Abstract
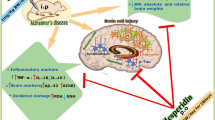
Alzheimer’s disease (AD) is a neurodegenerative pathology characterized by progressive impairment of memory, associated with neurochemical alterations and limited therapy. The aim of this study was to evaluate the effects of inosine on memory, neuroinflammatory cytokines, neurotrophic factors, expression of purinergic receptors, and morphological changes in the hippocampus and cerebral cortex of the rats with AD induced by streptozotocin (STZ). Male rats were divided into four groups: I, control; II, STZ; III, STZ plus inosine (50 mg/kg); and IV, STZ plus inosine (100 mg/kg). The animals received intracerebroventricular injections of STZ or buffer. Three days after the surgical procedure, animals were treated with inosine (50 mg/kg or 100 mg/kg) for 25 days. Inosine was able to prevent memory deficits and decreased the immunoreactivity of the brain A2A adenosine receptor induced by STZ. Inosine also increased the levels of brain anti-inflammatory cytokines (IL-4 and IL-10) and the expression of brain-derived neurotrophic factor and its receptor. Changes induced by STZ in the molecular layer of the hippocampus were attenuated by treatment with inosine. Inosine also protected against the reduction of immunoreactivity for synaptophysin induced by STZ in CA3 hippocampus region. However, inosine did not prevent the increase in GFAP in animals exposed to STZ. In conclusion, our findings suggest that inosine has therapeutic potential for AD through the modulation of different brain mechanisms involved in neuroprotection.










Similar content being viewed by others
Data Availability
Not applicable.
Code Availability
Not applicable.
References
Yiannopoulou KG, Papageorgiou SG (2020) Current and future treatments in alzheimer disease: an update. J Cent Ner Sys Dis 12:1179573520907397. https://doi.org/10.1177/1179573520907397
Kempuraj D, Mentor S, Thangavel R, Ahmed ME, Selvakumar GP, Raikwar SP, Dubova J, Zaheer S, Iyer S, Zaheer A (2019) Mast cells in stress, pain, blood-brain barrier, neuroinflammation and Alzheimer’s disease. Front Cell Neurosci 13:54. https://doi.org/10.3389/fncel.2019.00054
Gray SC, Kinghorn KJ, Woodling NS (2020) Shifting equilibriums in Alzheimer’s disease: the complex roles of microglia in neuroinflammation, neuronal survival and neurogenesis. Neural Regen Res 15:1208. https://doi.org/10.4103/1673-5374.272571
Hampel H, Messulam M, Cuello A, Farlow M, Giacobini E, Grossberg G, Khachaturian A, Vergallo A, Cavedo E, Synder P, Khachaturian Z (2018) The cholinergic system in the pathophysyology and tretament of Alzheimer’s disease. Brain 141:1917–1933. https://doi.org/10.1093/brain/awy132
Moore AM, Mahoney E, Dumitrescu L, De Jager PL, Koran M, Petyuk VA, Robinson R, Ruderfer D, Cox N, Schneider J, Bennet D, Jefferson A, Hohman T (2020) APOE ε4-specific associations of VEGF gene family expression with cognitive aging and Alzheimer’s disease. Neurobiol Aging 87:18–25. https://doi.org/10.1016/j.neurobiolaging.2019.10.021
