Abstract
Purpose
Patient-rated measures are considered the gold standard for assessing the outcome of spine surgery, but there is no consensus on the appropriate timing of follow-up. Journals often demand a minimum 2-year follow-up, but the indiscriminate application of this principle may not be warranted. We examined the course of change in patient outcomes up to 5 years after surgery for degenerative spinal disorders.
Methods
The data were evaluated from 4287 consecutive patients (2287 women, 2000 men; aged 62 ± 15 years) with degenerative disorders of the thoracolumbar spine, undergoing first-time surgery at the given level between 01/01/2005 and 31/12/2011. The Core Outcome Measures Index (COMI; scored 0–10) was completed by 4012 (94%) patients preoperatively, 4008 (93%) at 3-month follow-up, 3897 (91%) at 1-year follow-up, 3736 (87%) at 2-year follow-up, and 3387 (79%) at 5-year follow-up. 2959 (69%) completed the COMI at all five time-points.
Results
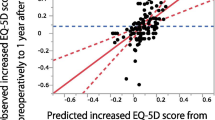
The individual COMI change scores from preoperatively to the various follow-up time-points showed significant correlations ranging from r = 0.50 (for change scores at the earliest vs the latest follow-up) to r = 0.75 (for change scores after 12- vs 24-month follow-up). Concordance with respect to whether the minimum clinically important change score was achieved at consecutive time-points was also good (70–82%). COMI decreased significantly (p < 0.05) from preop to 3 months (by 3.6 ± 2.8 points) and from 3 to 12 months (by 0.3 ± 2.4 points), then levelled off up to 5 years (0.04–0.05 point change; p > 0.05). The course of change up to 12 months differed slightly (p < 0.05) depending on pathology/whether fusion was carried out. For patients undergoing simple decompression, 3-month follow-up was sufficient; those undergoing fusion continued to show further slight but significant change up to 12 months.
Conclusions
Stable group mean COMI scores were observed for all patients from 12 months postoperatively onwards. The early postoperative results appeared to herald the longer term outcome. As such, a ‘wait and see policy’ in patients with a poor initial outcome at 3 months is not advocated. The insistence on a 2-year follow-up could result in a failure to intervene early to achieve better long-term outcomes.




Similar content being viewed by others
References
Buckwalter JA, Heckman JD, Petrie DP, AOA (2003) An AOA critical issue: aging of the North American population: new challenges for orthopaedics. J Bone Jt Surg Am 85-A:748–758
Mannion AF, Porchet F, Kleinstück F, Lattig F, Jeszenszky D, Bartanusz V, Dvorak J, Grob D (2009) The quality of spine surgery from the patient’s perspective: part 1. The Core Outcome Measures Index (COMI) in clinical practice. Eur Spine J 18:367–373
Roder C, Staub L, Dietrich D, Zweig T, Melloh M, Aebi M (2009) Benchmarking with Spine Tango: potentials and pitfalls. Eur Spine J 18(Suppl 3):305–311
Siepe CJ, Tepass A, Hitzl W, Meschede P, Beisse R, Korge A, Mayer HM (2009) Dynamics of improvement following total lumbar disc replacement: is the outcome predictable? Spine (Phila Pa 1976) 34:2579–2586. https://doi.org/10.1097/BRS.0b013e3181b612bd
Glassman SD, Schwab F, Bridwell KH, Shaffrey C, Horton W, Hu S (2009) Do 1-year outcomes predict 2-year outcomes for adult deformity surgery? Spine J 9:317–322. https://doi.org/10.1016/j.spinee.2008.06.450
Grob D, Dvorak J, Muentener M, Porchet F, Mannion AF (2004) Is a 2-year follow-up really necessary for all surgical outcome studies? In: Proceedings of the international society for the study of the lumbar spine, spine week. Porto, Portugal, May 2004
Adogwa O, Elsamadicy AA, Han JL, Cheng J, Karikari I, Bagley CA (2016) Do measures of surgical effectiveness at 1 year after lumbar spine surgery accurately predict 2-year outcomes? J Neurosurg Spine 25:689–696. https://doi.org/10.3171/2015.8.SPINE15476
