Abstract
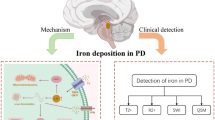
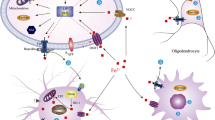
Focal iron accumulation associated with brain iron dyshomeostasis is a pathological hallmark of various neurodegenerative diseases (NDD). The application of iron-sensitive sequences in magnetic resonance imaging has provided a useful tool to identify the underlying NDD pathology. In the three major NDD, degeneration occurs in central nervous system (CNS) regions associated with memory (Alzheimer’s disease, AD), automaticity (Parkinson’s disease, PD) and motor function (amyotrophic lateral sclerosis, ALS), all of which require a high oxygen demand for harnessing neuronal energy. In PD, a progressive degeneration of the substantia nigra pars compacta (SNc) is associated with the appearance of siderotic foci, largely caused by increased labile iron levels resulting from an imbalance between cell iron import, storage and export. At a molecular level, α-synuclein regulates dopamine and iron transport with PD-associated mutations in this protein causing functional disruption to these processes. Equally, in ALS, an early iron accumulation is present in neurons of the cortico-spinal motor pathway before neuropathology and secondary iron accumulation in microglia. High serum ferritin is an indicator of poor prognosis in ALS and the application of iron-sensitive sequences in magnetic resonance imaging has become a useful tool in identifying pathology. The molecular pathways that cascade down from such dyshomeostasis still remain to be fully elucidated but strong inroads have been made in recent years. Far from being a simple cause or consequence, it has recently been discovered that these alterations can trigger susceptibility to an iron-dependent cell-death pathway with unique lipoperoxidation signatures called ferroptosis. In turn, this has now provided insight into some key modulators of this cell-death pathway that could be therapeutic targets for the NDD. Interestingly, iron accumulation and ferroptosis are highly sensitive to iron chelation. However, whilst chelators that strongly scavenge intracellular iron protect against oxidative neuronal damage in mammalian models and are proven to be effective in treating systemic siderosis, these compounds are not clinically suitable due to the high risk of developing iatrogenic iron depletion and ensuing anaemia. Instead, a moderate iron chelation modality that conserves systemic iron offers a novel therapeutic strategy for neuroprotection. As demonstrated with the prototype chelator deferiprone, iron can be scavenged from labile iron complexes in the brain and transferred (conservatively) either to higher affinity acceptors in cells or extracellular transferrin. Promising preclinical and clinical proof of concept trials has led to several current large randomized clinical trials that aim to demonstrate the efficacy and safety of conservative iron chelation for NDD, notably in a long-term treatment regimen.


Similar content being viewed by others
References
Acosta-Cabronero J, Cardenas-Blanco A, Betts MJ et al (2017) The whole-brain pattern of magnetic susceptibility perturbations in Parkinson’s disease. Brain 140:118–131. https://doi.org/10.1093/brain/aww278
Adachi Y, Sato N, Saito Y et al (2015) Usefulness of SWI for the detection of iron in the motor cortex in amyotrophic lateral sclerosis: usefulness of SWI for the diagnoses of ALS. J Neuroimaging 25:443–451. https://doi.org/10.1111/jon.12127
Aquino D, Contarino V, Albanese A et al (2014) Substantia nigra in Parkinson’s disease: a multimodal MRI comparison between early and advanced stages of the disease. Neurol Sci 35:753–758. https://doi.org/10.1007/s10072-013-1595-2
Ayton S, Lei P, Duce JA et al (2013) Ceruloplasmin dysfunction and therapeutic potential for Parkinson disease: ceruloplasmin in PD. Ann Neurol 73:554–559. https://doi.org/10.1002/ana.23817
Ayton S, Lei P, Hare DJ et al (2015) Parkinson’s disease iron deposition caused by nitric oxide-induced loss of -Amyloid precursor protein. J Neurosci 35:3591–3597. https://doi.org/10.1523/JNEUROSCI.3439-14.2015
Barbariga M, Curnis F, Andolfo A et al (2015) Ceruloplasmin functional changes in Parkinson’s disease-cerebrospinal fluid. Mol Neurodegeneration 10:59. https://doi.org/10.1186/s13024-015-0055-2
Belaidi AA, Bush AI (2016) Iron neurochemistry in Alzheimer’s disease and Parkinson’s disease: targets for therapeutics. J Neurochem 139:179–197. https://doi.org/10.1111/jnc.13425
Berg D, Roggendorf W, Schröder U et al (2002) Echogenicity of the substantia nigra: association with increased iron content and marker for susceptibility to nigrostriatal injury. Arch Neurol 59:999. https://doi.org/10.1001/archneur.59.6.999
Berg D, Hochstrasser H, Schweitzer KJ, Riess O (2006) Disturbance of iron metabolism in Parkinson’s disease ultrasonography as a biomarker. Neurotox res 9:1–13. https://doi.org/10.1007/BF03033302
Bunzeck N, Singh-Curry V, Eckart C et al (2013) Motor phenotype and magnetic resonance measures of basal ganglia iron levels in Parkinson’s disease. Parkinsonism Relat Disord 19:1136–1142. https://doi.org/10.1016/j.parkreldis.2013.08.011
Butler B, Saha K, Rana T et al (2015) Dopamine transporter activity is modulated by α-synuclein. J Biol Chem 290:29542–29554. https://doi.org/10.1074/jbc.M115.691592
Cabantchik ZI, Munnich A, Youdim MB, Devos D (2013) Regional siderosis: a new challenge for iron chelation therapy. Front Pharmacol. https://doi.org/10.3389/fphar.2013.00167
Cai M, Lee K-W, Choi S-M, Yang EJ (2015) TDP-43 modification in the hSOD1 G93A amyotrophic lateral sclerosis mouse model. Neurol Res 37:253–262. https://doi.org/10.1179/1743132814Y.0000000443