Butterfield DA, Mattson MP (2020) Apolipoprotein E and oxidative stress in brain with relevance to Alzheimer’s disease. Neurobiol Dis 138:104795. https://doi.org/10.1016/j.nbd.2020.104795
Hampel H, Caraci F, Cuello AC, Caruso G, Nisticò R, Corbo M, Baldacci F, Toschi N, Garaci F, Chiesa PA, Verdooner SR, Akman-Anderson L, Hernández F, Ávila J, Emanuele E, Valenzuela PL, Lucía A, Watling M, Imbimbo BP, Vergallo A, Lista S (2020) A path toward precision medicine for neuroinflammatory mechanisms in Alzheimer’s disease. Front Immunol 11:456. https://doi.org/10.3389/fimmu.2020.00456
Stanciu GD, Luca A, Rusu RN, Bild V, BescheaChiriac SI, Solcan C, Bild W, Ababei DC (2020) Alzheimer’s disease pharmacotherapy in relation to cholinergic system involvement. Biomolecules 10:40. https://doi.org/10.3390/biom10010040
Pacheco SM, Soares MSP, Gutierres JM, Gerzson MFB, Carvalho FB, Azambuja J, Shetinger MRC, Stefanello FM, Spanevello RM (2018) Anthocyanins as a potential pharmacological agent to manage memory deficit, oxidative stress and alterations in ion pump activity induced by experimental sporadic dementia of Alzheimer’s type. J Nutr Biochem 56:193–204. https://doi.org/10.1016/j.jnutbio.2018.02.014
Woods LT, Ajit D, Camden JM, Erb L, Weisman GA (2016) Purinergic receptors as potential therapeutic targets in Alzheimer’s disease. Neuropharmacology 104:169–179. https://doi.org/10.1016/j.neuropharm.2015.10.031
Tapia-Arancibia L, Aliaga E, Silhol M, Arancibia S (2008) New insights into brain BDNF function in normal aging and Alzheimer disease. Brain Res Rev 59:201–220. https://doi.org/10.1016/j.brainresrev.2008.07.007
Shen T, You Y, Joseph C, Mirzaei M, Klistorner A, Graham SL, Gupta V (2018) BDNF polymorphism: a review of its diagnostic and clinical relevance in neurodegenerative disorders. Aging Dis 9: 523–536. https://doi.org/10.14336/AD.2017.0717
Tebano MT, Martire A, Chiodi V, Ferrante A, Popoli P (2010) Role of adenosine A2A receptors in modulating synaptic functions and brain levels of BDNF: a possible key mechanism in the pathophysiology of Huntington’s disease. Sci World J 10:1768–1782. https://doi.org/10.1100/tsw.2010.164
Jerónimo-Santos A, Batalha VL, Mueller CE, Baqi Y, Sebastião AM, Lopes LV, Diógenes MJ (2014) Impact of in vivo chronic blockade of adenosine A2A receptors on the BDNF-mediated facilitation of LTP. Neuropharmacology 83:99–106. https://doi.org/10.1016/j.neuropharm.2014.04.006
Lu Y, Christian K, Lu B (2008) BDNF: a key regulator for protein synthesis-dependent LTP and long-term memory? Neurob Learn Mem 89:312–323. https://doi.org/10.1016/j.nlm.2007.08.018
Korte M, Kang H, Bonhoeffer T, Schuman E (1998) A role for BDNF in the late-phase of hippocampal long-term potentiation. Neuropharmacology 37:553–559. https://doi.org/10.1016/s0028-3908(98)00035-5
Phillips HS, Hains JM, Armanini M, Laramee GR, Johnson SA, Winslow JW (1991) BDNF mRNA is decreased in the hippocampus of individuals with Alzheimer’s disease. Neuron 7:695–702. https://doi.org/10.1016/0896-6273(91)90273-3
Connor B, Young D, Yan Q, Faull RLM, Synek B, Dragunow M (1997) Brain-derived neurotrophic factor is reduced in Alzheimer’s disease. Mol Brain Res 49:71–81. https://doi.org/10.1016/s0169-328x(97)00125-3
