Abstract
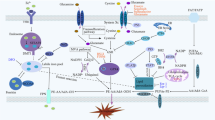
Plasma non-transferrin-bound iron (NTBI) exists when the plasma iron content exceeds the carrying capacity of transferrin and can be quickly cleared by the liver, pancreas, and other organs. However, whether it could enter the small intestine and its effects still remain unclear. Herein, these issues were explored. Mice were intravenously administrated of ferric citrate (treatment) or citrate acid (control) 10 min after the saturation of the transferrin. Two hours later, hepatic, duodenal, and jejunal iron content and distribution were measured and duodenal transcriptome sequencing was performed. Significant increase of duodenal and hepatic iron content was detected, indicating that plasma NTBI could be absorbed by the duodenum as well as the liver. A total of 103 differentially expressed genes were identified in the duodenum of mice in the treatment group compared to the control group. Gene Ontology (GO) functional analysis of these genes showed that they were mainly involved in defense response to virus and immune response. The results of Kyoto Encyclopedia of Genes and Genomes pathway (KEGG) analysis revealed that there were major changes in the hematopoietic cell lineage and some virus infection pathways between the two groups. Determination of 7 cytokines in the duodenum were further conducted, which demonstrated that the anti-inflammatory factors interferon (IL)-4 and IL-10 in the duodenum were significantly decreased after NTBI uptake. Our findings revealed that NTBI in plasma can enter the duodenum, which would change the duodenal hematopoietic cell lineage and have a negative impact on defense response to the virus and immune responses.










Similar content being viewed by others
References
Hentze M, Muckenthaler M, Galy B, Camaschella C (2010) Two to tango: regulation of Mammalian iron metabolism. Cell 142(1):24–38. https://doi.org/10.1016/j.cell.2010.06.028
Muckenthaler M, Rivella S, Hentze M, Galy B (2017) A red carpet for iron metabolism. Cell 168(3):344–361. https://doi.org/10.1016/j.cell.2016.12.034
Crielaard B, Lammers T, Rivella S (2017) Targeting iron metabolism in drug discovery and delivery. Nat Rev Drug Discovery 16(6):400–423. https://doi.org/10.1038/nrd.2016.248
Esposito BP, Breuer W, Sirankapracha P, Pootrakul P, Hershko C, Cabantchik ZI (2003) Labile plasma iron in iron overload: redox activity and susceptibility to chelation. Blood 102(7):2670–2677. https://doi.org/10.1182/blood-2003-03-0807
Evans RW, Rafique R, Zarea A, Rapisarda C, Cammack R, Evans PJ et al (2008) Nature of non-transferrin-bound iron: studies on iron citrate complexes and thalassemic sera. J Biol Inorg Chem 13(1):57–74. https://doi.org/10.1007/s00775-007-0297-8
Knutson MD (2019) Non-transferrin-bound iron transporters. Free Radic Biol Med 133:101–111. https://doi.org/10.1016/j.freeradbiomed.2018.10.413
Brissot P, Ropert M, Le Lan C, Loreal O (2012) Non-transferrin bound iron: a key role in iron overload and iron toxicity. BBA-Gen Subjects 1820(3):403–410. https://doi.org/10.1016/j.bbagen.2011.07.014
Jenkitkasemwong S, Wang CY, Coffey R, Zhang W, Chan A, Biel T et al (2015) SLC39A14 is required for the development of hepatocellular iron overload in murine models of hereditary hemochromatosis. Cell Metab 22(1):138–150. https://doi.org/10.1016/j.cmet.2015.05.002