Carboni E, Tatenhorst L, Tönges L et al (2017) deferiprone rescues behavioral deficits induced by mild iron exposure in a mouse model of alpha-synuclein aggregation. NeuroMol Med 19:309–321. https://doi.org/10.1007/s12017-017-8447-9
Chen L, Hambright WS, Na R, Ran Q (2015) Ablation of the ferroptosis inhibitor glutathione peroxidase 4 in neurons results in rapid motor neuron degeneration and paralysis. J Biol Chem 290:28097–28106. https://doi.org/10.1074/jbc.M115.680090
Cohen TJ, Hwang AW, Unger T et al (2012) Redox signalling directly regulates TDP-43 via cysteine oxidation and disulphide cross-linking: oxidative stress regulates TDP-43. EMBO J 31:1241–1252. https://doi.org/10.1038/emboj.2011.471
Conti A, Iannaccone S, Sferrazza B et al (2008) Differential expression of ceruloplasmin isoforms in the cerebrospinal fluid of amyotrophic lateral sclerosis patients. Prot Clin Appl 2:1628–1637. https://doi.org/10.1002/prca.200780081
Devos D, Moreau C, Devedjian JC et al (2014) Targeting chelatable iron as a therapeutic modality in Parkinson’s disease. Antioxid Redox Signal 21:195–210. https://doi.org/10.1089/ars.2013.5593
Dixon SJ, Lemberg KM, Lamprecht MR et al (2012) Ferroptosis: an iron-dependent form of nonapoptotic cell death. Cell 149:1060–1072. https://doi.org/10.1016/j.cell.2012.03.042
Doll S, Conrad M (2017) Iron and ferroptosis: a still ill-defined liaison: iron and ferroptosis. IUBMB Life 69:423–434. https://doi.org/10.1002/iub.1616
DoVan B, Gouel F, Jonneaux A et al (2016) Ferroptosis, a newly characterized form of cell death in Parkinson’s disease that is regulated by PKC. Neurobiol Dis 94:169–178. https://doi.org/10.1016/j.nbd.2016.05.011
Duce JA, Tsatsanis A, Cater MA et al (2010) Iron-export ferroxidase activity of β-amyloid precursor protein is inhibited by zinc in Alzheimer’s disease. Cell 142:857–867. https://doi.org/10.1016/j.cell.2010.08.014
Duce JA, Wong BX, Durham H et al (2017) Post translational changes to α-synuclein control iron and dopamine trafficking; a concept for neuron vulnerability in Parkinson’s disease. Mol Neurodegener 12:45. https://doi.org/10.1186/s13024-017-0186-8
Elliott JL (2001) Cytokine upregulation in a murine model of familial amyotrophic lateral sclerosis. Mol Brain Res 95:172–178. https://doi.org/10.1016/S0169-328X(01)00242-X
Evans TM, Bhattacharya A, Shi Y et al (2016) Moderate modulation of disease in the G93A model of ALS by the compound 2-(2-hydroxyphenyl)-benzoxazole (HBX). Neurosci Lett 624:1–7. https://doi.org/10.1016/j.neulet.2016.04.035
Faucheux BA, Nillesse N, Damier P et al (1995) Expression of lactoferrin receptors is increased in the mesencephalon of patients with Parkinson disease. Proc Natl Acad Sci 92:9603–9607. https://doi.org/10.1073/pnas.92.21.9603
Finkelstein DI, Hare DJ, Billings JL et al (2016) Clioquinol improves cognitive, motor function, and microanatomy of the alpha-synuclein hA53T transgenic mice. ACS Chem Neurosci 7:119–129. https://doi.org/10.1021/acschemneuro.5b00253
Finkelstein DI, Billings JL, Adlard PA et al (2017) The novel compound PBT434 prevents iron mediated neurodegeneration and alpha-synuclein toxicity in multiple models of Parkinson’s disease. Acta Neuropathol Commun 5:53. https://doi.org/10.1186/s40478-017-0456-2
Frakes AE, Ferraiuolo L, Haidet-Phillips AM et al (2014) Microglia induce motor neuron death via the classical nf-κb pathway in amyotrophic lateral sclerosis. Neuron 81:1009–1023. https://doi.org/10.1016/j.neuron.2014.01.013
Friedmann Angeli JP, Schneider M, Proneth B et al (2014) Inactivation of the ferroptosis regulator Gpx4 triggers acute renal failure in mice. Nat Cell Biol 16:1180–1191. https://doi.org/10.1038/ncb3064
Gajowiak A, Styś A, Starzyński RR et al (2016) Mice overexpressing both non-mutated human SOD1 and mutated SOD1G93A genes: a competent experimental model for studying iron metabolism in amyotrophic lateral sclerosis. Front Mol Neurosci. https://doi.org/10.3389/fnmol.2015.00082
Gal S, Zheng H, Fridkin M, Youdim MBH (2010) Restoration of nigrostriatal dopamine neurons in post-mptp treatment by the novel multifunctional brain-permeable iron chelator-monoamine oxidase inhibitor drug, M30. Neurotox Res 17:15–27. https://doi.org/10.1007/s12640-009-9070-9
Ghezzi P, Mennini T (2001) Tumor necrosis factor and motoneuronal degeneration: an open problem. Neuro Immuno Modul 9:178–182. https://doi.org/10.1159/000049024
Golko-Perez S, Mandel S, Amit T et al (2016) Additive neuroprotective effects of the multifunctional iron chelator M30 with enriched diet in a mouse model of amyotrophic lateral sclerosis. Neurotox Res 29:208–217. https://doi.org/10.1007/s12640-015-9574-4
Golko-Perez S, Amit T, Bar-Am O et al (2017) A novel iron chelator-radical scavenger ameliorates motor dysfunction and improves life span and mitochondrial biogenesis in SOD1G93A ALS mice. Neurotox Res 31:230–244. https://doi.org/10.1007/s12640-016-9677-6
Guiney SJ, Adlard PA, Bush AI et al (2017) Ferroptosis and cell death mechanisms in Parkinson’s disease. Neurochem Int 104:34–48. https://doi.org/10.1016/j.neuint.2017.01.004
Guzman JN, Sanchez-Padilla J, Wokosin D et al (2010) Oxidant stress evoked by pacemaking in dopaminergic neurons is attenuated by DJ-1. Nature 468:696–700. https://doi.org/10.1038/nature09536
Halon M, Sielicka-Dudzin A, Wozniak M et al (2010) Up-regulation of ferritin ubiquitination in skeletal muscle of transgenic rats bearing the G93A hmSOD1 gene mutation. Neuromuscul Disord 20:29–33. https://doi.org/10.1016/j.nmd.2009.08.014
Halon M, Kaczor JJ, Ziolkowski W et al (2014) Changes in skeletal muscle iron metabolism outpace amyotrophic lateral sclerosis onset in transgenic rats bearing the G93A hmSOD1 gene mutation. Free Radic Res 48:1363–1370. https://doi.org/10.3109/10715762.2014.955484