Asher AL, Chotai S, Devin CJ, Speroff T, Harrell FE Jr, Nian H, Dittus RS, Mummaneni PV, Knightly JJ, Glassman SD, Bydon M, Archer KR, Foley KT, McGirt MJ (2016) Inadequacy of 3-month Oswestry Disability Index outcome for assessing individual longer-term patient experience after lumbar spine surgery. J Neurosurg Spine 25:170–180. https://doi.org/10.3171/2015.11.SPINE15872
Parker SL, Asher AL, Godil SS, Devin CJ, McGirt MJ (2015) Patient-reported outcomes 3 months after spine surgery: is it an accurate predictor of 12-month outcome in real-world registry platforms? Neurosurg Focus 39:E17. https://doi.org/10.3171/2015.9.FOCUS15356
Zehnder P, Aghayev E, Fekete TF, Haschtmann D, Pigott T, Mannion AF (2016) Influence of previous surgery on patient-rated outcome after surgery for degenerative disorders of the lumbar spine. Eur Spine J. https://doi.org/10.1007/s00586-016-4383-x
Deyo RA, Battie M, Beurskens AJHM, Bombardier C, Croft P, Koes B, Malmivaara A, Roland M, Von Korff M, Waddell G (1998) Outcome measures for low back pain research. A proposal for standardized use. Spine 23:2003–2013
Ferrer M, Pellise F, Escudero O, Alvarez L, Pont A, Alonso J, Deyo R (2006) Validation of a minimum outcome core set in the evaluation of patients with back pain. Spine 31:1372–1379 (discussion 1380)
Mannion AF, Elfering A, Staerkle R, Junge A, Grob D, Semmer NK, Jacobshagen N, Dvorak J, Boos N (2005) Outcome assessment in low back pain: how low can you go? Eur Spine J 14:1014–1026
Pochon L, Kleinstuck FS, Porchet F, Mannion AF (2015) Influence of gender on patient-oriented outcomes in spine surgery. Eur Spine J. https://doi.org/10.1007/s00586-015-4062-3
Mannion AF, Porchet F, Kleinstuck FS, Lattig F, Jeszenszky D, Bartanusz V, Dvorak J, Grob D (2009) The quality of spine surgery from the patient’s perspective: part 2. Minimal clinically important difference for improvement and deterioration as measured with the Core Outcome Measures Index. Eur Spine J 18:374–379
Weinstein JN, Lurie JD, Tosteson TD, Zhao W, Blood EA, Tosteson AN, Birkmeyer N, Herkowitz H, Longley M, Lenke L, Emery S, Hu SS (2009) Surgical compared with nonoperative treatment for lumbar degenerative spondylolisthesis. four-year results in the Spine Patient Outcomes Research Trial (SPORT) randomized and observational cohorts. J Bone Jt Surg Am 91:1295–1304. https://doi.org/10.2106/JBJS.H.00913
Weinstein JN, Tosteson TD, Lurie JD, Tosteson AN, Hanscom B, Skinner JS, Abdu WA, Hilibrand AS, Boden SD, Deyo RA (2006) Surgical vs nonoperative treatment for lumbar disk herniation: the Spine Patient Outcomes Research Trial (SPORT): a randomized trial. JAMA 296:2441–2450. https://doi.org/10.1001/jama.296.20.2441
Birkmeyer NJO, Weinstein JN, Tosteson ANA, Tosteson TD, Skinner JS, Lurie JD, Deyo R, Wennberg JE (2002) Design of the Spine Patient Outcomes Research Trial (SPORT). Spine 27:1361–1372
Acknowledgements
We thank all the patients of the Schulthess Klinik who have contributed data to our in-house registry. We thank Dave O’Riordan, Gordana Balaban, Julian Amacker, Kirsten Clift, Selina Nauer, Sara Preziosa, Stéphanie Dosch, and Riccardo Curatolo for the administration of the Spine Tango Surgery and Patient Self-Assessment forms.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors declared that they have no potential conflict of interest.
Rights and permissions
About this article
Cite this article
Fekete, T.F., Loibl, M., Jeszenszky, D. et al. How does patient-rated outcome change over time following the surgical treatment of degenerative disorders of the thoracolumbar spine?. Eur Spine J 27, 700–708 (2018). https://doi.org/10.1007/s00586-017-5358-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-017-5358-2