Abstract
Background
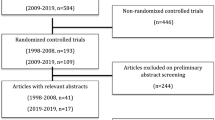
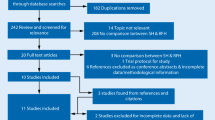
Severe life-threatening complications have been reported from the use of procedure for prolapsed haemorrhoids (PPH). First, we assessed post-operative complication rates over 4 years of PPH experience. We then sought to assess the impact of selection criteria for patients receiving PPH on post-operative complication rates and review our findings in the context of published literature.
Methods
Over a 4-year period 2006–2010 at Hinchingbrooke Hospital, all 118 patients receiving PPH were audited for readmissions with post-operative complications using the admission database. A further retrospective audit of 50 patients’ notes assessed the impact of selection criteria for PPH on post-operative complication rates. All PPH operations were performed by one of two senior colorectal consultants using the standard technique with a circular stapler.
Results
Of the 118 patients from the 4-year audit, 12 (10 %) patients were readmitted. Two (1.7 %) of these 12 patients had post-operative pain, six (5.1 %) had rectal bleeding, three (2.5 %) had urinary retention, and one (0.8 %) had localised infection. There was one (0.8 %) patient mortality resulting from severe sepsis from an infected intra-abdominal haemorrhagic collection. In the following audit of 50 patients’ notes, 15 patients had internal prolapsed haemorrhoids alone, of which one (6.6 %) experienced post-operative complications compared with six (55 %) of the 11 patients who had haemorrhoids and skin tags.
Conclusions
With careful selection of patients, PPH may be indicated for prolapsed internal haemorrhoids. More specific national guidelines are required with regard to contraindications to PPH.
Similar content being viewed by others
References
Burch J, Epstein D, Baba-Akbari A et al (2008) Stapled haemorrhoidectomy (haemorrhoidopexy) for the treatment of haemorrhoids: a systematic review and economic evaluation. Health Technol Assess 12:1–193
Madiba TE, Esterhuizen TM, Thomson SR (2009) Procedure for prolapsed haemorrhoids versus excisional haemorrhoidectomy: a systematic review and meta-analysis. S Afr Med J 99:43–53
National Institute of Clinical excellence (2010) Stapled haemorrhoidopexy for treatment of haemorrhoids. http://www.nice.org.uk/nicemedia/live/11835/36250/36250.pdf
Tjandra JJ, Chandra MK (2007) Systemic review on the procedure for prolapsed and haemorrhoids (stapled haemorrhoidopexy). Dis Colon Rectum 50:878–892
Senagore AJ, Singer M, Abcarian H et al (2004) Procedure for prolapse and hemorrhoids (PPH) multicenter study group. A prospective, randomized, controlled multicenter trial comparing stapled hemorrhoidopexy and Ferguson hemorrhoidectomy: perioperative and one-year results. Dis Colon Rectum 47:1824–1836
Beattie GC, McAdam TK, McIntosh SA, Loudon MA (2006) Day case stapled haemorrhoidopexy for prolapsing haemorrhoids. Colorectal Dis 8:56–61
Finco C, Sarzo G, Savastano S, Degregori S, Merigliano S (2006) Stapled haemorrhoidopexy in fourth degree haemorrhoidal prolapse: is it worthwhile? Colorectal Dis 8:130–134
Grigoropoulos P, Kalles V, Papapanagiotou I et al (2011) Early and late complications of stapled haemorrhoidopexy: a 6-year experience from a single surgical clinic. Tech Coloproctol 15:S79–S81
Ng KH, Ho KS, Ooi BS, Tang CL, Eu KW (2006) Experience of 3711 stapled haemorrhoidectomy operations. Br J Surg 93:226–230
Pescatori M, Gagliardi G (2008) Postoperative complications after procedure for prolapsed hemorrhoids (PPH) and stapled transanal rectal resection (STARR) procedures. Tech Coloproctol 12:7–19
Van de Stadt J, D’Hoore A, Duinslaeger M, Chasse E, Penninckx F (2005) Long-term results after excision haemorrhoidectomy versus stapled haemorrhoidopexy for prolapsing haemorrhoids; a Belgian prospective randomized trial. Acta Chir Belg 105:44–52
Cirocco WC (2008) Life threatening sepsis and mortality following stapled hemorrhoidopexy. Surgery 143:824–829
Pescatori M (2011) Rectal pocket syndrome following PPH and rectosigmoid resection. Tech Coloproctol 15:363
McCloud JM, Jameson JS, Scott AN (2006) Life-threatening sepsis following treatment for haemorrhoids: a systematic review. Colorectal Dis 8:748–755
http://www.fda.gov/cdrh/index.html. Accessed 23 April 2012
Faucheron JL, Voirin D, Abba J (2012) Rectal perforation with life-threatening peritonitis following stapled haemorrhoidopexy. Br J Surg 99:746–753
Gao XH, Wang HT, Chen JG, Yang XD, Qian Q, Fu CG (2010) Rectal perforation after procedure for prolapse and hemorrhoids: possible causes. Dis Colon Rectum 53:1439–1445
Acknowledgments
The authors would like to thank Hinchingbrooke Audit Department for helping to procure notes for the retrospective notes audit.
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Butterworth, J.W., Peravali, R., Anwar, R. et al. A four-year retrospective study and review of selection criteria and post-operative complications of stapled haemorrhoidopexy. Tech Coloproctol 16, 369–372 (2012). https://doi.org/10.1007/s10151-012-0862-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10151-012-0862-1