Hare DJ, Double KL (2016) Iron and dopamine: a toxic couple. Brain 139:1026–1035. https://doi.org/10.1093/brain/aww022
Hensley K (2003) Message and protein-level elevation of tumor necrosis factor α (TNFα) and TNFα-modulating cytokines in spinal cords of the G93A-SOD1 mouse model for amyotrophic lateral sclerosis. Neurobiol Dis 14:74–80. https://doi.org/10.1016/S0969-9961(03)00087-1
Hensley K, Floyd RA, Gordon B et al (2002) Temporal patterns of cytokine and apoptosis-related gene expression in spinal cords of the G93A-SOD1 mouse model of amyotrophic lateral sclerosis: gene expression changes in ALS mice. J Neurochem 82:365–374. https://doi.org/10.1046/j.1471-4159.2002.00968.x
Higashi S, Tsuchiya Y, Araki T et al (2010) TDP-43 physically interacts with amyotrophic lateral sclerosis-linked mutant CuZn superoxide dismutase. Neurochem Int 57:906–913. https://doi.org/10.1016/j.neuint.2010.09.010
Hilton JB, Kysenius K, White AR, Crouch PJ (2018) The accumulation of enzymatically inactive cuproenzymes is a CNS-specific phenomenon of the SOD1G37R mouse model of ALS and can be restored by overexpressing the human copper transporter hCTR1. Exp Neurol 307:118–128. https://doi.org/10.1016/j.expneurol.2018.06.006
Hirsch EC (2006) Altered regulation of iron transport and storage in Parkinson’s disease. In: Parvez H, Riederer P (eds) Oxidative stress and neuroprotection. Springer, Vienna, pp 201–204
Hochstrasser H, Tomiuk J, Walter U et al (2005) Functional relevance of ceruloplasmin mutations in Parkinson’s disease. FASEB J 19:1851–1853. https://doi.org/10.1096/fj.04-3486fje
Hopes L, Grolez G, Moreau C et al (2016) Magnetic resonance imaging features of the nigrostriatal system: biomarkers of Parkinson’s disease stages? plos One 11:e0147947. https://doi.org/10.1371/journal.pone.0147947
Howitt J, Gysbers AM, Ayton S et al (2014) Increased Ndfip1 in the substantia nigra of Parkinsonian brains is associated with elevated iron levels. PLoS One 9:e87119. https://doi.org/10.1371/journal.pone.0087119
Huddleston DE, Langley J, Sedlacik J et al (2017) In vivo detection of lateral-ventral tier nigral degeneration in Parkinson’s disease: MRI of Lateral-Ventral SNc in PD. Hum Brain Mapp 38:2627–2634. https://doi.org/10.1002/hbm.23547
Ignjatović A, Stević Z, Lavrnić D et al (2012) Inappropriately chelated iron in the cerebrospinal fluid of amyotrophic lateral sclerosis patients. Amyotroph Lateral Scler 13:357–362. https://doi.org/10.3109/17482968.2012.665929
Ignjatović A, Stević Z, Lavrnić S et al (2013) Brain iron MRI: a biomarker for amyotrophic lateral sclerosis brain iron MRI: a biomarker for ALS. J Magn Reson Imaging 38:1472–1479. https://doi.org/10.1002/jmri.24121
Ishikawa K, Nagura H, Yokota T, Yamanouchi H (1993) Signal loss in the motor cortex on magnetic resonance images in amyotrophic lateral sclerosis. Ann Neurol 33:218–222. https://doi.org/10.1002/ana.410330214
Jeon GS, Shim Y-M, Lee D-Y et al (2019) Pathological modification of TDP-43 in amyotrophic lateral sclerosis with SOD1 mutations. Mol Neurobiol 56:2007–2021. https://doi.org/10.1007/s12035-018-1218-2
Jeong SY (2006) Age-related changes in iron homeostasis and cell death in the cerebellum of ceruloplasmin-deficient mice. J Neurosci 26:9810–9819. https://doi.org/10.1523/JNEUROSCI.2922-06.2006
Jeong SY, Rathore KI, Schulz K et al (2009) Dysregulation of iron homeostasis in the CNS contributes to disease progression in a mouse model of amyotrophic lateral sclerosis. J Neurosci 29:610–619. https://doi.org/10.1523/JNEUROSCI.5443-08.2009
Kaur D, Yantiri F, Rajagopalan S et al (2003) Genetic or pharmacological iron chelation prevents MPTP-induced neurotoxicity in vivo. Neuron 37:899–909. https://doi.org/10.1016/S0896-6273(03)00126-0
Khadzhiev SN, Kadiev KM, Yampolskaya GP, Kadieva MKh (2013) Trends in the synthesis of metal oxide nanoparticles through reverse microemulsions in hydrocarbon media. Adv Coll Interface Sci 197–198:132–145. https://doi.org/10.1016/j.cis.2013.05.003
Kupershmidt L, Weinreb O, Amit T et al (2009) Neuroprotective and neuritogenic activities of novel multimodal iron-chelating drugs in motor-neuron-like NSC-34 cells and transgenic mouse model of amyotrophic lateral sclerosis. FASEB J 23:3766–3779. https://doi.org/10.1096/fj.09-130047
Kwan JY, Jeong SY, Van Gelderen P et al (2012) Iron accumulation in deep cortical layers accounts for MRI signal abnormalities in ALS: CORRELATING 7 Tesla MRI and pathology. PLoS One 7:e35241. https://doi.org/10.1371/journal.pone.0035241
Langley J, Huddleston DE, Sedlacik J et al (2017) Parkinson’s disease-related increase of T2*-weighted hypointensity in substantia nigra pars compacta: SNpc Hypointensity. Mov Disord 32:441–449. https://doi.org/10.1002/mds.26883
Lee DW, Rajagopalan S, Siddiq A et al (2009) Inhibition of prolyl hydroxylase protects against 1-Methyl-4-phenyl-1,2,3,6-tetrahydropyridine-induced Neurotoxicity: model for the potential involvement of the hypoxia-inducible factor pathway in Parkinson disease. J Biol Chem 284:29065–29076. https://doi.org/10.1074/jbc.M109.000638
Lei P, Ayton S, Finkelstein DI et al (2012) Tau deficiency induces parkinsonism with dementia by impairing APP-mediated iron export. Nat Med 18:291–295. https://doi.org/10.1038/nm.2613
Lei P, Ayton S, Appukuttan AT et al (2015) Clioquinol rescues Parkinsonism and dementia phenotypes of the tau knockout mouse. Neurobiol Dis 81:168–175. https://doi.org/10.1016/j.nbd.2015.03.015
Leveugle B, Spik G, Perl DP et al (1994) The iron-binding protein lactotransferrin is present in pathologic lesions in a variety of neurodegenerative disorders: a comparative immunohistochemical analysis. Brain Res 650:20–31. https://doi.org/10.1016/0006-8993(94)90202-X
