Abstract
Background
Intrahepatic cholangiocarcinoma (IHC) is a rare liver malignancy with a rising incidence worldwide. Since no standard treatment has been established so far, the aim of this study was to assess the safety and efficacy of repeated liver resection and/or radiofrequency ablation (RFA) in selected cases with recurrent IHC.
Patients and methods
The outcome of 13 patients who had been treated at least once for recurrent IHC by repeated liver resection and/or RFA was retrospectively analyzed. A total of 12 repeated liver resections and 8 radiofrequency ablations were performed in these patients between 2002 and 2008.
Results
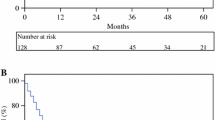
After a median follow-up period of 28 months after primary liver resection (12–69 months), seven patients (54%) are still alive and three of these patients (23% of the entire cohort) are regarded as disease-free. The median survival for all patients was 51 months (12–69 months). One- and three-year survival after primary surgery was 92 and 52%, respectively, with an overall complication rate of 7.6%.
Conclusion
According to the present data, repeated liver resection and radiofrequency ablation are feasible in select patients with recurrent IHC. Both procedures can be regarded as safe and might lead to a prolongation of patient survival.


Similar content being viewed by others
References
Ustundag Y, Bayraktar Y. Cholangiocarcinoma: a compact review of the literature. World J Gastroenterol. 2008;14(42):6458–66.
Endo I, Gonen M, Yopp AC, Dalal KM, Zhou Q, Klimstra D, et al. Intrahepatic cholangiocarcinoma. Rising frequency, improved survival, and determinants of outcome after resection. Ann Surg. 2008;248(1):84–96.
De Oliveira ML, Cunningham SC, Cameron JL, et al. Cholangiocarcinoma: thirty-one-year experience with 564 patients at a single institution. Ann Surg. 2007;245:755–62.
Hammill CW, Wong LL. Intrahepatic cholangiocarcinoma: a malignancy of increasing importance. J Am Coll Surg. 2008;207:594–603.
Chu KM, Lai EC, Al-Hadeedi S, Arcilla CE, Lo CM, Liu CL, et al. Intrahepatic cholangiocarcinoma. World J Surg. 1997;21:301–5.
Shimada K, Sano T, Sakamoto Y, et al. Surgical outcomes of the mass-forming plus periductal infiltrating types of intrahepatic cholangiocarcinoma: a comparative study with the typical mass-forming type of intrahepatic cholangiocarcinoma. World J Surg. 2007;31:2016–22.
Jonas S, Thelen A, Benckert C, Biskup W, Neumann UP, Rudolph B, et al. Extended liver resection for intrahepatic cholangiocarcinoma: a comparison of the prognostic accuracy of the fifth and sixth editions of the TNM classification. Ann Surg. 2009;249:303–9.
Shimota M, Kubota K. Multi-disciplinary treatment for cholangiocellular carcinoma. World J Gastroenterol. 2007;13(10):1500–4.
Tamandl D, Herberger B, Gruenberger B, Puhalla H, Klinger M, Gruenberger T. Influence of hepatic resection margin on recurrence and survival in intrahepatic cholangiocarcinoma. Ann Surg Oncol. 2008;15(10):2787–94.
Yamamoto M, Takasaki K, Otsubo T, Katsuragawa H, Katagiri S. Recurrence after surgical resection of intrahepatic cholangiocarcinoma. J Hepatobiliary Pancreat Surg. 2001;8:154–7.
Khan SA, Davidson BR, Goldin R, et al. Guidelines for the diagnosis and treatment of cholangiocarcinoma: consensus document. Gut. 2002;51:1–9.
Seehofer D, Kamphues C, Neuhaus P. Management of bile duct cancer. Expert Opin Pharmacother. 2008;9:2843–56.
Weber SM, Janargin WR, Klimstra D, et al. Intrahepatic cholangiocarcinoma: resectability, recurrence pattern, and outcomes. J Am Coll Surg. 2001;193:384–91.
Lang H, Sotiropoulos GC, Frühauf NR, Dömland M, Paul A, Kind EM, et al. Extended hepatectomy for intrahepatic cholangiocellular carcinoma (ICC): when is it worthwhile? Single center experience with 27 resections in 50 patients over a 5-year period. Ann Surg. 2005;241:134–43.
Kurosaki I, Hatakeyama K. Repeated hepatectomy for recurrent intrahepatic cholangiocarcinoma: report of two cases. Eur J Gastroenterol Hepatol. 2005;17:125–30.
Saiura A, Yamamoto J, Kokudo N, Koga R, Seki M, Hiki N, Yamada K, Natori T, Yamaguchi T. Intrahepatic cholangiocarcinoma: analysis of 44 consecutive resected cases including 5 cases with repeat resections. Am J Surg. 2009. doi: 10.1016/j.amjsurg.2008.12.035
Ohtsuka M, Kimura F, Shimizu H, Yoshidome H, Kato A, Yoshitomi H, et al. Significance of repeated resection for recurrent intrahepatic cholangiocarcinoma. Hepatogastroenterology. 2009;56(89):1–5.
Curley SA, Izzo F, Ellis LM, Nicolas VJ, Vallone P. Radiofrequency ablation of hepatocellular cancer in 110 patients with cirrhosis. Ann Surg. 2000;232:381–91.
Lu MD, Yin XY, Xie XY, Xu HX, Xu ZF, Liu GJ, et al. Percutaneous thermal ablation for recurrent hepatocellular carcinoma after hepatectomy. Br J Surg. 2005;92:1393–8.
Chen MS, Li JQ, Zheng Y, et al. A prospective randomized trial comparing percutaneous local ablative therapy and partial hepatectomy for small hepatocellular carcinoma. Ann Surg. 2006;243:321–8.
Lau WY, Lai ECH. The current role of radiofrequency ablation in the management of hepatocellular carcinoma: a systematic review. Ann Surg. 2009;249(1):20–5.
Taura K, Ikai I, Hatano E, et al. Implication of frequent local ablation therapy for intrahepatic recurrence in prolonged survival of patients with hepatocellular carcinoma undergoing hepatic resection: an analysis of 610 patients over 16 years old. Ann Surg. 2006;244:265–73.
Slakey DP. Radiofrequency ablation of recurrent cholangiocarcinoma. Ann Surg. 2002;68:395–7.
Fan WJ, Wu PH, Zhang L, Huang JH, Zhang FJ, Gu YK, et al. Radiofrequency ablation as a treatment for hilar cholangiocarcinoma. World J Gastroenterol. 2008;14(28):4540–5.
Zgodzinski W, Espat NJ. Radiofrequency ablation for incidentally identified primary intrahepatic cholangiocarcinoma. World J Gastroenterol. 2005;11(33):5239–40.
Author information
Authors and Affiliations
Corresponding author
About this article
Cite this article
Kamphues, C., Seehofer, D., Eisele, R.M. et al. Recurrent intrahepatic cholangiocarcinoma: single-center experience using repeated hepatectomy and radiofrequency ablation. J Hepatobiliary Pancreat Sci 17, 509–515 (2010). https://doi.org/10.1007/s00534-009-0256-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00534-009-0256-6