Abstract
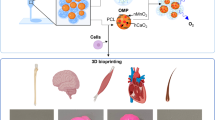
Natural hydrogels are widely used for 3D-bioprinting because of their qualities for tissue engineering. Recently, hydrogels have been combined with bioactive glasses, due to their angiogenic properties that aid tissue regeneration. In this work, we studied the printability and the rheological properties of gelatin–alginate–hyaluronic acid inks with 2–8% wt of 45S5 bioglass (BG) that followed a pseudoplastic behavior along the 3D-printing process. The reduction in the storage modulus of the inks after adding BG indicates that the microparticles might disrupt the polymeric network; furthermore, a reduction in the viscosity was determined at BG concentrations above 6%. Inks without BG or up to 2% evidenced the best printing fidelity on 10% infill scaffolds. The tensile modulus of crosslinked 40%-filled scaffolds increased from 130 kPa (without BG) to 160 kPa (6–8% BG). Moreover, a hydroxyapatite layer appeared in scaffolds containing BG 6% and 8% wt after being cultured for 2 days. Attachment and growth of fibroblasts on the scaffolds revealed their cytocompatibility, making these materials an alternative for further research on soft tissues regeneration.
Graphical abstract










Similar content being viewed by others
Data availability
The raw and processed data required to reproduce these findings are available to download from [https://data.mendeley.com/datasets/wwkpzj3vfk/2] [72].
References
Tarassoli SP, Jessop ZM, Al-Sabah A, Gao N, Whitaker S, Doak S, Whitaker IS (2018) Skin tissue engineering using 3D bioprinting: an evolving research field. J Plast Reconstr Aesthetic Surg 71:615–623. https://doi.org/10.1016/j.bjps.2017.12.006
Gao G, Cui X (2016) Three-dimensional bioprinting in tissue engineering and regenerative medicine. Biotechnol Lett 38:203–211. https://doi.org/10.1007/s10529-015-1975-1
Miri AK, Khalilpour A, Cecen B, Maharjan S, Shin SR, Khademhosseini A (2019) Multiscale bioprinting of vascularized models. Biomaterials 198:204–216. https://doi.org/10.1016/j.biomaterials.2018.08.006
Carrow JK, Kerativitayanan P, Jaiswal MK, Lokhande G, Gaharwar AK (2015) Polymers for bioprinting. In: Atala A, Yoo JJ (eds) Essentials of 3D biofabrication and translation. Elsevier Ltd, Berlin, pp 229–248. https://doi.org/10.1016/B978-0-12-800972-7.00013-X
Qiao Y, Xu S, Zhu T, Tang N, Bai X, Zheng C (2020) Preparation of printable double-network hydrogels with rapid self-healing and high elasticity based on hyaluronic acid for controlled drug release. Polymer (Guildf) 186:121994. https://doi.org/10.1016/j.polymer.2019.121994
Lu J, Guan F, Cui F, Sun X, Zhao L, Wang Y, Wang X (2019) Enhanced angiogenesis by the hyaluronic acid hydrogels immobilized with a VEGF mimetic peptide in a traumatic brain injury model in rats. Regen Biomater 6:325–334. https://doi.org/10.1093/rb/rbz027
Choi YS, Hong SR, Lee YM, Song KW, Park MH, Nam YS (1999) Studies on gelatin-containing artificial skin: II. Preparation and characterization of cross-linked gelatin-hyaluronate sponge. J Biomed Mater Res 48:631–639. https://doi.org/10.1002/(SICI)1097-4636(1999)48:5<631::AID-JBM6>3.0.CO;2-Y
Zhai P, Peng X, Li B, Liu Y, Sun H, Li X (2019) The application of hyaluronic acid in bone regeneration. Int J Biol Macromol. https://doi.org/10.1016/j.ijbiomac.2019.10.169
