Abstract
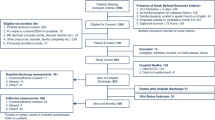
Patients hospitalized for acute heart failure (HF) tend to experience declines in physical function and activities of daily living (ADL) due to bed rest and restricted mobilization. This could result in some patients being transferred to rehabilitation hospitals. This study aims to examine the relationship between discharge disposition and 1-year readmission and mortality rates in HF patients. Nine hundred fifty six consecutive HF patients who were hospitalized for acute decompensated HF and underwent rehabilitation were divided into two groups: home (returned home) or transfer (transferred to rehabilitative or long-term care hospital units due to decline in physical function and/or ADL) groups. The primary and secondary outcomes were 1-year readmission and mortality rates after discharge, respectively. Of the 956 patients, 8.6% (n = 82) were transferred to rehabilitative or long-term care hospital units. Over a 1-year follow-up period, all-cause and HF readmission rates were 50.1% (n = 479) and 27.2% (n = 260), respectively. The transfer group had significantly lower readmission rates compared to home group after adjusting for the pre-existing risk factors (hazard ratio for all-cause and HF readmission: 0.600 and 0.552, 95% CI 0.401–0.897 and 0.314–0.969; P = 0.013 and P = 0.038, respectively). There was no significant relationship between discharge disposition and all-cause mortality rate. Low ADL defined as Barthel index < 60 points was identified as a predictor of all-cause and HF readmission among the home group (odds ratio for all-cause and HF readmission rates: 2.156 and 1.847, 95% CI 1.026–4.531 and 1.036–2.931; P = 0.043 and P = 0.037, respectively). This multi-center study demonstrated that HF patients transferred to rehabilitative or long-term care hospital units after an acute hospitalization had a significantly decreased 1-year all-cause and HF readmission rates compared to patients who returned to their home. These findings may help in selecting a discharge disposition for older HF patients with ADL decline.





Similar content being viewed by others
References
Shimokawa H, Miura M, Nochioka K, Sakata Y (2015) Heart failure as a general pandemic in Asia. Eur J Heart Fail 17:884–892
Yasuda S, Nakao K, Nishimura K, Miyamoto Y, Sumita Y, Shishido T, Anzai T, Tsutsui H, Ito H, Komuro I, Saito Y, Ogawa H, on the behalf of JROAD Investigators (2016) The current status of cardiovascular medicine in Japan—analysis of a large number of health records from a nationwide claim-based database, JROAD-DPC. Circ J 80:2327–2335
Yokota J, Takahashi R, Matsukawa Y, Matsushima K (2020) Examination of independent predictors of discharge disposition in acute phase hospitalized heart failure patients undergoing phase I cardiac rehabilitation. Eur J Phys Rehabil Med 56:780–786
Covinsky KE, Pierluissi E, Johnston CB (2011) Hospitalization-associated disability: “She was probably able to ambulate, but I’m not sure.” JAMA 306:1782–1793
Loyd C, Markland AD, Zhang Y, Fowler M, Harper S, Wright NC, Carter CS, Buford TW, Smith CH, Kennedy R, Brown CJ (2020) Prevalence of hospital-associated disability in older adults: a meta-analysis. J Am Med Dir Assoc 21:455–461
Fuentes-Abolafio IJ, Stubbs B, Pérez-Belmonte LM, Bernal-López MR, Gómez-Huelgas R, Cuesta-Vargas AI (2020) Physical functional performance and prognosis in patients with heart failure: a systematic review and meta-analysis. BMC Cardiovasc Disord 20:512
