Abstract
Purpose
To identify and summarize the evidence on the cost-effectiveness of photobiomodulation (PBM) therapy for the prevention and treatment of cancer treatment-related toxicities.
Methods
This systematic review was performed according to the Preferred Reporting Items for Systematic Reviews and Meta-Analyses statement (PRISMA) and Meta-analysis Of Observational Studies in Epidemiology (MOOSE). Scopus, MEDLINE/PubMed, and Embase were searched electronically.
Results
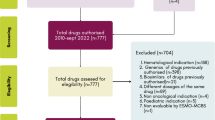
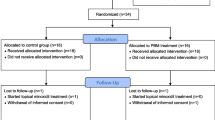
A total of 1490 studies were identified, and after a two-step review, 4 articles met the inclusion criteria. The included studies analyzed the cost-effectiveness of PBM therapy used in the context of lymphedema for breast cancer and oral mucositis (OM) induced by chemotherapy and radiotherapy. Better outcomes were associated with PBM therapy. The incremental cost-effectiveness ratio ranged from 3050.75 USD to 5592.10 USD per grade 3–4 OM case prevented. PBM therapy cost 21.47 USD per percentage point reduction in lymphedema in comparison with 80.51 USD for manual lymph drainage and physical therapy.
Conclusion
There is limited evidence that PBM therapy is cost-effective in the prevention and treatment of specific cancer treatment-related toxicities, namely, OM and breast cancer-related lymphedema. Studies may have underreported the benefits due to a lack of a comprehensive cost evaluation. This suggests a wider acceptance of PBM therapy at cancer treatment centers, which has thus far been limited by the number of robust clinical studies that demonstrate cost-effectiveness for the prevention and treatment of toxicities.

Similar content being viewed by others
Data availability
The authors confirm that the data supporting the findings of the study are available within the article and supplementary materials.
References
Calhoun EA, Chang CH, Welshman EE, Fishman DA, Lurain JR, Bennet CL (2001) Evaluating the total costs of chemotherapy-induced toxicity: results from a pilot study with ovarian cancer patients. Oncologist. 6:441–445
Calhoun EA, Bennett CL (2003) Evaluating the total costs of cancer. Cancer Netw 17:1
Shariati B, MacEntee MI, Yazdizadeh M (2013) The economics of dentistry: a neglected concern. Community Dent Oral Epidemiol 41:385–394
Boyages J, Xu Y, Koelmeyer L et al (2016) The financial cost of lymphedema borne by women with breast cancer. Psycho-Oncology. 26:849–855
Nonzee NJ, Dandade NA, Markossian T (2008) Evaluating the supportive care costs of severe radiochemotherapy-induced mucositis and pharyngitis. Cancer. 113(8):1446–1452
Dean LT, Moss SL, Ransome Y, Frasso-Jaramillo L, Zhang Y, Visvanathan K, Nicholas LH, Schmitz KH (2019) It still affects our economic situation: long-term economic burden of breast cancer and lymphedema. Support Care Cancer 27(5):1697–1708
Ripamonti CI, Molani P, Desti C (2017) A supportive care in cancer unit reduces costs and hospitalizations for transfusions in a comprehensive cancer center. Tumori. 103:449–456
Song X, Wilson KL, Kagan J, Panjabi S (2019) Cost of peripheral neuropathy in patients receiving treatment for multiple myeloma: a US administrative claims analysis. Ther Adv Hematol 10:1–28
Elting LS, Cookley CD, Chambers MS, Garden AS (2007) Risk, outcomes, and costs of radiation-induced oral mucositis among patients with head-and-neck malignancies. Int J Radiat Oncol Biol Phys 68:1110–1120
