Abstract
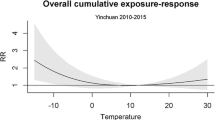
Hazardous thermal conditions resulting from climate change may play a role in cardiovascular disease development. We chose the Universal Thermal Climate Index (UTCI) as the exposure metric to evaluate the relationship between thermal conditions and cardiovascular mortality in Shenzhen, China. We applied quasi-Poisson regression non-linear distributed lag models to evaluate the exposure-response associations. The findings suggest that cardiovascular mortality risks were significantly increased under heat and cold stress, and the adverse effects of cold stress were stronger than heat stress. Referencing the 50th percentile of UTCI (25.4°C), the cumulative risk of cardiovascular mortality was 75% (RRlag0-21 =1.75, 95%CI: 1.32, 2.32) higher in the 1st percentile (3.5°C), and 40% (RRlag0-21=1.40, 95%CI: 1.09, 1.80) higher in the 99th percentile (34.1°C). We observed that individuals older than 65 years were more vulnerable to both cold and heat stress, and females were identified as more susceptible to heat stress than males. Moreover, increased mortality risks of hypertensive disease and cerebrovascular disease were observed under cold stress, while heat stress was related to higher risks of mortality for hypertensive disease and ischemic heart disease. We also observed a stronger relationship between cold stress and ischemic heart disease mortality during the cold season, as well as a significant impact of heat stress on cerebrovascular disease mortality in the warm season when compared to the analysis of the entire year. These results confirm the significant relationship between thermal stress and cardiovascular mortality, with age and sex as potential effect modifiers of this association. Providing affordable air conditioning equipment, increasing the amount of vegetation, and establishing comprehensive early warning systems that take human thermoregulation into account could all help to safeguard the well-being of the public, particularly vulnerable populations, in the event of future extreme weather.



Similar content being viewed by others
Data availability
The meteorological data are openly available in the National Tibetan Plateau Data Center (DOI:10.11888/AtmosphericPhysics.tpe.249369.file). The mortality data are not publicly available due to the access agreement. Still, it can be available with reasonable request and permission from the Shenzhen Center for Disease Control and Prevention.
References
Abrignani MG, Lombardo A, Braschi A, Renda N, Abrignani V (2022) Climatic influences on cardiovascular diseases. World. J Cardiol 14:152–169. https://doi.org/10.4330/wjc.v14.i3.152
Alahmad B, Khraishah H, Royé D, Vicedo-Cabrera AM, Guo Y, Papatheodorou SI et al (2023) Associations between extreme temperatures and cardiovascular cause-specific mortality: results from 27 countries. Circulation 147:35–46. https://doi.org/10.1161/circulationaha.122.061832
Altman DG, Bland JM (2003) Interaction revisited: the difference between two estimates. BMJ 326:219. https://doi.org/10.1136/bmj.326.7382.219
Analitis A, Katsouyanni K, Biggeri A, Baccini M, Forsberg B, Bisanti L et al (2008) Effects of cold weather on mortality: results from 15 European cities within the PHEWE Project. Am J Epidemiol 168:1397–1408. https://doi.org/10.1093/aje/kwn266
Anderson BG, Bell ML (2009) Weather-related mortality: how heat, cold, and heat waves affect mortality in the United States. Epidemiology 20:205–213. https://doi.org/10.1097/EDE.0b013e318190ee08
Baldwin JW, Benmarhnia T, Ebi KL, Jay O, Lutsko NJ, Vanos JK (2023) Humidity’s role in heat-related health outcomes: a heated debate. Environ Health Perspect 131:55001. https://doi.org/10.1289/ehp11807
Ban J, Xu D, He MZ, Sun Q, Chen C, Wang W et al (2017) The effect of high temperature on cause-specific mortality: a multi-county analysis in China. Environ Int 106:19–26. https://doi.org/10.1016/j.envint.2017.05.019
Basu R (2009) High ambient temperature and mortality: a review of epidemiologic studies from 2001 to 2008. Environ Health 8:40–40. https://doi.org/10.1186/1476-069X-8-40
Bhaskaran K, Gasparrini A, Hajat S, Smeeth L, Armstrong B (2013) Time series regression studies in environmental epidemiology. Int J Epidemiol 42:1187–1195. https://doi.org/10.1093/ije/dyt092
Biardeau LT, Davis LW, Gertler P, Wolfram C (2020) Heat exposure and global air conditioning. Nature Sustainability 3:25–28. https://doi.org/10.1038/s41893-019-0441-9