Allen SJ, Wilcock GK, Dawbarn D (1999) Profound and selective loss of catalytic TrkB immunoreactivity in Alzheimer’s disease. Biochem Biophys Res Commun 264:648–651. https://doi.org/10.1006/bbrc.1999.1561
Ferrer I, Marín C, Rey MJ, Ribalta T, Goutan E, Blanco R, Tolota E, Martí E (1999) BDNF and full-length and truncated TrkB expression in Alzheimer disease. Implications in therapeutic strategies. J Neuropathol Exp Neurol 58:729–739. https://doi.org/10.1097/00005072-199907000-00007
Holsinger RD, Schnarr J, Henry P, Castelo VT, Fahnestock M (2000) Quantitation of BDNF mRNA in human parietal cortex by competitive reverse transcription-polymerase chain reaction: decreased levels in Alzheimer’s disease. Mol Brain Res 76:347–354. https://doi.org/10.1016/s0169-328x(00)00023-1
Counil H, Krantic S (2020) Synaptic activity and (neuro)inflammation in Alzheimer’s disease: could exosomes be an additional link? J Alzheimer’s Dis 74:1029–1043. https://doi.org/10.3233/JAD-191237
Kamphuis W, Middeldorp J, Kooijman L, Sluijs JA, Kooi EJ, Moeton M, Freriks M, Mizee M, Hol E (2014) Glial fibrillary acidic protein isoform expression in plaque related astrogliosis in Alzheimer’s disease. Neurobiol Aging 35:492–510. https://doi.org/10.1016/j.neurobiolaging.2013.09.035
Rebola N, Pinheiro PC, Oliveira CR, Malva JO, Cunha RA (2003) Subcellular localization of adenosine A1 receptors in nerve terminals and synapses of the rat hippocampus. Brain Res 987:49–58. https://doi.org/10.1016/s0006-8993(03)03247-5
Cunha RA (2005) Neuroprotection by adenosine in the brain: from A 1 receptor activation to A 2A receptor blockade. Purinergic Sig 1:111–134. https://doi.org/10.1007/s11302-005-0649-1
Canas PM, Porciúncula LO, Simões AP, Augusto E, Silva HB, Machado NJ, Gonçalvez N, Alfaro T, Gonçalves F, Araújo I, Real J, Coelho J, Andrade G, Alemida R, Chen J, Kofalvi A, Cunha R (2018) Neuronal adenosine A2A receptors are critical mediators of neurodegeneration triggered by convulsions. eNeuro 26: ENEURO.0385–18.2018. https://doi.org/10.1523/ENEURO.0385-18.2018
Blum D, Sandau U, Laurent C, Batalha V, Leboucher A, Hamdane M, Pasquier F, Boison D, Buée L, Lopes L (2013) Adenosine receptors and Alzheimer’s disease. In Adenosine 385–407. Springer New York. https://doi.org/10.1007/978-1-4614-3903-5_19
Rahman A (2009) The role of adenosine in Alzheimer’s disease. Cur Neuropharmacol 7:207–216. https://doi.org/10.2174/157015909789152119
Faivre E, Coelho JE, Zornbach K, Malik E, Baqi Y, Schneider M, Cellai L, Carvalho K, Sebda S, Figeac M, Eddarkaoui S, Caillierez R, Chern Y, Heneka M, Sergeant N, Muller C, Bueé L, Lopes L, Bi V (2018) Beneficial effect of a selective adenosine A2A receptor antagonist in the APPswe/PS1dE9 mouse model of Alzheimer’s disease. Front Mol Neurosc 11:235. https://doi.org/10.3389/fnmol.2018.00235
da Rocha LF, de Oliveira APL, Accetturi BG, de Oliveira MI, Domingos HV, de Almeida CD (2013) Anti-inflammatory effects of inosine in allergic lung inflammation in mice: evidence for the participation of adenosine A2A and A3 receptors. Purinergic Signal 9:325–336. https://doi.org/10.1007/s11302-013-9351-x
