Abstract
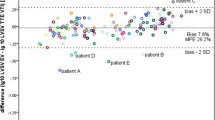
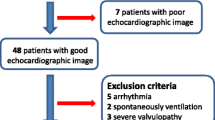
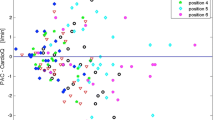
Background. Continuous and non-invasive measurement of cardiac output (CO) may contribute helpful information to the care and treatment of the critically ill pediatric patient. Different methods are available but their clinical verification is still a major problem. Aim. Comparison of reliability and safety of two continuous non-invasive methods with transthoracic echocardiography (TTE) for CO measurement: electric velocimetry technique (EV, Aesculon™) and transesophageal Doppler (TED, CardioQP™). Methods/Material. In 26 infants and children who had undergone corrective cardiac surgery at a median age of 3.5 (1–17) years CO and stroke volume (SV) were obtained by EV, TED and TTE. Each patient had five measurements on the first day after surgery, during mechanical ventilation and sedation. Results. Values for CO and SV from TED and EV correlated well with those of TTE (r = 0.85 and r = 0.88), but mean values were significantly lower than the values of TTE for TED (P = 0.02) and EV (P = 0.001). According to Bland-Altman analysis, bias was 0.36 l/min with a precision of 1.67 l/min for TED vs. TTE and 0.87 l/min (bias) with a precision of 3.26 l/min for EV vs. TTE. No severe adverse events were observed and the handling of both systems was easy in the sedated child. Conclusions. In pediatric patients non-invasive measurement of CO and SV with TED and EV is useful for continuous monitoring after heart surgery. Both new methods seem to underestimate cardiac output in terms of absolute values. However, TED shows tolerable bias and precision and may be helpful for continuous CO monitoring in a deeply sedated and ventilated pediatric patient, e.g. in the operating room or intensive care unit.
Article PDF
Similar content being viewed by others
References
Estagnasie P, Djedaini K, Mier L, Coste F, Dreyfuss D. Measurement of cardiac output by transesophageal echocardiography in mechanically ventilated patients. Comparison with thermodilution. Intensive Care Med 1997; 23: 753–759
Marcelino P, Germano N, Marum S, Fernandes AP, Ribeiro P, Lopes MG. Haemodynamic parameters obtained by transthoracic echocardiography and Swan-Ganz catheter: a comparative study in liver transplant patients. Acta Med Port 2006; 19: 197–205
Chew MS, Poelaert J. Accuracy and repeatability of pediatric cardiac output measurement using Doppler: 20-year review of the literature. Intensive Care Med 2003; 29: 1889–1894
Tibby SM, Hatherill M, Durward A, Murdoch IA. Are transoesophageal Doppler parameters a reliable guide to paediatric haemodynamic status and fluid management? Intensive Care Med 2001; 27: 201–205
Murdoch IA, Marsh MJ, Tibby SM, McLuckie A. Continuous haemodynamic monitoring in children: use of transoesophageal Doppler. Acta Paediatr 1995; 84: 761–764
Bearss MG, Yonutas DN, Allen WT. A complication with thermodilution cardiac outputs in centrally-placed pulmonary artery catheters. Chest 1982; 81: 527
Bossert T, Schmitt DV, Mohr FW. [Pulmonary artery rupture – fatal complication of catheter examination (thermodilution catheter)]. Z Kardiol 2000; 89: 54
Egan JR, Festa M, Cole AD, Nunn GR, Gillis J, Winlaw DS. Clinical assessment of cardiac performance in infants and children following cardiac surgery. Intensive Care Med 2005; 31: 568–573