Bittel J, Henane R (1975) Comparison of thermal exchanges in men and women under neutral and hot conditions. J Physiol 250:475–489. https://doi.org/10.1113/jphysiol.1975.sp011066
Blazejczyk K, Epstein Y, Jendritzky G, Staiger H, Tinz B (2012) Comparison of UTCI to selected thermal indices. Int J Biometeorol 56:515–535. https://doi.org/10.1007/s00484-011-0453-2
Błażejczyk K, Jendritzky G, Bröde P, Fiala D, Havenith G, Epstein Y et al (2013) An introduction to the Universal Thermal Climate Index (UTCI). Geographia Polonica 86:5–10. https://doi.org/10.7163/GPol.2013.1
Breitner S, Wolf K, Peters A, Schneider A (2014) Short-term effects of air temperature on cause-specific cardiovascular mortality in Bavaria, Germany. Heart 100:1272. https://doi.org/10.1136/heartjnl-2014-305578
Bröde P, Fiala D, Błażejczyk K, Holmér I, Jendritzky G, Kampmann B et al (2012) Deriving the operational procedure for the Universal Thermal Climate Index (UTCI). Int J Biometeorol 56:481–494. https://doi.org/10.1007/s00484-011-0454-1
Bunker A, Wildenhain J, Vandenbergh A, Henschke N, Rocklöv J, Hajat S et al (2016) Effects of air temperature on climate-sensitive mortality and morbidity outcomes in the elderly; a systematic review and meta-analysis of epidemiological evidence. EBioMedicine 6:258–268. https://doi.org/10.1016/j.ebiom.2016.02.034
Chen R, Wang C, Meng X, Chen H, Thach TQ, Wong CM et al (2013) Both low and high temperature may increase the risk of stroke mortality. Neurology 81:1064–1070. https://doi.org/10.1212/WNL.0b013e3182a4a43c
Chen R, Yin P, Wang L, Liu C, Niu Y, Wang W et al (2018) Association between ambient temperature and mortality risk and burden: time series study in 272 main Chinese cities. BMJ 363:k4306. https://doi.org/10.1136/bmj.k4306
Cheng X, Su H (2010) Effects of climatic temperature stress on cardiovascular diseases. Eur J Intern Med 21:164–167. https://doi.org/10.1016/j.ejim.2010.03.001
Curriero FC, Heiner KS, Samet JM, Zeger SL, Strug L, Patz JA (2002) Temperature and mortality in 11 cities of the eastern United States. Am J Epidemiol 155:80–87. https://doi.org/10.1093/aje/155.1.80
Davis RE, McGregor GR, Enfield KB (2016) Humidity: a review and primer on atmospheric moisture and human health. Environ Res 144:106–116. https://doi.org/10.1016/j.envres.2015.10.014
de Bont J, Jaganathan S, Dahlquist M, Persson Å, Stafoggia M, Ljungman P (2022) Ambient air pollution and cardiovascular diseases: an umbrella review of systematic reviews and meta-analyses. J Intern Med 291:779–800. https://doi.org/10.1111/joim.13467
de Freitas CR, Grigorieva EA (2014) The impact of acclimatization on thermophysiological strain for contrasting regional climates. Int J Biometeorol 58:2129–2137. https://doi.org/10.1007/s00484-014-0813-9
Di Napoli C, Barnard C, Prudhomme C, Cloke HL, Pappenberger F (2021) ERA5-HEAT: A global gridded historical dataset of human thermal comfort indices from climate reanalysis. Geoscience Data Journal 8:2–10. https://doi.org/10.1002/gdj3.102
Duan Y, Liao Y, Li H, Yan S, Zhao Z, Yu S et al (2019) Effect of changes in season and temperature on cardiovascular mortality associated with nitrogen dioxide air pollution in Shenzhen, China. Sci Total Environ 697:134051. https://doi.org/10.1016/j.scitotenv.2019.134051
Fiala D, Havenith G, Bröde P, Kampmann B, Jendritzky G (2012) UTCI-Fiala multi-node model of human heat transfer and temperature regulation. Int J Biometeorol 56:429–441. https://doi.org/10.1007/s00484-011-0424-7
Foster J, Hodder SG, Lloyd AB, Havenith G (2020) Individual responses to heat stress: implications for hyperthermia and physical work capacity. Front Physiol 11:541483. https://doi.org/10.3389/fphys.2020.541483
Gagge AP, Fobelets AP, Berglund LG (1986) A standard predictive index of human response to the thermal environment. ASHRAE Transactions 92:709–731
Gasparrini A (2011) Distributed lag linear and non-linear models in R: the package dlnm. J Stat Softw 43:1–20. https://doi.org/10.18637/jss.v043.i08
Gasparrini A (2014) Modeling exposure–lag–response associations with distributed lag non-linear models. Stat Med 33:881–899. https://doi.org/10.1002/sim.5963
Gasparrini, A., 2021. Distributed lag linear and non-linear models for time series data. https://cran.r-project.org/web/packages/dlnm/index.html. Accessed June 30, 2022.