Ruhal P, Dhingra D (2018) Inosine improves cognitive function and decreases aging-induced oxidative stress and neuroinflammation in aged female rats. Inflammopharmacology 26:1317–1329. https://doi.org/10.1007/s10787-018-0476-y
Junqueira SC, dos Santos CI, Lieberknecht V, Cunha MP, Calixto JB, Rodrigues ALS (2017) Inosine, an endogenous purine nucleoside, suppresses immune responses and protects mice from experimental autoimmune encephalomyelitis: a role for A2A adenosine receptor. Mol Neurobiol 54:3271–3285. https://doi.org/10.1007/s12035-016-9893-3
Markowitz C, Spitsin S, Zimmernan V, Jacobs V, Udupa J, Hooper C, Koprowski H (2009) The treatment with multiple sclerosis with inosine. J Altern Complement Med 15:619–625. https://doi.org/10.1089/acm.2008.0513
Herman JP, Watson SJ (1987) The rat brain in stereotaxic coordinates (2nd edn) by George Paxinos and Charles Watson. Trends Neurosci 10:439–439
Dachir S, Shabashov D, Trembovler V, Alexandrovich AG, Benowitz L, Shohami E (2014) Inosine improves functional recovery after experimental traumatic brain injury. Brain Res 1555:78–88. https://doi.org/10.1016/j.brainres.2014.01.044
Teixeira FC, Gutierres JM, Soares MSP, de Mattos BDS, Spohr L, Do Couto CA, Bona N, Assmann C, Morsch V, Da Cruz I, Stefanello F, Spanevello RM (2020) Inosine protects against impairment of memory induced by experimental model of Alzheimer disease: a nucleoside with multitarget brain actions. Psychopharmacol 237:811–823. https://doi.org/10.1007/s00213-019-05419-5
Ellman G, Courtney K, Andres V, Feather-Stone R (1961) A new and rapid colorimetric determination of acetylcholinesterase activity. Biochem Pharmacol 7:88–95. https://doi.org/10.1016/0006-2952(61)90145-9
Huf F, Bandiera F, Müller C, Gea L, Carvalho F, Rahmeier F, Reiter K, Tortorelli L, Gomez R, Fernandes M (2019) Comparative study on the effects of cigarette smoke exposure, ethanol consumption and association: behavioral parameters, apoptosis, glial fibrillary acid protein and S100b immunoreactivity in different regions of the rat hippocampus. Alcohol 77:101–112. https://doi.org/10.1016/j.alcohol.2018.08.009
Gulyaeva NV, Bobkova NV, Kolosova NG, Samokhin AN, Stepanichev MY (2017) Molecular and cellular mechanisms of sporadic Alzheimer’s disease: studies on rodent models in vivo. Biochemistry 82:1088–1102. https://doi.org/10.1134/S0006297917100029
Grieb P (2016) Intracerebroventricular streptozotocin injections as a model of Alzheimer’s disease: in search of a relevant mechanism. Mol Neurobiol 53:1741–1752. https://doi.org/10.1007/s12035-015-9132-3
Salkovic-Petrisic M, Hoyer S (2007) Central insulin resistance as a trigger for sporadic Alzheimer-like pathology: an experimental approach. J Neural Transm Suppl 72:217–233. https://doi.org/10.1007/978-3-211-73574-9_28
Knezovic A, Osmanovic-Barilar J, Curlin M, Hof PR, Simic G, Riederer P, Salkovic-Petrisic M (2015) Staging of cognitive deficits and neuropathological and ultrastructural changes in streptozotocin-induced rat model of Alzheimer’s disease. J Neural Transm 122: 577–592. 0.1007/s00702–015–1394–4
