Abstract
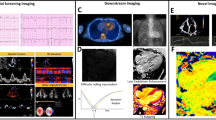
Cardiac amyloidosis (CA) is an underdiagnosed form of restrictive cardiomyopathy leading to a rapid progression into heart failure. Evaluation of CA requires a multimodality approach making use of echocardiography, cardiac magnetic imaging (CMR), and nuclear imaging. With superior tissue characterization, high-resolution imaging, and precise cardiac assessment, CMR has emerged as a versatile tool in the workup of cardiac amyloidosis with a wide array of parameters both visual and quantitative. This includes late gadolinium enhancement patterns, T1/T2 mapping, and extracellular volume (ECV) measurement providing robust diagnostic accuracies, patient stratification, and prognostication. Recent advancements have introduced new measures able to identify early disease, track disease progression, and response to therapy positioning CMR as an instrumental imaging modality in the era of rising interest in CA screening and emerging effective therapies.


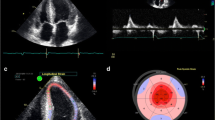
Similar content being viewed by others
Data availability
Not applicable.
Code availability
Not applicable.
References
Dorbala S, Ando Y, Bokhari S et al (2020) ASNC/AHA/ASE/EANM/HFSA/ISA/SCMR/SNMMI expert consensus recommendations for multimodality imaging in cardiac amyloidosis: part 2 of 2-diagnostic criteria and appropriate utilization. J Nucl Cardiol 27(2):659–673. https://doi.org/10.1007/s12350-019-01761-5. Accessed 25 Oct 2021
Dorbala S, Ando Y, Bokhari S et al (2019) ASNC/AHA/ASE/EANM/HFSA/ISA/SCMR/SNMMI expert consensus recommendations for multimodality imaging in cardiac amyloidosis: part 1 of 2-evidence base and standardized methods of imaging. J Nucl Cardiol 26(6):2065–2123. https://doi.org/10.1007/s12350-019-01760-6. Accessed 25 Oct 2021
Maceira AM, Joshi J, Prasad SK et al (2005) Cardiovascular magnetic resonance in cardiac amyloidosis. Circulation 111(2):186–193. https://doi.org/10.1161/01.CIR.0000152819.97857.9D. Accessed 19 Oct 2021
Kellman P, Arai AE, McVeigh ER, Aletras AH (2002) Phase-sensitive inversion recovery for detecting myocardial infarction using gadolinium-delayed hyperenhancement. Magn Reson Med. 47(2):372–383. https://doi.org/10.1002/mrm.10051. Accessed 25 Oct 2021
Fontana M, Pica S, Reant P et al (2015) Prognostic value of late gadolinium enhancement cardiovascular magnetic resonance in cardiac amyloidosis. Circulation. 2015;132(16):1570–1579. https://doi.org/10.1161/CIRCULATIONAHA.115.016567. Accessed 25 Oct 2021
Vogelsberg H, Mahrholdt H, Deluigi CC et al (2008) Cardiovascular magnetic resonance in clinically suspected cardiac amyloidosis: noninvasive imaging compared to endomyocardial biopsy. J Am Coll Cardiol 51(10):1022–1030. https://doi.org/10.1016/j.jacc.2007.10.049. Accessed 25 Oct 2021
Syed IS, Glockner JF, Feng D et al (2010) Role of cardiac magnetic resonance imaging in the detection of cardiac amyloidosis. JACC Cardiovasc Imaging 3(2):155–164. https://doi.org/10.1016/j.jcmg.2009.09.023. Accessed 25 Oct 2021
Ruberg FL, Appelbaum E, Davidoff R et al (2009) Diagnostic and prognostic utility of cardiovascular magnetic resonance imaging in light-chain cardiac amyloidosis. Am J Cardiol 103(4):544–549. https://doi.org/10.1016/j.amjcard.2008.09.105. Accessed 25 Oct 2021
Karamitsos TD, Piechnik SK, Banypersad SM et al (2013) Noncontrast T1 mapping for the diagnosis of cardiac amyloidosis. JACC Cardiovasc Imaging 6(4):488–497. https://doi.org/10.1016/j.jcmg.2012.11.013. Accessed 19 Oct 2021
