Abstract
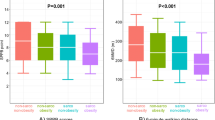
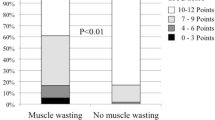
Heart failure (HF) can cause metabolic imbalances, leading to anabolic resistance and increased energy expenditure, which often results in weight loss and cachexia. Comprehensive cardiac rehabilitation (CR), including exercise, nutritional support, and risk management, is crucial for enhancing the health and quality of life of patients with HF and is expected to play a central role in the prevention and treatment of HF-associated cachexia. However, the prevalence of cachexia in patients with HF undergoing comprehensive outpatient CR is currently unknown, and the detailed characteristics including of motor function of such patients remain undefined. Therefore, this cross-sectional study aimed to investigate the prevalence and characteristics of cachexia and the relationship between cachexia and lower limb motor function in patients with HF undergoing outpatient CR. This study included 115 consecutive patients with HF (43% male; mean age, 78 ± 8 years) who underwent comprehensive outpatient CR. The cachexia status was assessed according to the definition proposed by the Asian Working Group on Cachexia in 2023. The Short Physical Performance Battery (SPPB) and Mini Nutritional Assessment Short-Form (MNA-SF) were used to evaluate motor function of the lower limbs and nutritional status, respectively. Multivariate logistic regression analyses were used to examine the potential relationship between cachexia and low SPPB scores (≤ 9 points). The prevalence of cachexia was 30% in this study. Compared with those without cachexia, patients with cachexia were significantly older and showed notable reductions in body mass index, MNA-SF scores, handgrip strength, gait speed, and SPPB scores. A multivariate logistic regression analysis, adjusted for confounders, revealed that both age (odds ratio [OR], 1.129; 95% confidence interval [CI], 1.034–1.248; P = 0.016) and presence of cachexia (OR, 3.783; 95% CI, 1.213–11.796; P = 0.022) were independently associated with low SPPB scores. These findings highlight the importance of focusing on cachexia in patients with HF as part of a comprehensive outpatient CR and may be crucial in developing treatments to improve lower limb motor function in patients with HF who develops cachexia.

Similar content being viewed by others
Data availability
The data supporting this study's findings are available from the corresponding author, M.K., upon reasonable request.
References
Sabban HN (2017) Silent disease progression in clinically stable heart failure. Eur J Heart Fail 19:469–478
Anker SD, Chua TP, Ponikowski P, Harrington D, Swan JW, Kox WJ, Poole-Wilson PA, Coats AJ (1997) Hormonal changes and catabolic/anabolic imbalance in chronic heart failure and their importance for cardiac cachexia. Circulation 96:526–534
Evans WJ, Morley JE, Argilés J, Bales C, Baracos V, Guttridge D, Jatoi A, Kalantar-Zadeh K, Lochs H, Mantovani G, Marks D, Mitch WE, Muscaritoli M, Najand A, Ponikowski P, Fanelli FR, Schambelan M, Schols A, Schuster M, Thomas D, Wolfe R, Anker SD (2008) Cachexia: a new definition. Clin Nutr 27:793–799
Arai H, Maeda K, Wakabayashi H, Naito T, Konishi M, Assantachai P, Auyeung WT, Chalermsri C, Chen W, Chew J, Chou MY, Hsu CC, Hum A, Hwang IG, Kaido T, Kang L, Kamaruzzaman SB, Kim M, Lee JSW, Lee WJ, Liang CK, Lim WS, Lim JY, Lim YP, Lo RSK, Ong T, Pan WH, Peng LN, Pramyothin P, Razalli NH, Saitoh M, Shahar S, Shi HP, Tung HH, Uezono Y, Haehling SV, Won CW, Woo J, Chen LK (2023) Diagnosis and outcomes of cachexia in Asia: working consensus report from the Asian working group for cachexia. J Cachexia Sarcopenia Muscle 14:1949–1958
Lønbro S, Dalgas U, Primdahl H, Johansen J, Nielsen JL, Aagaard P, Hermann AP, Overgaard J, Overgaard K (2013) Progressive resistance training rebuilds lean body mass in head and neck cancer patients after radiotherapy–results from the randomized DAHANCA 25B trial. Radiother Oncol 108:314–319
