Abstract
Background
Despite continued investigation, limited progress has been made in the adjuvant treatment of resected pancreatic cancer. Novel or targeted therapies are needed.
Methods
Multi-institutional, open-label, dose-finding, phase 2 trial evaluating the use of algenpantucel-L (NewLink Genetics Corporation, Ames, IA) immunotherapy in addition to chemotherapy and chemoradiotherapy in the adjuvant setting for resected pancreatic cancer (ClinicalTrials.gov identifier, NCT00569387). The primary outcome was 12-month disease-free survival. Secondary outcomes included overall survival and toxicity.
Results
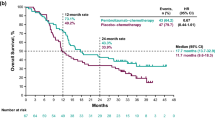
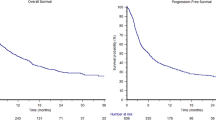
Seventy patients were treated with gemcitabine and 5-fluorouracil-based chemoradiotherapy as well as algenpantucel-L (mean 12 doses, range 1–14). After a median follow-up of 21 months, the 12-month disease-free survival was 62 %, and the 12-month overall survival was 86 %. The most common adverse events were injection site pain and induration.
Conclusions
The addition of algenpantucel-L to standard adjuvant therapy for resected pancreatic cancer may improve survival. A multi-institutional, phase 3 study is ongoing (ClinicalTrials.gov identifier, NCT01072981).


Similar content being viewed by others
References
Kalser MH, Ellenber SS. Pancreatic Cancer: Adjuvant Combined Radiation and Chemotherapy Following Curative Resection. Arch Surg 1985;120:899–903.
Klinkenbijl JH, Jeekel J, Sahmoud T, et al. Adjuvant Radiotherapy and 5-fluorouracil after Curative Resection of Cancer of the Pancreas and Periampullary Region: Phase III Trial of the EORTC Gastrointestinal Tract Cancer Cooperative Group. Ann Surg 1999;230:776–82.
Neoptolemos JP, Dunn JA, Stocken DD, et al. Adjuvant Chemoradiotherapy and Chemotherapy in Resectable Pancreas Cancer: A Randomised Controlled Trial. Lancet 2001;358:1576–1585.
Oettle H, Post S, Neuhaus P, et al. Adjuvant Chemotherapy with Gemcitabine vs. Observation in Patients Undergoing Curative-intent Resection of Pancreatic Cancer: A Randomized Controlled Trial. JAMA 2007;297:267–77.
Regine WF, Winter KA, Abrams RA, et al. Fluorouracil vs. Gemcitabine Chemotherapy Before and After Fluorouracil-Based Chemoradiation Following Resection of Pancreatic Adenocarcinoma: A Randomized Controlled Trial. JAMA 2008;299:1019–26.
Neoptolemos JP, Stocken DD, Bassi C, et al. Adjuvant Chemotherapy with Fluorouracil plus Folinic Acid vs. Gemcitabine Following Pancreatic Cancer Resection: A Randomized Controlled Trial. JAMA 2010;304:1073–81.
National Comprehensive Cancer Network Guidelines Version 2.2012—Pancreatic Adenocarcinoma. Available at: www.nccn.org. Accessed 15 March 2012
Joziasse DH, Oriol R. Xenotransplantation: the Importance of the Galα1,3Gal Epitope in Hyperacute Vascular Rejection. Biochim Biophy Acta 1999;1455:403–18.
Galili U, Mandrell RE, Hamadeh RM, et al. Interaction between Human Natural Anti-alpha-galactosyl Immunoglobulin G and Bacteria of the Human Flora. Infect Immun 1988;56:1730–37.
Baumann BC, Forte P, Hawley RJ, et al. Lack of Galactose-α-1,3-galactose Expression on Porcine Endothelial Cells Prevents Complement-induced Lysis but not Direct Xenogenic NK Cytotoxicity. J Immunol 2004;172:6460–7.
