Abstract
Objectives
In the burning mouth syndrome (BMS), patients experience a burning sensation in the oral cavity with no associated injury or clinical manifestation. The etiology of this condition is still poorly understood, and therefore, treatment is challenging. The aim of this study is to perform a systematic review of treatment possibilities described in the literature for BMS.
Materials and methods
PubMed, Embase, and SciELO databases were searched for randomized clinical trials published between 1996 and 2016.
Results
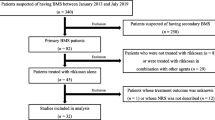
Following application of inclusion and exclusion criteria, 29 papers were analyzed and divided into five subcategories according to the type of treatment described: antidepressants, alpha-lipoic acid, phytotherapeutic agents, analgesic and anti-inflammatory agents, and non-pharmacological therapies. In each category, the results found were compared with regard to the methodology employed, sample size, assessment method, presence or absence of adverse effects, and treatment outcomes.
Conclusions
The analysis revealed that the use of antidepressants and alpha-lipoic acid has been showing promising results; however, more studies are necessary before we can have a first-line treatment strategy for patients with BMS.
Clinical relevance
To review systematically the literature about Burning Mouth Syndrome treatment may aid the clinicians to choose the treatment modality to improve patients symptoms based on the best evidence.


Similar content being viewed by others
Change history
30 July 2019
The original version of this article contained two mistakes. First, in the subchapter ���Alpha-lipoic acid (ALA)��� page 1895, reference 4 is cited three times, however reference 42 is the correct one.
30 July 2019
The original version of this article contained two mistakes. First, in the subchapter ���Alpha-lipoic acid (ALA)��� page 1895, reference 4 is cited three times, however reference 42 is the correct one.
References
Jimson S, Rajesh E, Krupaa RJ, Kasthuri M (2015) Burning mouth syndrome. J Pharm Bioallied Sci 7:S194–S196. https://doi.org/10.4103/0975-7406.155899
Oliveira GMR, Pereira HSC, Silva-Júnior GO et al (2013) Síndrome da Ardência Bucal: aspectos clínicos e tratamento. Revista do Hospital Universitário Pedro Ernesto, UERJ 12:21–29
Scala A, Checchi L, Montevecchi M, Marini I, Giamberardino MA (2003) Update on burning mouth syndrome: overview and patient management. Crit Rev Oral Biol Med Off Publ Am Assoc Oral Biol 14:275–291
Marino R, Picci RL, Ferro G, Carezana C, Gandolfo S, Pentenero M (2015) Peculiar alexithymic traits in burning mouth syndrome: case–control study. Clin Oral Investig 19:1799–1805. https://doi.org/10.1007/s00784-015-1416-5
Barker K, Savage N (2005) Burning mouth syndrome: an update on recent findings. Aust Dent J 50:220–223. https://doi.org/10.1111/j.1834-7819.2005.tb00363.x
López-Jornet P, Camacho-Alonso F, Andujar-Mateos P et al (2010) Burning mouth syndrome: an update. Med Oral Patol Oral Cir Bucal 15:e562–e568. https://doi.org/10.4317/medoral.15.e562
Aravindhan R, Vidyalakshmi S, Kumar MS, Satheesh C, Balasubramanium AM, Prasad VS (2014) Burning mouth syndrome: a review on its diagnostic and therapeutic approach. J Pharm Bioallied Sci 6:S21–S25. https://doi.org/10.4103/0975-7406.137255
Moher D, Liberati A, Tetzlaff J, Altman DG (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. J Clin Epidemiol 62:1006–1012. https://doi.org/10.1016/j.jclinepi.2009.06.005
Heckmann SM, Kirchner E, Grushka M, Wichmann MG, Hummel T (2012) A double-blind study on clonazepam in patients with burning mouth syndrome. Laryngoscope 122:813–816. https://doi.org/10.1002/lary.22490
Jurisic Kvesic A, Zavoreo I, Basic Kes V, Vucicevic Boras V, Ciliga D, Gabric D, Vrdoljak DV (2015) The effectiveness of acupuncture versus clonazepam in patients with burning mouth syndrome. Acupunct Med 33:289–292. https://doi.org/10.1136/acupmed-2015-010759
Gremeau-Richard C, Woda A, Navez ML, Attal N, Bouhassira D, Gagnieu MC, Laluque JF, Picard P, Pionchon P, Tubert S (2004) Topical clonazepam in stomatodynia: a randomised placebo-controlled study. Pain 108:51–57. https://doi.org/10.1016/j.pain.2003.12.002