Brissot P, Wright TL, Ma WL, Weisiger RA (1985) Efficient clearance of non-transferrin-bound iron by rat liver. Implications for hepatic iron loading in iron overload states. J Clin Invest 76(4):1463–70. https://doi.org/10.1172/JCI112125
Baek J, Shin H, Gao Y, Buehler P (2020) Ferroportin inhibition attenuates plasma iron, oxidant stress, and renal injury following red blood cell transfusion in guinea pigs. Transfusion 60(3):513–523. https://doi.org/10.1111/trf.15720
Aljwaid H, White D, Collard K, Moody A, Pinkney J (2015) Non-transferrin-bound iron is associated with biomarkers of oxidative stress, inflammation and endothelial dysfunction in type 2 diabetes. J Diabetes Complications 29(7):943–949. https://doi.org/10.1016/j.jdiacomp.2015.05.017
Ji C, Kosman DJ (2015) Molecular mechanisms of non-transferrin-bound and transferring-bound iron uptake in primary hippocampal neurons. J Neurochem 133(5):668–683. https://doi.org/10.1111/jnc.13040
Pinilla-Tenas J, Sparkman B, Shawki A, Illing A, Mitchell C, Zhao N et al (2011) Zip14 is a complex broad-scope metal-ion transporter whose functional properties support roles in the cellular uptake of zinc and nontransferrin-bound iron. Am J Physiol Cell Physiol 301(4):C862–C871. https://doi.org/10.1152/ajpcell.00479.2010
Gulec S, Anderson GJ, Collins JF (2014) Mechanistic and regulatory aspects of intestinal iron absorption. Am J Physiol Gastrointest Liver Physiol 307(4):G397-409. https://doi.org/10.1152/ajpgi.00348.2013
Yu X, Chen L, Ding H, Zhao Y, Feng J (2019) Iron transport from ferrous bisglycinate and ferrous sulfate in DMT1-knockout human intestinal Caco-2 cells. Nutrients. 11(3):485. https://doi.org/10.3390/nu11030485
Taylor KM, Morgan HE, Johnson A, Nicholson RI (2005) Structure-function analysis of a novel member of the LIV-1 subfamily of zinc transporters, ZIP14. FEBS Lett 579(2):427–432. https://doi.org/10.1016/j.febslet.2004.12.006
Jenkitkasemwong S, Wang CY, Mackenzie B, Knutson MD (2012) Physiologic implications of metal-ion transport by ZIP14 and ZIP8. Biometals 25(4):643–655. https://doi.org/10.1007/s10534-012-9526-x
Guthrie GJ, Aydemir TB, Troche C, Martin AB, Chang SM, Cousins RJ (2015) Influence of ZIP14 (slc39A14) on intestinal zinc processing and barrier function. Am J Physiol Gastrointest Liver Physiol 308(3):G171–G178. https://doi.org/10.1152/ajpgi.00021.2014
Núñez MT, Tapia V, Rojas A, Aguirre P, Gómez F, Nualart F (2010) Iron supply determines apical/basolateral membrane distribution of intestinal iron transporters DMT1 and ferroportin 1. Am J Physiol Cell Physiol 298(3):C477–C485. https://doi.org/10.1152/ajpcell.00168.2009
Yanatori I, Kishi F (2019) DMT1 and iron transport. Free Radic Biol Med 133:55–63. https://doi.org/10.1016/j.freeradbiomed.2018.07.020
Wang Y, Song W, Wang J, Wang T, Xiong X, Qi Z et al (2020) Single-cell transcriptome analysis reveals differential nutrient absorption functions in human intestine. J Exp Med 217(2). https://doi.org/10.1084/jem.20191130
Craven CM, Alexander J, Eldridge M, Kushner JP, Bernstein S, Kaplan J (1987) Tissue distribution and clearance kinetics of non-transferrin-bound iron in the hypotransferrinemic mouse: a rodent model for hemochromatosis. Proc Natl Acad Sci U S A 84(10):3457–3461. https://doi.org/10.1073/pnas.84.10.3457
Li X, Kshirsagar AV, Brookhart MA (2017) Safety of intravenous iron in hemodialysis patients. Hemodial Int 21(Suppl 1):S93–S103. https://doi.org/10.1111/hdi.12558