Rozentryt P, Haehling SV, Lainscak M, Nowak JU, Kalantar-Zadeh K, Polonski L, Anker SD (2010) The effects of a high-caloric protein-rich oral nutritional supplement in patients with chronic heart failure and cachexia on quality of life, body composition, and inflammation markers: a randomized, double-blind pilot study. J Cachexia Sarcopenia Muscle 1:35–42
Kitzman DW, Whellan DJ, Duncan P, Pastva AM, Mentz RJ, Reeves GR, Nelson MB, Chen H, Upadhya B, Reed SD, Espeland MA, Hewston L, O’Connor CM (2021) Physical rehabilitation for older patients hospitalized for heart failure. N Engl J Med 385:203–216
Kato M, Mori Y, Watanabe D, Onoda H, Fujiyama K, Toda M, Kito K (2022) Discharge disposition and 1-year readmission in acute-phase hospitalized patients with heart failure: a retrospective observational multi-center study. Heart Vessels 37:1551–1561
Chiarantini D, Volpato S, Sioulis F, Bartalucci F, Bianco LD, Mangani I, Pepe G, Tarantini F, Berni A, Marchionni N, Bari MD (2010) Lower extremity performance measures predict long-term prognosis in older patients hospitalized for heart failure. J Card Fail 16:390–395
Ishiyama D, Yamada M, Makino A, Iwasaki S, Otobe Y, Shinohara A, Nishio N, Kimura Y, Itagaki A, Koyama S, Yagi M, Matsunaga Y, Mizuno K, Matsushita K (2017) The cut-off point of short physical performance battery score for sarcopenia in older cardiac inpatients. Eur Geriatr Med 8:299–303
Jung HW, Baek JY, Jang IY, Guralnik JM, Rockwood K, Lee E, Kim DH (2021) Short physical performance battery as a crosswalk between frailty phenotype and deficit accumulation frailty index. J Gerontol A Biol Sci Med Sci 76:2249–2255
Reeves GR, Whellan DJ, O’Connor CM, Duncan P, Eggebeen JD, Morgan TM, Hewston LA, Pastva A, Patel MJ, Kitzman DW (2017) A novel rehabilitation intervention for older patients with acute decompensated heart failure: the REHAB-HF pilot study. JACC Heart Fail 5:359–366
Yamamoto K, Tsuchihashi-Makaya M, Kinugasa Y, Iida Y, Kamiya K, Kihara Y, Kono Y, Sato Y, Suzuki N, Takeuchi H, Higo T, Miyazawa Y, Miyajima I, Yamashina A, Yoshita K, Washida K, Kuzuya M, Takahashi T, Nakaya Y, Hasebe N, Tsutsui H, Japanese Heart Failure Society, Expert Consensus Writing Committee (2020) Japanese Heart Failure Society 2018 scientific statement on nutritional assessment and management in heart failure patients. Circ J 84:1408–1444
Ohata E, Nakatani E, Kaneda H, Fujimoto Y, Tanaka K, Takagi A (2023) Use of the Shizuoka hip fracture prognostic score (SHiPS) to Predict long-term mortality in patients with hip fracture in Japan: a cohort study using the Shizuoka Kokuho database. JBMR Plus 7:e10743
Higashizono K, Nakatani E, Hawke P, Fujimoto S, Oba N (2022) Risk factors for gallstone disease onset in Japan: findings from the Shizuoka Study, a population-based cohort study. PLoS ONE 17:e0274659
Anker SD, Ponikowski P, Varney S, Chua TP, Clark AL, Webb-Peploe KM, Harrington D, Kox WJ, Poole-Wilson PA, Coats AJ (1997) Wasting as independent risk factor for mortality in chronic heart failure. Lancet 349:1050–1053
Melenovsky V, Kotrc M, Borlaug BA, Marek T, Kovar J, Malek I, Kautzner J (2013) Relationships between right ventricular function, body composition, and prognosis in advanced heart failure. J Am Coll Cardiol 62:1660–1670
Emami A, Saitoh M, Valentova M, Sandek A, Evertz R, Ebner N, Loncar G, Springer J, Doehner W, Lainscak M, Hasenfuß G, Anker SD, Haehling SV (2018) Comparison of sarcopenia and cachexia in men with chronic heart failure: results from the studies investigating co-morbidities aggravating heart failure (SICA-HF). Eur J Heart Fail 20:1580–1587
Habedank D, Meyer FJ, Hetzer R, Anker SD, Ewert R (2013) Relation of respiratory muscle strength, cachexia and survival in severe chronic heart failure. J Cachexia Sarcopenia Muscle 4:277–285
