Abstract
Background
In recent years, scientific research has increasingly focused on Endocrine Disrupting Chemicals (EDCs) and demonstrated their relevant role in the functional impairment of endocrine glands. This induced regulatory authorities to ban some of these compounds and to carefully investigate others in order to prevent EDCs-related conditions. As a result, we witnessed a growing awareness and interest on this topic.
Aims
This paper aims to summarize current evidence regarding the detrimental effects of EDCs on pivotal endocrine glands like pituitary, thyroid and adrenal ones. Particularly, we directed our attention on the known and the hypothesized mechanisms of endocrine dysfunction brought by EDCs. We also gave a glimpse on recent findings from pioneering studies that could in the future shed a light on the pathophysiology of well-known, but poorly understood, endocrine diseases like hormone-producing adenomas.
Conclusions
Although intriguing, studies on endocrine dysfunctions brought by EDCs are challenging, in particular when investigating long-term effects of EDCs on humans. However, undoubtedly, it represents a new intriguing field of science research.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Background
Endocrine disrupting chemicals (EDCs) are defined as “exogenous chemicals or mixture of chemicals that interfere with any aspect of hormone action” [1]. Their extensive application in several fields (agricultural, industrial, residential and pharmaceutical), their ability to contaminate human body through virtually every route (inhalation, digestion and transdermal) [2, 3] and to accumulate even for years in the adipose tissue [4, 5], easily explains the danger that the chronic exposure, to even small doses, poses.
Given the complexity of the whole endocrine system and the variety of the involved substances, infinite are the possible levels interfered by EDCs: synthesis, secretion, transport, metabolism, or elimination of endogenous hormones [2, 6,7,8,9,10,11]. More recently, literature has focused on their supposed direct action on hormonal receptors and/or genomic expression [12]. Indeed, several mechanisms of action appear to be involved in endocrine disruption. They can act as total, partial, or inverted agonists or as antagonists for endocrine nuclear receptors [6, 10, 11], and even perform epigenetic changes, such as DNA methylation and/or acetylation and histone modifications [13, 14].
For comparable reasons, endocrine impairment induced by EDCs can express in a wide range of consequences: hormonal secretion, cell proliferation and cancer, growth, metabolism, sexual development, circadian clocks, and even, cognitive functions, neurodevelopment and behavior, mostly following recent literature on pre/postnatal exposure [1].
Indeed, several studies carried out during pregnancy and lactation, show that EDCs exert influence in both the exposed individual and in their offspring. Not only, EDCs damage during development, and not necessarily after conception, seems also able to transfer to future generations, through a process known as transgenerational inheritance [15].
All this can be explicated by the deleterious effects of EDCs on three of the main human endocrine axes: hypothalamus-pituitary, adrenal, and thyroid glands.
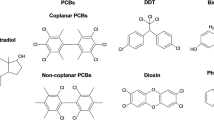
Table 1 presents some information about the main various substances you will find throughout this dissertation [16].
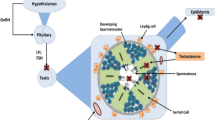
Pituitary gland
The pituitary gland is a potential target of EDCs, which can result in an alteration of the pituitary hormone-releasing patterns. The hypophysis seems to be vulnerable through direct and hypothalamic-mediated processes exerted by these compounds [1, 17]. However, EDCs mechanisms of action are still not fully figured out: over the entire lifespan of the individual, they could interfere with endogenous hormonal function, affecting the homeostatic system, or alter the genomic expression, e.g., through DNA methylation [1, 12].
A growing body of evidence is suggesting that EDCs can have an influence on tumorigenesis. Researchers described a link between EDCs and cancer burden, particularly with testicular, breast and prostate cancer [1]. Pituitary gland seems to be a potential target of these compounds, too. First epidemiological studies reported a higher incidence of pituitary adenomas due to previous exposure to dioxin [18] and a higher incidence of growth hormone- (GH-)secreting adenomas in a highly industrialized area nearby Messina, Italy [19]. Moreover, in vitro studies succeeded in demonstrating correlations between pollutants and stimulation of pituitary cells: benzene and phthalates increased cell proliferation via a deregulation of aryl hydrocarbon receptor (AHR) and AHR-interacting protein (AIP) [20], a tumor suppressor pathway that seems to be involved with other xenobiotics, such as polycyclic aromatic hydrocarbons and PCBs [21]. The involvement of AIP seems to play a key role: in fact, previous studies had already linked AIP gene mutations with familial isolated pituitary adenoma syndrome, familial somatotropinomas, and with apparently sporadic acromegaly [22, 23]. Moreover, in clinical practice AIP gene mutations are associated with an aggressive disease phenotype, which is less responsive to conventional medical treatment, as somatostatin analogues [19].
In addition, another influence of EDCs on the hypothalamic–pituitary–somatotropic axis can be hypothesized: an increase in GH secretion was reported for octyl- and nonyl-phenols, BPA [24], benzene, phthalates, and PCBs [25]. Furthermore, estrogens exert a direct stimulation of GH and prolactin (PRL) release [26, 27]; consequently, a potential increase in GH levels could be hypothesized for those EDCs with estrogenic activity, such as diethylstilbestrol and DDT [1].
Lactotroph cells also resulted to be susceptible to EDCs: the known estrogenic activity of BPA, and a similar activity performed by two pesticides (endosulphan and chlordane) seemed to induce PRL secretion both in vitro and in vivo [28,29,30]. Even metal ions with analogous endocrinological influence, the so-called “metalloestrogens” [31], such as lead and chromium, resulted to be positively associated with PRL release in humans [32,33,34]. However, this evidence resulted not to be conclusive: further studies documented that cadmium, mercury, molybdenum, and lead were inversely associated with PRL levels [34,35,36,37].
The impact made by EDCs on the hypothalamic-pituitary-thyroid axis is still unclear. In animals, reduced serum TSH and not univocal fT3 and fT4 responses were reported after exposition to pesticides and fungicides [38,39,40]; tributyltin chloride, however, was associated with increased TSH and diminished fT3 and fT4 serum levels [41, 42]. Even in humans, there were interesting findings: workers exposed to cadmium showed metal urinary concentrations to be directly correlated with serum TSH and inversely with fT3 and fT4 [43]. Furthermore, some studies demonstrated a lasting effect from mother to child: they reported a positive association between maternal and children blood levels of TSH and PFAS, PCBs, or dioxin [44,45,46], while BPA urinary levels in pregnant women resulted to be inversely associated with serum TSH, but not with fT3 and fT4 levels of newborns [47, 48].
Direct hypothalamic-pituitary-adrenal axis involvement with EDCs is still a matter of debate due to the lack of evidence, especially in human species. A few animal studies reported a direct suppression of this axis through a reduction in adrenocorticotrophic hormone (ACTH) and corticosterone levels after PCBs exposition [49], chiefly in female rats [50], or indirectly through reduction of hypothalamic corticosterone-releasing-factor mRNA [51]. BPA increased ACTH and corticosterone levels in male, but not in female rats [52].
Rising evidence outlines how EDCs can have implications for the neurohypophysis, which acts like a storage site of hypothalamic released hormone vasopressin (AVP) and oxytocin. In particular, in mammalians BPA peri-natal exposure was associated with upregulation of oxytocin release, both in males [53] and females [54] while no different number of oxytocin neurons was found after prenatal exposition to PCBs [55]. AVP function was reported to be influenced by BPA [54, 56] and PBDE exposure increased the number of AVP releasing neurons [57].
Wide is the literature about the influence of EDCs on hypothalamic-pituitary-gonadal axis. An intriguing subtopic is represented by puberty disruption. Puberty is a critical time orchestrated by a pulsatile release of hypothalamic gonadotropin-releasing hormone (GnRH) leading to an episodic systemic secretion of luteinizing hormone (LH) and follicle stimulating hormone (FSH) from the anterior pituitary gland [58]. This system is mainly regulated by hypothalamic kisspeptin neurons, which are usually inhibited during childhood [59]. These neurons and pituitary cells are sensitive to endocrine influences during fetal, neonatal, and juvenile development [60]. In literature, there are reports of early menarche in daughters of women exposed to pesticides and phytoestrogens [61, 62] and in girls consuming soy or exposed to PBDE [62,63,64] during infancy [65]. Finally, several animal models of EDCs exposure have confirmed their role on pubertal timing, even if the mechanisms of action are still not completely elucidated [66]. In mammalian, BPA seems to exert a stimulatory effect on kisspeptin-GnRH system [67,68,69] while other claim that BPA [70,71,72], PCBs [73], sewage sludge [74] can have an inhibitory effect. Moreover, mixed effects (BPA [75], PCBs [76], phthalates [77]) or no effect on kisspeptin-GnRH system are also reported [73].