Lu AM, Rajanala S, Mikkilineni SV et al (2016) The 5′-Untranslated Region of the C9orf72 mRNA Exhibits a Phylogenetic Alignment to the Cis-Aconitase Iron-Responsive Element; novel therapies for amytrophic lateral sclerosis. Novel 07:15–26. https://doi.org/10.4236/nm.2016.71003
Mahlknecht P, Krismer F, Poewe W, Seppi K (2017) Meta-analysis of dorsolateral nigral hyperintensity on magnetic resonance imaging as a marker for Parkinson’s disease: DNH on MRI as a Marker for PD. Mov Disord 32:619–623. https://doi.org/10.1002/mds.26932
Martin-Bastida A, Ward RJ, Newbould R et al (2017) Brain iron chelation by deferiprone in a phase 2 randomised double-blinded placebo controlled clinical trial in Parkinson’s disease. Sci Rep 7:1398. https://doi.org/10.1038/s41598-017-01402-2
Matak P, Matak A, Moustafa S et al (2016) Disrupted iron homeostasis causes dopaminergic neurodegeneration in mice. Proc Natl Acad Sci USA 113:3428–3435. https://doi.org/10.1073/pnas.1519473113
McCarthy RC, Park Y, Kosman DJ (2014) sAPP modulates iron efflux from brain microvascular endothelial cells by stabilizing the ferrous iron exporter ferroportin. EMBO Rep 15:809–815. https://doi.org/10.15252/embr.201338064
Meiser J, Weindl D, Hiller K (2013) Complexity of dopamine metabolism. Cell Commun Signal 11:34. https://doi.org/10.1186/1478-811X-11-34
Moreau C, Danel V, Devedjian JC, et al (2018) Could Conservative Iron Chelation Lead to Neuroprotection in Amyotrophic Lateral Sclerosis?© Caroline Moreau et al. 2018; Published by Mary Ann Liebert, Inc. This Open Access article distributed under the terms of the Creative Commons License (http://creativecommons.org/licenses/by/4.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Antioxid Redox Signal 29:742–748. https://doi.org/10.1089/ars.2017.7493
Nadjar Y, Gordon P, Corcia P et al (2012) Elevated serum ferritin is associated with reduced survival in amyotrophic lateral sclerosis. PLoS One 7:e45034. https://doi.org/10.1371/journal.pone.0045034
Nam Y, Gho S-M, Kim D-H et al (2017) Imaging of nigrosome 1 in substantia nigra at 3T using multiecho susceptibility map-weighted imaging (SMWI): nigrosome 1 Imaging Using SMWI. J Magn Reson Imaging 46:528–536. https://doi.org/10.1002/jmri.25553
Nuñez M, Chana-Cuevas P (2018) New perspectives in iron chelation therapy for the treatment of neurodegenerative diseases. Pharmaceuticals 11:109. https://doi.org/10.3390/ph11040109
Oba H, Araki T, Ohtomo K et al (1993) Amyotrophic lateral sclerosis: T2 shortening in motor cortex at MR imaging. Radiology 189:843–846. https://doi.org/10.1148/radiology.189.3.8234713
Perez C, Tong Y, Guo M (2008) Iron chelators as potential therapeutic agents for parkinsons disease. CBC 4:150–158. https://doi.org/10.2174/157340708786305952
Rajagopalan S, Rane A, Chinta SJ, Andersen JK (2016) Regulation of ATP13A2 via PHD2-HIF1 signaling is critical for cellular iron homeostasis: implications for Parkinson’s disease. J Neurosci 36:1086–1095. https://doi.org/10.1523/JNEUROSCI.3117-15.2016
Ramos P, Santos A, Pinto NR et al (2014) Iron levels in the human brain: a post-mortem study of anatomical region differences and age-related changes. J Trace Elem Med Biol 28:13–17. https://doi.org/10.1016/j.jtemb.2013.08.001
Rhodes SL, Buchanan DD, Ahmed I et al (2014) Pooled analysis of iron-related genes in Parkinson’s disease: association with transferrin. Neurobiol Dis 62:172–178. https://doi.org/10.1016/j.nbd.2013.09.019
Rossi ME, Ruottinen H, Saunamäki T et al (2014) Imaging brain iron and diffusion patterns. Acad Radiol 21:64–71. https://doi.org/10.1016/j.acra.2013.09.018
Sian G, Hare D, Double K (2019) Meta-analysis of copper and iron in Parkinson’s disease brain and biofluids. Mov Disord. https://doi.org/10.1002/mds.27947
Stevens CH, Guthrie NJ, van Roijen M et al (2019) Increased tau phosphorylation in motor neurons from clinically pure sporadic amyotrophic lateral sclerosis patients. J Neuropathol Exp Neurol 78:605–614. https://doi.org/10.1093/jnen/nlz041
Torii S, Shintoku R, Kubota C et al (2016) An essential role for functional lysosomes in ferroptosis of cancer cells. Biochem J 473:769–777. https://doi.org/10.1042/BJ20150658
Trostchansky A, Mastrogiovanni M, Miquel E et al (2018) Profile of arachidonic acid-derived inflammatory markers and its modulation by nitro-oleic acid in an inherited model of amyotrophic lateral sclerosis. Front Mol Neurosci 11:131. https://doi.org/10.3389/fnmol.2018.00131
Ulla M, Bonny JM, Ouchchane L et al (2013) Is R2* a new MRI biomarker for the progression of Parkinson’s disease? A Longitudinal Follow-Up. PLoS ONE 8:e57904. https://doi.org/10.1371/journal.pone.0057904
Vázquez-Costa JF, Mazón M, Carreres-Polo J et al (2018) Brain signal intensity changes as biomarkers in amyotrophic lateral sclerosis. Acta Neurol Scand 137:262–271. https://doi.org/10.1111/ane.12863
Veyrat-Durebex C, Corcia P, Mucha A et al (2014) Iron metabolism disturbance in a french cohort of ALS patients. Biomed Res Int 2014:1–6. https://doi.org/10.1155/2014/485723
Wang J, Jiang H, Xie J-X (2007) Ferroportin1 and hephaestin are involved in the nigral iron accumulation of 6-OHDA-lesioned rats: nigral iron accumulation of 6-OHDA-lesioned rats. Eur J Neurosci 25:2766–2772. https://doi.org/10.1111/j.1460-9568.2007.05515.x
Wang Q, Zhang X, Chen S et al (2011) Prevention of motor neuron degeneration by novel iron chelators in SOD1G93A transgenic mice of amyotrophic lateral sclerosis. Neurodegener Dis 8:310–321. https://doi.org/10.1159/000323469
Wang J-Y, Zhuang Q-Q, Zhu L-B et al (2016) Meta-analysis of brain iron levels of Parkinson’s disease patients determined by postmortem and MRI measurements. Sci Rep 6:36669. https://doi.org/10.1038/srep36669