Schaapherder AF, Daha MR, te Bulte MT, et al. Antibody-dependent cell-mediated cytotoxicity against porcine endothelium induced by a majority of human sera. Transplantation 1994;57:1376–82.
Watier H, Guillaumin JM, Vallee I, et al. Human NK cell-mediated direct and IG-dependent Cytotoxicity against Xenogeneic Porcine Epithelial Cells. Transpl Immunol 1996;4:293–9.
Watier H, Giollaumin JM, Piller F, et al. Removal of Terminal α-galactosyl Residues from Xenogeneic Porcine Endothelial Cells. Decrease in Complement-mediated cytotoxicity but Persistence of IgG1-mediated Antibody-dependent Cell-mediated Cytotoxicity. Transplantation 1996;62:105–13.
Bilimoria KY, Bentrem DJ, Ko CY, et al. Validation of the 6th Edition AJCC Pancreatic Cancer Staging System: Report from the National Cancer Database. Cancer 2007;110:738–44.
Brennan MF, Kattan MW, Klimstra D, Conlon K. Prognostic Nomogram for Patients Undergoing Resection for Adenocarcinoma of the Pancreas. Ann Surg 2004;240:293–8.
Zitvogel L, Apetoh L, Ghiringhelli F, et al. The Anticancer Immune Response: Indispensable for Therapeutic Success? J Clin Invest 2008;118:1991–2001.
Lutz E, Yeo CJ, Lillemoe KD, et al. A Lethally Irradiated Allogeneic Granulocyte-Macrophage Colony Stimulating Factor-Secreting Tumor Vaccine for Pancreatic Adenocarcinoma: A Phase II Trial of Safety, Efficacy, and Immune Activation. Ann Surg 2011;253:328–35.
Abou-Alfa GK, Chapman PB, Feilchenfeldt J, et al. Targeting Mutated K-ras in Pancreatic Adenocarcinoma Using an Adjuvant Vaccine. Am J Clin Oncol 2011;34:321–5.
Morse MA, Nair SK, Boczkowski D, et al. The Feasibility and Safety of Immunotherapy with Dendritic Cells Loaded with CEA mRNA Following Neoadjuvant Chemoradiotherapy and Resection of Pancreatic Cancer. Int J Gastrointest Cancer 2002;32:1–6.
Ramanathan RK, Lee KM, McKolanis J, et al. Phase I Study of a MUC1 Vaccine Composed of Different Doses of MUC1 Peptide with SB-A2 Adjuvant in Resected and Locally Advanced Pancreatic Cancer. Cancer Immunol Immunother 2005;54:254–64.
Maki RG, Livingston PO, Lewis JJ, et al. A Phase I Pilot Study of Autologous Heat Shock Protein Vaccine HXPPC-96 in Patients with Resected Pancreatic Adenocarcinoma. Dig Dis Sci 2007;52:1964–72.
Author information
Authors and Affiliations
Corresponding author
Additional information
Discussant
Dr. Christopher Wolfgang (Baltimore, MD): I would like to congratulate Dr. Hardacre and his colleagues on this well-done and well-presented study. I would also like to commend you in bringing together the multiple institutions to complete this trial in such a brief time.
While the current study does not directly prove efficacy of the vaccine, it does demonstrate an encouraging 1-year DFS of 62 %. This is favorable in comparison to historical survival data, which are in the range of 50 %, and to the contemporary RTOG 9704 trial that consists of a population of patients with identical adjuvant therapy minus the vaccine. Moreover, the dose–response of vaccine is highly suggestive of a specific biological response of the treatment. If these findings stand up in the phase III trial, it will be a significant leap forward in adjuvant therapy.
I have three questions:
1. It would be nice to know early in therapy if a particular patient will respond to the vaccine. In this way, alternative therapies can be considered in the nonresponders. As part of this study, or the upcoming phase III trial, are you assessing any parameters such as serum antibodies that may have the potential to predict response?