Gasparrini A, Armstrong B, Kenward MG (2010) Distributed lag non-linear models. Stat Med 29:2224–2234. https://doi.org/10.1002/sim.3940
Gasparrini A, Armstrong B, Kovats S, Wilkinson P (2012) The effect of high temperatures on cause-specific mortality in England and Wales. Occup Environ Med 69:56. https://doi.org/10.1136/oem.2010.059782
Gasparrini A, Guo Y, Hashizume M, Lavigne E, Zanobetti A, Schwartz J et al (2015) Mortality risk attributable to high and low ambient temperature: a multicountry observational study. Lancet 386:369–375. https://doi.org/10.1016/S0140-6736(14)62114-0
Giorgini P, Di Giosia P, Petrarca M, Lattanzio F, Stamerra CA, Ferri C (2017) Climate changes and human health: a review of the effect of environmental stressors on cardiovascular diseases across epidemiology and biological mechanisms. Curr Pharm Des 23:3247–3261. https://doi.org/10.2174/1381612823666170317143248
Goldberg MS, Gasparrini A, Armstrong B, Valois M-F (2011) The short-term influence of temperature on daily mortality in the temperate climate of Montreal, Canada. Environ Res 111:853–860. https://doi.org/10.1016/j.envres.2011.05.022
Gonzalez RR, Nishi Y, Gagge AP (1974) Experimental evaluation of standard effective temperature a new biometeorological index of man’s thermal discomfort. Int J Biometeorol 18:1–15
Guo Y, Li S, Zhang Y, Armstrong B, Jaakkola JJ, Tong S et al (2013) Extremely cold and hot temperatures increase the risk of ischaemic heart disease mortality: epidemiological evidence from China. Heart 99:195–203. https://doi.org/10.1136/heartjnl-2012-302518
Guo Y, Punnasiri K, Tong S (2012) Effects of temperature on mortality in Chiang Mai city, Thailand: a time series study. Environ Health 11:36–36. https://doi.org/10.1186/1476-069X-11-36
Havenith G, Fiala D, Błazejczyk K, Richards M, Bröde P, Holmér I et al (2012) The UTCI-clothing model. Int J Biometeorol 56:461–470. https://doi.org/10.1007/s00484-011-0451-4
He J, Yang K, Tang W, Lu H, Qin J, Chen Y et al (2020) The first high-resolution meteorological forcing dataset for land process studies over China. Scientific Data 7:25. https://doi.org/10.1038/s41597-020-0369-y
Höppe P (1999) The physiological equivalent temperature - a universal index for the biometeorological assessment of the thermal environment. Int J Biometeorol 43:71–75. https://doi.org/10.1007/s004840050118
Hu J, Wen Y, Duan Y, Yan S, Liao Y, Pan H et al (2020) The impact of extreme heat and heat waves on emergency ambulance dispatches due to external cause in Shenzhen, China. Environ Pollut 261:114156. https://doi.org/10.1016/j.envpol.2020.114156
Hu S, Kong L, Gao R, Zhu M, Wang W, Wang Y et al (2012) Outline of the report on cardiovascular disease in China, 2010. Biomed Environ Sci 25:251. https://doi.org/10.3967/0895-3988.2012.03.001
Huang Z, Lin H, Liu Y, Zhou M, Liu T, Xiao J et al (2015) Individual-level and community-level effect modifiers of the temperature–mortality relationship in 66 Chinese communities. BMJ Open 5:e009172. https://doi.org/10.1136/bmjopen-2015-009172
Jendritzky G, de Dear R, Havenith G (2012) UTCI—why another thermal index? Int J Biometeorol 56:421–428. https://doi.org/10.1007/s00484-011-0513-7
Kenney WL, Munce TA (2003) Invited review: aging and human temperature regulation. J Appl Physiol 95:2598–2603. https://doi.org/10.1152/japplphysiol.00202.2003
Kim CT, Lim YH, Woodward A, Kim H (2015) Heat-attributable deaths between 1992 and 2009 in Seoul, South Korea. PloS One 10:e0118577. https://doi.org/10.1371/journal.pone.0118577
Kottek M, Grieser J, Beck C, Rudolf B, Rubel F (2006) World Map of the Köppen-Geiger climate classification updated. Meteorol Z 15:259–263. https://doi.org/10.1127/0941-2948/2006/0130
