Abstract
Background
As a new-generation collagen stimulator, polycaprolactone (PCL) containing filler has been extensively applied in facial dermal fillers and other medical aesthetic fields. However, inadvertent intravascular injection of PCL may result in complications such as tissue edema, flap necrosis, and even blindness. To date, there is no effective treatment for PCL-induced intravascular embolism.
Objectives
The aim of this study was to identify a viable resolution for the embolism resulting from intravascular administration of PCL-containing fillers.
Methods
Two different animal experiments were performed: (1) PCL-induced rat inferior epigastric arteries embolism, followed by gross observation, histological evaluation, and cytokines analysis from serum; and (2) PCL-induced rabbit auricular artery embolism, immediately treated with heparin and nitroglycerin. The ears were then evaluated by gross observation, Laser speckle imaging, in vivo imaging system (IVIS) imaging, and histological evaluation. Saline and hyaluronic acids (HA) were used as controls, hyaluronidase was used as a positive drug.
Results
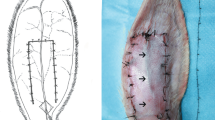
In a rat model of inferior epigastric arteries embolism, both intravascular injection of HA and PCL resulted in flap necrosis, indicating that the filler-induced intravascular embolism can lead to serious complications. In a rabbit model of auricular artery embolism, the combination treatment of heparin and nitroglycerin resulted in a relative blood reperfusion recovery of 80% in the ischemic area of the PCL group on day 7 post-operation, which was comparable to that of the HA group treated with hyaluronidase. Histological analysis revealed that the administration of heparin and nitroglycerin significantly attenuated intravascular thrombosis formation and inflammatory cell aggregation.
Conclusions
The combination of heparin and nitroglycerin effectively restores blood flow reperfusion in the intravascular embolization caused by PCL filler injection, alleviates local tissue edema and flap necrosis. These findings offer a novel approach for future clinical management of intravascular embolization with PCL-containing filler injection.
No Level Assigned
This journal requires that authors assign a level of evidence to each submission to which Evidence-Based Medicine rankings are applicable. This excludes Review Articles, Book Reviews, and manuscripts that concern Basic Science, Animal Studies, Cadaver Studies, and Experimental Studies. For a full description of these Evidence-Based Medicine ratings, please refer to the Table of Contents or the online Instructions to Authors www.springer.com/00266.








Similar content being viewed by others
References
Eppley BL, Dadvand B (2006) Injectable soft-tissue fillers: clinical overview. Plast Reconstr Surg 118(4) https://journals.lww.com/plasreconsurg/Fulltext/2006/09150/Injectable_Soft_Tissue_Fillers__Clinical_Overview.30.aspx
Donald II, Alam M, Kim J (2009) Injectable fillers for facial rejuvenation: a review. J Plast Reconstr Aesthet Surg 62(1):11–18
Tatjana P, David F (2013) Dermal fillers in aesthetics: an overview of adverse events and treatment approaches. Clin Cosmet Investig Dermatol 6:295–316
Koh IS, Lee W (2019) Hyaluronic acid filler and hyaluronidase. In: Filler complications. Springer, Singapore, pp 27–40. https://doi.org/10.1007/978-981-13-6639-0_2
Chiang YZ, Pierone G, Al-Niaimi F (2017) Dermal fillers: pathophysiology, prevention and treatment of complications. J Eur Acad Dermatol Venereol 31(3):405–413. https://doi.org/10.1111/jdv.13977
Wang D, Xiong S, Zeng N, Wu Y (2022) The facial vein on computed tomographic angiography: implications for plastic surgery and filler injection. Aesthet Surg J 42(5):319–326. https://doi.org/10.1093/asj/sjab391
Hirsch RJ, Narurkar V, Carruthers J (2006) Management of injected hyaluronic acid induced Tyndall effects. Lasers Surg Med 38(3):202–204. https://doi.org/10.1002/lsm.20283
Khatiwala VK, Shekhar N, Aggarwal S, Mandal UK (2008) Biodegradation of poly(ε-caprolactone) (PCL) film by Alcaligenes faecalis. J Polym Environ 16(1):61–67. https://doi.org/10.1007/s10924-008-0104-9
Moon SY, Eun DH, Park JH, Han MH, Lee SJ (2017) Foreign body reaction three years after injection with polycaprolactone (Ellanse®). Eur J Dermatol Ejd. 27(5):549
Christen M-O, Vercesi F (2020) Polycaprolactone: how a well-known and futuristic polymer has become an innovative collagen-stimulator in esthetics. Clin Cosmet Investig Dermatol 13:31–48. https://doi.org/10.2147/CCID.S229054
Pomin VH, Mulloy B (2015) Current structural biology of the heparin interactome. Curr Opin Struct Biol 34:17–25. https://doi.org/10.1016/j.sbi.2015.05.007
Björk I, Lindahl U (1982) Mechanism of the anticoagulant action of heparin. Mol Cell Biochem 48(3):161–182. https://doi.org/10.1007/BF00421226
Oduah EI, Linhardt RJ, Sharfstein ST (2016) Heparin: past, present, and future. Pharmaceuticals. https://doi.org/10.3390/ph9030038
Engelmann B, Massberg S (2013) Thrombosis as an intravascular effector of innate immunity. Nat Rev Immunol 13(1):34–45. https://doi.org/10.1038/nri3345
Stark K, Massberg S (2021) Interplay between inflammation and thrombosis in cardiovascular pathology. Nat Rev Cardiol 18(9):666–682. https://doi.org/10.1038/s41569-021-00552-1
Modin A, Björne H, Herulf M, Alving K, Weitzberg E, Lundberg JON (2001) Nitrite-derived nitric oxide: a possible mediator of ‘acidic–metabolic’ vasodilation. Acta Physiol Scand 171(1):9–16. https://doi.org/10.1046/j.1365-201X.2001.00771.x
Libby P (2002) Inflammation in atherosclerosis. Nature 420(6917):868–874. https://doi.org/10.1038/nature01323
Acknowledgements
The authors would like to thank Prof. for designing the experiment and critical revision of this manuscript.
Funding
The authors received no financial support for the research, authorship, and publication of this article, including payment of the article processing charge.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declared no potential conflicts of interest with respect to the research, authorship, and publication of this article.
Ethical Approval
All animal procedures were conducted in accordance with the Guide for Care and Use of Laboratory Animals by the Institutional Animal Care and Use Committee of SLAC (Shanghai Laboratory Animal Center) 20230124011.
Informed Consent
For this type of study, informed consent is not required.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The work described in this manuscript is original and has not been submitted to other journals. All authors have read and approved the submitted manuscript, the manuscript has not been submitted elsewhere nor published elsewhere in whole or in part. All authors have contributed to ted elsewhere nor published elsewhere in whole or in part. All authors have contributed to this study and approved this document and its submission to your journal.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Khan, A., Gong, L., Wang, Y. et al. Combination Administration of Heparin and Nitroglycerin for the Treatment of Polycaprolactone-Induced Intravascular Embolism: A Preclinical Investigation. Aesth Plast Surg (2024). https://doi.org/10.1007/s00266-024-03969-4
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00266-024-03969-4