Abstract
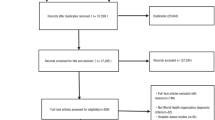
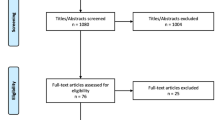
There were some case–control studies, nested case–control studies, and cohort studies with controversial results on the association between serum 25-hydroxyvitamin D [25(OH)D] and breast cancer risk. Case–control studies are prone to selection bias, which limit the strength and quality of the evidence. To overcome the shortcoming of the case–control studies, the meta-analysis of prospective studies including nested case–control studies and cohort studies was conducted. PubMed, Embase, and Web of Science databases were searched, and the last retrieval date was March 24, 2013. For the highest versus the lowest level of serum 25(OH)D, the relative risks (RRs) and its 95 % confidence intervals (CIs) from each study were used to estimate summary RR and its 95 % CI. Subgroup analyses by geographic region, menopausal status, and adjusted status of RR were also performed, respectively. A dose–response association between serum 25(OH)D concentration and breast cancer risk was assessed. Fourteen articles with 9,110 breast cancer cases and 16,244 controls were included in the meta-analysis. Overall, serum 25(OH)D levels were inversely significantly associated with breast cancer risk (RR = 0.845, 95 % CI = 0.750–0.951). Inversely statistically significant associations were observed in North American studies, postmenopausal women, and studies with adjusted and unadjusted RR, respectively. No statistically significant associations were observed in European studies and premenopausal women, respectively. Dose–response analysis showed that every 10 ng/mL increment in serum 25(OH)D concentration was associated with a significant 3.2 % reduction in breast cancer risk. This meta-analysis provides evidence of a significantly inverse association between serum 25(OH)D concentration and breast cancer risk.



Similar content being viewed by others
Abbreviations
- 25(OH)D:
-
25-Hydroxyvitamin D
- 1,25(OH)2D:
-
1,25-Dihydroxyvitamin D
- lα(OH)D3 :
-
1-α-Hydroxycholecalciferol
- RR:
-
Relative risk
- CI:
-
Confidence interval
- SE:
-
Standard error
- VDR:
-
Vitamin D receptor
References
Plum LA, DeLuca HF. Vitamin D, disease and therapeutic opportunities. Nat Rev Drug Discov. 2010;9:941–55.
Welsh J. Cellular and molecular effects of vitamin D on carcinogenesis. Arch Biochem Biophys. 2012;523:107–14.
Garland CF, Garland FC, Gorham ED, et al. The role of vitamin D in cancer prevention. Am J Public Health. 2006;96:252–61.
Holick MF. Vitamin D deficiency. N Engl J Med. 2007;357:266–81.
Essebag V, Genest Jr J, Suissa S, Pilote L. The nested case–control study in cardiology. Am Heart J. 2003;146:581–90.
Higgins JP, Thompson SG. Quantifying heterogeneity in a meta-analysis. Stat Med. 2002;21:1539–58.
DerSimonian R, Laird N. Meta-analysis in clinical trials. Control Clin Trials. 1986;7:177–88.
Mantel N, Haenszel W. Statistical aspects of the analysis of data from retrospective studies of disease. J Natl Cancer Inst. 1959;22:719–48.
Egger M, Davey Smith G, Schneider M, Minder C. Bias in meta-analysis detected by a simple, graphical test. BMJ. 1997;315:629–34.
Greenland S, Longnecker MP. Methods for trend estimation from summarized dose–response data, with applications to meta-analysis. Am J Epidemiol. 1992;135:1301–9.
Gilbert R, Martin RM, Beynon R, et al. Associations of circulating and dietary vitamin D with prostate cancer risk: a systematic review and dose–response meta-analysis. Cancer Causes Control. 2011;22:319–40.
Bertone-Johnson ER, Chen WY, Holick MF, et al. Plasma 25-hydroxyvitamin D and 1,25-dihydroxyvitamin D and risk of breast cancer. Cancer Epidemiol Biomarkers Prev. 2005;14:1991–7.
Chlebowski RT, Johnson KC, Kooperberg C, et al. Calcium plus vitamin D supplementation and the risk of breast cancer. J Natl Cancer Inst. 2008;100:1581–91.
Freedman DM, Chang SC, Falk RT, et al. Serum levels of vitamin D metabolites and breast cancer risk in the prostate, lung, colorectal, and ovarian cancer screening trial. Cancer Epidemiol Biomarkers Prev. 2008;17:889–94.