Finally, it is intriguing to consider the perturbation exerted by EDCs on circadian rhythms, which synchronize cell functions with the external light-dark cycle. Circadian clocks are highly conserved, endogenous time-keeping mechanisms that generate self-sustained oscillations with an approximately 24-h period [78]. The main characters of this regulation system are the clock genes; in the anterior hypothalamus, they encode for transcription factor like BMAL-CLOCK1 [79] that drives rhythmic expression of many clock-controlled genes, even in humans [80]. Alterations of this daily pattern seem to have potential detrimental effects on human health, including infertility, cancer [80,81,82], and also disruption of pituitary hormone release patterns [81, 83,84,85,86]. In fact, exposure to cadmium can disrupt rhythmic 24-h release of PRL [87], BPA and dioxin can alter the expression of BMAL gene [88, 89] and even tributyltin seems to have a harmful effect on this system [90]. Moreover, gestational exposure to PCBs disrupted the normal BMAL expression pattern [91,92,93].
The systematic study of the whole series of alterations to the pituitary gland made by EDCs results to be challenging, due to the high complexity of this gland. As we have seen, the various hypothalamic-pituitary axes can be involved in varying degrees. In conclusion, it is still a matter of debate the comprehension of the entity of EDCs burden on the etiopathogenesis of pituitary diseases.
Thyroid gland
An extraordinary variety of substances can interfere with the normal functioning of the thyroid gland. Given the complexity of the hypothalamus-pituitary-thyroid axis, the great amount of involved mechanisms is not surprising.
Historically involved processes include the inhibition of the sodium/iodine symporter (NIS) and of the thyroid-peroxidase enzyme (TPO), widely described for some ions that pollute water basins (nitrates, perchlorates) and cigarette smoke (thiocyanate) [94]. These are, among other substances, known as goitrogens in light of their ability to increase the volume of the gland, through the proliferative stimulus of lower thyroid hormones (THs).
Recent studies showed how often pre/postnatal exposure to EDCs is consistently associated to children neurodevelopment impairment, and although conclusive evidence about specific differences for age and genders still lacks, some studies seem to point out a higher susceptibility in young boys and an effect lasting up to 7 years of age or even until adulthood [95, 96]. It is hard to pinpoint the precise mechanisms between endocrine disruption and neurodevelopmental outcome because most of these epidemiological studies lacked in complete endocrine profiles. It is well-known that THs are central in normal cerebral development. Even transient and mild hypothyroidism in pregnancy is also associated with cognitive/neurobehavioral in the offspring (e.g., 3.9 IQ score loss in association with maternal fT4 < 2.5 mUI/L) [97]. Consequently, it is absolutely established the causal burden of goitrogens. Yet, such an impairment does not always coincide with a strong negative correlation with serum levels of THs [95, 98,99,100,101]. This observation shifted the focus of research on a downstream action. Particularly, it is now recognized that some chemicals, mainly flame retardants (PCBs, PBDEs), plasticizers (phthalates, BPA) and certain pesticides, can directly interfere with thyroid hormone receptors (THRs) and their transcriptional activity at several levels, which also made them suspect of increasing the risk of thyroid cancer [102].
Studies suggested an association of prenatal and infantile exposure to PCBs with inferior IQs in children [103], but less consistent is the evidence about correlation with T4 and TSH levels [104]. Interestingly, PCBs seem to be among the few substances capable of directly interfere with THRs, which added to the transport-globulin mechanism, could explain the direct cortical antigrowth action [105, 106]. The same, with minor difference, can be said of PBDEs, the employment of which raised with the abandonment of PCBs, in the 80 s [102, 107,108,109].
Research has shown that phthalates carry out their anti-thyroid action via a by-product of a gram-negative bacteria processing, which behave as a TPO inhibitor. They were also classified as “possibly carcinogenic to human” (Class 2B) by IARC [102, 110].
Recent studies found that BPA has a negative correlation with T4 levels in several large population-based studies [111,112,113,114]. Its action can be associated to its binding with thyroxin binding globulin (TBG) and Transthyretin (TTR) [115], to the interference with THRs [116] and, moreover, to an increased the expression of Dio1 gene and Ugt1ab, and consequently to an augmented catabolism of TH [117, 118]. BPA is known to stimulate the proto-oncogenic estrogen receptor (mER) and to activate nuclear factor kB (NF-kB), a transcription factor involved in development of thyroid cancer. Yet, studies investigating the association with thyroid cancer are limited [119, 120].
Full comprehension of this process is still far from reach and there are multiple factors being suggested: expression of THRs (Phthalates and BPA [121, 122]), interaction of the complex Retinoid X receptor (RXR) and THR with T3-response elements (TREs) (PCB [123]), recruitment/release of corepressors (BPA [9]), T3 binding to receptor (PBDEs, phthalates [124, 125]) and recruitment of coactivators (PCBs [126]).
The extent of how far environment and chemicals can interfere with thyroid gland functioning will always be a puzzle, because of the infinite possible mechanisms and the challenge of reaching superior quality evidence. Thyroid should be an example, though, of how such topics can have a great clinical and practical rebound. It is, consequently, of primary importance to obtain full disclosure on this subject and to design increasingly rigorous studies. Researchers’ efforts should today focus on new and barely explored fields of study, like other mechanisms than the decrease in THs blood levels and especially on the direct effect on molecular pathways and the interference with DNA transcription.
Adrenal gland
The human adrenal gland is a complex endocrine organ that produces both steroid hormones (glucocorticoids, mineralocorticoids and androgens) and amino acid-derived hormones (epinephrine and norepinephrine). Adrenal functional impairment can lead to both insufficiency and overproduction of hormones eliciting Addison’s disease (primary hypo-adrenalism), Cushing’s syndrome (hypercortisolism), Conn’s disease (primary hyperaldosteronism) as well as adrenal androgen excess, which can have a role in premature adrenarche and adrenogenital syndromes in children and in hirsutism and infertility in women. For what refers to adrenal medulla, a catecholamine-secreting lesion (pheochromocytoma) may give rise to severe signs and symptoms because of the augmented sympathetic activity.
Sometimes hormones overproduction can underlie hormone-producing adenomas or carcinomas and might result from exposure to drugs or exogenous EDCs [127].
In fact, recearchers demonstrated that the adrenal gland is the most frequently observed site of endocrine lesions as it is particularly sensitive to toxic assault [128]. There is a wide number of chemicals with recorded in vitro and in vivo adrenal effects covering most of their classes: pesticides, plasticizers, dioxins, PCBs and polycyclic aromatic hydrocarbons [128,129,130,131,132,133].
For what refers to pathophysiology, these EDCs influence steroid biosynthesis and metabolism either as inhibitors or rarely as activators of key enzymes, or on the level of the respective enzyme expression.
As previously stated, the adrenal gland is particularly vulnerable to toxicants and there are several causes. First, there are multiple targets for toxicological assault such as receptors, transcription factors and enzymes [134]. For instance, hydroxysteroids dehydrogenases are targets for BPA that may affect their activity as well as their expression [135]. Another target are sulfotransferases that are inhibited by phthalates, chlorinated phenols and also by some phytoestrogens [136, 137].
Second, during steroid hydroxylation reactions, reactive oxygen species (ROS) are generated causing oxidative stress. It has been shown that imbalance in redox balance is implicated in impaired adrenal steroidogenesis and, more specifically, in several potentially lethal adrenal disorders including X-linked adrenoleukodystrophy, triple A syndrome and most recently familial glucocorticoid deficiency [138]. This imbalance can be brought up again by BPA causing the inhibition of the anti-oxidant enzymes superoxide dismutase, catalase, glutathione reductase, and glutathione peroxidase [139].
Third, the adrenal cortex has specific mechanisms for the selective uptake of lipoproteins, which are subsequently stored in the large pools of esterified lipid. Studies revealed that adrenal cells can take up and concentrate a wide number of toxic agents, including DDT metabolites, methacrylonitrile, and PCB metabolites. Particularly, it seems that these chemicals could remain inactive within the adrenal tissue until a period of particularly high demand for adrenal steroids, when they may be mobilized and cause damage [140,141,142].
Another important aspect is the potential of the adrenal gland for lipid peroxidation, due to the high content of unsaturated fatty acids in its membrane. This process is implicated in the toxic effects of carbon tetrachloride on this tissue [143].
In addition, researchers reported that unlike other vertebrates such as fish and birds, the human adrenal gland is highly vascularized, and this rich blood supply facilitates the delivery of toxins and metabolic substrates as well as the efficient removal of steroid products [144].
Moreover, this endocrine organ has a high content of enzymes of the CYP family that have the potential for bioactivation of toxins that can cause a relevant damage to the gland [145]. In particular, CYPs are well known as biocatalysts for the transformation of diverse pollutants, including pesticides and polycyclic aromatic hydrocarbons [146,147,148].
For the sake of completeness, it is necessary to highlight that current evidence of the influence of EDCs in the adrenal gland is mainly driven by studies focusing on the adrenal cortex. In fact, there are only a few studies on adrenal medulla reporting its impaired development in rats after pre-natal and post-natal exposure to DDT [149, 150].
Although the number of studies focusing on the effects of EDCs on animals is quite consistent, the evidence in humans is lacking. One reason for that is the low availability of human adrenal cells for researchers [145].
This is a crucial issue as studies demonstrated that there are several differences between the adrenal grands of animals and humans (anatomical, physiological, etc…). Moreover, even a partial impairment of proper adrenal function may have severe consequences on human health, a very challenging aspect to investigate in animals.