Lam CKC, Lau KK-L (2018) Effect of long-term acclimatization on summer thermal comfort in outdoor spaces: a comparative study between Melbourne and Hong Kong. Int J Biometeorol 62:1311–1324. https://doi.org/10.1007/s00484-018-1535-1
Lee V, Zermoglio F, Ebi K (2019) Heat waves and human health: emerging evidence and experience to inform risk management. https://www.climatelinks.org/resources/heat-waves-and-human-health-emerging-evidence-and-experience-inform-risk-management. Accessed 27 Sept 2022
Lin S, Luo M, Walker RJ, Liu X, Hwang SA, Chinery R (2009) Extreme high temperatures and hospital admissions for respiratory and cardiovascular diseases. Epidemiology 20:738–746. https://doi.org/10.1097/EDE.0b013e3181ad5522
Lin Y-K, Sung F-C, Honda Y, Chen Y-J, Wang Y-C (2020) Comparative assessments of mortality from and morbidity of circulatory diseases in association with extreme temperatures. Sci Total Environ 723:138012. https://doi.org/10.1016/j.scitotenv.2020.138012
Liu C, Yavar Z, Sun Q (2015) Cardiovascular response to thermoregulatory challenges. Am J Physiol Heart Circ Physiol 309:H1793–H1812. https://doi.org/10.1152/ajpheart.00199.2015
Liu J, Varghese BM, Hansen A, Zhang Y, Driscoll T, Morgan G et al (2022) Heat exposure and cardiovascular health outcomes: a systematic review and meta-analysis. Lancet Planet Health 6:e484–e495. https://doi.org/10.1016/S2542-5196(22)00117-6
Ma P, Zhou J, Wang S, Li T, Fan X, Fan J et al (2018) Differences of hemorrhagic and ischemic strokes in age spectra and responses to climatic thermal conditions. Sci Total Environ 644:1573–1579. https://doi.org/10.1016/j.scitotenv.2018.07.080
Ma Y, Zhou L, Chen K (2020) Burden of cause-specific mortality attributable to heat and cold: a multicity time-series study in Jiangsu Province, China. Environ Int 144:105994. https://doi.org/10.1016/j.envint.2020.105994
Matzarakis A, Rutz F, Mayer H (2007) Modelling radiation fluxes in simple and complex environments—application of the RayMan model. Int J Biometeorol 51:323–334. https://doi.org/10.1007/s00484-006-0061-8
Matzarakis A, Rutz F, Mayer H (2010) Modelling radiation fluxes in simple and complex environments: basics of the RayMan model. Int J Biometeorol 54:131–139. https://doi.org/10.1007/s00484-009-0261-0
Mayer H, Höppe P (1987) Thermal comfort of man in different urban environments. Theor Appl Climatol 38:43–49. https://doi.org/10.1007/BF00866252
McGregor GR, Vanos JK (2018) Heat: a primer for public health researchers. Public Health 161:138–146. https://doi.org/10.1016/j.puhe.2017.11.005
Meade RD, Akerman AP, Notley SR, McGinn R, Poirier P, Gosselin P et al (2020) Physiological factors characterizing heat-vulnerable older adults: a narrative review. Environ Int 144:105909. https://doi.org/10.1016/j.envint.2020.105909
Mendis S (2017) Global progress in prevention of cardiovascular disease. Cardiovasc Diagn Ther:S32–S38. https://doi.org/10.21037/cdt.2017.03.06
Meteorological Bureau of Shenzhen Municipality (2022) General situation of climate and characteristics of four seasons in Shenzhen. http://weather.sz.gov.cn/qixiangfuwu/qihoufuwu/qihouguanceyupinggu/qihougaikuang/content/post_3573760.html. Accessed 24 Sept 2022
Moghadamnia MT, Ardalan A, Mesdaghinia A, Keshtkar A, Naddafi K, Yekaninejad MS (2017) Ambient temperature and cardiovascular mortality: a systematic review and meta-analysis. PeerJ 5:e3574–e3574. https://doi.org/10.7717/peerj.3574
Mora C, Counsell CWW, Bielecki CR, Louis LV (2017) Twenty-seven ways a heat wave can kill you. Circ Cardiovasc Qual Outcomes 10:e004233. https://doi.org/10.1161/CIRCOUTCOMES.117.004233
Narita K, Hoshide S, Kario K (2021) Seasonal variation in blood pressure: current evidence and recommendations for hypertension management. Hypertens Res 44:1363–1372. https://doi.org/10.1038/s41440-021-00732-z