Austin BA, Tang WHW, Rodriguez ER et al (2009) Delayed hyper-enhancement magnetic resonance imaging provides incremental diagnostic and prognostic utility in suspected cardiac amyloidosis. JACC Cardiovasc Imaging 2(12):1369–1377. https://doi.org/10.1016/j.jcmg.2009.08.008. Accessed 25 Oct 2021
Takeda M, Amano Y, Tachi M, Tani H, Mizuno K, Kumita S (2013) MRI differentiation of cardiomyopathy showing left ventricular hypertrophy and heart failure: differentiation between cardiac amyloidosis, hypertrophic cardiomyopathy, and hypertensive heart disease. Jpn J Radiol 31(10):693–700. https://doi.org/10.1007/s11604-013-0238-0. Accessed 25 Oct 2021
Deux J, Damy T, Rahmouni A, Mayer J, Planté-Bordeneuve V (2014) Noninvasive detection of cardiac involvement in patients with hereditary transthyretin associated amyloidosis using cardiac magnetic resonance imaging: a prospective study. Amyloid 21(4):246–255. https://doi.org/10.3109/13506129.2014.956924. Accessed 25 Oct 2021
Zhao L, Tian Z, Fang Q (2016) Diagnostic accuracy of cardiovascular magnetic resonance for patients with suspected cardiac amyloidosis: a systematic review and meta-analysis. BMC Cardiovasc Disord 16:129. https://doi.org/10.1186/s12872-016-0311-6. Accessed 25 Oct 2021
Martinez-Naharro A, Treibel TA, Abdel-Gadir A et al (2017) Magnetic resonance in transthyretin cardiac amyloidosis. J Am Coll Cardiol 70(4):466–477. https://doi.org/10.1016/j.jacc.2017.05.053. Accessed 19 Oct 2021
Dungu JN, Valencia O, Pinney JH et al (2014) CMR-based differentiation of AL and ATTR cardiac amyloidosis. JACC Cardiovasc Imaging 7(2):133–142.https://doi.org/10.1016/j.jcmg.2013.08.015. Accessed 25 Oct 2021
Martinez-Naharro A, Treibel TA, Abdel-Gadir A et al (2017) Magnetic resonance in transthyretin cardiac amyloidosis. J Am Coll Cardiol 70(4):466–477. https://doi.org/10.1016/j.jacc.2017.05.053. Accessed 25 Oct 2021
Martinez-Naharro A, Abdel-Gadir A, Treibel TA et al (2017) CMR-verified regression of cardiac AL amyloid after chemotherapy. JACC Cardiovasc Imaging 11(1):152–154. https://doi.org/10.1016/j.jcmg.2017.02.012. Accessed 19 Oct 2021
White JA, Kim HW, Shah D et al (2014) CMR imaging with rapid visual T1 assessment predicts mortality in patients suspected of cardiac amyloidosis. JACC Cardiovasc Imaging 7(2):143–156. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3951756/. https://doi.org/10.1016/j.jcmg.2013.09.019. Accessed 25 Oct 2021
Fontana M, Banypersad SM, Treibel TA et al (2014) Native T1 mapping in transthyretin amyloidosis. JACC Cardiovasc Imaging 7(2):157–165. https://doi.org/10.1016/j.jcmg.2013.10.008. Accessed 25 Oct 2021
Moon JC, Messroghli DR, Kellman P et al (2013) Myocardial T1 mapping and extracellular volume quantification: a society for cardiovascular magnetic resonance (SCMR) and CMR working group of the european society of cardiology consensus statement. J Cardiovasc Magn Reson 15(1):92. https://doi.org/10.1186/1532-429X-15-92
Banypersad SM, Sado DM, Flett AS et al (2013) Quantification of myocardial extracellular volume fraction in systemic AL amyloidosis. Circulation: Cardiovascular Imaging. 6(1):34–39. https://doi.org/10.1161/CIRCIMAGING.112.978627. Accessed 19 Oct 2021