Botte A, Leclerc F, Riou Y, Sadik A, Neve V, Rakza T, Richard A. Evaluation of a noninvasive cardiac output monitor in mechanically ventilated children. Pediatr Crit Care Med 2006; 7: 231–236
Ehlers KC, Mylrea KC, Waterson CK, Calkins JM. Cardiac output measurements. A review of current techniques and research. Ann Biomed Eng 1986; 14:219–239
Wodey E, Gai V, Carre F, Ecoffey C. Accuracy and limitations of continuous oesophageal aortic blood flow measurement during general anaesthesia for children: comparison with transcutaneous echography-Doppler. Paediatr Anaesth 2001; 11:309–317
Shoemaker WC, Wo CC, Chien LC, Lu K, Ahmadpour N, Belzberg H, Demetriades D. Evaluation of invasive and noninvasive hemodynamic monitoring in trauma patients. J Trauma 2006; 61:844–853; discussion 853–854
Cathignol D, Lavandier B, Muchada R. [Aortic flow measurement by transesophageal Doppler effect]. Ann Fr Anesth Reanim 1985; 4:438–443
Tibby SM, Hatherill M, Murdoch IA. Use of transesophageal Doppler ultrasonography in ventilated pediatric patients: derivation of cardiac output. Crit Care Med 2000; 28:2045–2050
Young LE, Blissitt KJ, Bartram DH, Clutton RE, Molony V, Jones RS. Measurement of cardiac output by transoesophageal Doppler echocardiography in anaesthetized horses: comparison with thermodilution. Br J Anaesth 1996; 77:773–780
Clark DI, Ahmed AB, Baxendale BR, Moran CG. Cardiac output during hemiarthroplasty of the hip. A prospective, controlled trial of cemented and uncemented prostheses. J Bone Joint Surg Br 2001; 83:414–418
Jaeggi P, Hofer CK, Klaghofer R, Fodor P, Genoni M, Zollinger A. Measurement of cardiac output after cardiac surgery by a new transesophageal Doppler device. J Cardiothorac Vasc Anesth 2003; 17:217–220
Larousse E, Asehnoune K, Dartayet B, Albaladejo P, Dubousset AM, Gauthier F, Benhamou D. The hemodynamic effects of pediatric caudal anesthesia assessed by esophageal Doppler. Anesth Analg 2002; 94:1165–1168, table of contents
Preiser JC, Daper A, Parquier JN, Contempre B, Vincent JL. Transthoracic electrical bioimpedance versus thermodilution technique for cardiac output measurement during mechanical ventilation. Intensive Care Med 1989; 15:221–223
Weiss S, Calloway E, Cairo J, Granger W, Winslow J. Comparison of cardiac output measurements by thermodilution and thoracic electrical bioimpedance in critically ill versus non-critically ill patients. Am J Emerg Med 1995; 13:626–631
Petersen JR, Jensen BV, Olsen F. [Impedance cardiography–non-invasive measurement of central hemodynamic data]. Ugeskr Laeger 1992; 154:255–260
O’Connell AJ, Tibballs J, Coulthard M. Improving agreement between thoracic bioimpedance and dye dilution cardiac output estimation in children. Anaesth Intensive Care 1991; 19:434–440
Martin M, Brown C, Bayard D, Demetriades D, Salim A, Gertz R, Azarow K, Wo CC, Shoemaker W. Continuous noninvasive monitoring of cardiac performance and tissue perfusion in pediatric trauma patients. J Pediatr Surg 2005; 40:1957–1963
Haycock GB, Schwartz GJ, Wisotsky DH. Geometric method for measuring body surface area: a height-weight formula validated in infants, children, and adults. J Pediatr 1978; 93:62–66
Tibby SM, Murdoch IA. Measurement of cardiac output and tissue perfusion. Curr Opin Pediatr 2002; 14:303–309
Gardin JM, Tobis JM, Dabestani A, Smith C, Elkayam U, Castleman E, White D, Allfie A, Henry WL. Superiority of two-dimensional measurement of aortic vessel diameter in Doppler echocardiographic estimates of left ventricular stroke volume. J Am Coll Cardiol 1985; 6:66–74