These subclinical and latent dysfunctions can be the result of the bioaccumulation of chemicals that might generate clinical effects only after several years of constant low-dose exposure [151]. In this light, recently researchers hypothesized that hormone-secreting adrenal adenomas could have a greater content of EDCs. A pioneering study by Fommei et al, despite being small-sized, reported a significantly higher concentration for α-, β-, and γ- Hexachlorocyclohexane (HCH) Hexachlorobenzene (HCB) and for PCBs in aldosterone-producing adenomas than in the normal cortex [152]. This aspect should be the focus of long-term ad hoc studies. Moreover, it is desirable a wider availability of human adrenal cells.
Conclusions
The striking results of scientific studies on EDCs and their detrimental effects on the endocrine system opened a new and intriguing field of research. In particular, investigators reported EDCs-related dysfunction of pituitary, thyroid and adrenal glands with supporting evidence. In recent years, researchers focused on the effects of bio-accumulation of chemicals and the possible role of this process on the formation of non-functioning or hormone-producing adenomas. However, we still require support for this hypothesis, so we encourage to conduct long-term ad hoc studies with a higher sample size. In addition, it is necessary to make human endocrine cells available for pre-clinical studies. Undoubtedly, we are just at the beginning of a long journey that will definitely give us new insights over the years. This research could prevent EDCs-related endocrine dysfunctions, providing robust evidence to the regulatory authorities to allow them to promote the use of safer compounds and to phase-out hazardous chemicals.
References
A.C. Gore, V.A. Chappell, S.E. Fenton, J.A. Flaws, A. Nadal, G.S. Prins, J. Toppari, R.T. Zoeller, EDC-2: the endocrine society’s second scientific statement on endocrine-disrupting chemicals. Endocr. Rev. 36, E1–E150 (2015). https://doi.org/10.1210/er.2015-1010
E.R. Kabir, M.S. Rahman, I. Rahman, A review on endocrine disruptors and their possible impacts on human health. Environ. Toxicol. Pharmacol. 40, 241–258 (2015). https://doi.org/10.1016/j.etap.2015.06.009
P. Balaguer, V. Delfosse, M. Grimaldi, W. Bourguet, Structural and functional evidences for the interactions between nuclear hormone receptors and endocrine disruptors at low doses. Comptes Rendus Biologies 340, 414–420 (2017). https://doi.org/10.1016/j.crvi.2017.08.002
J.J. Heindel, R. Newbold, T.T. Schug, Endocrine disruptors and obesity. Nat. Rev. Endocrinol. 11, 653–661 (2015). https://doi.org/10.1038/nrendo.2015.163
R.M. Sargis, Metabolic disruption in context: Clinical avenues for synergistic perturbations in energy homeostasis by endocrine disrupting chemicals. Endocr. Disruptors 3, e1080788 (2015). https://doi.org/10.1080/23273747.2015.1080788
W. Mnif, A.I.H. Hassine, A. Bouaziz, A. Bartegi, O. Thomas, B. Roig, Effect of endocrine disruptor pesticides: a review. Int. J. Environ. Res. Public. Health 8, 2265–2303 (2011). https://doi.org/10.3390/ijerph8062265
G.J. Nohynek, C.J. Borgert, D. Dietrich, K.K. Rozman, Endocrine disruption: Fact or urban legend? Toxicol. Lett. 223, 295–305 (2013). https://doi.org/10.1016/j.toxlet.2013.10.022
R. Kiyama, Y. Wada-Kiyama, Estrogenic endocrine disruptors: Molecular mechanisms of action. Environ. Int. 83, 11–40 (2015). https://doi.org/10.1016/j.envint.2015.05.012
K. Moriyama, T. Tagami, T. Usui, M. Naruse, T. Nambu, Y. Hataya, N. Kanamoto, Y. Li, A. Yasoda, H. Arai, K. Nakao, Antithyroid drugs inhibit thyroid hormone receptor-mediated transcription. J. Clin. Endocrinol. Metab. 92, 1066–1072 (2007). https://doi.org/10.1210/jc.2006-1621
S.de Coster, N.van Larebeke,, Endocrine-disrupting chemicals: associated disorders and mechanisms of action. J. Environ. Public Health 2012, 1–52 (2012). https://doi.org/10.1155/2012/713696
T.T. Schug, A. Janesick, B. Blumberg, J.J. Heindel, Endocrine disrupting chemicals and disease susceptibility. J. Steroid Biochem. Mol. Biol. 127, 204–215 (2011). https://doi.org/10.1016/j.jsbmb.2011.08.007
A.M. Zama, M. Uzumcu, Epigenetic effects of endocrine-disrupting chemicals on female reproduction: An ovarian perspective. Front. Neuroendocrinol. 31, 420–439 (2010). https://doi.org/10.1016/j.yfrne.2010.06.003
C. Monneret, What is an endocrine disruptor? Comptes Rendus Biologies 340, 403–405 (2017). https://doi.org/10.1016/j.crvi.2017.07.004
F. Baldi, A. Mantovani, A new database for food safety: EDID (endocrine disrupting chemicals–diet interaction database). Reprod. Toxicol. 26, 57 (2008). https://doi.org/10.1016/j.reprotox.2008.05.005
K. Svensson, E. Tanner, C. Gennings, C. Lindh, H. Kiviranta, S. Wikström, C.-G. Bornehag, Prenatal exposures to mixtures of endocrine disrupting chemicals and children’s weight trajectory up to age 5.5 in the SELMA study. Sci. Rep. 11, 11036 (2021). https://doi.org/10.1038/s41598-021-89846-5
Agency for Toxic Substances and Disease Registry. Available at https://www.atsdr.cdc.gov/. [Accessed April 10, 2022].
A. Gore, Neuroendocrine targets of endocrine disruptors. HORMONES 9, 16–27 (2010). https://doi.org/10.14310/horm.2002.1249
A.C. Pesatori, D. Consonni, M. Rubagotti, P. Grillo, P.A. Bertazzi, Cancer incidence in the population exposed to dioxin after the “Seveso accident”: twenty years of follow-up. Environ. Health 8, 39 (2009). https://doi.org/10.1186/1476-069X-8-39
S. Cannavò, F. Ferraù, M. Ragonese, L. Curtò, M.L. Torre, M. Magistri, A. Marchese, A. Alibrandi, F. Trimarchi, Increased prevalence of acromegaly in a highly polluted area. Eur. J. Endocrinol. 163, 509–513 (2010). https://doi.org/10.1530/EJE-10-0465
L. Tapella, A. Sesta, M.F. Cassarino, V. Zunino, M.G. Catalano, F.P. Giraldi, Benzene and 2-ethyl-phthalate induce proliferation in normal rat pituitary cells. Pituitary 20, 311–318 (2017). https://doi.org/10.1007/S11102-016-0777-3
S. Cannavo, F. Trimarchi, F. Ferraù, Acromegaly, genetic variants of the aryl hydrocarbon receptor pathway and environmental burden. Mol. Cell. Endocrinol. 457, 81–88 (2017). https://doi.org/10.1016/j.mce.2016.12.019
C. Lloyd, A. Grossman, The AIP (aryl hydrocarbon receptor-interacting protein) gene and its relation to the pathogenesis of pituitary adenomas. Endocrine 46, 387–396 (2014). https://doi.org/10.1007/s12020-013-0125-6
L.C. Hernández-Ramírez, P. Gabrovska, J. Dénes, K. Stals, G. Trivellin, D. Tilley, F. Ferraù, J. Evanson, S. Ellard, A.B. Grossman, F. Roncaroli, M.R. Gadelha, M. Korbonits, A. Agha, S.A. Akker, E.D. Aflorei, S. Alföldi, W. Arlt, B. Atkinson, A. Aulinas-Masó, S.J. Aylwin, P.F. Backeljauw, C. Badiu, S. Baldeweg, G. Bano, A. Barkan, J. Barwell, C. Bernal-González, G.M. Besser, J.S. Bevan, J. Blair, P. Bouloux, L. Bradley, M. Buchfelder, M. Cakir, N. Canham, P. Carroll, H.S. Chahal, T. Cheetham, F. Chentli, R.N. Clayton, M. Cohen, T. Cole, H. Courtney, E. Crowne, D. Cuthbertson, J. Dal, N. Dalantaeva, C. Daousi, K. Darzy, M. Dattani, J.H. Davies, J. Davis, M. de Castro, L. de Marinis, W. Drake, P. Dutta, L. Dzeranova, B. Edén-Engström, R. Eeles, M. Elfving, M. Elston, L. Emmerson, N. Fersht, S. Fica, S. Fischli, D. Flanagan, M. Fleseriu, P.U. Freda, T. Friedman, L.A. Frohman, P. Gallego, E. Gevers, E. Gláz, J.A. Goldman, A.P. Goldstone, M. Goth, L. Greenhalgh, J. Grieve, M. Guitelman, A. Gürlek, M. Gurnell, K. Horvath, T.A. Howlett, C. Höybye, S. Hunter, D. Iacovazzo, P. Igaz, W.J. Inder, T. Iwata, L. Izatt, S. Jagadeesh, G. Kaltsas, F. Kaplan, N. Karavitaki, D. Kastelan, M. Katz, T. Kearney, B. Khoo, C. Kiraly-Borri, R. Knispelis, G.L. Kovács, A.V. Kumar, E.R. Laws, R.M. Lechan, M.J. Levy, K. Lewandowski, J. Lo, N. Maartens, A. Matsuno, B. McGowan, S.E. McQuaid, M. Medic-Stojanoska, M. Mercado-Atri, E. Mezősi, D. Miljic, K.K. Miller, S. Modenesi, M.E. Molitch, J. Monson, D.G. Morris, P.J. Morrison, A. Munir, R.D. Murray, M. Musat, N. Musolino, L. Nachtigall, J. Newell-Price, A. Ogilvie, S.M. Orme, I. Paşcanu, A. Patócs, C. Patterson, S.H. Pearce, F. Pecori Giraldi, M. Pfeifer, V. Popovic, N. Poplawski, M. Powell, P. Pullan, R. Quinton, S. Radian, H. Randeva, A. Ribeiro-Oliveira, C. Rodd, F. Ryan, R. Salvatori, C. Schöfl, D. Shears, K. Shotliff, B.S. Soares, N. Somasundaram, A. Spada, J. Sperber, H.A. Spoudeas, S. Stewart, H. Storr, C. Strasburger, M.E. Street, F. Swords, R.V. Thakker, E. Tham, C. Thompson, D.M.O. Thorner, M. Tóth, P.J. Trainer, S. Tsagarakis, M. Tzanela, J. Vadász, V. Vaks, R. Verkauskiene, J.A. Wass, S.M. Webb, A. Weber, S. Yamada, S. Yarman, P. Yeoh, K. Yoshimoto, N.N. Zammitt, Landscape of familial isolated and young-onset pituitary adenomas: prospective diagnosis in AIP mutation carriers. J. Clin. Endocrinol. Metab. 100, e1242–e1254 (2015). https://doi.org/10.1210/jc.2015-1869
