Abstract
Background
The aim of this study is to compare and evaluate the results of stapled haemorrhoidectomy performed under local anaesthesia against those performed under spinal anaesthesia in terms of postoperative pain, bleeding per rectum, the time needed for return to normal bowel habits and resumption of normal physical activities (within one week of surgery), incidence of recurrence and stenosis (within three months of surgery).
Methodology
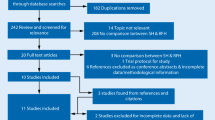
An open, prospective, single centre randomized controlled trial was conducted at PGIMER, DR. RML Hospital, New Delhi for a period of 15 months w.e.f. 01.11.2011. The study included 50 patients over the age of eighteen years, with bleeding per rectum and grades 3 and 4 haemorrhoids, who were randomized to either local or spinal anaesthesia. Group I included study subjects who had undergone stapler haemorrhoidectomy under local anaesthesia and group II comprised those submitted to the same procedure under spinal anaesthesia.
Results
A significant difference in duration of hospital stay post surgery was noted between the two groups. Those undergoing the procedure under local anaesthesia were discharged far sooner than those receiving spinal anaesthesia. It was also found that the immediate postoperative complications, namely headache and retention of urine, were common among group II patients whereas none of the patients in group I reported similar complaints. Otherwise, there was little significant difference between the two groups in terms of pain scores, postoperative bleeding per rectum, and the time required for the return of normal bowel habits and resumption of normal physical activities
Conclusion
Stapler haemorrhoidectomy under pudendal block with local skin and subcutaneous anaesthesia is a feasible and effective treatment modality.
Similar content being viewed by others
References
Thompson WHF. The nature of hemorrhoids. Br J Surg 1975; 62:542–52
Loder PB, Kamm MA, Nichells RJ, et al. Hemorrhoids pathology, pathophysiology and aetiology. Br J Surg 1994; 1:946–54
Pienninger JL, Surrell J. Non surgical treatment options for internal hemorrhoids. Am Fam Physician 1995; 52:821–34
Godeberge P. Daflon 500mg in the treatment ofhemorrhoidal disease: a demonstrated efficacy in comparison with placebo. Angiology 1994; 45:574–8
Steele RJG, Campbell K. Disorders of the anal canal: Haemorrhoids. Essential Surgical Practice; 4th edition: London, Arnold 2002; pp.627–45
Manzoor Ali, Zahid Ahmad Hashmi, Adnan Zafar. Swat, Haemorrhoidectomy using pudendal nerve, block and local infiltration. Gomal Journal of Medical Sciences 2010; 8:185–9
Abramowitz L, Godeberge P, Staumont G, et al. Clinical practice guidelines for the treatment of hemorrhoidal disease [in French]. Gastroenterol Clin Biol 2001; 25:674–702
Hulme-Moir M, Bartolo DC. Hemorrhoids. Gastroenterol Clin North Am 2001; 30:183–97
Morgado PJ, Suárez JA, Gómez LG, et al. Histoclinical basis for a new classification of hemorrhoidal disease. Dis Colon Rectum. 1988; 31:474–80
Aigner F, Gruber H, Conrad F, et al. Revised morphology and hemodynamics of the anorectal vascular plexus: impact on the course of hemorrhoidal disease. Int J Colorectal Dis 2009; 24:105–13
Chung YC, Hou YC, Pan AC. Endoglin (CD105) expression in the development of haemorrhoids. Eur J Clin Invest 2004; 34:107–12
Goenka MK, Kochhar R, Nagi B, et al. Rectosigmoid varices and other mucogal changes in patients with portal hypertension. Am J GAstroenterol. 1991; 86:1185–9.
