Abstract
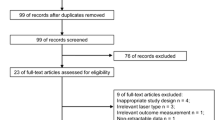
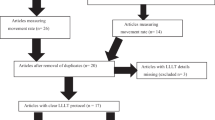
The aim of this study is to systematically summarize the available evidence regarding low-level laser therapy (LLLT) speed-up effect on dental alignment in comprehensive orthodontic treatment. An extensive electronic search was conducted in PubMed, ScienceDirect, Cochrane, Web of Science, and Scopus up to February 20, 2023. The Cochrane risk of bias tool and the Newcastle-Ottawa Quality Assessment Form were used by two authors independently to assess the risk of bias (RoB). Statistical analysis was performed by Review Manager 5.3. The eight eligible trials were reviewed and included in qualitative synthesis. Four studies reported the overall time of leveling and alignment (OLAT, days), enabling a synthesizing of the data. The meta-analysis results showed that LLLT significantly reduced the overall time of leveling and alignment compared to control group (MD=−30.36, 95% CI range −41.50 to −19.22, P<0.0001), with moderate heterogeneity (χ2=4.10, P=0.25, I2=27%). Based on the data available, statistically significant evidence with moderate risk of bias suggests that LLLT may have a positive effect on accelerating dental alignment. However, due to the differences in intervention strategy and evaluating method, the conclusions should be interpreted with caution.




Similar content being viewed by others
References
Uribe F, Padala S, Allareddy V, Nanda R (2014) Patients’, parents’, and orthodontists’ perceptions of the need for and costs of additional procedures to reduce treatment time. Am J Orthod Dentofacial Orthop 145(4 Suppl):65–73. https://doi.org/10.1016/j.ajodo.2013.12.015
Chung H, Dai T, Sharma SK, Huang YY, Carroll JD, Hamblin MR (2012) The nuts and bolts of low-level laser (light) therapy. Ann Biomed Eng 40:516–533. https://doi.org/10.1007/s10439-011-0454-7
Huang H, Williams RC, Kyrkanides S (2014) Accelerated orthodontic tooth movement: molecular mechanisms. Am J Orthod Dentofacial Orthop 146:620–632. https://doi.org/10.1016/j.ajodo.2014.07.007
Kasai K, Yuching Chou M, Yamaguchi M (2015) Molecular effects of low energy laser irradiation during orthodontic tooth movement. Semin Orthod 21:203–209. https://doi.org/10.1053/j.sodo.2015.06.007
Kim Y, Kim SS, Kim SJ, Kwon D, Jeon E, Son W (2008) Low level laser irradiation facilitates fibronectin and collagen type I turnover during tooth movement in rats. Lasers Med Sci 25:25–31. https://doi.org/10.1007/s10103-008-0585-8
Cavalcanti MF, Maria DA, de Isla N et al (2015) Evaluation of the proliferative effects induced by low-level laser therapy in bone marrow stem cell culture. Photomed Laser Surg 33:610–616. https://doi.org/10.1089/pho.2014.3864
Gkantidis N, Mistakidis I, Kouskoura T et al (2014) Effectiveness of non-conventional methods for accelerated orthodontic tooth movement: a systematic review and meta-analysis. J Dent 42(10):1300–1319. https://doi.org/10.1016/j.jdent.2014.07.013
Azzam A, Salah S, Hicham R, Thaer W, Reem H (2018) Efficiency of Er:YAG utilization in accelerating deep bite orthodontic treatment. Laser Ther 27:193–202. https://doi.org/10.5978/islsm.27_18-OR-15
Isola G, Matarese M, Briguglio F et al (2019) Effectiveness of low-level laser therapy during tooth movement: a randomized clinical trial. Mater (Basel) 12:2187. https://doi.org/10.3390/ma12132187
Shpack N, Davidovitch M, Sarne O et al (2008) Duration and anchorage management of canine retraction with bodily versus tipping mechanics. Angle Orthod 1:78. https://doi.org/10.2319/011707-24.1
Al-Shahrani I, Togoo RA, Hosmani J (2019) Photobiomodulation in acceleration of orthodontic tooth movement: a systematic review and meta analysis. Complementary Ther Med 47:102220. https://doi.org/10.1016/j.ctim.2019.102220