Schmidt C, Theilmeier G, Van Aken H, Korsmeier P, Wirtz SP, Berendes E, Hoffmeier A, Meissner A. Comparison of electrical velocimetry and transoesophageal Doppler echocardiography for measuring stroke volume and cardiac output. Br J Anaesth 2005; 95:603–610
Suttner S, Schollhorn T, Boldt J, Mayer J, Rohm KD, Lang K, Piper SN. Noninvasive assessment of cardiac output using thoracic electrical bioimpedance in hemodynamically stable and unstable patients after cardiac surgery: a comparison with pulmonary artery thermodilution. Intensive Care Med 2006; 32:2053–2058
Critchley L, Critchley J. A meta-analysis of studies using bias and precision statistics to compare cardiac output measurement techniques. J Clin Monit 1999; 15:85–91
Tibballs J, Hochmann M, Osborne A, Carter B. Accuracy of the BoMED NCCOM3 bioimpedance cardiac output monitor during induced hypotension: an experimental study in dogs. Anaesth Intensive Care 1992; 20:326–331
Chan JS, Segara D, Nair P. Measurement of cardiac output with a non-invasive continuous wave Doppler device versus the pulmonary artery catheter: a comparative study. Crit Care Resusc 2006; 8:309–314
Tan HL, Pinder M, Parsons R, Roberts B, van Heerden PV. Clinical evaluation of USCOM ultrasonic cardiac output monitor in cardiac surgical patients in intensive care unit. Br J Anaesth 2005; 94:287–291
Tibby SM, Murdoch IA. Monitoring cardiac function in intensive care. Arch Dis Child 2003; 88:46–52
Laupland KB, Bands CJ. Utility of esophageal Doppler as a minimally invasive hemodynamic monitor: a review. Can J Anaesth 2002; 49:393–401
Connors AF Jr., Speroff T, Dawson NV, Thomas C, Harrell FE Jr., Wagner D, Desbiens N, Goldman L, Wu AW, Califf RM, Fulkerson WJ Jr., Vidaillet H, Broste S, Bellamy P, Lynn J, Knaus WA. The effectiveness of right heart catheterization in the initial care of critically ill patients. SUPPORT Investigators. Jama 1996; 276:889–897
Shoemaker WC, Belzberg H, Wo CC, Milzman DP, Pasquale MD, Baga L, Fuss MA, Fulda GJ, Yarbrough K, Van DeWater JP, Ferraro PJ, Thangathurai D, Roffey P, Velmahos G, Murray JA, Asensio JA, ElTawil K, Dougherty WR, Sullivan MJ, Patil RS, Adibi J, James CB, Demetriades D. Multicenter study of noninvasive monitoring systems as alternatives to invasive monitoring of acutely ill emergency patients. Chest 1998; 114:1643–1652
Boyd O, Grounds RM, Bennett ED. A randomized clinical trial of the effect of deliberate perioperative increase of oxygen delivery on mortality in high–risk surgical patients. Jama 1993; 270:2699–2707
Mohan UR, Britto J, Habibi P, de Munter C, Nadel S. Noninvasive measurement of cardiac output in critically ill children. Pediatr Cardiol 2002; 23:58–61
Meijboom EJ, Rijsterborgh H, Bot H, De Boo JA, Roelandt JR, Bom N. Limits of reproducibility of blood flow measurements by Doppler echocardiography. Am J Cardiol 1987; 59:133–137
Su NY, Huang CJ, Tsai P, Hsu YW, Hung YC, Cheng CR. Cardiac output measurement during cardiac surgery: esophageal Doppler versus pulmonary artery catheter. Acta Anaesthesiol Sin 2002; 40:127–133
Robson SC, Boys RJ, Hunter S. Doppler echocardiographic estimation of cardiac output: analysis of temporal variability. Eur Heart J 1988; 9:313–318
Lalani AV, Lee SJ. Clinical echocardiography – an overview. Can Med Assoc J 1976; 114: 46–47, 50–54