Wang Y, Spincemaille P, Liu Z et al (2017) Clinical quantitative susceptibility mapping (QSM): biometal imaging and its emerging roles in patient care: Clinical QSM biometals. J Magn Reson Imaging 46:951–971. https://doi.org/10.1002/jmri.25693
Ward RJ, Zucca FA, Duyn JH et al (2014) The role of iron in brain ageing and neurodegenerative disorders. Lancet Neurol 13:1045–1060. https://doi.org/10.1016/S1474-4422(14)70117-6
Weinreb O, Mandel S, Youdim MBH, Amit T (2013) Targeting dysregulation of brain iron homeostasis in Parkinson’s disease by iron chelators. Free Radical Biol Med 62:52–64. https://doi.org/10.1016/j.freeradbiomed.2013.01.017
Whitnall M, Richardson DR (2006) Iron: a new target for pharmacological intervention in neurodegenerative diseases. Semin Pediatr Neurol 13:186–197. https://doi.org/10.1016/j.spen.2006.08.008
Wofford JD, Chakrabarti M, Lindahl PA (2017) Mössbauer spectra of mouse hearts reveal age-dependent changes in mitochondrial and ferritin iron levels. J Biol Chem 292:5546–5554. https://doi.org/10.1074/jbc.M117.777201
Wong BX, Tsatsanis A, Lim LQ et al (2014) β-Amyloid precursor protein does not possess ferroxidase activity but does stabilize the cell surface ferrous iron exporter ferroportin. PLoS One 9:e114174. https://doi.org/10.1371/journal.pone.0114174
Workman DG, Tsatsanis A, Lewis FW et al (2015) Protection from neurodegeneration in the 6-hydroxydopamine (6-OHDA) model of Parkinson’s with novel 1-hydroxypyridin-2-one metal chelators. Metallomics 7:867–876. https://doi.org/10.1039/C4MT00326H
Wu K-C, Liou H-H, Kao Y-H et al (2017) The critical role of Nramp1 in degrading α-synuclein oligomers in microglia under iron overload condition. Neurobiol Dis 104:61–72. https://doi.org/10.1016/j.nbd.2017.05.001
You L-H, Li F, Wang L et al (2015) Brain iron accumulation exacerbates the pathogenesis of MPTP-induced Parkinson’s disease. Neuroscience 284:234–246. https://doi.org/10.1016/j.neuroscience.2014.09.071
Youdim MBH, Fridkin M, Zheng H (2005) Bifunctional drug derivatives of MAO-B inhibitor rasagiline and iron chelator VK-28 as a more effective approach to treatment of brain ageing and ageing neurodegenerative diseases. Mech Ageing Dev 126:317–326. https://doi.org/10.1016/j.mad.2004.08.023
Zecca L, Berg D, Arzberger T et al (2005) In vivo detection of iron and neuromelanin by transcranial sonography: a new approach for early detection of substantia nigra damage. Mov Disord 20:1278–1285. https://doi.org/10.1002/mds.20550
Zeineddine R, Farrawell NE, Lambert-Smith IA, Yerbury JJ (2017) Addition of exogenous SOD1 aggregates causes TDP-43 mislocalisation and aggregation. Cell Stress Chaperones 22:893–902. https://doi.org/10.1007/s12192-017-0804-y
Zhang Z, Hou L, Song J-L et al (2014) Pro-inflammatory cytokine-mediated ferroportin down-regulation contributes to the nigral iron accumulation in lipopolysaccharide-induced Parkinsonian models. Neuroscience 257:20–30. https://doi.org/10.1016/j.neuroscience.2013.09.037
Zhu Y, Wang B, Tao K et al (2017) Iron accumulation and microglia activation contribute to substantia nigra hyperechogenicity in the 6-OHDA-induced rat model of Parkinson’s disease. Parkinsonism Relat Disord 36:76–82. https://doi.org/10.1016/j.parkreldis.2017.01.003
Zucca FA, Segura-Aguilar J, Ferrari E et al (2017) Interactions of iron, dopamine and neuromelanin pathways in brain aging and Parkinson’s disease. Prog Neurobiol 155:96–119. https://doi.org/10.1016/j.pneurobio.2015.09.012
Acknowledgements
The authors wish to thank the support of the Lille University Hospital University of Lille, INSERM, the NS-Park/FCRIN clinical research network for Parkinson’s disease, the FILSAN network for amyotrophic lateral sclerosis, the French Ministry of Health (PHRC for FAIRALS-II study) the European commission for the grant N° 633190 of the H2020 program; NCT02655315 (FAIRPARK-II study), the DN2M regional fund. The authors also thank the Fédération de la Recherche Clinique du CHU de Lille, the French Charity France Parkinson, the French Charity ARLSA. The authors wish to than ApoPharma for providing deferiprone and advices for the investigator drive studies. FAIRPARK-II study group (with the support of the Lille University Hospital and NS-Park/FCRIN clinical research network, www.fairpark2.eu; funded by European commission grant N° 633190 of the H2020 program; NCT02655315). Abbruzzese Giovanni University of Genove Italy. Allain Marie-Anne ALLAIN CHU Lille France. Anheim Mathieu, Department of Movement Disorders and Neurology, NS-Park/FCRIN Network, CHU Strasbourg, Strasbourg, France. Bakker Martijn University Nijmegen Medical Center, Donders Institute Brain Cognition & Behaviour Center for Neurosciences The Netherland. Balzer-Geldsetzer Monika ipps University Hospital Essen, GermanyUniversitat Marburg. Bargalló Núria Magnetic Resonance Unit, Neurorradiology Section, Centre de Diagnòstic per la Imatge (CDI), IDIBAPS, Hospital Clínic, Barcelona, Catalonia, Spain. Barone Paolo University of Salerno Italy. Basenau Sandra, Philipps Universitat Marburg, Germany. Benchetrit Eve ICM, Hôpital Pitié-Salpêtrière, Paris, France. Berg Daniela, Department of Neurology, Christian-Albrechts-University of Kiel, Kiel, Germany. Bloem Bas University Nijmegen Medical Center, Donders Institute Brain Cognition & Behaviour Center for Neurosciences The Netherland. Boraud Thomas Université de Bordeaux, Institut des Maladies Neurodégénératives, UMR CNRS 5293 and Department of Neurology, NS-Park/FCRIN Network, CHU de Bordeaux, Bordeaux, France. Bordet Regis, University de Lille, CHU de Lille, INSERM UMRS_1171, Service de Pharmacologie Clinique LICEND COEN Center Lille, France. Bouca Raquel Instituto de Medicina Molecular Lisboa Portugal. Bourdain