Rodríguez de Rivera Campillo E, López-López J, Chimenos-Küstner E (2010) Response to topical clonazepam in patients with burning mouth syndrome: a clinical study. Bull Group Int Rech Sci Stomatol Odontol 49:19–29
Tammiala-Salonen T, Forssell H (1999) Trazodone in burning mouth pain: a placebo-controlled, double-blind study. J Orofac Pain 13:83–88. https://doi.org/10.1016/S0022-3913(99)70067-3
Maina G, Vitalucci A, Gandolfo S, Bogetto F (2002) Comparative efficacy of SSRIs and amisulpride in burning mouth syndrome: a single-blind study. J Clin Psychiatry 63:38–43. https://doi.org/10.4088/JCP.v63n0108
Femiano F, Scully C (2002) Burning mouth syndrome (BMS): double blind controlled study of alpha-lipoic acid (thioctic acid) therapy. J Oral Pathol Med Off Publ Int Assoc Oral Pathol Am Acad Oral Pathol 31:267–269. https://doi.org/10.1034/j.1600-0714.2002.310503.x
Palacios-Sánchez B, Moreno-López L-A, Cerero-Lapiedra R et al (2015) Alpha lipoic acid efficacy in burning mouth syndrome. A controlled clinical trial. Med Oral Patol Oral Cir Bucal 20:e435–e440. https://doi.org/10.4317/medoral.20410
López-D’alessandro E, Escovich L (2011) Combination of alpha lipoic acid and gabapentin, its efficacy in the treatment of burning mouth syndrome: a randomized, double-blind, placebo controlled trial. Med Oral Patol Oral Cir Bucal 16:e635–e640. https://doi.org/10.4317/medoral.16942
Cavalcanti DR, da Silveira FRX (2009) Alpha lipoic acid in burning mouth syndrome—a randomized double-blind placebo-controlled trial. J Oral Pathol Med Off Publ Int Assoc Oral Pathol Am Acad Oral Pathol 38:254–261. https://doi.org/10.1111/j.1600-0714.2008.00735.x
López-Jornet P, Camacho-Alonso F, Leon-Espinosa S (2009) Efficacy of alpha lipoic acid in burning mouth syndrome: a randomized, placebo-treatment study. J Oral Rehabil 36:52–57. https://doi.org/10.1111/j.1365-2842.2008.01914.x
Carbone M, Pentenero M, Carrozzo M, Ippolito A, Gandolfo S (2009) Lack of efficacy of alpha-lipoic acid in burning mouth syndrome: a double-blind, randomized, placebo-controlled study. Eur J Pain Lond Engl 13:492–496. https://doi.org/10.1016/j.ejpain.2008.06.004
Valenzuela S, Pons-Fuster A, López-Jornet P (2016) Effect of a 2% topical chamomile application for treating burning mouth syndrome: a controlled clinical trial. J Oral Pathol Med Off Publ Int Assoc Oral Pathol Am Acad Oral Pathol 45:528–533. https://doi.org/10.1111/jop.12412
Cano-Carrillo P, Pons-Fuster A, López-Jornet P (2014) Efficacy of lycopene-enriched virgin olive oil for treating burning mouth syndrome: a double-blind randomised. J Oral Rehabil 41:296–305. https://doi.org/10.1111/joor.12147
da SLA, de SJTT, Teixeira MJ, de SSRDT (2014) The role of xerostomia in burning mouth syndrome: a case-control study. Arq Neuropsiquiatr 72:91–98. https://doi.org/10.1590/0004-282X20130218
López-Jornet P, Camacho-Alonso F, Molino-Pagan D (2013) Prospective, randomized, double-blind, clinical evaluation of Aloe vera Barbadensis, applied in combination with a tongue protector to treat burning mouth syndrome. J Oral Pathol Med Off Publ Int Assoc Oral Pathol Am Acad Oral Pathol 42:295–301. https://doi.org/10.1111/jop.12002
Spanemberg JC, López López J, de Figueiredo MAZ et al (2015) Efficacy of low-level laser therapy for the treatment of burning mouth syndrome: a randomized, controlled trial. J Biomed Opt 20:098001. https://doi.org/10.1117/1.JBO.20.9.098001
Silvestre F-J, Silvestre-Rangil J, Tamarit-Santafé C, Bautista D (2012) Application of a capsaicin rinse in the treatment of burning mouth syndrome. Med Oral Patol Oral Cir Bucal 17:e1–e4. https://doi.org/10.4317/medoral.17219
Sardella A, Lodi G, Demarosi F, Tarozzi M, Canegallo L, Carrassi A (2008) Hypericum perforatum extract in burning mouth syndrome: a randomized placebo-controlled study. J Oral Pathol Med Off Publ Int Assoc Oral Pathol Am Acad Oral Pathol 37:395–401. https://doi.org/10.1111/j.1600-0714.2008.00663.x
Spanemberg JC, Cherubini K, de Figueiredo MAZ, Gomes APN, Campos MM, Salum FG (2012) Effect of an herbal compound for treatment of burning mouth syndrome: randomized, controlled, double-blind clinical trial. Oral Surg Oral Med Oral Pathol Oral Radiol 113:373–377. https://doi.org/10.1016/j.oooo.2011.09.005