V.H. Dang, T.H. Nguyen, G.S. Lee, K.C. Choi, E.B. Jeung, In vitro exposure to xenoestrogens induces growth hormone transcription and release via estrogen receptor-dependent pathways in rat pituitary GH3 cells. Steroids 74, 707–714 (2009). https://doi.org/10.1016/j.steroids.2009.03.002
N. Fortunati, F. Guaraldi, V. Zunino, F. Penner, V. D’Angelo, F. Zenga, F.P. Giraldi, M.G. Catalano, E. Arvat, Effects of environmental pollutants on signaling pathways in rat pituitary GH3 adenoma cells. Environ. Res. 158, 660–668 (2017). https://doi.org/10.1016/j.envres.2017.07.015
J. Simard, J.-F. Hubert, T. Hosseinzadeh, F. Labrie, Stimulation of growth hormone release and synthesis by estrogens in rat anterior pituitary cells in culture. Endocrinology 119, 2004–2011 (1986). https://doi.org/10.1210/endo-119-5-2004
Y. Iwasaki, M. Morishita, M. Asai, A. Onishi, M. Yoshida, Y. Oiso, K. Inoue, Effects of hormones targeting nuclear receptors on transcriptional regulation of the growth hormone gene in the MtT/S rat somatotrope cell line. Neuroendocrinology 79, 229–236 (2004). https://doi.org/10.1159/000078787
R. Steinmetz, N.G. Brown, D.L. Allen, R.M. Bigsby, N. Ben-Jonathan, The environmental estrogen bisphenol a stimulates prolactin release in vitro and in vivo*. Endocrinology 138, 1780–1786 (1997). https://doi.org/10.1210/endo.138.5.5132
T.-Y. Chun, J. Gorski, High concentrations of bisphenol a induce cell growth and prolactin secretion in an estrogen-responsive pituitary tumor cell line. Toxicol. Appl. Pharmacol. 162, 161–165 (2000). https://doi.org/10.1006/taap.1999.8840
J. Rousseau, L. Cossette, S. Grenier, M.G. Martinoli, Modulation of prolactin expression by xenoestrogens. Gen. Comp. Endocrinol. 126, 175–182 (2002). https://doi.org/10.1006/gcen.2002.7789
K. Jurkowska, E.M. Kratz, E. Sawicka, A. Piwowar, The impact of metalloestrogens on the physiology of male reproductive health as a current problem of the XXI century. J. Physiol. Pharmacol. 70, 337–355 (2019). https://doi.org/10.26402/jpp.2019.3.02
R. Lucchini, E. Albini, I. Cortesi, D. Placidi, E. Bergamaschi, F. Traversa, L. Alessio, Assessment of neurobehavioral performance as a function of current and cumulative occupational lead exposure. Neurotoxicology 21, 805–811 (2000)
S. Govoni, F. Battaini, C. Fernicola, L. Castelletti, M. Trabucchi, Plasma prolactin concentrations in lead exposed workers. J. Environ. Pathol. Toxicol. Oncol. 7, 13–15 (n.d.).
J.D. Meeker, M.G. Rossano, B. Protas, M.P. Diamond, E. Puscheck, D. Daly, N. Paneth, J.J. Wirth, Multiple metals predict prolactin and thyrotropin (TSH) levels in men. Environ. Res. 109, 869–873 (2009). https://doi.org/10.1016/j.envres.2009.06.004
S. Telišman, B. Čolak, A. Pizent, J. Jurasović, P. Cvitković, Reproductive toxicity of low-level lead exposure in men. Environ. Res. 105, 256–266 (2007). https://doi.org/10.1016/j.envres.2007.05.011
C. de Burbure, J.-P. Buchet, A. Leroyer, C. Nisse, J.-M. Haguenoer, A. Mutti, Z. Smerhovský, M. Cikrt, M. Trzcinka-Ochocka, G. Razniewska, M. Jakubowski, A. Bernard, Renal and neurologic effects of cadmium, lead, mercury, and arsenic in children: evidence of early effects and multiple interactions at environmental exposure levels. Environ. Health Perspect. 114, 584–590 (2006). https://doi.org/10.1289/ehp.8202
L. Takser, D. Mergler, J. Lafond, Very low level environmental exposure to lead and prolactin levels during pregnancy. Neurotoxicology Teratol. 27, 505–508 (2005). https://doi.org/10.1016/j.ntt.2005.03.009
A. Laisi, R. Tuominen, P. Männistö, K. Savolainen, J. Mattila, The Effect of Maneb, Zineb, and Ethylenethiourea on the Humoral Activity of the Pituitary-Thyroid Axis in Rat. in (1985), pp. 253–258.
S.P. Pandey, B. Mohanty, The neonicotinoid pesticide imidacloprid and the dithiocarbamate fungicide mancozeb disrupt the pituitary–thyroid axis of a wildlife bird. Chemosphere 122, 227–234 (2015). https://doi.org/10.1016/J.CHEMOSPHERE.2014.11.061
H.J. Sun, H.B. Li, P. Xiang, X. Zhang, L.Q. Ma, Short-term exposure of arsenite disrupted thyroid endocrine system and altered gene transcription in the HPT axis in zebrafish. Environ. Pollut. 205, 145–152 (2015). https://doi.org/10.1016/J.ENVPOL.2015.05.037
S. Sharan, K. Nikhil, P. Roy, Disruption of thyroid hormone functions by low dose exposure of tributyltin: An in vitro and in vivo approach. Gen. Comp. Endocrinol. 206, 155–165 (2014). https://doi.org/10.1016/J.YGCEN.2014.07.027
A.P. Santos-Silva, M.N. Andrade, P. Pereira-Rodrigues, F.D. Paiva-Melo, P. Soares, J.B. Graceli, G.R.M. Dias, A.C.F. Ferreira, D.P. de Carvalho, L. Miranda-Alves, Frontiers in endocrine disruption: Impacts of organotin on the hypothalamus-pituitary-thyroid axis. Mol. Cell. Endocrinol. 460, 246–257 (2018). https://doi.org/10.1016/J.MCE.2017.07.038
M.V. Rosati, L. Montuori, T. Caciari, C. Sacco, M. Marrocco, G. Tomei, B. Scala, A. Sancini, V. Anzelmo, S. Bonomi, F. Tomei, Correlation between urinary cadmium and thyroid hormones in outdoor workers exposed to urban stressors. Toxicol. Ind. Health 32, 1978–1986 (2016). https://doi.org/10.1177/0748233715602833
V. Ballesteros, O. Costa, C. Iñiguez, T. Fletcher, F. Ballester, M.J. Lopez-Espinosa, Exposure to perfluoroalkyl substances and thyroid function in pregnant women and children: A systematic review of epidemiologic studies. Environ. Int. 99, 15–28 (2017). https://doi.org/10.1016/J.ENVINT.2016.10.015
C. Koopman-Esseboom, D.C. Morse, N. Weisglas-Kuperus, I.J. Lutkeschipholt, C.G. van der Paauw, L.G.M.T. Tuinstra, A. Brouwer, P.J.J. Sauer, Effects of dioxins and polychlorinated biphenyls on thyroid hormone status of pregnant women and their infants. Pediatr. Res. 36, 468–473 (1994). https://doi.org/10.1203/00006450-199410000-00009
L. Hagmar, Polychlorinated biphenyls and thyroid status in humans: a review. Thyroid 13, 1021–1028 (2003). https://doi.org/10.1089/105072503770867192
M.E. Romano, G.M. Webster, A.M. Vuong, R.T. Zoeller, A. Chen, A.N. Hoofnagle, A.M. Calafat, M.R. Karagas, K. Yolton, B.P. Lanphear, J.M. Braun, Gestational urinary bisphenol A and maternal and newborn thyroid hormone concentrations: The HOME Study. Environ. Res. 138, 453–460 (2015). https://doi.org/10.1016/J.ENVRES.2015.03.003
J. Chevrier, R.B. Gunier, A. Bradman, N.T. Holland, A.M. Calafat, B. Eskenazi, K.G. Harley, Maternal urinary bisphenol a during pregnancy and maternal and neonatal thyroid function in the CHAMACOS study. Environ. Health Perspect. 121, 138–144 (2013). https://doi.org/10.1289/ehp.1205092
L.A. Meserve, B.A. Murray, J.A. Landis, Influence of maternal ingestion of Aroclor 1254® (PCB) or Firemaster BP-6® (PBB) on unstimulated and stimulated corticosterone levels in young rats. Bull. Environ. Contamination Toxicol., 48, (1992). https://doi.org/10.1007/BF00195992.