Rodrigues D, Freitas M, Marisa Costa V, Arturo Lopez-Quintela M, Rivas J, Freitas P et al (2017) Quantitative histochemistry for macrophage biodistribution on mice liver and spleen after the administration of a pharmacological-relevant dose of polyacrylic acid-coated iron oxide nanoparticles. Nanotoxicology 11(2):256–266. https://doi.org/10.1080/17435390.2017.1291865
Franke GN, Kubasch AS, Cross M, Vucinic V, Platzbecker U (2020) Iron overload and its impact on outcome of patients with hematological diseases. Mol Aspects Med 75:100868. https://doi.org/10.1016/j.mam.2020.100868
Zhang LY, Liao XD, Lu L, Luo XG (2016) Kinetics of iron absorption by in situ ligated small intestinal loops of broilers involved in iron transporters. J Anim Sci 94(12):5219–5229. https://doi.org/10.2527/jas.2016-0713
Girijashanker K, He L, Soleimani M, Reed JM, Li H, Liu Z et al (2008) Slc39a14 gene encodes ZIP14, a metal/bicarbonate symporter: similarities to the ZIP8 transporter. Mol Pharmacol 73(5):1413–1423. https://doi.org/10.1124/mol.107.043588
Liuzzi JP, Aydemir F, Nam H, Knutson MD, Cousins RJ (2006) Zip14 (Slc39a14) mediates non-transferrin-bound iron uptake into cells. Proc Natl Acad Sci U S A 103(37):13612–13617. https://doi.org/10.1073/pnas.0606424103
Yoneyama M, Kikuchi M, Matsumoto K, Imaizumi T, Miyagishi M, Taira K et al (2005) Shared and unique functions of the DExD/H-box helicases RIG-I, MDA5, and LGP2 in antiviral innate immunity. J Immunol 175(5):2851–2858. https://doi.org/10.4049/jimmunol.175.5.2851
Saito T, Hirai R, Loo YM, Owen D, Johnson CL, Sinha SC et al (2007) Regulation of innate antiviral defenses through a shared repressor domain in RIG-I and LGP2. Proc Natl Acad Sci U S A 104(2):582–587. https://doi.org/10.1073/pnas.0606699104
Takahasi K, Kumeta H, Tsuduki N, Narita R, Shigemoto T, Hirai R et al (2009) Solution structures of cytosolic RNA sensor MDA5 and LGP2 C-terminal domains: identification of the RNA recognition loop in RIG-I-like receptors. J Biol Chem 284(26):17465–17474. https://doi.org/10.1074/jbc.M109.007179
Bamming D, Horvath CM (2009) Regulation of signal transduction by enzymatically inactive antiviral RNA helicase proteins MDA5, RIG-I, and LGP2. J Biol Chem 284(15):9700–9712. https://doi.org/10.1074/jbc.M807365200
Chopy D, Pothlichet J, Lafage M, Mégret F, Fiette L, Si-Tahar M et al (2011) Ambivalent role of the innate immune response in rabies virus pathogenesis. J Virol 85(13):6657–6668. https://doi.org/10.1128/JVI.00302-11
Zhao C, Hsiang TY, Kuo RL, Krug RM (2010) ISG15 conjugation system targets the viral NS1 protein in influenza A virus-infected cells. Proc Natl Acad Sci U S A 107(5):2253–2258. https://doi.org/10.1073/pnas.0909144107
Swaim CD, Scott AF, Canadeo LA, Huibregtse JM (2017) Extracellular ISG15 signals cytokine secretion through the LFA-1 integrin receptor. Mol Cell 68(3):581–90.e5. https://doi.org/10.1016/j.molcel.2017.10.003
Bogunovic D, Byun M, Durfee LA, Abhyankar A, Sanal O, Mansouri D et al (2012) Mycobacterial disease and impaired IFN-γ immunity in humans with inherited ISG15 deficiency. Science 337(6102):1684–1688. https://doi.org/10.1126/science.1224026
Kuang Z, Seo EJ, Leis J (2011) Mechanism of inhibition of retrovirus release from cells by interferon-induced gene ISG15. J Virol 85(14):7153–7161. https://doi.org/10.1128/JVI.02610-10
