Abstract
Objective
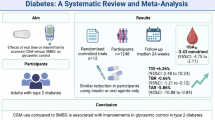
To compare the effects of two individualized nutritional follow-up intervention strategies (home visit or telephone consultation) with no follow-up, with regard to acute readmissions to hospital at two points in time, 30 and 90 days after discharge from hospital.
Design
Randomized clinical trial with two intervention groups and one control group, and monitoring on readmission at 30 and 90 days after discharge.
Setting
Intervention in the participants’ homes after discharge from hospital.
Participants
Inclusion: Malnourished geriatric patients and patients at risk of malnutrition (MNA<24), aged 75 years and older, living at home and alone. Exclusion: Nursing home residents and patients with terminal illnesses or cognitive impairment. Randomization: Upon discharge, the patients were stratified according to nutritional status (MNA), and assigned to one of three groups: ‘home visit’, ‘telephone’, or ‘control’ group. Intervention: Individualized nutritional counselling of the patient and the patient’s daily home carer by a clinical dietician one, two, and four weeks after discharge from hospital. The counselling was either in-person at the patient’s homes, or over the telephone. All patients received a diet plan on discharge. The control group received standard care, but no follow-up after discharge.
Measurements
Information on readmissions to hospital and mortality at 30 and 90 days after discharge was obtained from electronic patient records. Intention-to-treat (ITT) and per-protocol (PP) analyses were carried out.
Results
Two-hundred and eight participants were randomized, 73 to home visits, 68 to the telephone consultation group, and 67 to the control group. The mean age of the participants was 86.1 years. Home visit participants had a lower risk of readmission to hospital compared to control participants at 30 days after discharge (HR=0.4; 95% CI: 0.2-0.9, p=0.03) and 90 days after discharge (HR=0.4; 95% CI: 0.2-0.8, p<0.01). No significant difference was detected between the telephone consultation group and the control group, at either 30 days (HR=0.6, 95% CI: 0.3-1.3, p=0.18) or 90 days after discharge (HR=0.7, 95% CI: 0.4-1.3, p=0.23). The PP analysis revealed that the risk of readmission was significantly lower in the home visit group compared to the control group and the telephone consultation group compared to the control group, and this was evident at 30 days as well as at 90 days after discharge.
Conclusion
An individualized nutritional follow-up performed as home visits seems to reduce readmission to hospital 30 and 90 days after discharge. Intervention by telephone consultations may also prevent readmission, but only among participants who receive the full intervention.




Similar content being viewed by others
References
Kaiser MJ, Bauer JM, Ramsch C, Uter W, Guigoz Y, Cederholm T, et al. Frequency of malnutrition in older adults: a multinational perspective using the mini nutritional assessment. J Am Geriatr Soc 2010 Sep;58(9):1734–1738.
Charlton KE, Nichols C, Bowden S, Lambert K, Barone L, Mason M, et al. Older rehabilitation patients are at high risk of malnutrition: evidence from a large Australian database. J Nutr Health Aging 2010 Oct;14(8):622–628.
MacIntosh C, Morley JE, Chapman IM. The anorexia of aging. Nutrition 2000 Oct;16(10):983–995.
Garcia-Perez L, Linertova R, Lorenzo-Riera A, Vazquez-Diaz JR, Duque-Gonzalez B, Sarria-Santamera A. Risk factors for hospital readmissions in elderly patients: a systematic review. QJM 2011 Aug;104(8):639–651.
Drame M, Lang PO, Novella JL, Narbey D, Mahmoudi R, Laniece I, et al. Six-month outcome of elderly people hospitalized via the emergency department: the SAFES cohort. Rev Epidemiol Sante Publique 2012 Jun;60(3):189–196.
Soderstrom L, Rosenblad A, Adolfsson ET, Saletti A, Bergkvist L. Nutritional status predicts preterm death in older people: a prospective cohort study. Clin Nutr 2014 Apr;33(2):354–359.
Tsubota-Utsugi M, Kikuya M, Satoh M, Inoue R, Hosaka M, Metoki H, et al. Living situations associated with poor dietary intake among healthy Japanese elderly: the Ohasama Study. J Nutr Health Aging 2015 Apr;19(4):375–382.
Westergren A, Hagell P, Sjodahl Hammarlund C. Malnutrition and risk of falling among elderly without home-help service—a cross sectional study. J Nutr Health Aging 2014 Dec;18(10):905–911.
Dhaussy G, Drame M, Jolly D, Mahmoudi R, Barbe C, Kanagaratnam L, et al. Is health-related quality of life an independent prognostic factor for 12-month mortality and nursing home placement among elderly patients hospitalized via the emergency department? J Am Med Dir Assoc 2012 Jun;13(5):453–458.
Charlton K, Nichols C, Bowden S, Milosavljevic M, Lambert K, Barone L, et al. Poor nutritional status of older subacute patients predicts clinical outcomes and mortality at 18 months of follow-up. Eur J Clin Nutr 2012 11;66(11):1224–1228.
Stratton RJ, Hebuterne X, Elia M. A systematic review and meta-analysis of the impact of oral nutritional supplements on hospital readmissions. Ageing Res Rev 2013 Sep;12(4):884–897.
Beck AM, Holst M, Rasmussen HH. Oral nutritional support of older (65 years+) medical and surgical patients after discharge from hospital: systematic review and meta-analysis of randomized controlled trials. Clin Rehabil 2013 Jan;27(1):19–27.
