Abstract
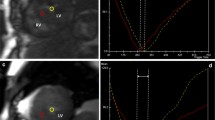
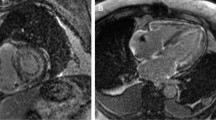
Late Gadolinium Enhancement (LGE) pattern of cardiac amyloidosis (CA) at cardiac magnetic resonance (CMR) examination is absent in approximately 30 % of patients. We tested whether the evaluation of myocardial gadolinium signal intensity (SI) decay (SID) has a higher diagnostic accuracy for CA. CMR was performed in 59 patients with systemic AL amyloidosis (36 males, 69 ± 10 years, mean ± SD), and 20 age/sex-matched healthy controls. LGE images were acquired every minute up to 8 min after gadolinium injection (time of inversion 250 ms). SI regions of interest were plotted in SI/time curves for endocardial (Endo) and epicardial layer of interventricular septum, cavity, and skeletal muscle as reference. SID (a negative exponential function described by the parameter TSID) was expressed as number of heart beats (HB) from each ROI. The typical LGE pattern for CA was detected in 42 patients (Ty-LGE), while 17 showed either absent LGE or an atypical pattern (ATy-LGE). A definite CA diagnosis was confirmed in all Ty-LGE patients and in 10/17 ATy-LGE patients. At ROC analysis Endo-TSID was the most accurate parameter to distinguish Ty-LGE and ATy-LGE patients from controls. A 269 HB threshold (mean + 2 SD Endo-TSID measured in controls) identified 51/52 patients with definite CA diagnosis, with 98 % sensitivity, 93 % specificity, and 96 % diagnostic accuracy. A direct relation was found between the extracellular volume and Endo-TSID in CA patients (r 0.72, 95 % CI 0.37–089, p < 0.001). the analysis of myocardial SID after gadolinium injection improves the accuracy of CMR for CA diagnosis.





Similar content being viewed by others
Abbreviations
- AL:
-
Amyloid light chain
- ARB:
-
Angiotensin receptor blocker
- BMI:
-
Body mass index
- CA:
-
Cardiac amyloidosis
- CKD:
-
Chronic kidney disease
- CMR:
-
Cardiac magnetic resonance
- COPD:
-
Chronic obstructive pulmonary disease
- EGFR:
-
Estimated glomerular filtration rate
- LGE:
-
Late gadolinium enhancement
- MGUS:
-
Monoclonal gammopathy of undetermined significance
- NYHA:
-
New York Heart Association
- ROI:
-
Region of interest
- SD:
-
Standard deviation
- SID:
-
Signal intensity decay
References
Falk RH (2005) Diagnosis and management of the cardiac amyloidosis. Circulation 112:2047–2060
Gertz MA, Comenzo R, Falk RH, Fermand JP, Hazenberg BP, Hawkins PN, Merlini G, Moreau P, Ronco P, Sanchorawala V, Sezer O, Solomon A, Grateau G (2005) Definition of organ involvement and treatment response in immunoglobulin light chain amyloidosis (AL): a consensus opinion from the 10th International Symposium on Amyloid and Amyloidosis, Tours, France, 18–22 April 2004. Am J Hematol 79:319–328
Sanchorawala V (2006) Light-chain (AL) amyloidosis: diagnosis and treatment. Clin J Am Soc Nephrol 1:1331–1341
Maceira AM, Joshi J, Prasad SK, Moon JC, Perugini E, Harding I, Sheppard MN, Poole-Wilson PA, Hawkins PN, Pennell DJ (2005) Cardiovascular magnetic resonance in cardiac amyloidosis. Circulation 111:186–193
Vogelsberg H, Mahrholdt H, Deluigi CC, Yilmaz A, Kispert EM, Greulich S, Klingel K, Kandolf R, Sechtem U (2008) Cardiovascular magnetic resonance in clinically suspected cardiac amyloidosis: noninvasive imaging compared to endomyocardial biopsy. J Am Coll Cardiol 51:1022–1030
Ruberg FL, Appelbaum E, Davidoff R, Ozonoff A, Kissinger KV, Harrigan C, Skinner M, Manning WJ (2009) Diagnostic and prognostic utility of cardiovascular magnetic resonance imaging in light-chain cardiac amyloidosis. Am J Cardiol 103:544–549
Sharma P, Socolow J, Patel S, Pettigrew RI, Oshinski JN (2006) Effect of Gd-DTPA-BMA on blood and myocardial T1 at 1.5T and 3T in humans. J Magn Reson Imaging 23:323–330