Kakuta S, Shibata S, Iwakura Y (2002) Genomic structure of the mouse 2′,5′-oligoadenylate synthetase gene family. J Interferon Cytokine Res 22(9):981–993. https://doi.org/10.1089/10799900260286696
Pulit-Penaloza JA, Scherbik SV, Brinton MA (2012) Activation of Oas1a gene expression by type I IFN requires both STAT1 and STAT2 while only STAT2 is required for Oas1b activation. Virology 425(2):71–81. https://doi.org/10.1016/j.virol.2011.11.025
Hu Y, Mao K, Zeng Y, Chen S, Tao Z, Yang C et al (2010) Tripartite-motif protein 30 negatively regulates NLRP3 inflammasome activation by modulating reactive oxygen species production. J Immunol 185(12):7699–7705. https://doi.org/10.4049/jimmunol.1001099
Shi M, Deng W, Bi E, Mao K, Ji Y, Lin G et al (2008) TRIM30 alpha negatively regulates TLR-mediated NF-kappa B activation by targeting TAB2 and TAB3 for degradation. Nat Immunol 9(4):369–377. https://doi.org/10.1038/ni1577
Sgarbanti M, Marsili G, Remoli AL, Orsatti R, Battistini A (2007) IRF-7: new role in the regulation of genes involved in adaptive immunity. Ann N Y Acad Sci 1095:325–333. https://doi.org/10.1196/annals.1397.036
Zhang Q, Bastard P, Liu Z, Le Pen J, Moncada-Velez M, Chen J et al (2020) Inborn errors of type I IFN immunity in patients with life-threatening COVID-19. Science 370(6515). https://doi.org/10.1126/science.abd4570
Li W, Hofer MJ, Jung SR, Lim SL, Campbell IL (2014) IRF7-dependent type I interferon production induces lethal immune-mediated disease in STAT1 knockout mice infected with lymphocytic choriomeningitis virus. J Virol 88(13):7578–7588. https://doi.org/10.1128/JVI.03117-13
Péléraux A, Karlsson L, Chambers J, Peterson PA (1996) Genomic organization of a mouse MHC class II region including the H2-M and Lmp2 loci. Immunogenetics 43(4):204–214. https://doi.org/10.1007/BF00587301
Walter W, Scheuer C, Loos M, Reichert TE, Maeurer MJ (2001) H2-Mbeta 1 and H2-Mbeta 2 heterodimers equally promote clip removal in I-A(q) molecules from autoimmune-prone DBA/1 mice. J Biol Chem 276(14):11086–11091. https://doi.org/10.1074/jbc.M006521200
Nowak J (2008) Role of HLA in hematopoietic SCT. Bone Marrow Transplant 42(Suppl 2):S71–S76. https://doi.org/10.1038/bmt.2008.288
Sandhu PK, Buchkovich NJ (2020) Human cytomegalovirus decreases major histocompatibility complex class II by regulating class II transactivator transcript levels in a myeloid cell line. J Virol 94(7). https://doi.org/10.1128/JVI.01901-19
Chen JJ, Zhang S (2019) Heme-regulated eIF2α kinase in erythropoiesis and hemoglobinopathies. Blood 134(20):1697–1707. https://doi.org/10.1182/blood.2019001915
Evstatiev R, Bukaty A, Jimenez K, Kulnigg-Dabsch S, Surman L, Schmid W et al (2014) Iron deficiency alters megakaryopoiesis and platelet phenotype independent of thrombopoietin. Am J Hematol 89(5):524–529. https://doi.org/10.1002/ajh.23682
Yamashita M, Dellorusso PV, Olson OC, Passegué E (2020) Dysregulated haematopoietic stem cell behaviour in myeloid leukaemogenesis. Nat Rev Cancer 20(7):365–382. https://doi.org/10.1038/s41568-020-0260-3
Höfer T, Rodewald HR (2018) Differentiation-based model of hematopoietic stem cell functions and lineage pathways. Blood 132(11):1106–1113. https://doi.org/10.1182/blood-2018-03-791517
Chen Y, Yu M, Zheng Y, Fu G, Xin G, Zhu W et al (2019) CXCR5(+)PD-1(+) follicular helper CD8 T cells control B cell tolerance. Nat Commun 10. https://doi.org/10.1038/s41467-019-12446-5