M.P. Reilly, C.D. Weeks, V.Y. Topper, L.M. Thompson, D. Crews, A.C. Gore, The effects of prenatal PCBs on adult social behavior in rats. Hormones Behav. 73, 47–55 (2015). https://doi.org/10.1016/j.yhbeh.2015.06.002
R. Salgado-Freiría, S. López-Doval, A. Lafuente, Perfluorooctane sulfonate (PFOS) can alter the hypothalamic–pituitary–adrenal (HPA) axis activity by modifying CRF1 and glucocorticoid receptors. Toxicol. Lett. 295, 1–9 (2018). https://doi.org/10.1016/J.TOXLET.2018.05.025
F. Chen, L. Zhou, Y. Bai, R. Zhou, L. Chen, Sex differences in the adult HPA axis and affective behaviors are altered by perinatal exposure to a low dose of bisphenol A. Brain Res. 1571, 12–24 (2014). https://doi.org/10.1016/j.brainres.2014.05.010
J.T. Wolstenholme, J.A. Taylor, S.R.J. Shetty, M. Edwards, J.J. Connelly, E.F. Rissman, Gestational exposure to low dose bisphenol A alters social behavior in juvenile mice. PLoS ONE 6, e25448 (2011). https://doi.org/10.1371/journal.pone.0025448
A.W. Sullivan, E.C. Beach, L.A. Stetzik, A. Perry, A.S. D’Addezio, B.S. Cushing, H.B. Patisaul, A novel model for neuroendocrine toxicology: neurobehavioral effects of BPA exposure in a prosocial species, the Prairie Vole (Microtus ochrogaster). Endocrinology 155, 3867–3881 (2014). https://doi.org/10.1210/en.2014-1379
M.P. Reilly, M.N. Kunkel, L.M. Thompson, A. Zentay, C.D. Weeks, D. Crews, L.K. Cormack, A.C. Gore, Effects of endocrine‐disrupting chemicals on hypothalamic oxytocin and vasopressin systems. J. Exp. Zool. Part. A: Ecol. Integr. Physiol. 337, 75–87 (2022). https://doi.org/10.1002/jez.2475
J.A. Goldsby, J.T. Wolstenholme, E.F. Rissman, Multi- and transgenerational consequences of bisphenol A on sexually dimorphic cell populations in mouse brain. Endocrinology 158, 21–30 (2017). https://doi.org/10.1210/en.2016-1188
A. Shah, C.G. Coburn, A. Watson-Siriboe, R. Whitley, A. Shahidzadeh, E.R. Gillard, R. Nichol, M. Leon-Olea, M. Gaertner, P.R.S. Kodavanti, M.C. Currás-Collazo, Altered cardiovascular reactivity and osmoregulation during hyperosmotic stress in adult rats developmentally exposed to polybrominated diphenyl ethers (PBDEs). Toxicol. Appl. Pharmacol. 256, 103–113 (2011). https://doi.org/10.1016/j.taap.2011.07.014
M.M. Grumbach, The neuroendocrinology of human puberty revisited. Horm. Res. Paediatrics 57, 2–14 (2002). https://doi.org/10.1159/000058094
A. Acevedo‐Rodriguez, A.S. Kauffman, B.D. Cherrington, C.S. Borges, T.A. Roepke, M. Laconi, Emerging insights into hypothalamic‐pituitary‐gonadal axis regulation and interaction with stress signalling. J. Neuroendocrinol. 30, (2018). https://doi.org/10.1111/jne.12590.
T.A. Roepke, N.C. Sadlier, Reproductive Toxicology: Impact of endocrine disruptors on neurons expressing GnRH or kisspeptin and pituitary gonadotropins. Reproduction 162, F131–F145 (2021). https://doi.org/10.1530/REP-20-0612
C. Wohlfahrt-Veje, H.R. Andersen, I.M. Schmidt, L. Aksglaede, K. Sørensen, A. Juul, T.K. Jensen, P. Grandjean, N.E. Skakkebaek, K.M. Main, Early breast development in girls after prenatal exposure to non-persistent pesticides. Int. J. Androl. 35, 273–282 (2012). https://doi.org/10.1111/j.1365-2605.2011.01244.x
K.J. Marks, T.J. Hartman, E.V. Taylor, M.E. Rybak, K. Northstone, M: Marcus, Exposure to phytoestrogens in utero and age at menarche in a contemporary British cohort. Environ. Res. 155, 287–293 (2017). https://doi.org/10.1016/j.envres.2017.02.030
K.G. Harley, S.A. Rauch, J. Chevrier, K. Kogut, K.L. Parra, C. Trujillo, R.H. Lustig, L.C. Greenspan, A. Sjödin, A. Bradman, B. Eskenazi, Association of prenatal and childhood PBDE exposure with timing of puberty in boys and girls. Environ. Int. 100, 132–138 (2017). https://doi.org/10.1016/j.envint.2017.01.003
G.C. Windham, S.M. Pinney, R.W. Voss, A. Sjödin, F.M. Biro, L.C. Greenspan, S. Stewart, R.A. Hiatt, L.H. Kushi, Brominated flame retardants and other persistent organohalogenated compounds in relation to timing of puberty in a longitudinal study of girls. Environ. Health Perspect. 123, 1046–1052 (2015). https://doi.org/10.1289/ehp.1408778
D. Franssen, T. Svingen, D.L. Rodriguez, M. Duursen, J. van, Boberg, A.S. Parent, A putative adverse outcome pathway network for disrupted female pubertal onset to improve testing and regulation of endocrine disrupting chemicals. Neuroendocrinology 112, 101–114 (2022). https://doi.org/10.1159/000515478
D. Lopez-Rodriguez, R. Scientist, D. Franssen, I.B. Science, S. Heger, P. Endocrinologist, A.-S. Parent, Endocrine-disrupting chemicals and their effects on puberty. Best. Pract. Res.: Clin. Endocrinol. Metab. 35, 101579 (2021). https://doi.org/10.1016/J.BEEM.2021.101579
W. Xi, C.K.F. Lee, W.S.B. Yeung, J.P. Giesy, M.H. Wong, X. Zhang, M. Hecker, C.K.C. Wong, Effect of perinatal and postnatal bisphenol A exposure to the regulatory circuits at the hypothalamus–pituitary–gonadal axis of CD-1 mice. Reprod. Toxicol. 31, 409–417 (2011). https://doi.org/10.1016/j.reprotox.2010.12.002
Y. Bai, F. Chang, R. Zhou, P.-P. Jin, H. Matsumoto, M. Sokabe, L. Chen, Increase of anteroventral periventricular kisspeptin neurons and generation of E2-induced LH-surge system in male rats exposed perinatally to environmental dose of bisphenol-A. Endocrinology 152, 1562–1571 (2011). https://doi.org/10.1210/en.2010-1042
L. Naulé, M. Picot, M. Martini, C. Parmentier, H. Hardin-Pouzet, M. Keller, I. Franceschini, S. Mhaouty-Kodja, Neuroendocrine and behavioral effects of maternal exposure to oral bisphenol A in female mice. J. Endocrinol. 220, 375–388 (2014). https://doi.org/10.1530/JOE-13-0607
H.B. Patisaul, K.L. Todd, J.A. Mickens, H.B. Adewale, Impact of neonatal exposure to the ERα agonist PPT, bisphenol-A or phytoestrogens on hypothalamic kisspeptin fiber density in male and female rats. NeuroToxicology 30, 350–357 (2009). https://doi.org/10.1016/j.neuro.2009.02.010
S.M. Losa-Ward, K.L. Todd, K.A. McCaffrey, K. Tsutsui, H.B. Patisaul, Disrupted Organization of RFamide Pathways in the Hypothalamus Is Associated with Advanced Puberty in Female Rats Neonatally Exposed to Bisphenol A1. Biol. Reprod. 87, (2012). https://doi.org/10.1095/biolreprod.112.100826.