Hubbard GP, Elia M, Holdoway A, Stratton RJ. A systematic review of compliance to oral nutritional supplements. Clin Nutr 2012 Jun;31(3):293–312.
Callen BL, Wells TJ. Views of community-dwelling, old-old people on barriers and aids to nutritional health. J Nurs Scholarsh 2003;35(3):257–262.
Nieuwenhuizen WF, Weenen H, Rigby P, Hetherington MM. Older adults and patients in need of nutritional support: Review of current treatment options and factors influencing nutritional intake. Clin Nutr 2010 /;29(2):160–169.
Spahn JM, Reeves RS, Keim KS, Laquatra I, Kellogg M, Jortberg B, et al. State of the evidence regarding behavior change theories and strategies in nutrition counseling to facilitate health and food behavior change. J Am Diet Assoc 2010 Jun;110(6):879–891.
Marshall S, Bauer J, Isenring E. The consequences of malnutrition following discharge from rehabilitation to the community: a systematic review of current evidence in older adults. J Hum Nutr Diet 2014 Apr;27(2):133–141.
Guigoz Y, Lauque S, Vellas BJ. Identifying the elderly at risk for malnutrition: The Mini Nutritional Assessment. Clin Geriatr Med 2002 11;18(4):737–757.
Vellas B, Guigoz Y, Garry PJ, Nourhashemi F, Bennahum D, Lauque S, et al. The Mini Nutritional Assessment (MNA) and its use in grading the nutritional state of elderly patients. Nutrition 1999 Feb;15(2):116–122.
Nordic nutrition recommendations 2012-integrating nutrition and physical activity.: Norden.
Sundhedsstyrelsen. Screening og behandling af patienter i ernæringsmæssig risiko. Vejledning til læger, sygeplejersker, social-og sundhedsassistenter, sygehjælpere og kliniske diætister. 2008.
Bekendtgørelse om uddannelse i de erhvervsfaglige fællesindgange. Sundhed, omsorg og pædagogik. Nr. 163 af 7. marts 2008. 2008.
Pedersen J, Pedersen P, Damsgaard E. Nutritional follow-up after discharge of malnourished geriatric patients-design of a randomized clinical study. Journal of Aging Research & Clinical Practice 2015;4(2):92–101.
Beck AM, Kjaer S, Hansen BS, Storm RL, Thal-Jantzen K, Bitz C. Follow-up home visits with registered dietitians have a positive effect on the functional and nutritional status of geriatric medical patients after discharge: a randomized controlled trial. Clin Rehabil 2013 Jun;27(6):483–493.
Gariballa S, Forster S, Walters S, Powers H. A randomized, double-blind, placebocontrolled trial of nutritional supplementation during acute illness. Am J Med 2006 Aug;119(8):693–699.
Boling PA. Care transitions and home health care. Clin Geriatr Med 2009 Feb;25(1):135–48, viii.
Menand E, Lenain E, Lazarovici C, Chatellier G, Saint-Jean O, Somme D, et al. French Multicenter Evaluation of the Appropriateness of Admission to the Emergency Department of the Over-80s. J Nutr Health Aging 2015 Jun;19(6):681–687.
Shepperd S, Lannin NA, Clemson LM, McCluskey A, Cameron ID, Barras SL. Discharge planning from hospital to home. Cochrane Database Syst Rev 2013 Jan 31;1:CD000313.
Gonseth J, Guallar-Castillon P, Banegas JR, Rodriguez-Artalejo F. The effectiveness of disease management programmes in reducing hospital re-admission in older patients with heart failure: a systematic review and meta-analysis of published reports. Eur Heart J 2004 Sep;25(18):1570–1595.
Coleman EA, Parry C, Chalmers S, Min SJ. The care transitions intervention: results of a randomized controlled trial. Arch Intern Med 2006 Sep 25;166(17):1822–1828.
Pedersen PU. Nutritional care: the effectiveness of actively involving older patients. J Clin Nurs 2005 02;14(2):247–255.
Munk T, Tolstrup U, Beck AM, Holst M, Rasmussen HH, Hovhannisyan K, et al. Individualised dietary counselling for nutritionally at-risk older patients following discharge from acute hospital to home: a systematic review and meta-analysis. J Hum Nutr Diet 2015 Mar 18.
Mowe M, Bosaeus I, Rasmussen HH, Kondrup J, Unosson M, Rothenberg E, et al. Insufficient nutritional knowledge among health care workers? Clin Nutr 2008 Apr;27(2):196–202.
Fletcher A, Carey E. Knowledge, attitudes and practices in the provision of nutritional care. Br J Nurs 2011 May 27-Jun 9;20(10):615–6, 618-20.
Bauer S, Halfens RJ, Lohrmann C. Knowledge and Attitudes of Nursing Staff Towards Malnutrition Care in Nursing Homes: A Multicentre Cross-Sectional Study. J Nutr Health Aging 2015;19(7):734–740.
Arvanitakis M, Coppens P, Doughan L, Van Gossum A. Nutrition in care homes and home care: recommendations-a summary based on the report approved by the Council of Europe. Clin Nutr 2009 Oct;28(5):492–496.
Rothman KJ. Epidemiology: an introduction. 2nd ed. Oxford; New York: Oxford University Press; 2012.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Lindegaard Pedersen, J., Pedersen, P.U. & Damsgaard, E.M. Nutritional follow-up after discharge prevents readmission to hospital - A randomized clinical trial. J Nutr Health Aging 21, 75–82 (2017). https://doi.org/10.1007/s12603-016-0745-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12603-016-0745-7