Frédéric, Hôpital Foch, Suresnes, France. Bouzas Jimena European Clinical Research Infrastructure Network-ERIC, France. Brefel-Courbon Christine, CHU de Toulouse, INSERM; Centre d’Investigation Clinique CIC1436, Services de Neurologie et de Pharmacologie Clinique, NS-Park/FCRIN Network, Toulouse, France. Bubenheim Michael CHU-Hôpitaux de Rouen France. Burn David, Faculty of Medical Sciences Newcastle University United Kingdom. Bush Ashley I., Oxidation Biology Unit, The Florey Institute of Neuroscience and Mental Health, The University of Melbourne, Parkville, Victoria, Australia. Cabantchik Ioav, Della Pergola Chair, Alexander Silberman Institute of Life Sciences, Hebrew University, Jerusalem, 91,904, Israel. Calvas Fabienne, CHU de Toulouse, INSERM; Centre d’Investigation Clinique CIC1436, Services de Neurologie et de Pharmacologie Clinique, NS-Park/FCRIN Network, Toulouse, France. Cámara Ana Parkinson’s disease & Movement Disorders Unit, Neurology Service, Hospital Clínic de Barcelona, IDIBAPS, University of Barcelona, CIBERNED, Barcelona, Catalonia, Spain. Carrière Nicolas, University de Lille, CHU de Lille, INSERM UMRS_1171, Service de Neurologie NS-Park/FCRIN Network LICEND COEN Center Lille, France. Chaigneau Véronique, NS-Park/FCRIN Network, Toulouse, France. Compta Yaroslau, Parkinson’s disease & Movement Disorders Unit, Neurology Service, Hospital Clínic de Barcelona, IDIBAPS Barcelona, Catalonia, Spain. Connelly John, ApoPharma Inc., Toronto, Canada. Cormier-Dequaire Florence Hôpital Pitié-Salpêtrière, Paris, France. Corvol Jean-Christophe, Sorbonne Universités, UPMC Univ Paris 06, and INSERM UMRS_1127 and CIC_1422, and CNRS UMR_7225, and AP-HP, and ICM, Hôpital Pitié-Salpêtrière, NS-Park/FCRIN Network, Département des maladies du système nerveux, Paris, France. Cranston Amy University of Newcastle upon Tyne UK. De Bie Rob, Academisch Medisch Centrum Universiteit van Amsterdam.Amsterdam, Netherlands. De Marzi Roberto, Department of Neurology, Medical University Innsbruck, Innsbruck, Austria. Defebvre Luc, University de Lille, CHU de Lille, INSERM UMRS_1171, Service de Neurologie NS-Park/FCRIN Network LICEND COEN Center Lille, France. Degos Bertrand Hôpital Pitié-Salpêtrière, Paris, France. Demotes Jacques, European Clinical Research Infrastructure Network-ERIC, France. Dellapina Estelle, NS-Park/FCRIN Network, Toulouse, France. Deplanque Dominique, University de Lille, CHU de Lille, INSERM UMRS_1171, Service de Pharmacologie Clinique et CIC-CHU Lille, LICEND COEN Center Lille, France. Devedjian Jean-Christophe, University de Lille, CHU de Lille, INSERM UMRS_1171, NS-Park/FCRIN Network LICEND COEN Center Lille, France. Devos David, University de Lille, CHU de Lille, INSERM UMRS_1171, Service de Pharmacologie Clinique et service de Neurologie NS-Park/FCRIN Network LICEND COEN Center Lille, France. Dexter David, Imperial College London London United Kingdom. Dodel Richard, University Hospital Essen, GermanyPhilipps Universitat Marburg Germany. Dongmo Carole Hôpital Pitié-Salpêtrière, Paris, France. Duce James, School of Biomedical Sciences, Faculty of Biological Sciences, University of Leeds, Leeds, West Yorkshire, UK & Oxidation Biology Unit, The Florey Institute of Neuroscience and Mental Health, The University of Melbourne, Parkville, Victoria, Australia. Duhamel Alain, CHU Lille France. Dupouy Julia, CHU de Toulouse, INSERM; Centre d’Investigation Clinique CIC1436, Services de Neurologie et de Pharmacologie Clinique, NS-Park/FCRIN Network, Toulouse, France. Durif Franck, Department of Movement Disorders and Neurology, NS-Park/FCRIN Network, CHU Clermont-Ferrand, Clermont-Ferrand, France. Dusek Petr, Dept. of Neurology, Charles University, Prague, Czech Republic. Eusebio Alexandre, Department of Neurology and Movement Disorders – APHM Timone University Hospital and Institut de Neurosciences de la Timone, NS-Park/FCRIN Network, AMU-CNRS UMR 7289, Marseille, France. Eyvrard Frédéric, Pharmacy, CHU de Toulouse, Toulouse, France. Fernández Manel Parkinson’s disease & Movement Disorders Unit, Neurology Service, Hospital Clínic de Barcelona, IDIBAPS, University of Barcelona, CIBERNED, Barcelona, Catalonia, Spain. Ferreira Joaquim, Instituto de Medicina Molecular Lisboa Portugal. Forni Gian Luca, Ospedia Galliera Italy. Foubert-Samier Alexandra Université de Bordeaux, Institut des Maladies Neurodégénératives, UMR CNRS 5293 and Department of Neurology, NS-Park/FCRIN Network, CHU de Bordeaux, Bordeaux, France. Fradette Caroline, ApoPharma Inc., Toronto, Canada. Fréville Laëtitia, Centre pour l’Acquisition et le Traitement des Images (www.cati-neuroimaging.com); Sorbonne Universités, UPMC Univ Paris 06, CNRS, INSERM, Laboratoire d’Imagerie Biomédicale, F-75013, Paris, France. Galitzky Monique, CHU de Toulouse, INSERM; Centre d’Investigation Clinique CIC1436, Services de Neurologie et de Pharmacologie Clinique, NS-Park/FCRIN Network, Toulouse, France. Gaudebout Cecile Hôpital Pitié-Salpêtrière, Paris, France. Gelé Patrick CHU de Lille CHU Lille France. Giladi Nir Tel Aviv Sourasky Medical Center Israel. Grabli David Hôpital Pitié-Salpêtrière, Paris, France. Grolez Guillaume University de Lille, CHU de Lille, INSERM UMRS_1171, Service de Neurologie NS-Park/FCRIN Network LICEND COEN Center Lille, France. Guyon Pauline CHU Lille France. Habert Marie-Odile, Sorbonne Universités, UPMC Univ Paris 06, CNRS, INSERM, Laboratoire d’Imagerie Biomédicale, AP-HP, Hôpital Pitié-Salpêtrière, Département de Médecine Nucléaire, F-75013, Paris, France. Harroch Estelle, CHU de Toulouse, INSERM; Centre d’Investigation Clinique CIC1436, Services de Neurologie et de Pharmacologie Clinique, Toulouse, France. Hartmann Andreas Hôpital