Contessi Negrini N, Celikkin N, Tarsini P, Farè S, Święszkowski W (2020) Three-dimensional printing of chemically crosslinked gelatin hydrogels for adipose tissue engineering. Biofabrication 12:025001. https://doi.org/10.1088/1758-5090/ab56f9
Axpe E, Oyen ML (2016) Applications of alginate-based bioinks in 3D bioprinting. Int J Mol Sci. https://doi.org/10.3390/ijms17121976
Aderibigbe BA, Buyana B (2018) Alginate in wound dressings. Pharmaceutics. https://doi.org/10.3390/pharmaceutics10020042
Gao T, Gillispie GJ, Copus JS, Kumar APR, Seol YJ, Atala A, Yoo JJ, Lee SJ (2018) Optimization of gelatin-alginate composite bioink printability using rheological parameters: a systematic approach. Biofabrication. https://doi.org/10.1088/1758-5090/aacdc7
Skardal A, Mack D, Kapetanovic E, Atala A, Jackson JD, Yoo J, Soker S (2012) Bioprinted amniotic fluid-derived stem cells accelerate healing of large skin wounds. Stem Cells Transl Med 1:792–802
Heidenreich AC, Pérez-Recalde M, González Wusener A, Hermida ÉB (2020) Collagen and chitosan blends for 3D bioprinting: a rheological and printability approach. Test, Polym. https://doi.org/10.1016/j.polymertesting.2019.106297
Wüst S, Godla ME, Müller R, Hofmann S (2014) Tunable hydrogel composite with two-step processing in combination with innovative hardware upgrade for cell-based three-dimensional bioprinting. Acta Biomater 10:630–640. https://doi.org/10.1016/j.actbio.2013.10.016
Shim JH, Lee JS, Kim JY, Cho DW (2012) Bioprinting of a mechanically enhanced three-dimensional dual cell-laden construct for osteochondral tissue engineering using a multi-head tissue/organ building system. J Micromechanics Microengineering. https://doi.org/10.1088/0960-1317/22/8/085014
Markstedt K, Mantas A, Tournier I, Martínez Ávila H, Hägg D, Gatenholm P (2015) 3D bioprinting human chondrocytes with nanocellulose-alginate bioink for cartilage tissue engineering applications. Biomacromolecules. 16:1489–1496. https://doi.org/10.1021/acs.biomac.5b00188
Wang Y, Huang X, Shen Y, Hang R, Zhang X, Wang Y, Yao X, Tang B (2019) Direct writing alginate bioink inside pre-polymers of hydrogels to create patterned vascular networks. J Mater Sci 54:7883–7892. https://doi.org/10.1007/s10853-019-03447-2
Mohandas A, Anisha BS, Chennazhi KP, Jayakumar R (2015) Chitosan-hyaluronic acid/VEGF loaded fibrin nanoparticles composite sponges for enhancing angiogenesis in wounds. Colloids Surfaces B Biointerfaces 127:105–113. https://doi.org/10.1016/j.colsurfb.2015.01.024
Xiong S, Zhang X, Lu P, Wu Y, Wang Q, Sun H, Heng BC, Bunpetch V, Zhang S, Ouyang H (2017) A Gelatin-sulfonated silk composite scaffold based on 3d printing technology enhances skin regeneration by stimulating epidermal growth and dermal neovascularization. Sci Rep 7:1–12. https://doi.org/10.1038/s41598-017-04149-y
Sun G, Shen YI, Kusuma S, Fox-Talbot K, Steenbergen CJ, Gerecht S (2011) Functional neovascularization of biodegradable dextran hydrogels with multiple angiogenic growth factors. Biomaterials 32:95–106. https://doi.org/10.1016/j.biomaterials.2010.08.091
Yu H, Peng J, Xu Y, Chang J, Li H (2016) Bioglass activated skin tissue engineering constructs for wound healing. ACS Appl Mater Interfaces 8:703–715. https://doi.org/10.1021/acsami.5b09853
