse H. The health of newly arrived refugees to the top end of Australia: results of a clinical audit at the Darwin Refugee Health Service. Aust J Prim Health. 2012 Jan;18(3):242–7.
Chaves NJ, Gibney KB, Leder, O’Brien DP, Marshall C, Biggs BA. Screening practices for infectious diseases among Burmese refugees in Australia. Emerg Infect Dis. 2009;15:1769–72. https://doi.org/10.3201/eid1511.090777.
Paxton GA, Sangster KJ, Maxwell EL, McBride CRJ, Drewe RH. Post-arrival health screening in Karen refugees in Australia. PLoS ONE. 2012;7(5):e38194. https://doi.org/10.1371/journal.pone.0038194.
McLeod A, Reeve M. The health status of quota refugees screened by New Zealand’s Auckland Public Health Service between 1995 and 2000. N Z Med J. 2005;118(1224):U1702.
Rungan S, Reeve AM, Reed PW, Voss L. Health needs of refugee children younger than 5 years arriving in New Zealand. Pediatr Infect Dis J. 2013 Dec;32(12):e432–6.
The Auckland Regional Public Health Service. http://www.arphs.govt.nz/health-information/promoting-health-wellbeing/refugee-health/service
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Ahmed A. Adeel declares that he has no conflict of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by the author.
Additional information
This article is part of the Topical Collection on Tropical Diseases in Conflict Regions
Rights and permissions
About this article
Cite this article
Adeel, A.A. Schistosomiasis in International Refugees and Migrant Populations. Curr Trop Med Rep 4, 256–267 (2017). https://doi.org/10.1007/s40475-017-0128-0
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40475-017-0128-0