Nagaya N, Uematsu M, Kojima M, Date Y, Nakazato M, Okumura H, Hosoda H, Shimizu W, Yamagishi M, Oya H, Koh H, Yutani C, Kangawa K (2001) Elevated circulating level of ghrelin in cachexia associated with chronic heart failure: relationships between ghrelin and anabolic/catabolic factors. Circulation 104:2034–2038
Maekawa E, Noda T, Maeda D, Yamashita M, Uchida S, Hamazaki N, Nozaki K, Saito H, Saito K, Ogasahara Y, Konishi M, Kitai T, Iwata K, Jujo K, Wada H, Kasai T, Nagamatsu H, Ozawa T, Izawa K, Yamamoto S, Aizawa N, Yonezawa R, Oka K, Ako J, Momomura S, Kagiyama N, Matsue Y, Kamiya K (2023) Prognostic impact of cachexia by multi-assessment in older adults with heart failure: FRAGILE-HF cohort study. J Cachexia Sarcopenia Muscle 14:2143–2151
Konishi M, Ishida J, Springer J, Anker SD, Haehling SV (2016) Cachexia research in Japan: facts and numbers on prevalence, incidence and clinical impact. J Cachexia Sarcopenia Muscle 7:515–519
Soenen S, Chapman IM (2013) Body weight, anorexia, and undernutrition in older people. J Am Med Dir Assoc 14:642–648
Hamaguchi S, Tsuchihashi-Makaya M, Kinugawa S, Goto D, Yokota T, Goto K, Yamada S, Yokoshiki H, Takeshita A, Tsutsui H, JCARE-CARD Investigators (2010) Body mass index is an independent predictor of long-term outcomes in patients hospitalized with heart failure in Japan. Circ J 74:2605–2611
Horwich TB, Fonarow GC, Hamilton MA, MacLellan WR, Woo MA, Tillisch JH (2001) The relationship between obesity and mortality in patients with heart failure. J Am Coll Cardiol 38:789–795
Nagai T, Yoshikawa T, Saito Y, Takeishi Y, Yamamoto K, Ogawa H, Anzai T, JASPER Investigators (2018) Clinical characteristics, management, and outcomes of Japanese patients hospitalized for heart failure with preserved ejection fraction—a report from the Japanese heart failure syndrome with preserved ejection fraction (JASPER) registry. Circ J 82:1534–1545
Nakai M, Iwanaga Y, Kanaoka K, Sumita Y, Nishioka Y, Myojin T, Kubo S, Okada K, Soeda T, Noda T, Sakata Y, Imamura T, Saito Y, Yasuda S, Miyamoto Y (2022) Age-dependent association of discharge heart-failure medications with clinical outcomes in a super-aged society. Biomed Pharmacother 155:113761
Valentova M, Haehling SV, Bauditz J, Doehner W, Ebner N, Bekfani T, Elsner S, Sliziuk V, Scherbakov N, Murín J, Anker SD, Sandek A (2016) Intestinal congestion and right ventricular dysfunction: a link with appetite loss, inflammation, and cachexia in chronic heart failure. Eur Heart J 37:1684–1691
Valentova M, Anker SD, Haehling SV (2022) Cardiac cachexia revisited: the role of wasting in heart failure. Cardiol Clin 40:199–207
Okoshi MP, Capalbo RV, Romeiro FG, Okoshi K (2017) Cardiac cachexia: perspectives for prevention and treatment. Arq Bras Cardiol 108:74–80
Kubo I, Izawa KP, Kajisa N, Ogura A, Kanai M, Nishio R, Matsumoto D (2022) Relationship between physical function at discharge and hospital meal intake in elderly patients with heart failure. Heart Vessels 37:1740–1748
Acknowledgements
The authors thank all staff of the Omote-jyunkankika Cardiovascular Clinic for facilitating this study.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: this research was supported by JSPS KAKENHI (grant number 21K17501).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflict of interest to disclose.
Consent to participate
Informed consent was obtained from all individual participants included in this study.
Consent to publication
The participants have consented to the submission of this article to the journal.
Ethical approval
The study design was approved by the Ethics Committee of Tokoha University (23-03).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Kato, M., Ono, S., Seko, H. et al. Relationship between cachexia and short physical performance battery scores in patients with heart failure attending comprehensive outpatient cardiac rehabilitation. Heart Vessels (2024). https://doi.org/10.1007/s00380-024-02400-x
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00380-024-02400-x