F. Ruiz-Pino, D. Miceli, D. Franssen, M.J. Vazquez, A. Farinetti, J.M. Castellano, G. Panzica, M. Tena-Sempere, Environmentally Relevant Perinatal Exposures to Bisphenol A Disrupt Postnatal Kiss1/NKB Neuronal Maturation and Puberty Onset in Female Mice. Environ. Health Perspect. 127, (2019). https://doi.org/10.1289/EHP5570.
S.M. Dickerson, S.L. Cunningham, H.B. Patisaul, M.J. Woller, A.C. Gore, Endocrine disruption of brain sexual differentiation by developmental PCB exposure. Endocrinology 152, 581–594 (2011). https://doi.org/10.1210/en.2010-1103
M. Bellingham, P.A. Fowler, M.R. Amezaga, S.M. Rhind, C. Cotinot, B. Mandon-Pepin, R.M. Sharpe, N.P. Evans, Exposure to a complex cocktail of environmental endocrine-disrupting compounds disturbs the kisspeptin/GPR54 system in ovine hypothalamus and pituitary gland. Environ. Health Perspect. 117, 1556–1562 (2009). https://doi.org/10.1289/ehp.0900699
S.M. Dickerson, S.L. Cunningham, A.C. Gore, Prenatal PCBs disrupt early neuroendocrine development of the rat hypothalamus. Toxicol. Appl. Pharmacol. 252, 36–46 (2011). https://doi.org/10.1016/j.taap.2011.01.012
D.M. Walker, B.A. Kermath, M.J. Woller, A.C. Gore, Disruption of reproductive aging in female and male rats by gestational exposure to estrogenic endocrine disruptors. Endocrinology 154, 2129–2143 (2013). https://doi.org/10.1210/en.2012-2123
J. Hu, G. Du, W. Zhang, H. Huang, D. Chen, D. Wu, X. Wang, Short-term neonatal/prepubertal exposure of dibutyl phthalate (DBP) advanced pubertal timing and affected hypothalamic kisspeptin/GPR54 expression differently in female rats. Toxicology 314, 65–75 (2013). https://doi.org/10.1016/j.tox.2013.09.007
J.A. Mohawk, C.B. Green, J.S. Takahashi, Central and peripheral circadian clocks in mammals. Annu. Rev. Neurosci. 35, 445–462 (2012). https://doi.org/10.1146/annurev-neuro-060909-153128
A. Sehgal, Physiology flies with time. Cell 171, 1232–1235 (2017). https://doi.org/10.1016/j.cell.2017.11.028
A. Sen, M.T. Sellix, The circadian timing system and environmental circadian disruption: From follicles to fertility. Endocrinology 157, 3366–3373 (2016). https://doi.org/10.1210/en.2016-1450
K. Ikegami, S. Refetoff, Evan Cauter, T. Yoshimura, Interconnection between circadian clocks and thyroid function. Nat. Rev. Endocrinol. 15, 590–600 (2019). https://doi.org/10.1038/S41574-019-0237-Z
N.M. Kettner, C.A. Katchy, L. Fu, Circadian gene variants in cancer. Ann. Med. 46, 208 (2014). https://doi.org/10.3109/07853890.2014.914808
S.-H. Yoo, S. Yamazaki, P.L. Lowrey, K. Shimomura, C.H. Ko, E.D. Buhr, S.M. Siepka, H.-K. Hong, W.J. Oh, O.J. Yoo, M. Menaker, J.S. Takahashi, PERIOD2::LUCIFERASE real-time reporting of circadian dynamics reveals persistent circadian oscillations in mouse peripheral tissues. Proc. Natl Acad. Sci. 101, 5339–5346 (2004). https://doi.org/10.1073/pnas.0308709101
A.M. Neumann, C.X. Schmidt, R.M. Brockmann, H. Oster, Circadian regulation of endocrine systems. Autonomic Neurosci.: Basic. Clin. 216, 1–8 (2019). https://doi.org/10.1016/j.autneu.2018.10.001
G.M. Leclerc, F.R. Boockfor, Pulses of prolactin promoter activity depend on a noncanonical E-box that can bind the circadian proteins CLOCK and BMAL1. Endocrinology 146, 2782–2790 (2005). https://doi.org/10.1210/en.2005-0100
S.A. Patel, A. Chaudhari, R. Gupta, N. Velingkaar, R.V. Kondratov, Circadian clocks govern calorie restriction—mediated life span extension through BMAL1‐ and IGF‐1‐dependent mechanisms. FASEB J. 30, 1634–1642 (2016). https://doi.org/10.1096/fj.15-282475
V. Jiménez-Ortega, P.C. Barquilla, P. Fernández-Mateos, D.P. Cardinali, A.I. Esquifino, Cadmium as an endocrine disruptor: correlation with anterior pituitary redox and circadian clock mechanisms and prevention by melatonin. Free. Radic. Biol. Med. 53, 2287–2297 (2012). https://doi.org/10.1016/J.FREERADBIOMED.2012.10.533
N. Loganathan, A. Salehi, J.A. Chalmers, D.D. Belsham, Bisphenol A alters Bmal1, Per2, and Rev-Erba mRNA and requires Bmal1 to increase neuropeptide Y expression in hypothalamic neurons. Endocrinology 160, 181–192 (2019). https://doi.org/10.1210/en.2018-00881
M. Mukai, T.M. Lin, R.E. Peterson, P.S. Cooke, S.A. Tischkau, Behavioral rhythmicity of mice lacking AhR and attenuation of light-induced phase shift by 2,3,7,8-tetrachlorodibenzo-p-dioxin. J. Biol. Rhythm. 23, 200–210 (2008). https://doi.org/10.1177/0748730408316022
R. Kopp, I.O. Martínez, J. Legradi, J. Legler, Exposure to endocrine disrupting chemicals perturbs lipid metabolism and circadian rhythms. J. Environ. Sci. 62, 133–137 (2017). https://doi.org/10.1016/j.jes.2017.10.013
D.M. Walker, B.M. Goetz, A.C. Gore, Dynamic postnatal developmental and sex-specific neuroendocrine effects of prenatal polychlorinated biphenyls in rats. Mol. Endocrinol. 28, 99–115 (2014). https://doi.org/10.1210/me.2013-1270
M.R. Bell, L.M. Thompson, K. Rodriguez, A.C. Gore, Two-hit exposure to polychlorinated biphenyls at gestational and juvenile life stages: 1. Sexually dimorphic effects on social and anxiety-like behaviors. Hormones Behav. 78, 168–177 (2016). https://doi.org/10.1016/j.yhbeh.2015.11.007
N. Kiliç, S. Sandal, N. Çolakoglu, S. Kutlu, A. Seyran, B. Yilmaz, Endocrine disruptive effects of polychlorinated biphenyls on the thyroid gland in female rats. Tohoku J. Exp. Med. 206, 327–332 (2005). https://doi.org/10.1620/tjem.206.327
L.E. Braverman, X. He, S. Pino, M. Cross, B. Magnani, S.H. Lamm, M.B. Kruse, A. Engel, K.S. Crump, J.P. Gibbs, The effect of perchlorate, thiocyanate, and nitrate on thyroid function in workers exposed to perchlorate long-term. J. Clin. Endocrinol. Metab. 90, 700–706 (2005). https://doi.org/10.1210/jc.2004-1821
K.G. Harley, R.B. Gunier, K. Kogut, C. Johnson, A. Bradman, A.M. Calafat, B. Eskenazi, Prenatal and early childhood bisphenol A concentrations and behavior in school-aged children. Environ. Res. 126, 43–50 (2013). https://doi.org/10.1016/j.envres.2013.06.004
E.F. Fitzgerald, S. Shrestha, M.I. Gomez, R.J. McCaffrey, E.A. Zimmerman, K. Kannan, S. Hwang, Polybrominated diphenyl ethers (PBDEs), polychlorinated biphenyls (PCBs) and neuropsychological status among older adults in New York. NeuroToxicology 33, 8–15 (2012). https://doi.org/10.1016/j.neuro.2011.10.011
D. Levie, T.I.M. Korevaar, S.C. Bath, A. Dalmau-Bueno, M. Murcia, M. Espada, M. Dineva, J.M. Ibarluzea, J. Sunyer, H. Tiemeier, M. Rebagliato, M.P. Rayman, R.P. Peeters, M. Guxens, Thyroid function in early pregnancy, child IQ, and autistic traits: a meta-analysis of individual participant data. J. Clin. Endocrinol. Metab. 103, 2967–2979 (2018). https://doi.org/10.1210/jc.2018-00224
O. Boucher, G. Muckle, J.L. Jacobson, R.C. Carter, M. Kaplan-Estrin, P. Ayotte, É. Dewailly, S.W. Jacobson, Domain-specific effects of prenatal exposure to PCBs, mercury, and lead on infant cognition: results from the environmental contaminants and child development study in Nunavik. Environ. Health Perspect. 122, 310–316 (2014). https://doi.org/10.1289/ehp.1206323
Y. Kim, E. Ha, E. Kim, H. Park, M. Ha, J. Kim, Y. Hong, N. Chang, B. Kim, Prenatal exposure to phthalates and infant development at 6 months: prospective mothers and children’s environmental health (MOCEH) study. Environ. Health Perspect. 119, 1495–1500 (2011). https://doi.org/10.1289/ehp.1003178
A. Chen, K. Yolton, S.A. Rauch, G.M. Webster, R. Hornung, A. Sjödin, K.N. Dietrich, B.P. Lanphear, Prenatal polybrominated diphenyl ether exposures and neurodevelopment in U.S. children through 5 years of age: the HOME study. Environ. Health Perspect. 122, 856–862 (2014). https://doi.org/10.1289/ehp.1307562
N. el Majidi, M. Bouchard, G. Carrier, Systematic analysis of the relationship between standardized biological levels of polychlorinated biphenyls and thyroid function in pregnant women and newborns. Chemosphere 98, 1–17 (2014). https://doi.org/10.1016/j.chemosphere.2013.10.006
International Agency for Research on Cancer Classifications. Available at https://monographs.iarc.who.int/agents-classified-by-the-iarc/. [Accessed April 7, 2022].