Li H, Wu Z, Zhou Y, Chang J (2019) Bioglass for skin regeneration. In: García-Gareta E (eds) Biomaterials for skin repair and regeneration. Elsevier Ltd, Berlin, pp 225–250. https://doi.org/10.1016/B978-0-08-102546-8.00008-X
Leu A, Leach JK (2008) Proangiogenic potential of a collagen/bioactive glass substrate. Pharm Res 25:1222–1229. https://doi.org/10.1007/s11095-007-9508-9
Kolan KCR, Semon JA, Bromet B, Day DE, Leu MC (2019) Bioprinting with human stem cell-laden alginate-gelatin bioink and bioactive glass for tissue engineering. Int J Bioprinting 5:3–15. https://doi.org/10.18063/ijb.v5i2.2.204
Liu G, Pastakia M, Fenn MB, Kishore V (2016) Saos-2 cell-mediated mineralization on collagen gels: effect of densification and bioglass incorporation. J Biomed Mater Res—Part A 104:1121–1134. https://doi.org/10.1002/jbm.a.35651
Gao L, Zhou Y, Peng J, Xu C, Xu Q, Xing M, Chang J (2019) A novel dual-adhesive and bioactive hydrogel activated by bioglass for wound healing. NPG Asia Mater. https://doi.org/10.1038/s41427-019-0168-0
Zhou Z, Chen J, Peng C, Huang T, Zhou H, Ou B, Chen J, Liu Q, He S, Cao D, Huang H, Xiang L (2014) Fabrication and physical properties of gelatin/sodium alginate/hyaluronic acid composite wound dressing hydrogel. J Macromol Sci Part A Pure Appl Chem 51:318–325. https://doi.org/10.1080/10601325.2014.882693
Alemdar N (2016) Fabrication of a novel bone ash-reinforced gelatin/alginate/hyaluronic acid composite film for controlled drug delivery. Carbohydr Polym 151:1019–1026. https://doi.org/10.1016/j.carbpol.2016.06.033
Khorshidi S, Karkhaneh A (2016) A self-crosslinking tri-component hydrogel based on functionalized polysaccharides and gelatin for tissue engineering applications. Mater Lett 164:468–471. https://doi.org/10.1016/j.matlet.2015.11.041
Singh D, Tripathi A, Zo SM, Singh D, Han SS (2014) Synthesis of composite gelatin-hyaluronic acid-alginate porous scaffold and evaluation for in vitro stem cell growth and in vivo tissue integration. Colloids Surfaces B Biointerfaces 116:502–509. https://doi.org/10.1016/j.colsurfb.2014.01.049
Nocera AD, Comín R, Salvatierra NA, Cid MP (2018) Development of 3D printed fibrillar collagen scaffold for tissue engineering. Biomed Microdevices 20:1–13. https://doi.org/10.1007/s10544-018-0270-z
Amer MH, Rose FRAJ, Shakesheff KM, Modo M, White LJ (2017) Translational considerations in injectable cell-based therapeutics for neurological applications: concepts, progress and challenges. Med, Npj Regen. https://doi.org/10.1038/s41536-017-0028-x
Kyle S, Jessop ZM, Al-Sabah A, Whitaker IS (2017) Printability’’ of candidate biomaterials for extrusion based 3D printing: state-of-the-art. Adv Healthc Mater 6:1–16. https://doi.org/10.1002/adhm.201700264
Øyvind H, Harper DAT, Ryan PD (2001) PAST: paleontological statistics software package for education and data analysis. Palaeontol Electron 4:1–9
Ouyang L, Yao R, Zhao Y, Sun W (2016) Effect of bioink properties on printability and cell viability for 3D bioplotting of embryonic stem cells. Biofabrication 8:1–12. https://doi.org/10.1088/1758-5090/8/3/035020
Zuidema JM, Rivet CJ, Gilbert RJ, Morrison FA, A, (2014) protocol for rheological characterization of hydrogels for tissue engineering strategies. J Biomed Mater Res–Part B Appl Biomater 102:1063–1073. https://doi.org/10.1002/jbm.b.33088