Motoki H, Nishimura M, Kanai M, Kimura K, Minamisawa M, Yamamoto S, Saigusa T, Ebisawa S, Okada A, Kuwahara K (2019) Impact of inpatient cardiac rehabilitation on Barthel Index score and prognosis in patients with acute decompensated heart failure. Int J Cardiol 293:125–130
Tsutsui H, Isobe M, Ito H, Ito H, Okumura K, Ono M, Kitakaze M, Kinugawa K, Kihara Y, Goto Y, Komuro I, Saiki Y, Saito Y, Sakata Y, Sato N, Sawa Y, Shiose A, Shimizu W, Shimokawa H, Seino Y, Node K, Higo T, Hirayama A, Makaya M, Masuyama T, Murohara T, Momomura SI, Yano M, Yamazaki K, Yamamoto K, Yoshikawa T, Yoshimura M, Akiyama M, Anzai T, Ishihara S, Inomata T, Imamura T, Iwasaki YK, Ohtani T, Onishi K, Kasai T, Kato M, Kawai M, Kinugasa Y, Kinugawa S, Kuratani T, Kobayashi S, Sakata Y, Tanaka A, Toda K, Noda T, Nochioka K, Hatano M, Hidaka T, Fujino T, Makita S, Yamaguchi O, Ikeda U, Kimura T, Kohsaka S, Kosuge M, Yamagishi M, Yamashina A, Japanese Circulation Society and the Japanese Heart Failure Society Joint Working Group (2019) JCS 2017/JHFS 2017 guideline on diagnosis and treatment of acute and chronic heart failure—digest version. Circ J 83:2084–2184
Huynh QL, Negishi K, De Pasquale CG, Hare JL, Leung D, Stanton T, Marwick TH (2019) Cognitive domains and postdischarge outcomes in hospitalized patients with heart failure. Circ Heart Fail 12:e006086
von Elm E, Altman DG, Egger M, Pocock SJ, Gøtzsche PC, Vandenbroucke JP, Initiative STROBE (2007) Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement: guidelines for reporting observational studies. BMJ 335:806–808
Izawa H, Yoshida T, Ikegame T, Izawa KP, Ito Y, Okamura H, Osada N, Kinugawa S, Kubozono T, Kono Y, Kobayashi K, Nishigaki K, Higo T, Hirashiki A, Miyazawa Y, Morio Y, Yanase M, Yamada S, Ikeda H, Momomura SI, Kihara Y, Yamamoto K, Goto Y, Makita S, Japanese Association of Cardiac Rehabilitation Standard Cardiac Rehabilitation Program Planning Committee (2019) Standard cardiac rehabilitation program for heart failure. Circ J 83:2394–2398
JCS Joint Working Group (2014) Guidelines for diagnosis and treatment of patients with vasospastic angina (Coronary Spastic Angina) (JCS 2013). Circ J 78:2779–2801
Kato M, Mori Y, Watanabe D, Onoda H, Fujiyama K, Toda M, Kito K (2021) Relationship between average daily rehabilitation time and decline in instrumental activity of daily living among older patients with heart failure: a preliminary analysis of a multicenter cohort study, SURUGA-CARE. PLoS One 16:e0254128
OECD Health Statistics 2021 Definitions, Sources and Methods. https://www.oecd.org/els/health-systems/Table-of-Content-Metadata-OECD-Health-Statistics-2021.pdf (Accessed 08 Aug 2021)
Bodner TE (2008) What improves with increased missing data imputations? Struct Equ Modeling 15:651–675. https://doi.org/10.1080/10705510802339072WOS:000260426800005 (Accessed 29 Nov 2021)
Kamiya K, Sato Y, Takahashi T, Tsuchihashi-Makaya M, Kotooka N, Ikegame T, Takura T, Yamamoto T, Nagayama M, Goto Y, Makita S, Isobe M (2020) Multidisciplinary cardiac rehabilitation and long-term prognosis in patients. Circ Heart Fail 13:e006798
Deutz NE, Matheson EM, Matarese LE, Luo M, Baggs GE, Nelson JL, Hegazi RA, Tappenden KA, Ziegler TR, NOURISH Study Group (2016) Readmission and mortality in malnourished, older, hospitalized adults treated with a specialized oral nutritional supplement: a randomized clinical trial. Clin Nutr 35:18–26
Agra Bermejo RM, González Ferreiro R, Varela Román A, Gómez Otero I, Kreidieh O, Conde Sabarís P, Rodríguez-Mañero M, Moure González M, Seoane Blanco A, Virgós Lamela A, García Castelo A, González Juanatey JR (2017) Nutritional status is related to heart failure severity and hospital readmissions in acute heart failure. Int J Cardiol 230:108–114