P.W. Stewart, E. Lonky, J. Reihman, J. Pagano, B.B. Gump, T. Darvill, The relationship between prenatal PCB exposure and intelligence (IQ) in 9-year-old children. Environ. Health Perspect. 116, 1416–1422 (2008). https://doi.org/10.1289/ehp.11058
M.S. Bloom, J.E. Vena, J.R. Olson, P.J. Kostyniak, Assessment of polychlorinated biphenyl congeners, thyroid stimulating hormone, and free thyroxine among New York State anglers. Int. J. Hyg. Environ. Health 212, 599–611 (2009). https://doi.org/10.1016/j.ijheh.2009.04.005
W. Miyazaki, T. Iwasaki, A. Takeshita, C. Tohyama, N. Koibuchi, Identification of the functional domain of thyroid hormone receptor responsible for polychlorinated biphenyl–mediated suppression of its action in vitro. Environ. Health Perspect. 116, 1231–1236 (2008). https://doi.org/10.1289/ehp.11176
K.J. Gauger, S. Giera, D.S. Sharlin, R. Bansal, E. Iannacone, R.T. Zoeller, Polychlorinated biphenyls 105 and 118 form thyroid hormone receptor agonists after cytochrome P4501A1 activation in rat pituitary GH3 cells. Environ. Health Perspect. 115, 1623–1630 (2007). https://doi.org/10.1289/ehp.10328
J.B. Herbstman, A. Sjödin, M. Kurzon, S.A. Lederman, R.S. Jones, V. Rauh, L.L. Needham, D. Tang, M. Niedzwiecki, R.Y. Wang, F. Perera, Prenatal exposure to PBDEs and neurodevelopment. Environ. Health Perspect. 118, 712–719 (2010). https://doi.org/10.1289/ehp.0901340
A. Julander, M. Karlsson, K. Hagström, C.G. Ohlson, M. Engwall, I.-L. Bryngelsson, H. Westberg, B. van Bavel, Polybrominated diphenyl ethers—plasma levels and thyroid status of workers at an electronic recycling facility. Int. Arch. Occup. Environ. Health 78, 584–592 (2005). https://doi.org/10.1007/s00420-005-0627-5
M.E. Turyk, V.W. Persky, P. Imm, L. Knobeloch, R. Chatterton, H.A. Anderson, Hormone disruption by PBDEs in adult male sport fish consumers. Environ. Health Perspect. 116, 1635–1641 (2008). https://doi.org/10.1289/ehp.11707
E. Gaitan, R.C. Cooksey, D. Matthews, R. Presson, In vitro measurement of antithyroid compounds and environmental Goitrogens. J. Clin. Endocrinol. Metab. 56, 767–773 (1983). https://doi.org/10.1210/jcem-56-4-767
J.D. Meeker, K.K. Ferguson, Relationship between urinary phthalate and bisphenol A concentrations and serum thyroid measures in U.S. adults and adolescents from the national health and nutrition examination survey (NHANES) 2007–2008. Environ. Health Perspect. 119, 1396–1402 (2011). https://doi.org/10.1289/ehp.1103582
C. Park, W. Choi, M. Hwang, Y. Lee, S. Kim, S. Yu, I. Lee, D. Paek, K. Choi, Associations between urinary phthalate metabolites and bisphenol A levels, and serum thyroid hormones among the Korean adult population - Korean National Environmental Health Survey (KoNEHS) 2012–2014. Sci. Total. Environ. 584–585, 950–957 (2017). https://doi.org/10.1016/j.scitotenv.2017.01.144
C. Sriphrapradang, L. Chailurkit, W. Aekplakorn, B. Ongphiphadhanakul, Association between bisphenol A and abnormal free thyroxine level in men. Endocrine 44, 441–447 (2013). https://doi.org/10.1007/s12020-013-9889-y
T. Wang, J. Lu, M. Xu, Y. Xu, M. Li, Y. Liu, X. Tian, Y. Chen, M. Dai, W. Wang, S. Lai, Y. Bi, G. Ning, Urinary Bisphenol A Concentration and Thyroid Function in Chinese Adults. Epidemiology 24, 295–302 (2013). https://doi.org/10.1097/EDE.0b013e318280e02f
G.R. Marchesini, A. Meimaridou, W. Haasnoot, E. Meulenberg, F. Albertus, M. Mizuguchi, M. Takeuchi, H. Irth, A.J. Murk, Biosensor discovery of thyroxine transport disrupting chemicals. Toxicol. Appl. Pharmacol. 232, 150–160 (2008). https://doi.org/10.1016/j.taap.2008.06.014
M.L. Jugan, M. Lévy-Bimbot, M. Pomérance, S. Tamisier-Karolak, J.P. Blondeau, Y. Lévi, A new bioluminescent cellular assay to measure the transcriptional effects of chemicals that modulate the alpha-1 thyroid hormone receptor. Toxicol. Vitr. 21, 1197–1205 (2007). https://doi.org/10.1016/j.tiv.2007.03.020
M.M. da Silva, C.F.L. Gonçalves, L. Miranda-Alves, R.S. Fortunato, D.P. Carvalho, A.C.F. Ferreira, Inhibition of type 1 iodothyronine deiodinase by bisphenol A. Horm. Metab. Res. 51, 671–677 (2019). https://doi.org/10.1055/a-0919-3879
S. Lee, C. Kim, H. Shin, Y. Kho, K. Choi, Comparison of thyroid hormone disruption potentials by bisphenols A, S, F, and Z in embryo-larval zebrafish. Chemosphere 221, 115–123 (2019). https://doi.org/10.1016/j.chemosphere.2019.01.019
D. Cuomo, I. Porreca, G. Cobellis, R. Tarallo, G. Nassa, G. Falco, A. Nardone, F. Rizzo, M. Mallardo, C. Ambrosino, Carcinogenic risk and Bisphenol A exposure: A focus on molecular aspects in endoderm derived glands. Mol. Cell. Endocrinol. 457, 20–34 (2017). https://doi.org/10.1016/j.mce.2017.01.027
D. Gentilcore, I. Porreca, F. Rizzo, E. Ganbaatar, E. Carchia, M. Mallardo, M. de Felice, C. Ambrosino, Bisphenol A interferes with thyroid specific gene expression. Toxicology 304, 21–31 (2013). https://doi.org/10.1016/j.tox.2012.12.001
S. Iwamuro, M. Yamada, M. Kato, S. Kikuyama, Effects of bisphenol A on thyroid hormone-dependent up-regulation of thyroid hormone receptor α and β and down-regulation of retinoid X receptor γ in Xenopus tail culture. Life Sci. 79, 2165–2171 (2006). https://doi.org/10.1016/j.lfs.2006.07.013
S. Sugiyama, N. Shimada, H. Miyoshi, K. Yamauchi, Detection of thyroid system–disrupting chemicals using in vitro and in vivo screening assays in Xenopus laevis. Toxicological Sci. 88, 367–374 (2005). https://doi.org/10.1093/toxsci/kfi330
A.I. Castillo, R. Sánchez-Martínez, J.L. Moreno, O.A. Martínez-Iglesias, D. Palacios, A. Aranda, A permissive retinoid X receptor/thyroid hormone receptor heterodimer allows stimulation of prolactin gene transcription by thyroid hormone and 9-cis-retinoic acid. Mol. Cell. Biol. 24, 502–513 (2004). https://doi.org/10.1128/MCB.24.2.502-513.2004
S. Kitamura, S. Shinohara, E. Iwase, K. Sugihara, N. Uramaru, H. Shigematsu, N. Fujimoto, S. Ohta, Affinity for thyroid hormone and estrogen receptors of hydroxylated polybrominated diphenyl ethers. J. Health Sci. 54, 607–614 (2008). https://doi.org/10.1248/jhs.54.607
S. Kitamura, T. Kato, M. Iida, N. Jinno, T. Suzuki, S. Ohta, N. Fujimoto, H. Hanada, K. Kashiwagi, A. Kashiwagi, Anti-thyroid hormonal activity of tetrabromobisphenol A, a flame retardant, and related compounds: Affinity to the mammalian thyroid hormone receptor, and effect on tadpole metamorphosis. Life Sci. 76, 1589–1601 (2005). https://doi.org/10.1016/j.lfs.2004.08.030
A.C. Bianco, D. Salvatore, B. Gereben, M.J. Berry, P.R. Larsen, Biochemistry, cellular and molecular biology, and physiological roles of the iodothyronine selenodeiodinases. Endocr. Rev. 23, 38–89 (2002). https://doi.org/10.1210/edrv.23.1.0455
