Abstract
Introduction
Considering the controversial relationship between blood lipid levels and osteopenia and osteoporosis (OP), we performed this meta-analysis.
Materials and methods
Using specific keywords and related words, we searched PubMed, Embase, and Cochrane Library databases. The Newcastle–Ottawa Scale form was used to evaluate the quality of the literature. According to the inclusion and exclusion criteria, we systematically screened the literature to extract relevant information and data. ReVman 5.3 and Stata 13.0 software were used for statistical analysis. Results were expressed as the mean difference (MD) and 95% confidence interval (95% CI). The heterogeneity test was conducted according to I2 and Q tests. Egger’s test was used to quantitatively evaluate publication bias.
Results
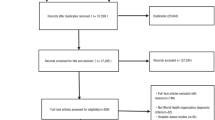
This analysis involved 12 studies (12,395 subjects). The quality of the literature was acceptable. Among subjects who were not taking lipid-lowering drugs, total cholesterol (TC) (MD = 0.11 mmol/L, 95%CI: − 0.03, 0.25; I2 = 21%; P = 0.36), triglycerides (TG) (MD = − 0.01 mmol/L, 95%CI: − 0.09, 0.07; I2 = 6%; P = 0.34), and low-density lipoprotein cholesterol (LDL-C) (MD = 0.10 mmol/L, 95%CI: 0.00, 0.19; I2 = 0%; P = 0.74) in the osteopenia were not significantly increased/decreased. There were no significant differences in LDL-C (MD = 0.02 mmol/L, 95%CI: − 0.09, 0.13; I2 = 0%; P = 0.74) in postmenopausal women in osteopenia. TG (MD = − 0.04 mmol/L, 95%CI: − 0.14,0.07; I2 = 49%; P = 0.07) was unchanged in the osteoporosis (OP) group in subjects without taking lipid-lowering drugs. HDL-C was elevated in OP group (MD = 0.05 mmol/L, 95%CI: 0.03, 0.07; I2 = 31%; P = 0.15) but not in osteopenia group (MD = 0.01 mmol/L, 95%CI: − 0.01, 0.02; I2 = 38%; P = 0.14) in all subjects.
Conclusion
HDL-C was elevated in patients with OP.






Similar content being viewed by others
Availability of data and material
The original data can be obtained by email request.
Abbreviations
- BMD:
-
Bone mineral density
- BMI:
-
Body mass index
- HDL-C:
-
High-density lipoprotein cholesterol
- LDL-C:
-
Low-density lipoprotein cholesterol
- MD:
-
Mean difference
- TC:
-
Total cholesterol
- TG:
-
Triglyceride
- OP:
-
Osteoporosis
- 95%CI:
-
95% Confidence interval
References
Zhang Y, Chai Y, Pan X, Shen H, Wei X, Xie Y (2019) Tai chi for treating osteopenia and primary osteoporosis: a meta-analysis and trial sequential analysis. Clin Interv Aging 14:91–104
Bliuc D, Nguyen ND, Alarkawi D, Nguyen TV, Eisman JA, Center JR (2015) Accelerated bone loss and increased post-fracture mortality in elderly women and men. Osteoporos Int 26:1331–1339
Gerber LM, Bener A, Al-Ali HM, Hammoudeh M, Liu LQ, Verjee M (2015) Bone mineral density in midlife women: the study of women’s health in qatar. Climacteric 18:316–322
Acar B, Ozay AC, Ozay OE, Okyay E, Sisman AR, Ozaksoy D (2016) Evaluation of thyroid function status among postmenopausal women with and without osteoporosis. Int J Gynaecol Obstet 134:53–57
Li Y, Hui M, Chang X, Li M, Wang Y, Zhang B, Yu J (2018) BMI reduction and vitamin D insufficiency mediated osteoporosis and fragility fractures in patients at nutritional risk: a cross-sectional study. Eur J Clin Nutr 72:455–459
Gu LJ, Lai XY, Wang YP, Zhang JM, Liu JP (2019) A community-based study of the relationship between calcaneal bone mineral density and systemic parameters of blood glucose and lipids. Medicine (Baltimore) 98:e16096
Ersoy GS, Simsek EE, Vatansever D, Kasikci HO, Keser B, Sakin O (2017) Lipid profile and plasma atherogenic index in postmenopausal osteoporosis. North Clin Istanb 4:237–241
Li S, Guo H, Liu Y, Wu F, Zhang H, Zhang Z, Xie Z, Sheng Z, Liao E (2015) Relationships of serum lipid profiles and bone mineral density in postmenopausal Chinese women. Clin Endocrinol (Oxf) 82:53–58
Alay I, Kaya C, Cengiz H, Yildiz S, Ekin M, Yasar L (2020) The relation of body mass index, menopausal symptoms, and lipid profile with bone mineral density in postmenopausal women. Taiwan J Obstet Gynecol 59:61–66