Havenith SH, Remmerswaal EB, Idu MM, van Donselaar-van der Pant KA, van der Bom N, Bemelman FJ et al (2014) CXCR5+CD4+ follicular helper T cells accumulate in resting human lymph nodes and have superior B cell helper activity. Int Immunol. 26(3):183–92. https://doi.org/10.1093/intimm/dxt058
Morita R, Schmitt N, Bentebibel SE, Ranganathan R, Bourdery L, Zurawski G et al (2011) Human blood CXCR5(+)CD4(+) T cells are counterparts of T follicular cells and contain specific subsets that differentially support antibody secretion. Immunity 34(1):108–121. https://doi.org/10.1016/j.immuni.2010.12.012
Baba M, Imai T, Nishimura M, Kakizaki M, Takagi S, Hieshima K et al (1997) Identification of CCR6, the specific receptor for a novel lymphocyte-directed CC chemokine LARC. J Biol Chem 272(23):14893–14898. https://doi.org/10.1074/jbc.272.23.14893
Facciotti F, Larghi P, Bosotti R, Vasco C, Gagliani N, Cordiglieri C et al (2020) Evidence for a pathogenic role of extrafollicular, IL-10-producing CCR6. Proc Natl Acad Sci U S A 117(13):7305–7316. https://doi.org/10.1073/pnas.1917834117
Wang J, Ma L, Yang S, Wang S, Wei X, Song S (2016) IL-10-expressing Th2 cells contribute to the elevated antibody production in rheumatoid arthritis. Inflammation 39(3):1017–1024. https://doi.org/10.1007/s10753-016-0331-5
Ebrahimi Daryani N, Saghazadeh A, Moossavi S, Sadr M, Shahkarami S, Soltani S et al (2017) Interleukin-4 and interleukin-10 gene polymorphisms in patients with inflammatory bowel disease. Immunol Invest 46(7):714–729. https://doi.org/10.1080/08820139.2017.1360343
Hider RC (2002) Nature of nontransferrin-bound iron. Eur J Clin Invest 32(Suppl 1):50–54. https://doi.org/10.1046/j.1365-2362.2002.0320s1050.x
Hod EA, Zhang N, Sokol SA, Wojczyk BS, Francis RO, Ansaldi D et al (2010) Transfusion of red blood cells after prolonged storage produces harmful effects that are mediated by iron and inflammation. Blood 115(21):4284–4292. https://doi.org/10.1182/blood-2009-10-245001
Porter JB, Garbowski M (2014) The pathophysiology of transfusional iron overload. Hematol Oncol Clin North Am 28(4):683–701, vi. https://doi.org/10.1016/j.hoc.2014.04.003
Linder GE, Chou ST (2021) Red cell transfusion and alloimmunization in sickle cell disease. Haematologica. https://doi.org/10.3324/haematol.2020.270546
Ozment CP, Turi JL (2009) Iron overload following red blood cell transfusion and its impact on disease severity. Biochim Biophys Acta 1790(7):694–701. https://doi.org/10.1016/j.bbagen.2008.09.010
Moukalled NM, El Rassi FA, Temraz SN, Taher AT (2018) Iron overload in patients with myelodysplastic syndromes: an updated overview. Cancer 124(20):3979–3989. https://doi.org/10.1002/cncr.31550
Acknowledgements
The authors would like to give thanks to Novogene for helping with the transcriptome sequence.
Funding
The authors would like to give thanks for the financial support of the National Natural Science Foundation of China (No. 31772607) and Zhejiang Provincial Key Research and Development Program (2019C02051).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Yu, X., Zhang, Q., Ding, H. et al. Plasma Non-transferrin-Bound Iron Could Enter into Mice Duodenum and Negatively Affect Duodenal Defense Response to Virus and Immune Responses. Biol Trace Elem Res 201, 786–799 (2023). https://doi.org/10.1007/s12011-022-03200-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12011-022-03200-y