Üretürk SE, Saraç M, Fıratlı S, Can ŞB, Güven Y, Fıratlı E (2017) The effect of low-level laser therapy on tooth movement during canine distalization. Lasers Med Sci 32:757–764. https://doi.org/10.1007/s10103-017-2159-0
Sousa MV, Scanavini MA, Sannomiya EK, Velasco LG, Angelieri F (2011) Influence of low-level laser on the speed of orthodontic movement. Photomed Laser Surg 29:191–196. https://doi.org/10.1089/pho.2009.2652
Doshi-Mehta G, Bhad-Patil WA (2012) Efficacy of low-intensity laser therapy in reducing treatment time and orthodontic pain: a clinical investigation. Am J Orthod Dentofacial Orthop 141:289–297. https://doi.org/10.1016/j.ajodo.2011.09.009
Qamruddin I, Alam MK, Mahroof V, Fida M, Khamis MF, Husein A (2017) Effects of low-level laser irradiation on the rate of orthodontic tooth movement and associated pain with self-ligating brackets. Am J Orthod Dentofacial Orthop 152:622–630. https://doi.org/10.1016/j.ajodo.2017.03.023
Karadeniz C, Lee K, Lindsay D et al (2022) Oral appliance-generated malocclusion traits during the long-term management of obstructive sleep apnea in adults: a systematic review and meta-analysis. Angle Orthod 2:92. https://doi.org/10.2319/041921-316.1
Ren C, Mcgrath C, Yang Y (2015) The effectiveness of low-level diode laser therapy on orthodontic pain management: a systematic review and meta-analysis. Lasers Med 30(7):1881–1893. https://doi.org/10.1007/s10103-015-1743-4
Mistakidis I, Katib H, Vasilakos G, Kloukos D, Gkantidis N (2016) Clinical outcomes of lingual orthodontic treatment: a systematic review. Eur J Orthod 38:447–458. https://doi.org/10.1177/2320206819881607
Ghaffar Y, Sharaby FE, Negm IM (2022) Effect of low-level laser therapy on the time needed for leveling and alignment of mandibular anterior crowding: a randomized controlled clinical trial. Angle Orthod 4:92. https://doi.org/10.2319/102721-795.1
Lo Giudice A, Nucera R, Leonardi R, Paiusco A, Baldoni M, Caccianiga G (2020) A comparative assessment of the efficiency of orthodontic treatment with and without photobiomodulation during mandibular decrowding in young subjects: a single-center, single-blind randomized controlled trial. Photobiomodul Photomed Laser Surg 38(5):272–279. https://doi.org/10.1089/photob.2019.4747
Nahas AZ, Samara SA, Rastegar-Lari TA (2016) Decrowding of lower anterior segment with and without photobiomodulation: a single center, randomized clinical trial. Lasers Med Sci 32(1):1–7. https://doi.org/10.1007/s10103-016-2094-5
Hasan MMAA, Sultan K, Hamadah O (2016) Low-level laser therapy effectiveness in accelerating orthodontic tooth movement: a randomized controlled clinical trial. Angle Orthod 87(4). https://doi.org/10.2319/062716-503.1
Shehawy T, Hussein FA, Awady A (2020) Outcome of photodynamic therapy on orthodontic leveling and alignment of mandibular anterior segment: a controlled clinical trial. Photodiagnosis Photodyn Ther 31:101903. https://doi.org/10.1016/j.pdpdt.2020.101903
Caccianiga G, Paiusco A, Perillo L et al (2017) Does low-level laser therapy enhance the efficiency of orthodontic dental alignment? Results from a randomized pilot study. Photomed Laser Surg 2016:4215. https://doi.org/10.1089/pho.2016.4215
Shaughnessy T, Kantarci A, Kau CH et al (2016) Intraoral photobiomodulation-induced orthodontic tooth alignment: a preliminary study. BMC Oral Health:16. https://doi.org/10.1186/s12903-015-0159-7
Kau CH, Kantarci A, Shaughnessy T et al (2013) Photobiomodulation accelerates orthodontic alignment in the early phase of treatment. Prog Orthod 14(1):1–9. https://doi.org/10.1186/2196-1042-14-42