Arancio F, Di Michele R, Denna V, Bertoni PD, Tosetto C, Bardon G, Carucci M, Delpini A. [Methods of determination of stroke volume from M-mode echocardiogram of the aortic valve and aortic root. A comparative evaluation]. G Ital Cardiol 1985; 15:600–607
Poutanen T, Jokinen E, Sairanen H, Tikanoja T. Left atrial and left ventricular function in healthy children and young adults assessed by three dimensional echocardiography. Heart 2003; 89:544–549
Akiba T, Yoshikawa M, Kinoda M, Otaki S, Ishii K, Kobayashi Y, Sato T. Angiocardiographic estimation of left and right ventricular volume characteristics in normal infants and children. Tohoku J Exp Med 1985; 146:313–320
Akiba T, Nakasato M, Sato S, Kikai A. Angiographic determination of left and right ventricular volumes and left ventricular mass in normal infants and children. Tohoku J Exp Med 1995; 177:153–160
Poutanen T, Tikanoja T, Sairanen H, Jokinen E. Normal aortic dimensions and flow in 168 children and young adults. Clin Physiol Funct Imaging 2003; 23:224–229
Monsel A, Salvat-Toussaint A, Durand P, Haas V, Baujard C, Rouleau P, El Aouadi S, Benhamou D, Asehnoune K. The transesophageal Doppler and hemodynamic effects of epidural anesthesia in infants anesthetized with sevoflurane and sufentanil. Anesth Analg 2007; 105:46–50
Pianosi P, Garros D. Comparison of impedance cardiography with indirect Fick (CO2) method of measuring cardiac output in healthy children during exercise. Am J Cardiol 1996; 77:745–749
Thangathurai D, Charbonnet C, Roessler P, Wo CC, Mikhail M, Yoahida R, Shoemaker WC. Continuous intraoperative noninvasive cardiac output monitoring using a new thoracic bioimpedance device. J Cardiothorac Vasc Anesth 1997; 11:440–444
Woo MA, Hamilton M, Stevenson LW, Vredevoe DL. Comparison of thermodilution and transthoracic electrical bioimpedance cardiac outputs. Heart Lung 1991; 20:357–362
Osthaus WA, Huber D, Beck C, Winterhalter M, Boethig D, Wessel A, Sumpelmann R. Comparison of electrical velocimetry and transpulmonary thermodilution for measuring cardiac output in piglets. Paediatr Anaesth 2007; 17:749–755
Boldt J, Kling D, Thiel A, Hempelmann G. [Non-invasive versus invasive cardiovascular monitoring. Determination of stroke volume and pulmonary hydration using a new bioimpedance monitor]. Anaesthesist 1988; 37:218–223
Imhoff M, Lehner JH, Lohlein D. Noninvasive whole-body electrical bioimpedance cardiac output and invasive thermodilution cardiac output in high-risk surgical patients. Crit Care Med 2000; 28:2812–2818
Braden DS, Leatherbury L, Treiber FA, Strong WB. Noninvasive assessment of cardiac output in children using impedance cardiography. Am Heart J 1990; 120:1166–1172
Acknowledgement
We are grateful for editorial assistance by Anne Gale of the Deutsches Herzzentrum Berlin.
Author information
Authors and Affiliations
Corresponding author
Additional information
Schubert S, Schmitz T, Weiss M, Nagdyman N, Huebler M, Alexi-Meskishvili V, Berger F, Stiller B. Continuous, non-invasive techniques to determine cardiac output in children after cardiac surgery: evaluation of transesophageal Doppler and electric velocimetry.
Rights and permissions
About this article
Cite this article
Schubert, S., Schmitz, T., Weiss, M. et al. Continuous, non-invasive techniques to determine cardiac output in children after cardiac surgery: evaluation of transesophageal Doppler and electric velocimetry. J Clin Monit Comput 22, 299–307 (2008). https://doi.org/10.1007/s10877-008-9133-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10877-008-9133-0