Iles L, Pfluger H, Phrommintikul A, Cherayath J, Aksit P, Gupta SN, Kaye DM, Taylor AJ (2008) Evaluation of diffuse myocardial fibrosis in heart failure with cardiac magnetic resonance contrast-enhanced T1 mapping. J Am Coll Cardiol 52:1574–1580
Piechnik SK, Ferreira VM, Dall’Armellina E, Cochlin LE, Greiser A, Neubauer S, Robson MD (2010) Shortened Modified Look-Locker Inversion recovery (ShMOLLI) for clinical myocardial T1-mapping at 1.5 and 3 T within a 9 heartbeat breathhold. J Cardiovasc Magn Reson 12:69
Flett AS, Hayward MP, Ashworth MT, Hansen MS, Taylor AM, Elliott PM, McGregor C, Moon JC (2010) Equilibrium contrast cardiovascular magnetic resonance for the measurement of diffuse myocardial fibrosis: preliminary validation in humans. Circulation 122:138–144
Fontana M, White SK, Banypersad SM, Sado DM, Maestrini V, Flett AS, Piechnik SK, Neubauer S, Roberts N, Moon JC (2012) Comparison of T1 mapping techniques for ECV quantification. Histological validation and reproducibility of ShMOLLI versus multibreath-hold T1 quantification equilibrium contrast CMR. J Cardiovasc Magn Reson 14:88
Milanesi M, Barison A, Positano V, Masci PG, De Marchi D, Marinelli L, Hardy CJ, Foo TK, Landini L, Lombardi M (2013) Modified cine inversion recovery pulse sequence for the quantification of myocardial T1 and gadolinium partition coefficient. J Magn Reson Imaging 37:109–118
Sechtem U, Pflugfelder P, Higgins CB (1987) Quantification of cardiac function by conventional and cine magnetic resonance imaging. Cardiovasc Intervent Radiol 10:365–373
Maceira AM, Prasad SK, Khan M, Pennell DJ (2006) Reference right ventricular systolic and diastolic function normalized to age, gender and body surface area from steady-state free precession cardiovascular magnetic resonance. Eur Heart J 27:2879–2888
Maceira AM, Prasad SK, Khan M, Pennell DJ (2006) Normalized left ventricular systolic and diastolic function by steady state free precession cardiovascular magnetic resonance. J Cardiovasc Magn Reson 8:417–426
Aquaro GD, Todiere G, Barison A, Strata E, Marzilli M, Pingitore A, Lombardi M (2011) Myocardial blood flow and fibrosis in hypertrophic cardiomyopathy. J Card Fail 17:384–391
Tofts PS, Brix G, Buckley DL, Evelhoch JL, Henderson E, Knopp MV, Larsson HB, Lee TY, Mayr NA, Parker GJ, Port RE, Taylor J, Weisskoff RM (1999) Estimating kinetic parameters from dynamic contrast-enhanced T(1)-weighted MRI of a diffusible tracer: standardized quantities and symbols. J Magn Reson Imaging 10:223–232
Perugini E, Rapezzi C, Piva T, Leone O, Bacchi-Reggiani L, Riva L, Salvi F, Lovato L, Branzi A, Fattori R (2006) Non-invasive evaluation of the myocardial substrate of cardiac amyloidosis by gadolinium cardiac magnetic resonance. Heart 92:343–349
Banypersad SM, Sado DM, Flett AS, Gibbs SD, Pinney JH, Maestrini V, Cox AT, Fontana M, Whelan CJ, Wechalekar AD, Hawkins PN, Moon JC (2013) Quantification of myocardial extracellular volume fraction in systemic AL amyloidosis: an equilibrium contrast cardiovascular magnetic resonance study. Circ Cardiovasc Imaging 6:34–39
Maceira AM, Prasad SK, Hawkins PN, Roughton M, Pennell DJ (2008) Cardiovascular magnetic resonance and prognosis in cardiac amyloidosis. J Cardiovasc Magn Reson 25:10–54
Conflict of interest
No conflict of interest declared.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Aquaro, G.D., Pugliese, N.R., Perfetto, F. et al. Myocardial signal intensity decay after gadolinium injection: a fast and effective method for the diagnosis of cardiac amyloidosis. Int J Cardiovasc Imaging 30, 1105–1115 (2014). https://doi.org/10.1007/s10554-014-0436-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10554-014-0436-6