Pitié-Salpêtrière, Paris, France. Hirsch Denise, INSERM - Transfert SA Paris. Hopfner Franziska Department of Neurology, Christian-Albrechts-University of Kiel, Kiel, Germany. Jurado Camille, Pharmacy, CHU de Toulouse, Toulouse, France. Kaiser Andreas Medizinische Universitat Innsbruck Austria. Klaus Seppi Medizinische Universitat Innsbruck. Kouassi Nadège, CHU de Toulouse, INSERM; Centre d’Investigation Clinique CIC1436, Services de Neurologie et de Pharmacologie Clinique, Toulouse, France. Labreuch Julien CHU de Lille CHU Lille France. Lacomblez Lucette Hôpital Pitié-Salpêtrière, Paris, France. Lanthaler Barbara Medizinische Universitat Innsbruck Austria. Le Forestier Nadine Assistance Publique – Hôpitaux de Paris France. Le Naour Stéphanie INSERM - Transfert SA Paris France. Le Toullec Benjamin Hôpital Pitié-Salpêtrière, Paris, France. Locatelli Maxime, Centre pour l’Acquisition et le Traitement des Images (www.cati-neuroimaging.com); ICM Institut du Cerveau et de la Moelle épinière, CNRS UMR7225, INSERM U1127, UPMC, F-75013, Paris, France. Lomeña Francisco Nuclear Medicine Department, Hospital Clíınic, IDIBAPS, University of Barcelona, CIBERSAM, Barcelona, Catalonia, Spain. Longato Nadine Department of Movement Disorders and Neurology, NS-Park/FCRIN Network, CHU Strasbourg, Strasbourg, France. Lützen Ulf Department of Nuclear Medicine, Molecular Diagnostic Imaging and Therapy, University Hospital of Schleswig–Holstein (UKSH), Campus Kiel, Germany. Maetzler Corina Department of Neurology, Christian-Albrechts-University of Kiel, Kiel, Germany. Maetzler Walter, Department of Neurology, Christian-Albrechts-University of Kiel, Kiel, Germany. Mahlknecht Philipp Medizinische Universitat Innsbruck Austria. Mangone Graziella Hôpital Pitié-Salpêtrière, Paris, France. Mariani Louise-Laure Hôpital Pitié-Salpêtrière, Paris, France. Marques Ana, Department of Movement Disorders and Neurology, NS-Park/FCRIN Network, CHU Clermont-Ferrand, Clermont-Ferrand, France. Matthias Löhle, MD, Department of Neurology, University of Rostock, Rostock, Germany. Meissner Wassilios G., Université de Bordeaux, Institut des Maladies Neurodégénératives, UMR CNRS 5293 and Department of Neurology, NS-Park/FCRIN Network, CHU de Bordeaux, Bordeaux, France. Michon Amelie, European Clinical Research Infrastructure Network-ERIC, France. Moreau Caroline, University de Lille, CHU de Lille, INSERM UMRS_1171, Service de Neurologie NS-Park/FCRIN Network LICEND COEN Center Lille, France. Nardocci Nardo Nardocci Istitu Besta Italy. Nosal Florence CHU de Lille France. Nyholm Dag Uppsala University Sweden. Oeckl Patrick Universitaet Ulm Germany. Ory Fabienne, CHU de Toulouse, INSERM; Centre d’Investigation Clinique CIC1436, Services de Neurologie et de Pharmacologie Clinique, Toulouse, France. Otto Markus, Universitaet Ulm Germany. Ouk Thavarak University de Lille, CHU de Lille, INSERM UMRS_1171, Service de Neurologie NS-Park/FCRIN Network LICEND COEN Center Lille, France. Pavese Nicola University of Newcastle upon Tyne UK. Peball Marina Medizinische Universitat Innsbruck Austria. Phillips Clélie Department of Movement Disorders and Neurology, NS-Park/FCRIN Network, CHU Strasbourg, Strasbourg, France. Pineau Fanny Hôpital Pitié-Salpêtrière, Paris, France. Planellas Lluís Parkinson’s disease & Movement Disorders Unit, Neurology Service, Hospital Clínic de Barcelona, IDIBAPS, University of Barcelona, CIBERNED, Barcelona, Catalonia, Spain. Poewe Werner, Department of Neurology, Medical University Innsbruck, Innsbruck, Austria. Pop-Ilieva Lydia, ApoPharma Inc., Toronto, Canada. Post Bart, Radboud University Nijmegen Medical Center, Donders Institute Brain Cognition & Behaviour Center for Neurosciences The Netherland. Rabier Aurélie Inserm NS-Park/FCRIN Network, Toulouse, France. Rascol Olivier, Université de Toulouse, UPS, CHU de Toulouse, INSERM; Centre d’Investigation Clinique CIC1436, Services de Neurologie et de Pharmacologie Clinique, UMR TONIC, NS-Park/FCRIN Network, NeuroToul COEN Center, Toulouse, France. Riedel Christian Department of Neuroradiology, Christian-Albrechts University, Kiel, Germany. Rodrigues Maura Hôpital Pitié-Salpêtrière, Paris, France. Rose Christian Hopital Saint-Vincent-de-Paul Lille France. Roullet-Solignac Isabelle Movement Disorders Unit, Hopital Neurologique, Hospices Civils de Lyon, Université de Lyon, Université Claude Bernard Lyon 1, CNRS Institut des Sciences Cognitives, Centre de Neurosciences, Cognitives, UMR 5229, NS-Park/FCRIN Network, Bron Lyon France. Rozova Anna, ApoPharma Inc., Toronto, Canada. Růžička Evžen, Dept. of Neurology, Charles University, Prague, Czech Republic. Salis Alexandra, Inserm NS-Park/FCRIN Network, Toulouse, France. Schäffer Eva Department of Neurology, University Hospital Schleswig–Holstein, Christian-Albrechts University Kiel, Germany. Scherfler Christoph Department of Neurology, Medical University Innsbruck, Innsbruck, Austria. Schiefermeier Natalia, Department of Neurology, Medical University Innsbruck, Innsbruck, AustriaSeppi Klaus Department of Neurology, Medical University Innsbruck, Innsbruck, AustriaSmagghe Delphine, INSERM - Transfert SA Paris France. Silva Tânia, Instituto de Medicina Molecular Lisboa Portugal. Socha Julie Hôpital Pitié-Salpêtrière, Paris, France. Souyris Corinne, CHU de Toulouse, INSERM; Centre d’Investigation Clinique CIC1436, Services de Neurologie et de Pharmacologie Clinique, Toulouse, France. Spampinato Umberto Université de Bordeaux, Institut des Maladies Neurodégénératives, UMR CNRS 5293 and Department of Neurology, NS-Park/FCRIN Network, CHU de Bordeaux, Bordeaux, France. Spino Michael, ApoPharma Inc., Toronto, Canada. Steel Alison University of Newcastle upon Tyne UK. Sweta