Nyadanu SD, Tessema GA, Mullins B, Pereira G (2022) Maternal acute thermophysiological stress and stillbirth in Western Australia, 2000–2015: a space-time-stratified case-crossover analysis. Sci Total Environ 836:155750. https://doi.org/10.1016/j.scitotenv.2022.155750
Ou CQ, Song YF, Yang J, Chau PY, Yang L, Chen PY et al (2013) Excess winter mortality and cold temperatures in a subtropical city, Guangzhou, China. PloS One 8:e77150. https://doi.org/10.1371/journal.pone.0077150
Ou CQ, Yang J, Ou QQ, Liu HZ, Lin GZ, Chen PY et al (2014) The impact of relative humidity and atmospheric pressure on mortality in Guangzhou, China. Biomed Environ Sci 27:917–925. https://doi.org/10.3967/bes2014.132
Pan R, Okada A, Yamana H, Yasunaga H, Kumazawa R, Matsui H et al (2023) Association between ambient temperature and cause-specific cardiovascular disease admissions in Japan: a nationwide study. Environ Res 225:115610. https://doi.org/10.1016/j.envres.2023.115610
Pantavou K (2021) Outdoor thermal environment and heat-related symptoms of pedestrians: an application of the UTCI for health risk assessment. In: Krüger EL (ed) Applications of the Universal Thermal Climate Index UTCI in Biometeorology: Latest Developments and Case Studies. Springer International Publishing, Cham, pp 137–153. https://doi.org/10.1007/978-3-030-76716-7_7
Psistaki K, Dokas IM, Paschalidou AK (2023) Analysis of the heat- and cold-related cardiovascular mortality in an urban mediterranean environment through various thermal indices. Environ Res 216:114831. https://doi.org/10.1016/j.envres.2022.114831
Qiao Z, Guo Y, Yu W, Tong S (2015) Assessment of short- and long-term mortality displacement in heat-related deaths in Brisbane, Australia, 1996–2004. Environ Health Perspect 123:766–772. https://doi.org/10.1289/ehp.1307606
Qiu H, Tian L, Ho KF, Yu IT, Thach TQ, Wong CM (2016) Who is more vulnerable to death from extremely cold temperatures? A case-only approach in Hong Kong with a temperate climate. Int J Biometeorol 60:711–717. https://doi.org/10.1007/s00484-015-1065-z
Rai M, Breitner S, Huber V, Zhang S, Peters A, Schneider A (2023) Temporal variation in the association between temperature and cause-specific mortality in 15 German cities. Environ Res 229:115668. https://doi.org/10.1016/j.envres.2023.115668
Requia WJ, Alahmad B, Schwartz JD, Koutrakis P (2023) Association of low and high ambient temperature with mortality for cardiorespiratory diseases in Brazil. Environ Res 234:116532. https://doi.org/10.1016/j.envres.2023.116532
Rodrigues M, Santana P, Rocha A (2019) Effects of extreme temperatures on cerebrovascular mortality in Lisbon: a distributed lag non-linear model. Int J Biometeorol 63:549–559. https://doi.org/10.1007/s00484-019-01685-2
Romaszko J, Draganska E, Jalali R, Cymes I, Glinska-Lewczuk K (2022) Universal Climate Thermal Index as a prognostic tool in medical science in the context of climate change: a systematic review. Sci Total Environ 828:154492. https://doi.org/10.1016/j.scitotenv.2022.154492
Roth GA, Mensah GA, Johnson CO, Addolorato G, Ammirati E, Baddour LM et al (2020) Global burden of cardiovascular diseases and risk factors, 1990–2019: update from the GBD 2019 study. J Am Coll Cardiol 76:2982–3021. https://doi.org/10.1016/j.jacc.2020.11.010
Santurtún A, Almendra R, Fdez-Arroyabe P, Sanchez-Lorenzo A, Royé D, Zarrabeitia MT et al (2020) Predictive value of three thermal comfort indices in low temperatures on cardiovascular morbidity in the Iberian peninsula. Sci Total Environ 729:138969. https://doi.org/10.1016/j.scitotenv.2020.138969
