Abstract
Purpose
For patients with hormone receptor positive breast cancer, survivorship entails prolonged self-management of adjuvant treatment in the form of daily hormone therapy. Although sustained daily adherence across the 5-year course of therapy is associated with improved recurrence-free survival outcomes, adherence is suboptimal and many women discontinue hormone therapy prematurely. Factors associated with breast cancer survivors’ nonadherence and nonpersistence are not comprehensively understood. Furthermore, psychosocial variables have only received limited research attention, despite their documented relationships with adherence in other chronic illness populations.
Methods
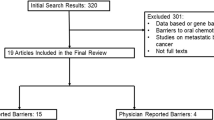
A systematic literature review identified 14 studies that analyzed relationships between psychosocial factors and breast cancer survivors’ adherence and/or persistence with adjuvant hormone therapy.
Results
Although identified relationships were complex and at times inconsistent, salient conclusions emerged. Interpersonal factors, in the form of positive social support and patient-centered interactions with medical providers, as well as intrapersonal factors, such as anxiety and beliefs about the relative benefits of medication use, were reliably associated with better adherence and persistence. Depression did not demonstrate the negative impact on adherence that has been observed in other medical populations. No relationships between quality of life and adherence were identified.
Conclusions
Adjuvant hormone therapy appears to be a unique context for medication adherence, which warrants further attention and more rigorous analysis in future research.
Implications for Cancer Survivors
Individual patients’ psychosocial characteristics and health care preferences should be considered when striving to optimize medication adherence.

Similar content being viewed by others
References
American Cancer Society. Breast cancer facts & figures, 2011-2012. Atlanta: American Cancer Society; 2011.
American Cancer Society. Cancer treatment and survivorship facts & figures 2012-2013. Atlanta: American Cancer Society; 2012.
Li CI, Daling JR, Malone KE. Incidence of invasive breast cancer by hormone receptor status from 1992 to 1998. J Clin Oncol. 2003;21:28–34.
Berry DA, Cronin KA, Plevritis SK, Fryback DG, Clarke L, Zelen M, et al. Effect of screening and adjuvant therapy on mortality from breast cancer. N Engl J Med. 2005;353:1784–92.
DeSantis C, Ma J, Bryan L, Jemal A. Breast cancer statistics. CA-Cancer J Clin. 2013. doi:10.3322/caac.21203.
Hewitt M, Greenfield S, Stovall E, editors. From cancer patient to cancer survivor: lost in transition. Washington: The National Academies Press; 2005.
Haque R, Ahmed SA, Fisher A, Avila CC, Shi J, Guo A, et al. Effectiveness of aromatase inhibitors and tamoxifen in reducing subsequent breast cancer. Cancer Med. 2012;1:318–27.
Early Breast Cancer Trialists’ Collaborative Group (EBCTCG), Davies C, Godwin J, Gray R, Clarke M, Cutter D, et al. Relevance of breast cancer hormone receptors and other factors to the efficacy of adjuvant tamoxifen: patient-level meta-analysis of randomised trials. Lancet. 2011;378:771–84.
Davies C, Pan H, Godwin J, Gray R, Arriagada R, Raina V, et al. Long-term effects of continuing adjuvant tamoxifen to 10 years versus stopping at 5 years after diagnosis of oestrogen receptor-positive breast cancer: ATLAS, a randomised trial. Lancet. 2013;381:805–16.
Burstein HJ, Prestrud AA, Seidenfeld J, Anderson H, Buchholz TA, Davidson NE, et al. American Society of Clinical Oncology clinical practice guideline: update on adjuvant endocrine therapy for women with hormone receptor–positive breast cancer. J Clin Oncol. 2010;28:3784–96.
Cella D, Fallowfield L, Barker P, Cuzick J, Locker G, Howell A. Quality of life of postmenopausal women in the ATAC (“Arimidex”, tamoxifen, alone or in combination) trial after completion of 5 years’ adjuvant treatment for early breast cancer. Breast Cancer Res Tr. 2006;100:273–84.
Cella D, Fallowfield L. Recognition and management of treatment-related side effects for breast cancer patients receiving adjuvant endocrine therapy. Breast Cancer Res Tr. 2008;107:167–80.
Huiart L, Bouhnik A, Rey D, Tarpin C, Cluze C, Bendiane MK, et al. Early discontinuation of tamoxifen intake in younger women with breast cancer: is it time to rethink the way it is prescribed? Eur J Cancer. 2012;48:1939–46.
Makubate B, Donnan PT, Dewar JA, Thompson AM, McCowan C. Cohort study of adherence to adjuvant endocrine therapy, breast cancer recurrence and mortality. British J Cancer. 2013;108:1515–24.
McCowan C, Shearer J, Donnan PT, Dewar JA, Crilly M, Thompson AM, et al. Cohort study examining tamoxifen adherence and its relationship to mortality in women with breast cancer. British J Cancer. 2008;99:1763–8.
Xu S, Yang Y, Tao W, Song Y, Chen Y, Ren Y, et al. Tamoxifen adherence and its relationship to mortality in 116 men with breast cancer. Breast Cancer Res Tr. 2012;136:495–502.
Waterhouse DM, Calzone KA, Mele C, Brenner DE. Adherence to oral tamoxifen: a comparison of patient self-report, pill counts, and microelectronic monitoring. J Clin Oncol. 1993;11:1189–97.
Murphy CC, Bartholomew LK, Carpentier MY, Bluethmann SM, Vernon SW. Adherence to adjuvant hormonal therapy among breast cancer survivors in clinical practice: a systematic review. Breast Cancer Res Tr. 2012;134:459–78.
Huiart L, Ferdynus C, Giorgi R. A meta-regression analysis of the available data on adherence to adjuvant hormonal therapy in breast cancer: summarizing the data for clinicians. Breast Cancer Res Tr. 2013;138:325–8.