Cruz D, Kohara E, Ribeiro M, Wetter N (2004) Effects of low intensity laser therapy on the orthodontic movement velocity of human teeth: a preliminary study. Lasers Surg Med 35:117–120. https://doi.org/10.1002/lsm.20076
Limpanichkul W, Godfrey K, Srisuk N, Rattanayatikul C (2006) Effects of low-level laser therapy on the rate of orthodontic tooth movement. Orthod Craniofac Res 9:38–43. https://doi.org/10.1111/j.1601-6343.2006.00338.X
Bjordal JM, Couppé C, Chow RT, Tunér J, Ljunggren EA (2003) A systematic review of low level laser therapy with location-specific doses for pain from chronic joint disorders. Aust J Physiother 49:107–116. https://doi.org/10.1016/S0004-9514(14)60127-6
Lanzafame RJ, Stadler I, Kurtz AF, Connelly R, Peter TA Sr, Brondon P et al (2007) Reciprocity of exposure time and irradiance on energy density during photoradiation on wound healing in a murine pressure ulcer model. Lasers Surg Med 39:534–542. https://doi.org/10.1002/lsm.20600
Varella AM, Revankar AV, Patil AK (2018) Low-level laser therapy increases interleukin-1β in gingival crevicular fluid and enhances the rate of orthodontic tooth movement. Am J Orthod Dentofacial Orthop 154:535–544. https://doi.org/10.1016/j.ajodo.2019.01.004
Hamblin MR, Demidova TN (2016) Mechanisms for low-light therapy. Proc SPIE 6140:1–12. https://doi.org/10.1117/12.730340
Sommer AP, Pinheiro AL, Mester AR, Franke RP, Whelan HT (2001) Biostimulatory windows in low-intensity laser activation: lasers, scanners, and NASA’s light emitting diode array system. J Clin Laser Med Surg 19:29–33. https://doi.org/10.1089/104454701750066910
Goulart CS, Nouer PRA, Martins LM, Garbin IUL, Lizarelli RFZ (2006) Photoradiation and orthodontic movement: experimental study with canines. Photomed Laser Surg 24:192–196. https://doi.org/10.1089/pho.2006.24.192
E. Bernabé, C. Flores-Mir, Estimating arch length discrepancy through Little’s irregularity index for epidemiological use. Eur J Orthod 28 269–273. 10.1093/ejo/cji112
Nordstrom B, Shoji T, Anderson WC, Fields HW Jr, Beck FM, Kim D-G et al (2018) Comparison of changes in irregularity and transverse width with nickel-titanium and niobium-titanium-tantalum-zirconium archwires during initial orthodontic alignment in adolescents: a double-blind randomized clinical trial. Angle Orthod 88:348–354. https://doi.org/10.2319/061417-393.1
Goonewardene RW, Goonewardene MS, Razza JM, Murray K (2008) Accuracy and validity of space analysis and irregularity index measurements using digital models. Aust Orthod J 24:83–90. https://doi.org/10.1016/j.archoralbio.2008.07.002
Funding
This study was supported by the Qingdao Key Health Discipline Development Fund (2022–2024) and the Qingdao Clinical Research Center for Oral Diseases (22-3-7-lczx-7-nsh).
Author information
Authors and Affiliations
Contributions
DH-Z carried out data acquisition and drafted the manuscript. QQ Zhang and YQ-Du were involved in data interpretation and literature research and contributed significantly to the preparation of the manuscript. YJ Zang and SQ Niu formulated the table of “Characteristics of included studies.” FC-Hou and BL designed and coordinated the study and had significant impact in drafting the manuscript. All authors have read and agreed to the published version of the manuscript. All authors read and approved the final manuscript
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
ESM 1
(DOCX 17 kb)
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Zheng, DH., Du, YQ., Zhang, QQ. et al. Effect of low-level laser therapy on orthodontic dental alignment: a systematic review and meta-analysis. Lasers Med Sci 38, 184 (2023). https://doi.org/10.1007/s10103-023-03835-w
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s10103-023-03835-w