Saucy A, Ragettli MS, Vienneau D, de Hoogh K, Tangermann L, Schäffer B et al (2021) The role of extreme temperature in cause-specific acute cardiovascular mortality in Switzerland: a case-crossover study. Sci Total Environ 790:147958. https://doi.org/10.1016/j.scitotenv.2021.147958
Schlader ZJ, Mündel T (2012) Heat Acclimatization. In: Mooren FC (ed) Encyclopedia of exercise medicine in health and disease. Springer, Berlin Heidelberg, Berlin, Heidelberg, pp 391–393. https://doi.org/10.1007/978-3-540-29807-6_95
Skutecki R, Jalali R, Dragańska E, Cymes I, Romaszko J, Glińska-Lewczuk K (2019) UTCI as a bio-meteorological tool in the assessment of cold-induced stress as a risk factor for hypertension. Sci Total Environ 688:970–975. https://doi.org/10.1016/j.scitotenv.2019.06.280
Son JY, Liu J, Bell M (2019) Temperature-related mortality: a systematic review and investigation of effect modifiers. Environ Res Lett 14. https://doi.org/10.1088/1748-9326/ab1cdb
Staiger H, Laschewski G, Matzarakis A (2019) Selection of appropriate thermal indices for applications in human biometeorological studies. Atmosphere 10(1):18. https://doi.org/10.3390/atmos10010018
Statistics Bureau of Shenzhen Municipality (2021) Shenzhen Statistical Yearbook 2021. http://tjj.sz.gov.cn/attachment/0/950/950362/9491388.pdf. Accessed 22 Jun 2022
Sun Z (2010) Cardiovascular responses to cold exposure. Front Biosci (Elite Ed) 2:495–503. https://doi.org/10.2741/e108
Tao J, Zhang Y, Li Z, Yang M, Huang C, Hossain MZ et al (2023) Daytime and nighttime high temperatures differentially increased the risk of cardiovascular disease: a nationwide hospital-based study in China. Environ Res 236:116740. https://doi.org/10.1016/j.envres.2023.116740
The Writing Committee of the Report on Cardiovascular Health Diseases in China (2022) Report on cardiovascular health and diseases in China 2021: an updated summary. Biomed Environ Sci 35:573. https://doi.org/10.3967/bes2022.079
United Nations Sustainable Development Agenda (2015) Transforming our world: the 2030 Agenda for Sustainable Development. https://sdgs.un.org/2030agenda. Accessed 17 Aug 2022
Urban A, Di Napoli C, Cloke HL, Kyselý J, Pappenberger F, Sera F et al (2021) Evaluation of the ERA5 reanalysis-based Universal Thermal Climate Index on mortality data in Europe. Environ Res 198:111227. https://doi.org/10.1016/j.envres.2021.111227
Urban A, Kyselý J (2014) Comparison of UTCI with other thermal indices in the assessment of heat and cold effects on cardiovascular mortality in the Czech Republic. Int J Environ Res Public Health 11:952–967. https://doi.org/10.3390/ijerph110100952
Vanos JK, Baldwin JW, Jay O, Ebi KL (2020) Simplicity lacks robustness when projecting heat-health outcomes in a changing climate. Nat Commun 11:6079. https://doi.org/10.1038/s41467-020-19994-1
Wang P, Zhang X, Hashizume M, Goggins WB, Luo C (2021) A systematic review on lagged associations in climate–health studies. Int J Epidemiol 50:1199–1212. https://doi.org/10.1093/ije/dyaa286
Wang X, Li G, Liu L, Westerdahl D, Jin X, Pan X (2015) Effects of extreme temperatures on cause-specific cardiovascular mortality in China. Int J Environ Res Public Health 12:16136–16156. https://doi.org/10.3390/ijerph121215042
Weihs P, Staiger H, Tinz B, Batchvarova E, Rieder H, Vuilleumier L et al (2012) The uncertainty of UTCI due to uncertainties in the determination of radiation fluxes derived from measured and observed meteorological data. Int J Biometeorol 56:537–555. https://doi.org/10.1007/s00484-011-0416-7
World Health Organization (2021) Cardiovascular diseases (CVDs). https://www.who.int/en/news-room/fact-sheets/detail/cardiovascular-diseases-(cvds). Accessed 18 Aug 2021
Xia Y, Shi C, Li Y, Jiang X, Ruan S, Gao X et al (2023) Effects of ambient temperature on mortality among elderly residents of Chengdu city in Southwest China, 2016-2020: a distributed-lag non-linear time series analysis. BMC Public Health 23:149. https://doi.org/10.1186/s12889-022-14931-x
