Abstract
Objectives
The main goal of the present study was to compare the biomechanical stability of locking plates and conventional miniplate combinations in human mandibles reconstructed with fibular grafts.
Materials and methods
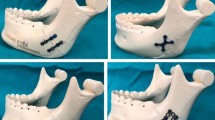
A specially developed and well-proven testing device reproduced the in vivo loading conditions on the mandible. Cadaveric human mandibles (n = 12) reconstructed with harvested human fibular bone grafts were divided into two groups, and different osteosynthesis systems were applied using two lines of plates per osteotomy. On the test apparatus, the specimens were stressed to failure, and interfragmentary movement was monitored and quantified with a contact-free optical measurement system.
Results
The relevant interfragmentary movement results from a Euclidean summary calculation which considered all three spatial angles around the axes. Using values up to a maximum load of 300 N, the conventional six-hole miniplates (profile 1.0) had an average value of 7.45° ± 1.46°, and the locking six-hole plates (profile 1.3) had an average value of 12.16° ± 2.37° for rotational interfragmentary movement. The miniplate system exhibited a significantly superior performance in fixation compared to the fixed-angle system (p < 0.05).
Conclusion
According to these biomechanical experiments, both osteosynthesis devices provided sufficient stabilization at loads of up to 300 N. The six-hole miniplate system provided better stabilization of the osteotomy gap for mandibles reconstructed with fibular grafts.
Clinical relevance
The osteosynthesis system is essential for primary stability and the avoidance of pseudarthrosis formation. This study demonstrates that the miniplates provide sufficient stabilization and offers a method to improve fixation in reconstructed mandibles.



Similar content being viewed by others
References
Hölzle F, Mohr C, Wolff K-D (2008) Reconstructive oral and maxillofacial surgery. Dtsch Arztebl Int 105:815–822
Taylor GI, Miller GDH, Ham FJ (1975) The free vascularized bone graft. A clinical extension of microvascular techniques. Plast Reconstr Surg 55:533–544
Hidalgo DA (1989) Fibula free flap: a new method of mandible reconstruction. Plast Reconstr Surg 84:71–79
Raveh J, Stich H, Sutter F, Greiner R (1984) Use of the titanium-coated hollow screw and reconstruction plate system in bridging of lower jaw defects. J Oral Maxillofac Surg 42:281–294
Herford A, Ellis E III (1998) Use of a locking reconstruction bone plate/screw system for mandibular surgery. J Oral Maxillofac Surg 56:1261–1265
Hidalgo DA (1989) Titanium miniplate fixation in free flap mandible reconstruction. Ann Plast Surg 23:498–507
Kim M-R, Donoff RB (1992) Critical analysis of mandibular reconstruction using AO reconstruction plates. J Oral Maxillofac Surg 50:1152–1157
Boyd JB, Mulholland RS, Davidson J, Gullane PJ, Rotstein LE, Brown DH, Freeman JE, Irish JC (1995) The free flap and plate in oromandibular reconstruction: long-term review and indications. Plast Reconstr Surg 95:1018–1028
Spencer KR, Sizeland A, Taylor GI, Wiesenfeld D (1999) The use of titanium reconstruction plates in patients with oral cancer. Int J Oral Maxillofac Surg 28:288–290
Haug RH, Street CC, Goltz M (2002) Does plate adaptation affect stability? A biomechanical comparison of locking and nonlocking plates. J Oral Maxillofac Surg 60:1319–1326
Schupp W, Arzdorf M, Linke B, Gutwald R (2007) Biomechanical testing of different osteosynthesis systems for segmental resection of the mandible. J Oral Maxillofac Surg 65:924–930
Chiodo TA, Ziccardi VB, Janal M, Sabitini C (2006) Failure strength of 2.0 locking versus 2.0 conventional Synthes mandibular plates: a laboratory model. J Oral Maxillofac Surg 64:1475–1479
Doty JM, Pienkowski D, Goltz M, Haug RH, Valentino J, Arosarena OA (2004) Biomechanical evaluation of fixation techniques for bridging segmental mandibular defects. Arch Otolaryngol Head Neck Surg 130:1388–1392
Döbele S, Horn C, Eichhorn S, Buchholtz A, Lenich A, Burgkart R, Nüssler AK, Lucke M, Andermatt D, Koch R, Stöckle U (2010) The dynamic locking screw (DLS) can increase interfragmentary motion on the near cortex of locked plating constructs by reducing the axial stiffness. Langenbecks Arch Surg 395:421–428
Ellis E 3rd, Graham J (2002) Use of a 2.0-mm locking plate/screw system for mandibular fracture surgery. J Oral Maxillofac Surg 60:642–645
Perren S (2003) Backgrounds of the technology of internal fixators. Injury 34, no. Supplement 2:B1–B3
Frigg R (2003) Development of the locking compression plate. Injury 34, no. Supplement 2:B6–B10
Miller DL, Goswami T (2007) A review of locking compression plate biomechanics and their advantages as internal fixators in fracture healing. Clin Biomech 22:1049–1062
Schmal H, Strohm P, Jaeger M, Südkamp N (2011) Flexible fixation and fracture healing: do locked plating ‘internal fixators’ resemble external fixators? J Orthop Trauma 25:S15–S20