Han W, Wang ZJ, Zhao B, et al. Pathologic change of elastic fibers with difference of microvessel density and expression of angiogenesis-related proteins in internal hemorrhoid tissues. Zhonghua Weichang Waike Zazhi 2005; 8:56–9
Yoon SO, Park SJ, Yun CH, et al. Roles of matrix metalloproteinases in tumor metastasis and angiogenesis. J Biochem Mol Biol 2003; 36:128–37
Aigner F, Bodner G, Gruber H, et al. The vascular nature of hemorrhoids. J GAstrointest Surg 2006; 10:1044–50
Stankevicius E, Kevelaitis E, Vainorius E, et al. Role of nitric oxide and other endothelium-derived factors. Medicina (Kaunas) 2003; 39:333–41
Sun WM, Peck RJ, Shorthouse AJ, et al. Haemorrhoids are associated not with hypertrophy of the internal anal sphincter, but with hypertension of the anal cushions. Br J Surg 1992; 79:592–4
Ho YH, Seow-Choen F, Goh HS. Haemorrhoidectomy and disordered rectal and anal physiology in patients with prolapsed haemorrhoids. Br J Surg 1995; 82:596–8
Patel M. Haemorrhoids (Piles). Http//www.proctocure. com/haemorrhoids. Htm. Shreyas Ano-rectal Hospital and Research Centre
Longo A. Treatment of haemorrhoidal disease by reduction of mucosa and haemorrhoidal prolapse with a circular suturing device: A new procedure. Proceedings of the 6th World Congress of Endoscopic Surgery, Rome, 3-6 June 1998; pp. 777–84
Caviglia A, Del Grammastro A, Crocetta R, Straniero A, Giorgiano F. Feasibility of stapled haemorrhoidopexy in Day Surgery. European Review for Medical and Pharmacological Sciences 2009; 13:295–8
Burch J, Epstein D, Gari AB, et al. Stapled haemorrhoidopexy for the treatment of haemorrhoids: a systematic review. Colorectal Dis 2009; 11:233–43; discussion 243
Giordano P, Gravante G, Sorge R, et al. Long-term outcomes of stapled hemorrhoidopexy vs conventional hemorrhoidectomy: a meta-analysis of randomized controlled trials. Arch Surg 2009; 144:266–72
Ravo B, Amato A, Bianco V, et al. Complications after stapled hemorrhoidectomy: can they be prevented? Tech Coloproctol 2002; 6:83–8
Mehigan BJ, Monson JR, Hartley JE. Stapling procedure for haemorrhoids versus Milligan-MorGAn haemorrhoidectomy: randomised controlled trial. Lancet 2000; 355:782–5
Arun Kumar Paul. Obstetric Anesthesia and Analgesia. Clinical Anesthesia 2006; 1st ed: pp. 222–60
Aitkenhead AR, Smith G. Obstetric Anesthesia and Analgesia. In: Textbook of Anesthesia 1996; 3rd ed: pp. 533–50
Edward Morgan G, Maghed S. Mikhail, Michael J. Murray. Pain Management-Pudendal Nerve Block. Lange Clinical Anesthesiology 2002; 3rd ed: pp. 309–43
Haveran LA, Sturrock PR, Sun MY, et al. Simple harmonic scalpel hemorrhoidectomy utilizing local anesthesia combined with intravenous sedation: a safe and rapid alternative to conventional hemorrhoidectomy. Int J Colorectal Dis 2007; 22:801–6
Potchavit Aphinives. Perianal block for ambulatory hemorrhoidectomy, an easy technique for general surgeon. J Med Assoc Thai 2009; 92:195–7
Hahn MB, McQuillan PM, Sheplock GJ. Regional anaesthesia, an atlas of anatomy and techniques 2000; 38:270
Cameron JL. Current Surgical Therapy; 4th edition: pp. 267
Atkinson RS, Rushman GB, Lee JA. Obstetric anesthesia. In: A synopsis of anesthesia. 10th ed: pp. 531
Ong CH, Chee Boon Foo E, Keng V. Ambulatory circular stapled haemorrhoidectomy under local anaesthesia versus circular stapled haemorrhoidectomy under regional anaesthesia. ANZ J Surg 2005; 75:184–6
Torre FL, Nicolai AP. Clinical use of micronized purified flavonoid fraction for treatment of symptoms after hemorrhoidectomy: results of a randomized, controlled, clinical trial. Diseases of the Colon and Rectum 2004; 7:704–10
Kushwaha R, Huchings W, Davies C, et al. Randomized clinical trial comparing day-care open haemorrhoidectomy under local versus general anaesthesia. Br J Surg 2008; 95:555–63
Gerjy R, Lindhoff-Larson A, Sjodahi R, et al. Randomized clinical trial of stapled haemorrhoidopexy performed under local block versus general anaesthesia. Br J Surg 2008; 95:1344–51
Author information
Authors and Affiliations
Corresponding authors
Rights and permissions
About this article
Cite this article
Kumar, N., Kapur, N. Comparative study of stapled haemorrhoidectomy under local anaesthesia versus spinal anaesthesia. Hellenic J Surg 88, 85–92 (2016). https://doi.org/10.1007/s13126-016-0292-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13126-016-0292-z