Malvern Instruments (2012) White paper—understanding yield stress. https://www.atascientific.com.au/wp-content/uploads/2017/02/MRK1782-01.pdf. Accessed 16 June 2021
Malvern Instruments (2016) White paper—a basic introduction to rheology. https://cdn.technologynetworks.com/TN/Resources/PDF/WP160620BasicIntroRheology.pdf. Accessed 16 June 2021
Liu S, Hu Y, Zhang J, Bao S, Xian L, Dong X, Zheng W, Li Y, Gao H, Zhou W (2019) Bioactive and biocompatible macroporous scaffolds with tunable performances prepared based on 3D printing of the pre-crosslinked sodium alginate/hydroxyapatite hydrogel ink. Macromol Mater Eng 304:1–11. https://doi.org/10.1002/mame.201800698
Hazur J, Detsch R, Karakaya E, Kaschta J, Teßmar J, Schneidereit D, Friedrich O, Schubert DW, Boccaccini AR (2020) Improving alginate printability for biofabrication: establishment of a universal and homogeneous pre-crosslinking technique. Biofabrication. https://doi.org/10.1088/1758-5090/ab98e5
Daniel-da-Silva AL, Pinto F, Lopes-da-Silva JA, Trindade T, Goodfellow BJ, Gil AM (2008) Rheological behavior of thermoreversible κ-carrageenan/nanosilica gels. J Colloid Interface Sci 320:575–581. https://doi.org/10.1016/j.jcis.2008.01.035
Puvanenthiran A, Stevovitch-Rykner C, McCann TH, Day L (2014) Synergistic effect of milk solids and carrot cell wall particles on the rheology and texture of yoghurt gels. Food Res Int 62:701–708. https://doi.org/10.1016/j.foodres.2014.04.023
Lu HD, Charati MB, Kim IL, Burdick JA (2012) Injectable shear-thinning hydrogels engineered with a self-assembling Dock-and-Lock mechanism. Biomaterials 33:2145–2153. https://doi.org/10.1016/j.biomaterials.2011.11.076
Gao F, Xu Z, Liang Q, Liu B, Li H, Wu Y, Zhang Y, Lin Z, Wu M, Ruan C, Liu W (2018) Direct 3D printing of high strength biohybrid gradient hydrogel scaffolds for efficient repair of osteochondral defect. Adv Funct Mater 28:1–13. https://doi.org/10.1002/adfm.201706644
Guo Z, Xia J, Mi S, Sun W (2020) Mussel-inspired naturally derived double-network hydrogels and their application in 3D printing: from soft, injectable bioadhesives to mechanically strong hydrogels. ACS Biomater Sci Eng 6:1798–1808. https://doi.org/10.1021/acsbiomaterials.9b01864
Wang LL, Highley CB, Yeh Y-C, Galarraga JH, Uman S, Burdick JA (2018) 3D extrusion bioprinting of single- and double-network hydrogels containing dynamic covalent crosslinks, Arthritis Care Res. Biomed Mater Res A 106:865–875. https://doi.org/10.1002/jbm.a.36323
Wilson SA, Cross LM, Peak CW, Gaharwar AK (2017) Shear-thinning and thermo-reversible nanoengineered inks for 3D bioprinting. ACS Appl Mater Interfaces 9:43449–43458. https://doi.org/10.1021/acsami.7b13602
Townsend JM, Beck EC, Gehrke SH, Berkland CJ, Detamore MS (2019) Flow behavior prior to crosslinking: the need for precursor rheology for placement of hydrogels in medical applications and for 3D bioprinting. Prog Polym Sci 91:126–140. https://doi.org/10.1016/j.progpolymsci.2019.01.003
Picout DR, Ross-Murphy SB (2003) Rheology of biopolymer solutions and gels. Sci World J 3:105–121. https://doi.org/10.1100/tsw.2003.15
Iwamoto S, Kumagai H (1998) Analysis of the dielectric relaxation of a gelatin solution. Biosci Biotechnol Biochem 62:1381–1387. https://doi.org/10.1271/bbb.62.1381
