Abstract
Purpose
The purpose of the study was to determine how air flow profiles affect fine particle fractions (FPF) (<5 μm) from dry powder aerosol formulations and whether laser diffraction (LD) could be used to measure FPF of aerosols generated by variable flows.
Materials and Methods
Carrier-based formulations containing 1.5% w/w micronized salbutamol base blended with the 63–90 μm fraction of alpha-lactose monohydrate or sorbitol or maltose were aerosolised from a model glass device using either a constant flow rate or a predetermined flow profile. The FPFs of the same aerosolised particles were first measured by LD and then by a liquid impinger. Volunteer inhalation airflow profiles and 3-phase (acceleration, constant flow rate and deceleration) square wave airflow profiles were generated using the Electronic Lung™ and an Inhalation Profile Recorder. Similar experiments were conducted for a carrier-free formulation from the Bricanyl Turbohaler™.
Results
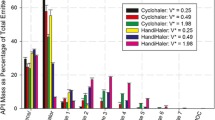
Salbutamol FPFs of all carrier-based formulations were found to increase by increasing the initial flow increase rate (FIR) from 200 to 600 l min−1 s−1 although they could be placed in an increasing order of maltose blend < sorbitol blend < lactose blend. A significant linear correlation was found between FPFs measured by LD and by inertial impaction (R 2 = 0.95, p < 0.01, ANOVA). For the Bricanyl Turbohaler™, increasing FIR from 120 to 600 l min−1 s−1 for a constant peak flow rate (PFR) of 60 l min−1 increased the mean Terbutaline FPF from 18.2% to 45.5%. For the volunteer inhalation profiles, a higher FIR tended to be associated with higher PFR, leading to a marked increase in drug FPF due to the combined effect of FIR and PFR.
Conclusion
Drug FPF from either carrier-free or carrier-based formulations is determined by both FIR and PFR. LD is a viable technique to measure the performance of dry powder aerosol formulations at realistic inspiratory flow profiles.





Similar content being viewed by others
References
M. Dolovich. Characterisation of medical aerosols: physical and clinical requirements for new inhalers. Aerosol. Sci. Tech. 22: 392–399 (1995).
A. H. de Boer, D. Gjaltema, and P. Hagedoorn. Inhalation characteristics and their effect on in vitro drug delivery from dry powder inhalers. Part 2: effect of peak flow rate (PIFR) and inspiration time on the in vitro drug release from 3 types of commercial dry powder inhalers. Int. J. Pharm. 138:45–56 (1996).
D. L. Ross, and R. K. Schultz. Effect of inhalation flow rate on the dosing characteristics of dry powder inhaler (DPI) and metered dose inhaler (MDI) products. J. Aerosol Med. 9:215–226 (1996).
A. Brindley, B. S. Sumby, and J. J. Smith. The characterisation of inhalation devices by an inhalation simulator: the Electronic Lung. J. Aerosol Med. 7:197–200 (1994).
P. K. P. Burnell, L. Petchey, D. Prime, and B. S. Sumby. Patient inhalation profiles and dose emission characteristics from dry powder inhalers. In B. R. Byron, R. N. Dalby, and S. J. Farr (eds.), Respiratory Drug Delivery V, Phoenix, Arizona, 1996.
V. S. Chavan, and R. N. Dalby. Effect of rise in simulated inspiratory flow rate and carrier particle size on powder emptying from dry powder inhalers. AAPS PharmSCi 2(article 10): 1–7 (2000).
V. S. Chavan, and R. N. Dalby. Novel system to investigate the effects of inhaled volume and rates of rise in simulated inspiratory air flow on fine particle output from a dry powder inhaler. AAPS PharmSci 4(article 6):1–6 (2001).
S. P. Newman, A. H. Hollingworth, and A. R. Clarke. Effect of different modes of inhalation on drug delivery from a dry powder inhaler. Int. J. Pharm. 102:127–132 (1994).
G. Persson, B. Olsson, and S. Soliman. The impact of inspiratory effort on inspiratory flow through Turbuhaler™ in asthmatic patients. Eur. Respir. J. 10:681–684 (1997).
B. K. P. Burnell, A. Malton, K. Reavill, and M. H. E. Ball. Design, validation and initial testing of the electronic lung™ device. J. Aerosol. Sci. 29:1011–1025 (1998).
A. Brindley, K. J. Reavill, B. S. Sumby, and I. J. Smith. The in-vitro characterization of inhalation devices using the electronic lung™. In B. R. Byron, R. N. Dalby, and S. J. Farr (eds.), Respiratory Drug Delivery IV, Interpharm, Buffalo Grove, Illinois, 1994.
A. H. de Boer, G. K. Bolhuis, D. Gjatema, and P. Hagedoorn. Inhalation characteristics and their effects on in vitro drug delivery from dry powder inhalers. Part 3: the effect of flow increase rate (FIR) on the in vitro drug release from the Pulmicort 200 Turbuhaler. Int. J. Pharm. 153:67–77 (1997).
W. H. Finlay, and M. G. Gehmlich. Inertial sizing of aerosol inhaled from two dry powder inhalers with realistic breath patterns versus constant flow rates. Int. J. Pharm. 210:83–95 (2000).
X. M. Zeng, H. B. MacRitchie, C. Marriott, and G. P. Martin. Correlation between inertial impaction and laser diffraction sizing data for aerosolized carrier-based dry powder formulations. Pharm. Res. 23(9):2200–2209 (2006).
G. P. Martin, H. B. MacRitchie, C. Marriott, and X. M. Zeng. Characterisation of a carrier-free dry powder aerosol formulation using inertial impaction and laser diffraction. Pharm. Res. 23(9):2210–2219 (2006).
D. S. MacArthur and S. G. Fleck. The Electronic Lung™—Bridging the gap between in vitro and in vivo testing. In Proc. drug delivery to the lungs VI, London, 1995.
T. Small, S. Doig, G. J. Gibson, B. Johal, P. K. P. Burnell, and R. Jenkins. Use of inhalation profiles from patients with severe obstructive lung disease using the Diskus™ inhaler and Turbuhaler™ inhaler to evaluate device performance ex vivo. In Proc. European Respiratory Society Annual Congress, Berlin, 1997.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Martin, G.P., Marriott, C. & Zeng, XM. Influence of Realistic Inspiratory Flow Profiles on Fine Particle Fractions of Dry Powder Aerosol Formulations. Pharm Res 24, 361–369 (2007). https://doi.org/10.1007/s11095-006-9156-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11095-006-9156-5