McCullough ML, Stevens VL, Patel R, et al. Serum 25-hydroxyvitamin D concentrations and postmenopausal breast cancer risk: a nested case control study in the Cancer Prevention Study-II Nutrition Cohort. Breast Cancer Res. 2009;11:R64.
Rejnmark L, Tietze A, Vestergaard P, et al. Reduced prediagnostic 25-hydroxyvitamin D levels in women with breast cancer: a nested case–control study. Cancer Epidemiol Biomarkers Prev. 2009;18:2655–60.
Almquist M, Bondeson AG, Bondeson L, Malm J, Manjer J. Serum levels of vitamin D, PTH and calcium and breast cancer risk—a prospective nested case–control study. Int J Cancer. 2010;127:2159–68.
Engel P, Fagherazzi G, Boutten A, et al. Serum 25(OH) vitamin D and risk of breast cancer: a nested case–control study from the French E3N cohort. Cancer Epidemiol Biomarkers Prev. 2010;19:2341–50.
Eliassen AH, Spiegelman D, Hollis BW, Horst RL, Willett WC, Hankinson SE. Plasma 25-hydroxyvitamin D and risk of breast cancer in the Nurses’ Health Study II. Breast Cancer Res. 2011;13:R50.
Eliassen AH, Tworoger SS, Bertone-Johnson E, Rosner B, Willett WC, Hankinson SE. Circulating vitamin D and breast cancer risk: repeated exposure assessment and 18 years of follow-up in the Nurses’ Health Study. Cancer Res. 2011;71:4633.
Amir E, Cecchini RS, Ganz PA, et al. 25-Hydroxy vitamin-D, obesity, and associated variables as predictors of breast cancer risk and tamoxifen benefit in NSABP-P1. Breast Cancer Res Treat. 2012;133:1077–88.
Neuhouser ML, Manson JE, Millen A, et al. The influence of health and lifestyle characteristics on the relation of serum 25-hydroxyvitamin D with risk of colorectal and breast cancer in postmenopausal women. Am J Epidemiol. 2012;175:673–84.
Mohr SB, Gorham ED, Alcaraz JE, et al. Serum 25-hydroxyvitamin D and breast cancer in the military: a case–control study utilizing pre-diagnostic serum. Cancer Causes Control. 2013;24:495–504.
Ordonez-Mena JM, Schottker B, Haug U, et al. Serum 25-hydroxyvitamin D and cancer risk in older adults: results from a large German prospective cohort study. Cancer Epidemiol Biomarkers Prev. 2013;22:905–16.
Green AK, Hankinson SE, Bertone-Johnson ER, Tamimi RM. Mammographic density, plasma vitamin D levels and risk of breast cancer in postmenopausal women. Int J Cancer. 2010;127:667–74.
Colston KW, Chander SK, Mackay AG, Coombes RC. Effects of synthetic vitamin D analogues on breast cancer cell proliferation in vivo and in vitro. Biochem Pharmacol. 1992;44:693–702.
Chen P, Li M, Gu X, et al. Higher blood 25(OH)D level may reduce the breast cancer risk: evidence from a Chinese population based case–control study and meta-analysis of the observational studies. PLoS One. 2013;8:e49312.
Mohr SB, Gorham ED, Alcaraz JE, et al. Serum 25-hydroxyvitamin D and prevention of breast cancer: pooled analysis. Anticancer Res. 2011;31:2939–48.
Yin L, Grandi N, Raum E, Haug U, Arndt V, Brenner H. Meta-analysis: serum vitamin D and breast cancer risk. Eur J Cancer. 2010;46:2196–205.
Gandini S, Boniol M, Haukka J, et al. Meta-analysis of observational studies of serum 25-hydroxyvitamin D levels and colorectal, breast and prostate cancer and colorectal adenoma. Int J Cancer. 2011;128:1414–24.
Chen P, Hu P, Xie D, Qin Y, Wang F, Wang H. Meta-analysis of vitamin D, calcium and the prevention of breast cancer. Breast Cancer Res Treat. 2010;121:469–77.
Acknowledgments
This work was supported by the grants from the National Natural Science Foundation of China (no. 30972516), Natural Science Foundation of Hebei Province (no. C2010000481), and Hebei Province Health Bureau Foundation (no. 20090004).
Conflicts of interest
None
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Wang, D., Vélez de-la-Paz, O.I., Zhai, JX. et al. Serum 25-hydroxyvitamin D and breast cancer risk: a meta-analysis of prospective studies. Tumor Biol. 34, 3509–3517 (2013). https://doi.org/10.1007/s13277-013-0929-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13277-013-0929-2