Teramatsu H, Shiraishi J, Matsushima Y, Araki M, Okazaki T, Saeki S (2019) Using physical function to predict hospital readmission within 1 year in patients with heart failure. Prog Rehabil Med 4:20190018
Kitzman DW, Whellan DJ, Duncan P, Pastva AM, Mentz RJ, Reeves GR, Nelson MB, Chen H, Upadhya B, Reed SD, Espeland MA, Hewston L, O’Connor CM (2021) Physical rehabilitation for older patients hospitalized for heart failure. N Engl J Med 385:203–216
Uemura Y, Shibata R, Takemoto K, Koyasu M, Ishikawa S, Murohara T, Watarai M (2018) Prognostic impact of the preservation of activities of daily living on post-discharge outcomes in patients with acute heart failure. Circ J 82:2793–2799
Saitoh M, Takahashi Y, Okamura D, Akiho M, Suzuki H, Noguchi N, Yamaguchi Y, Hori K, Adachi Y, Takahashi T (2021) Prognostic impact of hospital-acquired disability in elderly patients with heart failure. ESC Heart Fail 8:1767–1774
Ades PA, Keteyian SJ, Balady GJ, Houston-Miller N, Kitzman DW, Mancini DM, Rich MW (2013) Cardiac rehabilitation exercise and self-care for chronic heart failure. JACC Heart Fail 1:540–547
van Diepen S, Majumdar SR, Bakal JA, McAlister FA, Ezekowitz JA (2008) Heart failure is a risk factor for orthopedic fracture: a population-based analysis of 16,294 patients. Circulation 118:1946–1952
Otto CM (2020) Heartbeat: risk of stroke in patients with heart failure. Heart 106:549–551
Waring T, Gross K, Soucier R, ZuWallack R (2017) Measured physical activity and 30-day rehospitalization in heart failure patients. J Cardiopulm Rehabil Prev 37:124–129
Takabayashi K, Fujita R, Iwatsu K, Ikeda T, Morikami Y, Ichinohe T, Yamamoto T, Takenaka K, Okuda M, Nakajima O, Koito H, Terasaki Y, Kitamura T, Kitaguchi S, Nohara R (2020) Impact of home- and community-based services in the long-term care insurance system on outcomes of patients with acute heart failure: Insights from the Kitakawachi Clinical Background and Outcomes of Heart Failure Registry. Geriatr Gerontol Int 20:967–973
Statistics of ministry of health, labour and welfare in Japan. https://www.mhlw.go.jp/english/database/db-hw/lifetb19/dl/lifetb19-01.pdf (Accessed 01 Sep 2021)
Katano S, Yano T, Ohori K, Kouzu H, Nagaoka R, Honma S, Shimomura K, Inoue T, Takamura Y, Ishigo T, Watanabe A, Koyama M, Nagano N, Fujito T, Nishikawa R, Ohwada W, Hashimoto A, Katayose M, Ishiai S, Miura T (2021) Barthel index score predicts mortality in elderly heart failure—a goal of comprehensive cardiac rehabilitation. Circ J. https://doi.org/10.1253/circj.CJ-21-058
Acknowledgements
We thank all staff of the participating hospitals, Shizuoka Medical Center, Juntendo University Shizuoka Hospital, Shizuoka City Hospital, Fujinomiya City General Hospital, and Hamamatsu University Hospital, for facilitating this multi-center study. We also thank Fumi Nihei Green and Akira Kubo for editing a draft of this manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflicts of interest associated with this manuscript.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Kato, M., Mori, Y., Watanabe, D. et al. Discharge disposition and 1-year readmission in acute-phase hospitalized patients with heart failure: a retrospective observational multi-center study. Heart Vessels 37, 1551–1561 (2022). https://doi.org/10.1007/s00380-022-02059-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00380-022-02059-2