Gutierres JM, Carvalho FB, Schetinger MRC, Marisco P, Agostinho P, RodriguesM RubinMA, Schmatz R, da Silva CR, de P Cognato G, Farias JG, Signor C, Morsch VM, Mazzanti CM, Bogo M, Bonan CD, Spanevello R, (2014) Anthocyanins restore behavioral and biochemical changes caused by streptozotocin-induced sporadic dementia of Alzheimer’s type. Life Sci 96:7–17. https://doi.org/10.1016/j.lfs.2013.11.014
Oliveira J, Abdalla F, Dornelles GL, Adefegha S, Palma TV, Signor C, Berbardi JS, Bladissarelli J, Lenz LS, Magni LP, Rubin MA, Pillat MM, Andrade CM (2016) Berberine proctects against memory impairment and anxiogenic-like behavior in rats submitted to sporadic Alzheimer’s like dementia: involvement of acetylcholinesterase and cell death. Neurotoxiclogy 57:241–250. https://doi.org/10.1016/j.neuro.2016.10.008
Gerzson MF, Bona NP, Soares MS, Teixeira FC, Rahmeier FL, Carvalho FB, Cruz MF, Onzi G, Lenz G, Gonçalves R, Spanevello R, Stefanello FM (2020) Tannic acid ameliorates STZ-induced Alzheimer’s disease-like impairment of memory, neuroinflammation, neuronal death and modulates Akt expression. Neurot Res 37:1009–1017. https://doi.org/10.1007/s12640-020-00167-3
Gomez G, Sitkovsky MV (2003) Differential requirement for A2a and A3 adenosine receptors for the protective effect of inosine in vivo. Blood 102:4472–4478. https://doi.org/10.1182/blood-2002-11-3624
Stockwell J, Jakova E, Cayabyab FS (2017) Adenosine A1 and A2A receptors in the brain: current research and their role in neurodegeneration. Molecules 22:676. https://doi.org/10.3390/molecules22040676
Pagnussat N, Almeida AS, Marques DM, Nunes F, Chenet GC, Botton PHS (2015) Adenosine A2A receptors are necessary and sufficient to trigger memory impairment in adult mice. Br J Pharmacol 172:3831–3845. https://doi.org/10.1111/bph.13180
Silva A, Lemos C, Gonçalves F, Pilássova A, Machado N, Silva H, Canas P, Cunha R, Lopes J, Agostinho P (2018) Blockade of adenosine receptors recovers early deficits of memory and plasticity in the triple transgenic mouse modelo f Alzheimer’s disease. Neurobiol Dis 117:72–81. https://doi.org/10.1016/j.nbd.2018.05.024
El-Shamarka ME, Kozman MR, Messiha BA (2020) The protective effect of inosine against rotenone-induced Parkinson’s disease in mice; role of oxido-nitrosative stress, ERK phosphorylation, and A2AR expression. Naunyn-Schmiedeberg’s Arch Pharmacol 393:1041–1053. https://doi.org/10.1007/s00210-019-01804-1
Lu B, Nagappan G, Lu Y (2014) BDNF and synaptic plasticity, cognitive function, and dysfunction. Handb Exp Pharmacol 220:223–250. https://doi.org/10.1007/978-3-642-45106-5_9
Sebastião A, Assaife-Lopes N, Diógenes M, Vaz S, Ribeiro J (2011) Modulation of brain-derived neurotrophic fator (BDNF) actions in the nervous system by adenosine A (2A) receptors and the role of lipid rafts. Biochim Biophys Acta 1808:1340–1349. https://doi.org/10.1016/j.bbamem.2010.06.028
Tebano MT, Martire A, Potenza R, Pepponi R, Armida M, Domenici M, Schwarzchild M, Chen J, Popoli P (2008) Adenosine A(2A) receptors are required for normal BDNF levels and BDNF-induced potentiation of synaptic transmission in the mouse hippocampus. J Neurochem 104:279–286. https://doi.org/10.1111/j.1471-4159.2007.05046.x
