Abstract
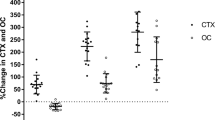
To assess if altered bone turnover following bariatric surgery is related to metabolic consequences of the surgical procedure or weight loss. We evaluated serum markers reflecting bone turnover and metabolic pathways at baseline and after 1-year in a controlled non-randomized clinical trial comparing Roux-en-Y gastric bypass surgery (n = 74) with lifestyle intervention (n = 63) on obesity-related comorbidities. The decrease in body mass index (BMI) was larger in the surgery (−14.0 kg/m2) compared to lifestyle (−3.7 kg/m2). Markedly increased bone turnover was observed following surgery compared to lifestyle intervention and was correlated with change in BMI. Stepwise multivariable regression analysis revealed that group (β = 0.31, p < 0.01), and changes in BMI (β = −0.28, p < 0.01), dickkopf-1 (β = 0.20, p < 0.001) and sclerostin (β = 0.11, p < 0.05) were predictors of change in the bone resorption marker N-terminal telopeptide. Our data support that mechanisms related to the procedure itself and changes in secreted Wnt antagonists may contribute to increased bone turnover following bariatric surgery.




Similar content being viewed by others
References
E.W. Yu, Bone metabolism after bariatric surgery. J. Bone Miner. Res. 29, 1507–1518 (2014)
M.P. Hage, F.G. El-Hajj, Bone and mineral metabolism in patients undergoing Roux-en-Y gastric bypass. Osteoporos. Int. 25, 423–439 (2014)
E.M. Stein, S.J. Silverberg, Bone loss after bariatric surgery: causes, consequences, and management. Lancet Diab. Endocrinol. 2, 165–174 (2014)
W.J. Pories, Bariatric surgery: risks and rewards. J. Clin. Endocrinol. Metab. 93, S89–S96 (2008)
E.W. Yu, M.L. Bouxsein, M.S. Putman, E.L. Monis, A.E. Roy, J.S. Pratt, W.S. Butsch, J.S. Finkelstein, Two-year changes in bone density after Roux-en-Y gastric bypass surgery. J. Clin. Endocrinol. Metab. 100, 1452–1459 (2015)
A.H. Maghrabi, K. Wolski, B. Abood, A. Licata, C. Pothier, D.L. Bhatt, S. Nissen, S.A. Brethauer, J.P. Kirwan, P.R. Schauer, S.R. Kashyap, Two-year outcomes on bone density and fracture incidence in patients with T2DM randomized to bariatric surgery versus intensive medical therapy. Obesity 23, 2344–2348 (2015)
K.M. Nakamura, E.G. Haglind, J.A. Clowes, S.J. Achenbach, E.J. Atkinson, L.J. Melton III, K.A. Kennel, Fracture risk following bariatric surgery: a population-based study. Osteoporos. Int. 25, 151–158 (2014)
A. Lalmohamed, F. de Vries, M.T. Bazelier, A. Cooper, T.P. van Staa, C. Cooper, N.C. Harvey, Risk of fracture after bariatric surgery in the United Kingdom: population based, retrospective cohort study. BMJ 345, e5085 (2012)
S. Ahlin, M. Peltonen, L. Anveden, P. Jacobson, K. Sjôholm, P.A. Svensson, I. Larsson, I. Nâslund, L. Sjôstrôm, L.M. Carlsson, Bariatric surgery increases the risk of osteoporosis and fractures in women in the Swedish Obese Subjects study. Obes. Facts 8(Suppl 1), 50–51 (2015)
S. Ikramuddin, C.J. Billington, W.J. Lee, J.P. Bantle, A.J. Thomas, J.E. Connett, D.B. Leslie, W.B. Inabnet III, R.W. Jeffery, K. Chong, L.M. Chuang, M.G. Sarr, M.D. Jensen, A. Vella, L. Ahmed, K. Belani, J.L. Schone, A.E. Olofson, H.A. Bainbridge, P.S. Laqua, Q. Wang, J. Korner, Roux-en-Y gastric bypass for diabetes (the Diabetes Surgery Study): 2-year outcomes of a 5-year, randomised, controlled trial. Lancet Diab. Endocrinol. 3, 413–422 (2015)
M.M. Brzozowska, A. Sainsbury, J.A. Eisman, P.A. Baldock, J.R. Center, Bariatric surgery, bone loss, obesity and possible mechanisms. Obes. Rev. 14, 52–67 (2013)
C. Muschitz, R. Kocijan, C. Marterer, A.R. Nia, G.K. Muschitz, H. Resch, P. Pietschmann, Sclerostin levels and changes in bone metabolism after bariatric surgery. J. Clin. Endocrinol. Metab. 100, 891–901 (2015)
S. Savastano, S.C. Di, L. Barrea, A. Colao, The complex relationship between obesity and the somatropic axis: the long and winding road. Growth Hormon. IGF Res. 24, 221–226 (2014)
G. Karsenty, F. Oury, The central regulation of bone mass, the first link between bone remodeling and energy metabolism. J. Clin. Endocrinol. Metab. 95, 4795–4801 (2010)
E. Biver, C. Salliot, C. Combescure, L. Gossec, P. Hardouin, I. Legroux-Gerot, B. Cortet, Influence of adipokines and ghrelin on bone mineral density and fracture risk: a systematic review and meta-analysis. J. Clin. Endocrinol. Metab. 96, 2703–2713 (2011)