Brayton KM, Hirsch AT, O’Brien PJ, Cheville A, Karaca-Mandic P, Rockson SG (2014) Lymphedema prevalence and treatment benefits in cancer: impact of a therapeutic intervention on health outcomes and costs lymphedema - consequence of cancer or its treatment. PLoS ONE 9(12):e114597
DeLand MM, Weiss RA, McDaniel DH, Geronemus RG (2007) Treatment of radiation-induced dermatitis with light-emitting diode (LED) photomodulation. Lasers Surg Med 39:164–168
Lima EMT, Lima EJG, de Andrade MF, Bergmann A (2012) Low-level laser therapy in secondary lymphedema after breast cancer: systematic review. Lasers Med Sci 29(3):1289–1295
Argenta PA, Ballman KV, Geller MA, Carson LF, Ghebre R, Mullany SA, Teoh DG, Winterhoff BJ, Rivard CL, Erickson BK (2016) The effect of photobiomodulation on chemotherapy-induced peripheral neuropathy: a randomized, sham-controlled clinical trial. Gynecol Oncol 144(1):159–166
Robijns J, Censabella S, Bulens P, Maes A, Mebis J (2017) The use of low-level light therapy in supportive care for patients with breast cancer: review of the literature. Lasers Med Sci 32(1):229–242
Weissheimer C, Curra M, Gregianin LJ, Daudt LE, Wagner VP, Martins MAT, Martins MD (2017) New photobiomodulation protocol prevents oral mucositis in hematopoietic stem cell transplantation recipients - a retrospective study. Lasers Med Sci 32(9):2013–2021
Zhang X, Li H, Li Q, Li Y, Li C, Zhu M, Zhao B, Li G (2018) Application of red light phototherapy in the treatment of radioactive dermatitis in patients with head and neck cancer. World J Surge Oncol 16(1):222
Sonis TS, Hashemi S, Epstein JB et al (2016) Could the biological robustness of low level laser therapy (Photobiomodulation) impact its use in the management of mucositis in head and neck cancer patients. Oral Oncol 54:7–14
Hamblin MR, Nelson ST, Strahan J (2018) Photobiomodulation and cancer: what is the truth? Photomed Laser Surg 36(5):241–245
González-Arriagada WA, Ramos LMA, Andrade MAC, Lopes MA (2018) Efficacy of low-level laser therapy as an auxiliary tool for management of acute side effects of head and neck radiotherapy. J Cosmet Laser Ther 20:2,117–2,122
De Pauli Paglioni M, Alves CGB, Fontes EK et al (2019) Is photobiomodulation therapy effective in reducing pain caused by toxicities related to head and neck cancer treatment? A systematic review. Support Care Cancer 27(11):4043–4054
Zadick Y, Arany PR, Fregnani ER et al (2019) Systematic review of photobiomodulation for the management of oral mucositis in cancer patients and clinical practice guidelines. Support Care Cancer 27(10):3969–3983
Bezinelli LM, Eduardo FP, Lopes RMG et al (2014) Cost-effectiveness of the introduction of specialized oral care with laser therapy in hematopoietic stem cell transplantation. Hematol Oncol 32:31–39
Moher D, Liberati A, Tetzlaff J, Altman DG, PRISMA Group (2010) PRISMA Group. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Int J Surg 8:336–341
Stroup DF, Berlin JA, Morton SC, Olkin I, Williamson GD, Rennie D, Moher D, Becker BJ, Sipe TA, Thacker SB (2000) Meta-analysis of observational studies in epidemiology: a proposal for reporting. Meta-analysis of Observational Studies in Epidemiology (MOOSE) group. JAMA. 283:2008–2012
Ouzzani M, Hammady H, Fedorowicz Z, Elmagarmid A (2016) Rayyan – a web and mobile app for systematic reviews. Syst Rev 5:210
Campbell and cochrane economics methods group and the evidence for policy and practice information and coordinating centre. CCEMG–EPPI - centre cost converter (v.1.6). http://eppi.ioe.ac.uk/costconversion/default.aspx. Accessed 18 March 2020.