Dimic A, Popovic MR, Tasic I, Djordjevic D, Stojanovic S, Stamenkovic B, Popovic D, Milenkovic S, Dimic M, Nedovic J (2012) Relation between bone density and certain parameters of lipid status in postmenopausal women. Cent Eur J Med 7:642–649
Arikan DC, Coskun A, Ozer A, Kilinc M, Atalay F, Arikan T (2011) Plasma selenium, zinc, copper and lipid levels in postmenopausal Turkish women and their relation with osteoporosis. Biol Trace Elem Res 144:407–417
Bijelic R, Balaban J, Milicevic S (2016) Correlation of the lipid profile, BMI and bone mineral density in postmenopausal women. Mater Sociomed 28:412–415
Han W, Bai X, Wang N, Han L, Sun X, Chen X (2017) Association between lumbar bone mineral density and serum uric acid in postmenopausal women: a cross-sectional study of healthy Chinese population. Arch Osteoporos 12:50
Huang C, Li S (2016) Association of blood neutrophil lymphocyte ratio in the patients with postmenopausal osteoporosis. Pak J Med Sci 32:762–765
Pliatsika P, Antoniou A, Alexandrou A, Panoulis C, Kouskouni E, Augoulea A, Dendrinos S, Aravantinos L, Creatsa M, Lambrinoudaki I (2015) Serum lipid levels and bone mineral density in Greek postmenopausal women. Gynecol Endocrinol 28:655–660
Qi H, Bao J, An G, Ouyang G, Zhang P, Wang C, Ying H, Ouyang P, Ma B, Zhang Q (2016) Association between the metabolome and bone mineral density in pre- and post-menopausal Chinese women using GC-MS. Mol Biosyst 12:2265–2275
Sivas F, Alemdaroğlu E, Elverici E, Kuluğ T, Özoran K (2009) Serum lipid profile: Its relationship with osteoporotic vertebrae fractures and bone mineral density in Turkish postmenopausal women. Rheumatol Int 29:885–890
Verit FF, Celik H, Yazgan P, Erel O, Geyikli I (2007) Paraoxonase-1 activity as a marker of atherosclerosis is not associated with low bone mineral density in healthy postmenopausal women. Arch Gynecol Obstet 275:353–359
Chen YY, Wang WW, Yang L, Chen WW, Zhang HX (2018) Association between lipid profiles and osteoporosis in postmenopausal women: a meta-analysis. Eur Rev Med Pharmacol Sci 22:1–9
Trimpou P, Odén A, Simonsson T, Wilhelmsen L, Landin-Wilhelmsen K (2011) High serum total cholesterol is a long-term cause of osteoporotic fracture. Osteoporos Int 22:1615–1620
An T, Hao J, Sun S, Li R, Yang M, Cheng G, Zou M (2017) Efficacy of statins for osteoporosis: a systematic review and meta-analysis. Osteoporos Int 28:47–57
Chan MY, Nguyen ND, Center JR, Eisman JA, Nguyen TV (2012) Absolute fracture-risk prediction by a combination of calcaneal quantitative ultrasound and bone mineral density. Calcif Tissue Int 90:128–136
Parhami F, Garfinkel A, Demer LL (2000) Role of lipids in osteoporosis. Arterioscler Thromb Vasc Biol 20:2346–2348
Acknowledgements
We thank Melissa Crawford, PhD, from Liwen Bianji, Edanz Editing China (www.liwenbianji.cn/ac), for editing the English text of a draft of this manuscript.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
HZ: Conceptualization, Methodology, Writing—original draft. YL, MZ and LQ: Methodology, Software. YT: Conceptualization, Writing—review and editing. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflicts of interest
All other authors have no conflicts of interest.
Ethics approval
All analyses were based on previous published studies, thus no ethical approval and patient consent are required.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Consent for publication
This manuscript has been approved by all co-authors and has not been published before.
Code availability
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
About this article
Cite this article
Zhao, H., Li, Y., Zhang, M. et al. Blood lipid levels in patients with osteopenia and osteoporosis:a systematic review and meta-analysis. J Bone Miner Metab 39, 510–520 (2021). https://doi.org/10.1007/s00774-020-01189-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00774-020-01189-9