Xu R, Shi C, Wei J, Lu W, Li Y, Liu T et al (2022) Cause-specific cardiovascular disease mortality attributable to ambient temperature: a time-stratified case-crossover study in Jiangsu province, China. Ecotoxicol Environ Saf 236:113498. https://doi.org/10.1016/j.ecoenv.2022.113498
Yang C, Meng X, Chen R, Cai J, Zhao Z, Wan Y et al (2015a) Long-term variations in the association between ambient temperature and daily cardiovascular mortality in Shanghai, China. Sci Total Environ 538:524–530. https://doi.org/10.1016/j.scitotenv.2015.08.097
Yang J, Yin P, Zhou M, Ou C-Q, Guo Y, Gasparrini A et al (2015b) Cardiovascular mortality risk attributable to ambient temperature in China. Heart 101:1966. https://doi.org/10.1136/heartjnl-2015-308062
Yang K, He J (2019) China meteorological forcing dataset (1979-2018). National Tibetan Plateau Data Center. https://doi.org/10.11888/AtmosphericPhysics.tpe.249369.file
Yang L, Li L, Lewington S, Guo Y, Sherliker P, Bian Z et al (2015c) Outdoor temperature, blood pressure, and cardiovascular disease mortality among 23 000 individuals with diagnosed cardiovascular diseases from China. Eur Heart J 36:1178–1185. https://doi.org/10.1093/eurheartj/ehv023
Yi W, Chan APC (2015) Effects of temperature on mortality in Hong Kong: a time series analysis. Int J Biometeorol 59:927–936. https://doi.org/10.1007/s00484-014-0895-4
Yu W, Mengersen K, Hu W, Guo Y, Pan X, Tong S (2011) Assessing the relationship between global warming and mortality: lag effects of temperature fluctuations by age and mortality categories. Environ Pollut 159:1789–1793. https://doi.org/10.1016/j.envpol.2011.03.039
Zhang W, Du G, Xiong L, Liu T, Zheng Z, Yuan Q et al (2021) Extreme temperatures and cardiovascular mortality: assessing effect modification by subgroups in Ganzhou, China. Glob Health Action 14:1965305. https://doi.org/10.1080/16549716.2021.1965305
Acknowledgements
We appreciate the Shenzhen Center for Disease Control and Prevention for the data collection. We also thank the National Tibetan Plateau Data Center for providing the meteorological dataset.
Funding
The work was supported by the National Natural Science Foundation of China (Grant Nos. 82173628 and 81973004).
Author information
Authors and Affiliations
Contributions
Maidina Jingesi: conceptualization, formal analysis, visualization, writing—original draft preparation, critical review, and editing. Shuhua Lan: data curation, validation, and visualization. Jing Hu: validation, critical review, and editing. Mengyi Dai: data curation, critical review, and editing. Suli Huang: data curation, investigation, and technical support. Siyi Chen: data curation. Ning Liu: data curation. Ziquan Lv: data curation. Jiajia Ji: data curation. Xiaoheng Li: data curation. Peng Wang: validation, supervision, reviewing, and editing. Jinquan Cheng: investigation, funding acquisition, and supervision. Ji Peng: investigation, funding acquisition, and supervision. Ping Yin: investigation, funding acquisition, supervision, reviewing, and editing.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
Not applicable.
Consent for publication
Not applicable.
Competing interests
The authors declare no competing interests.
Additional information
Maidina Jingesi and Shuhua Lan contribute equally to this paper.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Jingesi, M., Lan, S., Hu, J. et al. Association between thermal stress and cardiovascular mortality in the subtropics. Int J Biometeorol 67, 2093–2106 (2023). https://doi.org/10.1007/s00484-023-02565-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00484-023-02565-6