Muto J, Lee H, Lee L, Uwaya A, Park J, Nakajima S, Nagata K, Ohno M, Ohsawa I, Mikami T (2014) Oral administration of inosine produces antidepressant-like effects in mice. Sci Rep 4:4199. https://doi.org/10.1038/srep04199
Tartaglia N, Du J, Tyler WJ, Neale E, Pozzo-Miller L, Lu B (2001) Protein synthesis-dependent and independent regulation of hippocampal synapses by brain derived neurotrophic factor. J Biol Chem 276:37585–37593. https://doi.org/10.1074/jbc.M101683200
Tarsa L, Goda Y (2002) Synaptophysin regulates activity-dependent synapse formation in cultured hippocampal neurons. Proc Natl Acad Sci 99:1012–1016. https://doi.org/10.1073/pnas.022575999
Kwon S, Chapman E (2011) Synaptophysin regulates the kinetics of synaptic vesicle endocytosis in central neurons. Neuron 70:847–854. https://doi.org/10.1016/j.neuron.2011.04.001
McMahon H, Bolshakov V, Hammer R, Siegelbaum S, Sudhof T (1996) Synaptophysin, a major synaptic vesicle protein, is not essential for neurotransmitter release. Proc Natl Acad Sci 93:4460–4764. https://doi.org/10.1073/pnas.93.10.4760
Sye C, Troncoso J, Kawas C, Peter M, Price D, Martin D (1997) Loss of the presynaptic vesicle protein synaptophysin in hippocampus correlates with cognitive decline in Alzheimer disease. J Neuropathol Exp Neurol 56:933–944. https://doi.org/10.1097/00005072-199708000-00011
Kesner R (2007) Behavioral functions of the CA3 subregion of the hippocampus. Leran Mem 14:771–778. https://doi.org/10.1101/lm.688207
Schwab C, McGeer PL (2008) Inflammatory aspects of Alzheimer disease and other neurodegenerative disorders. J Alzheimer’s Dis 13:359–369. https://doi.org/10.3233/jad-2008-13402
Gadani SP, Cronk JC, Norris GT, Kipnis J (2012) IL-4 in the brain: a cytokine to remember. J Immunol 189: 4213–4219. 0.4049/jimmunol.1202246
Gambi F, Reale M, Iarlori C, Salone A, Toma L, Paladini C (2004) Alzheimer patients treated with an AChE inhibitor show higher IL-4 and lower IL-1β levels and expression in peripheral blood mononuclear cells. J Clin Psychopharmacol 24:314–321. https://doi.org/10.1097/01.jcp.0000125683.74595.2f
Strle K, Zhou JH, Broussard SR, Venters HD, Johnson RW, Freund GG, Dantzer R, Kelley K (2002) IL-10 promotes survival of microglia without activating Akt. J Neuroimmunol 122:9–19. https://doi.org/10.1016/s0165-5728(01)00444-1
Rossi C, Cusimano M, Zambito M, Finardi A, Capotondo A, Garcia-Manteiga JM, Comi G, Martino G, Muzio M (2018) Interleukin 4 modulates microglia homeostasis and attenuates the early slowly progressive phase of amyotrophic lateral sclerosis. Cell Death Dis 9:1–16. https://doi.org/10.1038/s41419-018-0288-4
De Jonge WJ, Ulloa L (2007) The alpha7 nicotinic acetylcholine receptor as a pharmacological target for inflammation. Br J Pharmacol 151:915–929. https://doi.org/10.1038/sj.bjp.0707264
Das UN (2007). Acetylcholinesterase and butyrylcholinesterase as possible markers of low-grade systemic inflammation. Med Sci Monit 13: RA214-RA221.