2. Knowing that chemotherapy, and to a greater extent chemoradiotherapy, is immunosuppressive can you comment on the timing of the chemoradiation in relation the administration of vaccine. Was there any consideration given to treating with chemoradiation in the neoadjuvant setting or even administering the vaccine in the neoadjuvant setting? The second part of this question is will these patients get continued vaccine boosts for life?
3. Finally, would you be able to give us some insight on the design of your phase III trial?
Closing discussant
Dr. Jeffrey M. Hardacre: Please respond here.
Chris, thank you so much for your comments and questions.
With regard to your first question, a number of correlative studies were done during the phase 2 study and are being done during the phase 3 study. They include the measurement of anti-CEA antibodies, anti-mesothelin antibodies, and anti-alpha-gal antibodies. The data from the phase 2 study suggest some trends in terms of antibody levels and clinical outcome, but the numbers are too small to make any definitive statement. Hopefully, with the larger population in the phase 3 trial some clear correlations will appear so that we can perhaps better individualize treatment. We have also seen some suggestion of persistent eosinophilia correlating with clinical outcome, and that will also be further looked into.
Your question regarding the timing of vaccination is one that I also had a difficult time conceptualizing. It does seem odd to be trying to stimulate the immune system with the vaccine while suppressing it with the standard adjuvant therapy. The rationale is the emerging concept of chemoimmunotherapy. The basis for the effectiveness of chemoimmunotherapy has multiple parts. The first is the direct cytotoxic effect of the chemotherapy. The second is antigen shedding. That is to say that the lysis of cancer cells may release tumor-specific antigens that enhance a patient’s immune response. The third is that the lymphotoxic effect of the chemotherapy may impact to a greater degree suppressor T cells as compared to cytotoxic T cells or natural killer cells. Finally, there is the concept of chemosensitization. There is literature suggesting that immunotherapy may make subsequent chemotherapy more effective. Anecdotally, we have three patients who, after recurrence, achieved complete radiographic responses to subsequent chemotherapy with the duration of response being 6–36 months. For the last part of this question, thought is being given to using the vaccine in the neoadjuvant setting for patients with borderline resectable cancers.
The phase 3 trial differs in a number of ways from the phase 2. The most important is that this is a randomized trial of standard adjuvant therapy with or without vaccine. Other differences include the fact that the primary outcome is overall survival and that there are options for the standard therapy. For the phase 3 trial, the standard therapy may be either gemcitabine alone or gemcitabine combined with 5FU-based radiation therapy. The patient and oncologist will decide on the type of standard therapy; then, the randomization to vaccine or no vaccine occurs. Also, given the potential dose–response seen in the phase 2 study, the vaccine dose is 300 million cells in the phase 3, and patients will get booster vaccines monthly out to 1 year after completing the standard therapy. Lastly, the window for starting therapy after surgery has been extended to 10 weeks, which should allow a few more people to enroll that may not have recovered enough at 6–7 weeks.
Appendix: Participating Institutions
Appendix: Participating Institutions
University Hospitals Seidman Cancer Center/Case Western Reserve University
Northshore University Health System
Rhode Island Hospital
Northwestern University
University of Miami
Indiana University Melvin and Bren Simon Cancer Center
University of Southern California
Thomas Jefferson University
University of Colorado
Mayo Clinic-Scottsdale
California Pacific Medical Center
Baylor College of Medicine
Lahey Clinic
University of Texas-San Antonio
University of California-Irvine
University of New Mexico
Rights and permissions
About this article
Cite this article
Hardacre, J.M., Mulcahy, M., Small, W. et al. Addition of Algenpantucel-L Immunotherapy to Standard Adjuvant Therapy for Pancreatic Cancer: a Phase 2 Study. J Gastrointest Surg 17, 94–101 (2013). https://doi.org/10.1007/s11605-012-2064-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-012-2064-6