Mukherjee A, Srinivas G, Bagchi B (2001) Reentrant behavior of relaxation time with viscosity at varying composition in binary mixtures. Phys Rev Lett 86:5926–5929. https://doi.org/10.1103/PhysRevLett.86.5926
Ahmed J, Mulla M, Maniruzzaman M (2019) Rheological and dielectric behavior of 3d-printable chitosan/graphene oxide hydrogels. ACS Biomater Sci Eng 6:88–99. https://doi.org/10.1021/acsbiomaterials.9b00201
Zhangfeng Z (2010) Rheology and phase change of polymers and vesicles. PhD Dissertation, National University of Singapore
Sepulveda P, Jones JR, Hench LL (2002) In vitro dissolution of melt-derived 45S5 and sol-gel derived 58S bioactive glasses. J Biomed Mater Res 62:301–311. https://doi.org/10.1002/jbm.10207
Waltimo T, Brunner TJ, Vollenweider M, Stark WJ, Zehnder M (2007) Antimicrobial effect of nanometric bioactive glass 45S5. J Dent Res 86:754–757. https://doi.org/10.1177/154405910708600813
Gao Q, He Y, Zhong Fu J, Liu A, Ma L (2015) Coaxial nozzle-assisted 3D bioprinting with built-in microchannels for nutrients delivery. Biomaterials 61:203–215. https://doi.org/10.1016/j.biomaterials.2015.05.031
Shamloo A, Sarmadi M, Aghababaie Z, Vossoughi M (2018) Accelerated full-thickness wound healing via sustained bFGF delivery based on a PVA/chitosan/gelatin hydrogel incorporating PCL microspheres. Int J Pharm 537:278–289. https://doi.org/10.1016/j.ijpharm.2017.12.045
Zhou Y, Gao L, Peng J, Xing M, Han Y, Wang X, Xu Y, Chang J (2018) Bioglass activated albumin hydrogels for wound healing. Adv Healthc Mater 7:1–13. https://doi.org/10.1002/adhm.201800144
Jiang Y, Zhou J, Shi H, Zhao G, Zhang Q, Feng C, Xv X (2020) Preparation of cellulose nanocrystal/oxidized dextran/gelatin (CNC/OD/GEL) hydrogels and fabrication of a CNC/OD/GEL scaffold by 3D printing. J Mater Sci 55:2618–2635. https://doi.org/10.1007/s10853-019-04186-0
Alexander H, Cook T (2006) Variations with age in the mechanical properties of human skin in vivo. J Tissue Viability 16:6–11. https://doi.org/10.1016/S0965-206X(06)63002-7
Guimarães CF, Gasperini L, Marques AP, Reis RL (2020) The stiffness of living tissues and its implications for tissue engineering. Nat Rev Mater 5:351–370. https://doi.org/10.1038/s41578-019-0169-1
Thompson ID, Hench LL (1998) Mechanical properties of bioactive glasses, glass-ceramics and composites. Proc Inst Mech Eng Part H J Eng Med 212:127–136. https://doi.org/10.1243/0954411981533908
Yoruç ABH, Aydınoğlu A (2017) The precursors effects on biomimetic hydroxyapatite ceramic powders. Mater Sci Eng C 75:934–946. https://doi.org/10.1016/j.msec.2017.02.049
Martín AR, Patel JM, Zlotnick HM, Carey JL, Mauck RL (2019) Emerging therapies for cartilage regeneration in currently excluded ‘red knee’ populations. Med, Npj Regen. https://doi.org/10.1038/s41536-019-0074-7
Gao G, Schilling AF, Yonezawa T, Wang J, Dai G, Cui X (2014) Bioactive nanoparticles stimulate bone tissue formation in bioprinted three-dimensional scaffold and human mesenchymal stem cells. Biotechnol J 9:1–23. https://doi.org/10.1002/biot.201400305.Submitted
Fedorovich NE, Schuurman W, Wijnberg HM, Prins HJ, Van Weeren PR, Malda J, Alblas J, Dhert WJA (2012) Biofabrication of osteochondral tissue equivalents by printing topologically defined, cell-laden hydrogel scaffolds. Tissue Eng—Part C Methods 18:33–44. https://doi.org/10.1089/ten.tec.2011.0060