Rao AA, Sridhar GR, Das UN (2007) Elevated butyrylcholinesterase and acetylcholinesterase may predict the development of type 2 diabetes mellitus and Alzheimer’s disease. Med Hypotheses 69:1272–1276. https://doi.org/10.1016/j.mehy.2007.03.032
Mushtaq G, Greig H, N, A Khan J, A Kamal M, (2014) Status of acetylcholinesterase and butyrylcholinesterase in Alzheimer’s disease and type 2 diabetes mellitus. CNS Neurol Disord Drug Targets 13:1432–1439. https://doi.org/10.2174/1871527313666141023141545
Li C, Zhao R, Gao K, Wei Z, Yin M, Lau L, Chui D, Yu A (2011) Astrocytes: implications for neuroinflammatory pathogenesis of Alzheimer’s disease. Curr Alzheimer Res 8:67–80. https://doi.org/10.2174/156720511794604543
Ben Haim L, Carrillo-de Sauvage MA, Ceyzériat K, Escartin C (2015) Elusive roles for reactive astrocytes in neurodegenerative diseases. Front Cellu Neurosci 9:278. https://doi.org/10.3389/fncel.2015.00278
Salkovic-Petrisic M, Knezovic A, Hoyer S, Riederer P (2013) What have we learned from the streptozotocin-induced animal model of sporadic Alzheimer’s disease, about the therapeutic strategies in Alzheimer’s research. J Neural Transm 120:233–252. https://doi.org/10.1007/s00702-012-0877-9
Shepardson NE, Shankar GM, Selkoe DJ (2011) Cholesterol level and statin use in Alzheimer disease: I. Review of epidemiological and preclinical studies. Arch Neurol 68:1239–1244. https://doi.org/10.1001/archneurol.2011.203
Ophir G, Amariglio N, Jacob-Hirsch J, Elkon R, Rechavi G, Michaelson DM (2005) Apolipoprotein E4 enhances brain inflammation by modulation of the NF-κB signaling cascade. Neurobiol Dis 20:709–718. https://doi.org/10.1016/j.nbd.2005.05.002
Lima D, Hacke ACM, Inaba J, Pessôa CA, Kerman K (2020) Electrochemical detection of specific interactions between apolipoprotein E isoforms and DNA sequences related to Alzheimer’s disease. Bioelectrochemistry 133:107447. https://doi.org/10.1016/j.bioelechem.2019.107447
Acknowledgements
The authors acknowledge the Conselho Nacional de Desenvolvimento Científico e Tecnológico and Fundação de Amparo à Pesquisa do Rio Grande do Sul. We would like to thank Editage (www.editage.com) for English language editing.
Funding
This study was funded by Fundação de Amparo à Pesquisa do Rio Grande do Sul (FAPERGS)—grant number: 19/2551–0001712-0). This study was also financed in part by the Coordenação de Aperfeiçoamento de Pessoal de Nível Superior, Brazil (CAPES—Finance code 001).
Author information
Authors and Affiliations
Contributions
Fernanda C. Teixeira, Jessié M. Gutierres, Mayara S.P. Soares: experimental design, animal treatment, memory behavior, biochemical analysis, statistical analysis, result interpretation, and manuscript preparation.
Eduardo B. Blödorn, William B. Domingues, Vinicius C. Farias: quantitative real-time polymerase chain reaction of BDNF and tyrosine receptor kinase B (TrkB).
Karine P. Reichert, Maria Rosa Chitolina: analysis of adenosine receptors.
Relber A. Gonçalves: cytokine analysis.
Adriana M. Zago, Fabiano B. Carvalho, Marilda C. Fernandes: histological analysis and immunoreactivity of glial fibrillary acid protein (GFAP) and synaptophysin.
Francieli M. Stefanello: experimental design and result interpretation.
Roselia M. Spanevello: experimental design, result interpretation, discussion, manuscript preparation, and funding.
Corresponding authors
Ethics declarations
Ethics Approval
The Committee of Ethics and Animal Experimentation of the Federal University of Pelotas, Brazil, under protocol number CEEA 4808–2017, approved all animal procedures. The use of animals was in accordance with the Brazilian Guidelines for the Care and Use of Animals in Scientific Research Activities (DBCA), which is in agreement with the National Council of Control of Animal Experimentation (CONCEA).
Consent to Participate
Not applicable.
Consent for Publication
Not applicable.
Conflicts of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Teixeira, F.C., Soares, M.S.P., Blödorn, E.B. et al. Investigating the Effect of Inosine on Brain Purinergic Receptors and Neurotrophic and Neuroinflammatory Parameters in an Experimental Model of Alzheimer’s Disease. Mol Neurobiol 59, 841–855 (2022). https://doi.org/10.1007/s12035-021-02627-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12035-021-02627-z