K. Nanba, A.R. Blinder, W.E. Rainey, Primary cultures and cell lines for “in vitro” modeling of the human adrenal cortex. Tohoku J. Exp. Med. 253, 217–232 (2021). https://doi.org/10.1620/tjem.253.217
W. Ribelin, The effects of drugs and chemicals upon the structure of the adrenal gland. Fundamental Appl. Toxicol. 4, 105–119 (1984). https://doi.org/10.1016/0272-0590(84)90224-0
S. Szabo, I. Lippe, Th.: Adrenal gland: chemically induced structural and functional changes in the cortex. Toxicol. Pathol. 17, 317–329 (1989). https://doi.org/10.1177/019262338901700208
J.T. Sanderson, The steroid hormone biosynthesis pathway as a target for endocrine-disrupting chemicals. Toxicological Sci. 94, 3–21 (2006). https://doi.org/10.1093/toxsci/kfl051
S.A. Whitehead, S. Rice, Endocrine-disrupting chemicals as modulators of sex steroid synthesis. Best. Pract. Res. Clin. Endocrinol. Metab. 20, 45–61 (2006). https://doi.org/10.1016/j.beem.2005.09.003
K.Svechnikov, G.Izzo, L.Landreh, J.Weisser, O.Söder,, Endocrine disruptors and leydig cell function. J. Biomed. Biotechnol 2010, 1–10 (2010). https://doi.org/10.1155/2010/684504
E.C. Bonefeld-Jørgensen, M. Long, M.V. Hofmeister, A.M. Vinggaard, Endocrine-disrupting potential of bisphenol A, bisphenol A dimethacrylate, 4- n -nonylphenol, and 4- n -octylphenol in vitro: new data and a brief review. Environ. Health Perspect. 115, 69–76 (2007). https://doi.org/10.1289/ehp.9368
J.P. Hinson, P.W. Raven, Adrenal toxicology. In Endocrine and Hormonal Toxicology, edited by K.C. Rush (Wiley, 1999), pp. 67–90.
J. Guo, X. Yuan, L. Qiu, W. Zhu, C. Wang, G. Hu, Y. Chu, L. Ye, Y. Xu, R.-S. Ge, Inhibition of human and rat 11β-hydroxysteroid dehydrogenases activities by bisphenol A. Toxicol. Lett. 215, 126–130 (2012). https://doi.org/10.1016/j.toxlet.2012.10.002
R.H. Waring, S. Ayers, A.J. Gescher, H.-R. Glatt, W. Meinl, P. Jarratt, C.J. Kirk, T. Pettitt, D. Rea, R.M. Harris, Phytoestrogens and xenoestrogens: The contribution of diet and environment to endocrine disruption. J. Steroid Biochem. Mol. Biol. 108, 213–220 (2008). https://doi.org/10.1016/j.jsbmb.2007.09.007
R. Harris, R. Waring, Sulfotransferase inhibition: potential impact of diet and environmental chemicals on steroid metabolism and drug detoxification. Curr. Drug. Metab. 9, 269–275 (2008). https://doi.org/10.2174/138920008784220637
R. Prasad, J.C. Kowalczyk, E. Meimaridou, H.L. Storr, L.A. Metherell, Oxidative stress and adrenocortical insufficiency. J. Endocrinol. 221, R63–R73 (2014). https://doi.org/10.1530/JOE-13-0346
R. Meli, A. Monnolo, C. Annunziata, C. Pirozzi, M.C. Ferrante, Oxidative stress and BPA toxicity: an antioxidant approach for male and female reproductive dysfunction. Antioxidants 9, 405 (2020). https://doi.org/10.3390/antiox9050405
B.-O. Lund, Å. Bergman, I. Brandt, Metabolic activation and toxicity of a DDT-metabolite, 3-methylsulphonyl-DDE, in the adrenal Zona fasciculata in mice. Chem.-Biol. Interact. 65, 25–40 (1988). https://doi.org/10.1016/0009-2797(88)90028-2
A. Ahmed, Comparative disposition of acrylonitrile and methacrylonitrile: quantitative whole-body autoradiographic studies in rats. Fundamental Appl. Toxicol. 33, 49–59 (1996). https://doi.org/10.1006/faat.1996.0142
I. Brandt, Å. Bergman, PCB methyl sulphones and related compounds: identification of target cells and tissues in different species. Chemosphere 16, 1671–1676 (1987). https://doi.org/10.1016/0045-6535(87)90147-0
W. Brogan, Effects of carbon tetrachloride on adrenocortical structure and function in guinea pigs. Toxicol. Appl. Pharmacol. 75, 118–127 (1984). https://doi.org/10.1016/0041-008X(84)90082-6
G. Vinson, J. Hinson, Blood flow and hormone secretion in the adrenal gland. In The Adrenal Gland, edited by V. James (Raven Press, 1992), pp. 71–86.
J.P. Hinson, P.W. Raven, Effects of endocrine-disrupting chemicals on adrenal function. Best. Pract. Res. Clin. Endocrinol. Metab. 20, 111–120 (2006). https://doi.org/10.1016/j.beem.2005.09.006
K. Alejo-González, E. Hanson-Viana, R. Vazquez-Duhalt, Enzymatic detoxification of organophosphorus pesticides and related toxicants. J. Pestic. Sci. 43, 1–9 (2018). https://doi.org/10.1584/jpestics.D17-078
A.O. Docea, L. Vassilopoulou, D. Fragou, A.L. Arsene, C. Fenga, L. Kovatsi, D. Petrakis, V.N. Rakitskii, A.E. Nosyrev, B.N. Izotov, K.S. Golokhvast, A.M. Zakharenko, A. Vakis, C. Tsitsimpikou, N. Drakoulis, CYP polymorphisms and pathological conditions related to chronic exposure to organochlorine pesticides. Toxicol. Rep. 4, 335–341 (2017). https://doi.org/10.1016/j.toxrep.2017.05.007
H. Yamazaki, T. Shimada, M.V. Martin, F.P. Guengerich, Stimulation of cytochrome P450 reactions by Apo-cytochromeb 5. J. Biol. Chem. 276, 30885–30891 (2001). https://doi.org/10.1074/jbc.M105011200
N.V. Yaglova, E.P. Timokhina, V.V. Yaglov, S.S. Obernikhin, S.V. Nazimova, D.A. Tsomartova, Changes in histophysiology of the adrenal medulla in rats after prenatal and postnatal exposure to endocrine disruptor DDT. Bull. Exp. Biol. Med. 169, 398–400 (2020). https://doi.org/10.1007/s10517-020-04895-6
E.P. Timokhina, S.V. Nazimova, D.A. Tsomartova, N.V. Yaglova, S.S. Obernikhin, V.V. Yaglov, Morphological and cytophysiological changes in the adult rat adrenal medulla after prenatal and postnatal exposure to endocrine-disrupting DDT. Sovremennye Tehnologii v. Med. 12, 50 (2020). https://doi.org/10.17691/stm2020.12.2.06
R.M. Sargis, Metabolic disruption in context: Clinical avenues for synergistic perturbations in energy homeostasis by endocrine disrupting chemicals. Endocr. Disruptors 3, e1080788 (2015). https://doi.org/10.1080/23273747.2015.1080788
E. Fommei, R. Turci, A. Ripoli, S. Balzan, F. Bianchi, L. Morelli, A. Coi, Evidence for persistent organochlorine pollutants in the human adrenal cortex. J. Appl. Toxicol. 37, 1091–1097 (2017). https://doi.org/10.1002/jat.3460
Funding
Open access funding provided by Università degli Studi di Torino within the CRUI-CARE Agreement.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Writing – original draft preparation: F.E., L.M., and M.R.. Critical revision: G.M., N.P., R.R.G., L.P., S.G., R.G., Supervision: R.G. and S.G.. All authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Egalini, F., Marinelli, L., Rossi, M. et al. Endocrine disrupting chemicals: effects on pituitary, thyroid and adrenal glands. Endocrine 78, 395–405 (2022). https://doi.org/10.1007/s12020-022-03076-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-022-03076-x