Messroghli DR, Moon JC, Ferreira VM et al (2017) Clinical recommendations for cardiovascular magnetic resonance mapping of T1, T2, T2* and extracellular volume: a consensus statement by the society for cardiovascular magnetic resonance (SCMR) endorsed by the european association for cardiovascular imaging (EACVI). J Cardiovasc Magn Reson 19(1):75. https://doi.org/10.1186/s12968-017-0389-8. Accessed 25 Oct 2021
Mekinian A, Lions C, Leleu X et al (2010) Prognosis assessment of cardiac involvement in systemic AL amyloidosis by magnetic resonance imaging. Am J Med 123(9):864–868. https://doi.org/10.1016/j.amjmed.2010.03.022. Accessed 25 Oct 2021
Fontana M, Treibel TA, Martinez-Naharro A et al (2017) A case report in cardiovascular magnetic resonance: the contrast agent matters in amyloid. BMC Med Imaging 17(1):3. https://doi.org/10.1186/s12880-016-0173-5. Accessed 25 Oct 2021
Banypersad SM, Fontana M, Maestrini V et al (2015) T1 mapping and survival in systemic light-chain amyloidosis. Eur Heart J 36(4):244–251. https://doi.org/10.1093/eurheartj/ehu444. Accessed 19 Oct 2021
Martinez-Naharro A, Kotecha T, Norrington K et al (2019) Native T1 and extracellular volume in Transthyretin amyloidosis. JACC Cardiovasc Imaging 12(5):810–819. https://doi.org/10.1016/j.jcmg.2018.02.006. Accessed 19 Oct 2021
Raina S, Lensing SY, Nairooz RS et al (2016) Prognostic value of late gadolinium enhancement CMR in systemic amyloidosis. JACC Cardiovasc Imaging 9(11):1267–1277. https://doi.org/10.1016/j.jcmg.2016.01.036. Accessed 25 Oct 2021
Bulluck H, White SK, Rosmini S et al (2015) T1 mapping and T2 mapping at 3T for quantifying the area-at-risk in reperfused STEMI patients. J Cardiovasc Magn Reson 17(1):73. https://doi.org/10.1186/s12968-015-0173-6
Lurz P, Luecke C, Eitel I et al (2016) Comprehensive cardiac magnetic resonance imaging in patients with suspected myocarditis: the MyoRacer-trial. J Am Coll Cardiol 67(15):1800–1811. https://doi.org/10.1016/j.jacc.2016.02.013. Accessed 5 Nov 2021
Bohnen S, Radunski UK, Lund GK et al (2015) Performance of T1 and T2 mapping cardiovascular magnetic resonance to detect active myocarditis in patients with recent-onset heart failure. Circulation: Cardiovas Imaging 8(6):e003073. https://doi.org/10.1161/circimaging.114.003073. Accessed 5 Nov 2021
Legou F, Tacher V, Damy T et al (2017) Usefulness of T2 ratio in the diagnosis and prognosis of cardiac amyloidosis using cardiac MR imaging. Diagn Interv Imaging 98(2):125–132. https://doi.org/10.1016/j.diii.2016.08.007. Accessed 5 Nov 2021
Wassmuth R, Abdel-Aty H, Bohl S, Schulz-Menger J (2011) Prognostic impact of T2-weighted CMR imaging for cardiac amyloidosis. Eur Radiol 21(8):1643–1650. https://doi.org/10.1007/s00330-011-2109-3. Accessed 5 Nov 2021
Kotecha T, Martinez-Naharro A, Treibel TA et al (2018) Myocardial edema and prognosis in Amyloidosis. J Am Coll Cardiol 71(25):2919–2931. https://doi.org/10.1016/j.jacc.2018.03.536. Accessed 5 Nov 2021
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Research studies involving humans and/or animals
Not applicable.
Ethics approval
Not applicable.
Consent to participate
Not applicable.
Consent for publication
Not applicable.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Saad, J.M., Ahmed, A.I., Han, Y. et al. Cardiovascular magnetic resonance for suspected cardiac amyloidosis: where are we now?. Heart Fail Rev 27, 1543–1548 (2022). https://doi.org/10.1007/s10741-022-10226-w
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10741-022-10226-w