D. Hofso, N. Nordstrand, L.K. Johnson, T.I. Karlsen, H. Hager, T. Jenssen, J. Bollerslev, K. Godang, R. Sandbu, J. Roislien, J. Hjelmesaeth, Obesity-related cardiovascular risk factors after weight loss: a clinical trial comparing gastric bypass surgery and intensive lifestyle intervention. Eur. J. Endocrinol. 163, 735–745 (2010)
M. Malone, Recommended nutritional supplements for bariatric surgery patients. Ann. Pharmacother. 42, 1851–1858 (2008)
K. Abegg, N. Gehring, C.A. Wagner, A. Liesegang, M. Schiesser, M. Bueter, T.A. Lutz, Roux-en-Y Gastric bypass surgery reduces bone mineral density and induces metabolic acidosis in rats. Am. J. Physiol. Regul. Integr. Comp. Physiol. 305, R999–R1009 (2013)
A.G. Robling, A.B. Castillo, C.H. Turner, Biomechanical and molecular regulation of bone remodeling. Annu. Rev. Biomed. Eng. 8, 455–498 (2006)
C.S. Riedt, R.E. Brolin, R.M. Sherrell, M.P. Field, S.A. Shapses, True fractional calcium absorption is decreased after Roux-en-Y gastric bypass surgery. Obesity 14, 1940–1948 (2006)
N.A. Sims, T.J. Martin, Coupling the activities of bone formation and resorption: a multitude of signals within the basic multicellular unit. Bonekey Rep. 3, 481 (2014)
A.G. Robling, P.J. Niziolek, L.A. Baldridge, K.W. Condon, M.R. Allen, I. Alam, S.M. Mantila, J. Gluhak-Heinrich, T.M. Bellido, S.E. Harris, C.H. Turner, Mechanical stimulation of bone in vivo reduces osteocyte expression of Sost/sclerostin. J. Biol. Chem. 283, 5866–5875 (2008)
A.R. Wijenayaka, M. Kogawa, H.P. Lim, L.F. Bonewald, D.M. Findlay, G.J. Atkins, Sclerostin stimulates osteocyte support of osteoclast activity by a RANKL-dependent pathway. PLoS One 6, e25900 (2011)
K. Fujita, S. Janz, Attenuation of WNT signaling by DKK-1 and -2 regulates BMP2-induced osteoblast differentiation and expression of OPG, RANKL and M-CSF. Mol. Cancer 6, 71 (2007)
Y.W. Qiang, Y. Chen, N. Brown, B. Hu, J. Epstein, B. Barlogie, J.D. Shaughnessy Jr, Characterization of Wnt/beta-catenin signalling in osteoclasts in multiple myeloma. Br. J. Haematol. 148, 726–738 (2010)
L. Pederson, M. Ruan, J.J. Westendorf, S. Khosla, M.J. Oursler, Regulation of bone formation by osteoclasts involves Wnt/BMP signaling and the chemokine sphingosine-1-phosphate. Proc. Natl. Acad. Sci. USA 105, 20764–20769 (2008)
T. Ueland, N.C. Olarescu, A.P. Jorgensen, K. Otterdal, P. Aukrust, K. Godang, T. Lekva, J. Bollerslev, Increased serum and bone matrix levels of the secreted Wnt antagonist DKK-1 in patients with growth hormone deficiency in response to growth hormone treatment. J. Clin. Endocrinol. Metab. 100, 736–743 (2015)
R. Armamento-Villareal, C. Sadler, N. Napoli, K. Shah, S. Chode, D.R. Sinacore, C. Qualls, D.T. Villareal, Weight loss in obese older adults increases serum sclerostin and impairs hip geometry but both are prevented by exercise training. J. Bone Miner. Res. 27, 1215–1221 (2012)
A.G. Costa, S. Cremers, E. Dworakowski, M. Lazaretti-Castro, J.P. Bilezikian, Comparison of two commercially available ELISAs for circulating sclerostin. Osteoporos. Int. 25, 1547–1554 (2014)
C. Muschitz, R. Kocijan, J. Haschka, A. Zendeli, T. Pirker, C. Geiger, A. Muller, B. Tschinder, A. Kocijan, C. Marterer, A. Nia, G.K. Muschitz, H. Resch, P. Pietschmann, The impact of vitamin D, calcium, protein supplementation, and physical exercise on bone metabolism after bariatric surgery: the BABS study. J. Bone Miner. Res. (2015). doi:10.1002/jbmr.2707
H.Z. Ke, W.G. Richards, X. Li, M.S. Ominsky, Sclerostin and Dickkopf-1 as therapeutic targets in bone diseases. Endocr. Rev. 33, 747–783 (2012)
Funding
This research did not receive any specific grant from any funding agency in the public, commercial or not-for-profit sector.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Informed consent
The regional ethics committee of the Southern Norway Regional Health Authority approved the study. Written informed consent was provided by all participants including permission to perform laboratory analysis.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Hofsø, D., Bollerslev, J., Sandbu, R. et al. Bone resorption following weight loss surgery is associated with treatment procedure and changes in secreted Wnt antagonists. Endocrine 53, 313–321 (2016). https://doi.org/10.1007/s12020-016-0903-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-016-0903-z