Bajaj Medizinische Universitat Innsbruck Austria. Thalamas Claire, CHU de Toulouse, INSERM; Centre d’Investigation Clinique CIC1436, Services de Neurologie et de Pharmacologie Clinique, Toulouse, France. Teodor Danaila Movement Disorders Unit, Hopital Neurologique, Hospices Civils de Lyon, Université de Lyon, Université Claude Bernard Lyon 1, CNRS Institut des Sciences Cognitives, Centre de Neurosciences, Cognitives, UMR 5229, NS-Park/FCRIN Network, Bron Lyon France. Teresa Anna Instituto de Medicina Molecular Lisboa Portugal. Thibault Laetitia, CHU Lille France. Thobois Stéphane, Movement Disorders Unit, Hopital Neurologique, Hospices Civils de Lyon, Université de Lyon, Université Claude Bernard Lyon 1, CNRS Institut des Sciences Cognitives, Centre de Neurosciences, Cognitives, UMR 5229, NS-Park/FCRIN Network, Bron Lyon FranceFrance. Tison François Université de Bordeaux, Institut des Maladies Neurodégénératives, UMR CNRS 5293 and Department of Neurology, NS-Park/FCRIN Network, CHU de Bordeaux, Bordeaux, France. Tolosa Eduardo, Parkinson’s disease & Movement Disorders Unit, Neurology Service, Hospital Clínic de Barcelona, IDIBAPS, University of Barcelona, CIBERNED, Barcelona, Catalonia, Spain. Tranchant Christine, Department of Movement Disorders and Neurology, NS-Park/FCRIN Network, CHU Strasbourg, Strasbourg, France. Tricta Fernando, ApoPharma Inc., Toronto, Canada. Trifirò Gianluca Trifirò University of Messina & Erasmus Medical Center, Rotterdam The Netherlands. Uwe Walter, MD, Department of Neurology, University of Rostock, Rostock, Germany. Vidailhet Marie Hôpital Pitié-Salpêtrière, Paris, France. Wang Yi, PhD, Departments of Radiology and Biomedical Engineering, Cornell University, New York, USA. Werkmann Mario Medizinische Universitat Innsbruck Austria. Yilmas Rezzak Department of Neurology, University Hospital Schleswig–Holstein, Christian-Albrechts University Kiel, Germany. You Hana Hôpital Pitié-Salpêtrière, Paris, France. Zeuner Kirsten Department of Neurology, University Hospital Schleswig–Holstein, Christian-Albrechts University Kiel, Germany. The investigators of the 24 centres.
Author information
Authors and Affiliations
Consortia
Contributions
(1) The research project: A: conception; B: organization; C: execution. (2) The manuscript: A: writing of the first draft, B. review and critical comment. DD: A1, B1, C1, A2, B2. IC: B1, C1, A2, B2. CM: C1, B2. VD: C1, B2. LMS: C1, B2. HB: C1, B2. FG: C1, A2, B2. ASR: B1, C1, A2, B2. JD: B1, C1, A2, B2. JCD: B1, C1, A2, B2
Corresponding author
Ethics declarations
Conflict of interest
The authors have no financial disclosures to make or potential conflicts of interest to report in relation to this study. The paper is referring to four academic studies including two translational studies already published : FAIRPARK-I (Efficacy and Safety of the Iron Chelator Deferiprone in Parkinson's Disease Protocol ID: 2008-006842-25; ClinicalTrials.gov: NCT00943748) and SAFEFAIR-ALS (Efficacy and Safety of the Iron Chelator Deferiprone in Amyotrophic lateral sclerosis Protocol ID: 2013-001228-21; ClinicalTrials.gov: NCT02164253) and two in progress : FAIRPARK-II (with the French NS-Park network, which is funded by a grant from the European Commission Horizon 2020 PHC13 2014-2015 (N° 633190): “Conservative iron chelation as a disease-modifying strategy in Parkinson’s disease: a multicentre, parallel-group, placebo-controlled, randomized clinical trial of deferiprone” Protocol ID: 2015_22; Clinical trial: NCT02655315 http://fairpark2.eu) and FAIRALS-II (Conservative Iron Chelation by Deferiprone as a Disease-modifying Strategy for Amyotrophic Lateral Sclerosis using a Multicentre, Parallel-group, Placebo-controlled, Randomized Clinical Trial on 240 patients. Protocol ID: 2017-003763-35; ClinicalTrials.gov: NCT03293069 funded by the French Ministry of Health, PHRC-N2017). ApoPharma provided deferiprone and advices on the molecule for the four investigator drive studies. Caroline Moreau has received grants from the France Parkinson charity. She has received various honoraria from pharmaceutical companies for consultancy and lectures on Parkinson’s disease at symposia such as Aguettant, Abbvie, Medtronic, Novartis. James Duce has received research funding from Alzheimer’s Society, Alzheimer’s Research UK, European Commission, Parkinson’s UK and NHMRC. He serves as a scientific advisor on the FAIRPARK II but has no financial disclosures. Ioav Cabantchik consults for Aferrix Ltd (Israel) and Hinoman (Ltd) Israel and has been an invited speaker in meetings organized by Apopharma (Canada) for which he received lecturer honoraria. David Devos has received PHRC grants from the French Ministry of Health and research funding from the ARSLA charity, France Parkinson charity, Credit Agricole Fundation. He has led two pilot investigator driven studies with DFP provided for free by ApoPharma (FAIRPARK-I and SAFE-FAIR ALS-I). He is leading two large investigator driven studies with DFP provided for free by ApoPharma (FAIRPARK-II and FAIR ALS-II). He served on advisory boards, served as a consultant and given lectures for pharmaceutical companies such as Orkyn, Everpharma, Abbvie, Boston Scientific, Lundbeck. Jean-Christophe Devedjian, Véronique Danel, Laura Mahoney-Sanchez, Hind Bouchaoui, Anne-Sophie Rolland have nothing to declare.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Devos, D., Cabantchik, Z.I., Moreau, C. et al. Conservative iron chelation for neurodegenerative diseases such as Parkinson’s disease and amyotrophic lateral sclerosis. J Neural Transm 127, 189–203 (2020). https://doi.org/10.1007/s00702-019-02138-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00702-019-02138-1