Gutwald R, Alpert B, Schmelzeisen R (2003) Principle and stability of locking plates. Kejo J Med 52:21–24
Wagner M (2003) General principles for the clinical use of the LCP. Injury - Int J Care Injured 34, no. B:31–42
Jewer DD, Boyd JB, Manktelow RT, Zuker RM, Rosen IB, Gullane PJ, Rotstein LE, Freeman JE (1989) Orofacial and mandibular reconstruction with the iliac crest free flap: a review of 60 cases and a new method of classification. Plast Reconstr Surg 84:391–403
Steiner T, Raith S, Eichhorn S, Döbele S, Trainotti S, Müller S, Eder M, Kovacs L, Burgkart R, Wolff K-D, Hölzle F (2012) Evaluation of a new optical measuring system for experiments on fractured human mandibles: a biomechanical feasibility study in maxillofacial surgery. Clin Oral Investig 16:1535–1542
Koolstra JH, Eijden TMGJ (2001) A method to predict muscle control in the kinematically and biomechanically indeterminate human masticatory system. J Biomech 34:1179–1188
Steinhauser E, Diehl P, Hadaller M, Schauwecker J, Busch R, Gradinger R, Mittelmeier W (2006) Biomechanical investigation of the effect of high hydrostatic pressure treatment on the mechanical properties of human bone. J Biomed Mater Res B Appl Biomater 76:130–135
Shetty V, McBrearty D, Fourney M, Caputo AA (1995) Fracture line stability as a function of the internal fixation system: an in vitro comparison using a mandibular angle fracture model. J Oral Maxillofac Surg 53:791–802
Strackee S, Kroon F, Bos K (2001) Fixation methods in mandibular reconstruction using fibula grafts: a comparative study into the relative strength of three different osteosynthesis. Head Neck 23:1–7
Meyer C, Kahn J, Lambert A, Boutemy P, Wilk A (2000) Development of a static simulator of the mandible. J Craniomaxillofac Surg 28:278–286
Meyer C, Kahn J-L, Boutemi P, Wilk A (2002) Photoelastic analysis of bone deformation in the region of the mandibular condyle during mastication. J Craniomaxillofac Surg 30:160–169
Kimura A, Nagasao T, Kaneko T, Tamaki T, Miyamoto J, Nakajima T (2006) Adequate fixation of plates for stability during mandibular reconstruction. J Craniomaxillofac Surg 34:193–200
Knoll W, Gaida A, Maurer P (2006) Analysis of mechanical stress in reconstruction plates for bridging mandibular angle defects. J Craniomaxillofac Surg 34:201–209
Schuller-Gotzburg P, Pleschberger M, Rammerstorfer F, Krenkel C (2009) 3D-FEM and histomorphology of mandibular reconstruction with the titanium functionally dynamic bridging plate. Int J Oral Maxillofac Surg 38:1298–1305
Shaw R, Kanatas A, Lowe D, Stat C, Brown J, Rogers S, Vaughan D (2004) Comparison of miniplates and reconstruction plates in mandibular reconstruction. Head Neck 26:456–463
Militsakh O, Wallace D, Kriet J, Girod D, Olvera M, Tsue T (2004) Use of the 2.0-mm locking reconstruction plate in primary oromandibular reconstruction after composite resection. Otolaryngol Head Neck Surg 131:660–665
Farwell D, Kezirian E, Heydt J, Yueh B, Futran N (2006) Efficacy of small reconstruction plates in vascularized bone graft mandibular reconstruction. Head Neck 28:573–579
Knott P, Suh J, Nabili V, Sercarz J, Head C, Abemayor E, Blackwell K (2007) Evaluation of hardware-related complications in vascularized bone grafts with locking mandibular reconstruction plate fixation. Arch Otolaryngol Head Neck Surg 133:1302–1306
Robey A, Spann M, McAuliff T, Meza J, Hollins R, Johnson P (2008) Comparison of miniplates and reconstruction plates in fibular flap reconstruction of the mandible. Plast Reconstr Surg 122:1733–1738
Sikes JWJ, Smith BR, Mukherjee DP, Coward KA (1998) Comparison of fixation strengths of locking head and conventional screws, in fracture and reconstruction models. J Oral Maxillofac Surg 56:468–473
Haug RH (1993) Effect of screw number on reconstruction plating. Oral Surg Oral Med Oral Pathol 75:664–668
Champy M, Lodde JP, Jaeger JH, Wilk A (1976) Mandibular osteosynthesis according to the Michelet technique. Rev Stomatol Chir Maxillofac 77:569–576
Haerle F, Champy M, Terry B (2009) Atlas of craniomaxillofacial osteosynthesis—microplates, miniplates, and screws, 2nd edn. Georg Thieme, Stuttgart, p. 4
Acknowledgments
We would like to thank the International Bone Research Association (IBRA), Basel, Switzerland, for making these studies possible by providing essential support in the form of a research grant.
Conflict of interest
On behalf of all of the authors of this manuscript, we certify that there is no actual or potential conflict of interest in relation to this article. Additionally, we declare that there exists no financial or personal relationship with other people or organizations that could inappropriately influence this work.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Trainotti, S., Raith, S., Kesting, M. et al. Locking versus nonlocking plates in mandibular reconstruction with fibular graft—a biomechanical ex vivo study. Clin Oral Invest 18, 1291–1298 (2014). https://doi.org/10.1007/s00784-013-1105-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-013-1105-1