Shemilt I, Thomas J, Morciano M (2010) A web-based tool for adjusting costs to a specific target currency and price year. Evid Policy 6:51–59
Munn Z, Moola S, Lisy K, Riitano D, The Joanna Briggs Institute (2014) The Joanna Briggs Institute Reviewer’s Manual 2014 Edition: Meta-Analysis of Statistics Assessment and Review Instrument (MAStARI) critical appraisal tools Comparable cohort/Case control studies. International Journal of Surgery, Adelaide
Evers S, Goossens M, de Vet H, van Tulder M, Ament A (2005) Criteria list for assessment of methodological quality of economic evaluations: consensus on health economic criteria. Int J Technol Assess Health Care 21:240–245
Piller N, Thelander A (1995) Treating chronic post-mastectomy lymphedema with low level laser therapy: a cost effective strategy to reduce severity and improve the quality of survival. Laser Ther 7:163–168
Antunes HS, Schluckebier LF, Herchenhorn D et al (2016) Cost-effectiveness of low-level laser therapy (LLLT) in head and neck cancer patients receiving concurrent chemoradiation. Oral Oncol 52:85–90
Martins AFL, Nogueira TE, Morais MO, de Sousa-Neto SS, Oton-Leite AF, Valadares MC et al (2020) Cost-effectiveness randomized clinical trial on the effect of photobiomodulation therapy for prevention of radiotherapy-induced severe oral mucositis in Brazilian cancer hospital setting. Support Care Cancer [published online ahead of print, 2020 Jul 3]
WHO (1979) Handbook for reporting results of cancer treatment. WHO Offset Publication No. 48. World Health Organization, Geneva
Simoes A, Eduardo FP, Luiz AC, Campos L, Sá PHRN, Cristófaro M, Marques M, Eduardo CP (2009) Laser phototherapy as topical prophylaxis against head and neck cancer radiotherapy-induced oral mucositis: comparison between low and high/low power lasers. Lasers Surg Med 41:264–270
Ridner SH, Poage-Hooper E, Kanar C, Doersam JK, Bond SM, Dietrich MS (2013) A Pilot randomized trial evaluating low-level laser therapy as an alternative treatment to manual lymphatic drainage for breast cancer-related lymphedema. Oncol Nurs Forum 40(4):383–393
Gobbo M, Ottaviani G, Perinetti G, Ciriello F, Beorchia A, Giacca M, Di Lenarda R, Rupel K, Tirelli G, Zacchigna S, Biasotto M (2014) Evaluation of nutritional status in head and neck radio-treated patients affected by oral mucositis: efficacy of class IV laser therapy. Support Care Cancer 22(7):1851–1856
Shin SS, Jang B, Suh HS et al (2019) Effectiveness, safety, and economic evaluation of topical application of an herbal ointment, Jaungo, for radiation dermatitis after breast conserving surgery in patients with breast cancer (GREEN study). Medicine (Baltimore) 98:15
Elting LS, Chang Y (2019) Cost of oral complications of cancer treatment therapies: estimates and a blueprint for future study. J Natl Cancer Inst Monogr 53:116–123
Elting LS, Cooksley C, Chambers M, Cantor SB, Manzullo E, Rubenstein EB (2003) The burdens of cancer therapy - clinical and economic outcomes of chemotherapy-induced mucositis. Cancer. 98:7
Peterman A, Cella D, Glandon G, Dobrez D, Yount S (2001) Mucositis in Head and neck cancer: economic and quality-of-life outcomes. J Natl Cancer Inst Monogr 29:45–51
Sonis ST, Oster G, Fuchs H, Bellm L, Bradford WZ, Edelsberg J, Hayden V, Eilers J, Epstein JB, LeVeque FG, Miller C, Peterson DE, Schubert MM, Spijkervet FKL, Horowitz M (2001) Oral mucositis and the clinical and economic outcomes of hematopoietic stem-cell transplantation. J Clin Oncol 19:2201–2205
Rodrigo SM, Cunha A, Pozza DH, Blaya DS, Moraes JF, Weber JBB, de Oliveira MG (2009) Analysis of the systemic effect of red and infrared laser therapy on wound repair. Photomed Laser Surg 27(6):929–935
Costa MM, Silva SB, Quinto ALP, Pasquinello PFS, de Queiroz dos Santos V, de Cássia SG, Veiga DF (2014) Phototherapy 660 nm for the prevention and treatment of radiodermatitis in breast cancer patients receiving radiation therapy: study protocol for a randomized controlled trial. Trials. 15:330
Funding
This study is financially supported by the São Paulo Research Foundation (FAPESP) processes numbers 2018/02233-6 and 2018/23479-3, as well as the National Council for Scientific and Technological Development (CNPq).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Kauark-Fontes, E., Rodrigues-Oliveira, L., Epstein, J.B. et al. Cost-effectiveness of photobiomodulation therapy for the prevention and management of cancer treatment toxicities: a systematic review. Support Care Cancer 29, 2875–2884 (2021). https://doi.org/10.1007/s00520-020-05949-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-020-05949-1