Treldal C, Jacobsen CB, Mogensen S, Rasmussen M, Jacobsen J, Petersen J, Lynge Pedersen AM, Andersen O (2016) Effect of a local anesthetic lozenge in relief of symptoms in burning mouth syndrome. Oral Dis 22:123–131. https://doi.org/10.1111/odi.12386
Grémeau-Richard C, Dubray C, Aublet-Cuvelier B, Ughetto S, Woda A (2010) Effect of lingual nerve block on burning mouth syndrome (stomatodynia): a randomized crossover trial. Pain 149:27–32. https://doi.org/10.1016/j.pain.2009.11.016
Toida M, Kato K, Makita H, Long NK, Takeda T, Hatakeyama D, Yamashita T, Shibata T (2009) Palliative effect of lafutidine on oral burning sensation. J Oral Pathol Med Off Publ Int Assoc Oral Pathol Am Acad Oral Pathol 38:262–268. https://doi.org/10.1111/j.1600-0714.2008.00736.x
Sardella A, Uglietti D, Demarosi F, Lodi G, Bez C, Carrassi A (1999) Benzydamine hydrochloride oral rinses in management of burning mouth syndrome. A clinical trial. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 88:683–686. https://doi.org/10.1016/S1079-2104(99)70010-7
Sugaya NN, da Silva ÉFP, Kato IT et al (2016) Low intensity laser therapy in patients with burning mouth syndrome: a randomized, placebo-controlled study. Braz Oral Res 30:e108. https://doi.org/10.1590/1807-3107BOR-2016.vol30.0108
Umezaki Y, Badran BW, DeVries WH et al (2016) The efficacy of daily prefrontal repetitive transcranial magnetic stimulation (rTMS) for burning mouth syndrome (BMS): a randomized controlled single-blind study. Brain Stimul 9:234–242. https://doi.org/10.1016/j.brs.2015.10.005
López-Jornet P, Camacho-Alonso F, Andujar-Mateos P (2011) A prospective, randomized study on the efficacy of tongue protector in patients with burning mouth syndrome. Oral Dis 17:277–282. https://doi.org/10.1111/j.1601-0825.2010.01737.x
Miziara ID, Filho BCA, Oliveira R, Rodrigues dos Santos RM (2009) Group psychotherapy: an additional approach to burning mouth syndrome. J Psychosom Res 67:443–448. https://doi.org/10.1016/j.jpsychores.2009.01.013
Netto FOG, Diniz IMA, Grossmann SMC, de Abreu MHNG, do Carmo MAV, Aguiar MCF (2011) Risk factors in burning mouth syndrome: a case–control study based on patient records. Clin Oral Investig 15:571–575. https://doi.org/10.1007/s00784-010-0419-5
Sun A, Wu K-M, Wang Y-P, Lin HP, Chen HM, Chiang CP (2013) Burning mouth syndrome: a review and update. J Oral Pathol Med 42:649–655. https://doi.org/10.1111/jop.12101
Singh U, Jialal I (2008) Alpha-lipoic acid supplementation and diabetes. Nutr Rev 66:646–657. https://doi.org/10.1111/j.1753-4887.2008.00118.x
Tirosh O, Sen CK, Roy S, Kobayashi MS, Packer L (1999) Neuroprotective effects of alpha-lipoic acid and its positively charged amide analogue. Free Radic Biol Med 26:1418–1426. https://doi.org/10.1016/S0891-5849(99)00014-3
Arivazhagan P, Panneerselvam C (2000) Effect of DL-alpha-lipoic acid on neural antioxidants in aged rats. Pharmacol Res 42:219–222. https://doi.org/10.1006/phrs.2000.0679
Marino R, Torretta S, Capaccio P, Pignataro L, Spadari F (2010) Different therapeutic strategies for burning mouth syndrome: preliminary data. J Oral Pathol Med Off Publ Int Assoc Oral Pathol Am Acad Oral Pathol 39:611–616. https://doi.org/10.1111/j.1600-0714.2010.00922.x
Pozza DH, Fregapani PW, Weber JBB et al (2008) Analgesic action of laser therapy (LLLT) in an animal model. Med Oral Patol Oral Cir Bucal 13:E648–E652
Romeo U, Del Vecchio A, Capocci M et al (2010) The low level laser therapy in the management of neurological burning mouth syndrome. A pilot study. Ann Stomatol (Roma) 1:14–18
Kim M-J, Kim J, Chang J-Y, Kim YY, Kho HS (2017) Polymorphisms of interleukin-1β and MUC7 genes in burning mouth syndrome. Clin Oral Investig 21:949–955. https://doi.org/10.1007/s00784-016-1866-4
Funding
The work was supported by the Coordenação de Aperfeiçoamento de Pessoal de Nível Superior (Brazil).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed consent
For this type of study, formal consent is not required.
Rights and permissions
About this article
Cite this article
de Souza, I.F., Mármora, B.C., Rados, P.V. et al. Treatment modalities for burning mouth syndrome: a systematic review. Clin Oral Invest 22, 1893–1905 (2018). https://doi.org/10.1007/s00784-018-2454-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-018-2454-6