Lash TL, Fox MP, Westrup JL, Fink AK, Silliman RA. Adherence to tamoxifen over the 5-year course. Breast Cancer Res Treat. 2006;99:215–20.
Barron TI, Connolly R, Bennett K, Feely J, Kennedy MJ. Early discontinuation of tamoxifen. Cancer. 2007;109:832–9.
Partridge AH, Wang PS, Winer EP, Avorn J. Nonadherence to adjuvant tamoxifen therapy in women with primary breast cancer. J Clin Oncol. 2003;21:602–6.
Demissie S, Silliman RA, Lash TL. Adjuvant tamoxifen: predictors of use, side effects, and discontinuation in older women. J Clin Oncol. 2001;19:322–8.
Fink AK, Gurwitz J, Rakowski W, Guadagnoli E, Silliman RA. Patient beliefs and tamoxifen discontinuance in older women with estrogen receptor-positive breast cancer. J Clin Oncol. 2004;22:3309–15.
Cluze C, Rey D, Huiart L, BenDiane MK, Bouhnik AD, Berenger C, et al. Adjuvant endocrine therapy with tamoxifen in young women with breast cancer: determinants of interruptions vary over time. Ann Oncol. 2012;23:882–90.
Liu Y, Malin JL, Diamant AL, Thind A, Maly RC. Adherence to adjuvant hormone therapy in low-income women with breast cancer: the role of provider-patient communication. Breast Cancer Res Tr. 2012;137:829–36.
DiMatteo MR, Lepper HS, Croghan TW. Depression is a risk factor for noncompliance with medical treatment: meta-analysis of the effects of anxiety and depression on patient adherence. Arch Intern Med. 2000;160:2101–7.
DiMatteo RM. Social support and patient adherence to medical treatment: a meta-analysis. Health Psychol. 2004;23:207–18.
Gallant MP. The influence of social support on chronic illness self-management: a review and directions for research. Health Educ Behav. 2003;30:170–95.
Christensen AJ. Patient adherence to medical treatment regimens: bridging the gap between behavioral science and biomedicine. New Haven: Yale University Press; 2004.
Christensen AJ, Howren MB, Hillis SL, Kaboli P, Carter BL, Cvengros JA, et al. Patient and physician beliefs about control over health: symmetrical beliefs predict medication regimen adherence. J Gen Intern Med. 2010;25:397–402.
Cvengros JA, Christensen AJ, Cunningham C, Hillis SL, Kaboli PJ. Patient preference for and reports of provider behavior: impact of symmetry on patient outcomes. Health Psychol. 2009;28:660–7.
Fann JR, Thomas-Rich A, Katon WJ, Cowley D, Pepping M, McGregor BA, et al. Major depression after breast cancer: a review of epidemiology and treatment. Gen Hosp Psychiat. 2008;30:112–26.
Henselmans I, Helgeson VS, Seltman H, de Vries J, Sanderman R, Ranchor AV. Identification and prediction of distress trajectories in the first year after a breast cancer diagnosis. Health Psychol. 2010;29:160–8.
van Londen GJ, Beckjord EB, Dew MA, Cooper KL, Davidson NE, Bovbjerg, et al. Associations between adjuvant endocrine therapy and onset of physical and emotional concerns among breast cancer survivors. Support Care Cancer. 2013. doi:10.1007/s00520-013-2041-y.
Hadji P, Ziller V, Kyvernitakis J, Bauer M, Haas G, Schmidt M, et al. Persistence in patients with breast cancer treated with tamoxifen or aromatase inhibitors: a retrospective database analysis. Breast Cancer Res Tr. 2013;138:185–91.
Kostev K, Waehlert L, Jockwig A, Jockwig B, Hadji P. Physicians’ influence on breast cancer patient compliance. GMS Ger Med Sci. 2014;12(Doc03):20140120.
Huiart L, Bouhnik A-D, Rey D, Rousseau F, Retornaz F, Meresse M, et al. Complementary or alternative medicine as possible determinant of decreased persistence to aromatase inhibitor therapy among older women with non-metastatic breast cancer. PLoS One. 2013;8:e81677.
Kyvernitakis I, Ziller V, Hars O, Bauer M, Kalder M, Hadji P. Prevalence of menopausal symptoms and their influence on adherence in women with breast cancer. Climacteric. 2013;00:1–8.
Kostev K, May U, Hog D, Eisel J, Kremmers T, Kosteic M, et al. Adherence in tamoxifen therapy after conversion to a rebate pharmaceutical in breast cancer patients in Germany. Int J Clin Pharm Th. 2013;51:969–75.
Grunfeld EA, Hunter MS, Sikka P, Mittal S. Adherence beliefs among breast cancer patients taking tamoxifen. Patient Educ Couns. 2005;59:97–102.
Kahn KL, Schneider EC, Malin JL, Adams JL, Epstein AM. Patient centered experiences in breast cancer: predicting long-term adherence to tamoxifen use. Med Care. 2007;45:431–9.
Acknowledgments
Alan J. Christensen’s time in preparation of this article was supported, in part, by the Behavioral Research Program in the Division of Cancer Control and Population Sciences, National Cancer Institute and the Office of Social and Behavioral Sciences Research at the National Institutes of Health.
Conflict of interest
All authors declare that they have no conflict of interest.
Informed consent/animal studies
No animal or human studies were carried out by the authors for this article.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Van Liew, J.R., Christensen, A.J. & de Moor, J.S. Psychosocial factors in adjuvant hormone therapy for breast cancer: an emerging context for adherence research. J Cancer Surviv 8, 521–531 (2014). https://doi.org/10.1007/s11764-014-0374-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11764-014-0374-2