Okabayashi R, Nakamura M, Okabayashi T, Tanaka Y, Nagai A, Yamashita K (2009) Efficacy of polarized hydroxyapatite and silk fibroin composite dressing gel on epidermal recovery from full-thickness skin wounds. J Biomed Mater Res—Part B Appl Biomater 90:641–646. https://doi.org/10.1002/jbm.b.31329
Ji DY, Kuo TF, Da Wu H, Yang JC, Lee SY (2012) A novel injectable chitosan/polyglutamate polyelectrolyte complex hydrogel with hydroxyapatite for soft-tissue augmentation. Carbohydr Polym 89:1123–1130. https://doi.org/10.1016/j.carbpol.2012.03.083
Liu M, Huang C, Zhao Z, Wang A, Li P, Fan Y, Zhou G (2019) Nano-hydroxyapatite(n-HA) involved in the regeneration of rat nerve injury triggered by overloading stretch. Med Nov Technol Devices 4:100022. https://doi.org/10.1016/j.medntd.2019.100022
Ribeiro N, Sousa A, Cunha-Reis C, Oliveira AL, Granja PL, Monteiro FJ, Sousa SR (2021) New prospects in skin regeneration and repair using nanophased hydroxyapatite embedded in collagen nanofibers, nanomedicine nanotechnology. Biol Med 33:102353. https://doi.org/10.1016/j.nano.2020.102353
Bertuola M, Aráoz B, Gilabert U, Gonzalez-Wusener A, Pérez-Recalde M, Arregui C, Hermida ÉB (2020) Inks of gelatin-alginate-hyaluronic acid for 3D printing: effects of bioglass 45S5 addition on printability, rheology and on scaffold tensile modulus. Mendeley Data. https://doi.org/10.17632/wwkpzj3vfk.4
Acknowledgements
Authors would like to acknowledge Lantos Lab for SEM-EDS measurements, Laboratory of Applied Crystallography of National University of San Martin for the X-ray determination, LIFE-SI and its developer Adén Díaz Nocera for his constant support with the 3D-bioprinter and Ing. Lucía Garaventa for the valuable discussions about the rheology of the systems.
Funding
This study was funded by the Argentinian Ministry of Education through its Secretary of University Policies—“Universities Adding Value” (Grant: RESOL-2016–2373-E-APN-SECPU#ME, Project: Bioinks). M.B. is a postdoctoral fellow of CONICET. B.A., A.G.W., M.P.R., C.O.A. and E.B.H. are researchers at CONICET.
Author information
Authors and Affiliations
Contributions
UG, AG-W, ÉBH and CA collected resources. MP-R, MB and BA performed writing—original draft. MP-R, MB, BA and ÉBH performed writing—review & editing. BA and ÉBH were responsible for supervision and performed project administration. ÉBH was responsible for funding acquisition. MP-R, AG-W, CA and MB were involved in visualization. MB was involved in formal analysis and validation. AG-W, MB, BA and CA performed methodology. UG, MB and BA were involved in investigation. Conceptualization was performed by MB and BA.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Handling Editor: Maude Jimenez.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Supplementary file2 (MP4 374864 KB)
Rights and permissions
About this article
Cite this article
Bertuola, M., Aráoz, B., Gilabert, U. et al. Gelatin–alginate–hyaluronic acid inks for 3D printing: effects of bioglass addition on printability, rheology and scaffold tensile modulus. J Mater Sci 56, 15327–15343 (2021). https://doi.org/10.1007/s10853-021-06250-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10853-021-06250-0