Abstract
Tau and amyloid beta (Aβ) are the prime suspects for driving pathology in Alzheimer’s disease (AD) and, as such, have become the focus of therapeutic development. Recent research, however, shows that these proteins have been highly conserved throughout evolution and may have crucial, physiological roles. Such functions may be lost during AD progression or be unintentionally disrupted by tau- or Aβ-targeting therapies. Tau has been revealed to be more than a simple stabiliser of microtubules, reported to play a role in a range of biological processes including myelination, glucose metabolism, axonal transport, microtubule dynamics, iron homeostasis, neurogenesis, motor function, learning and memory, neuronal excitability, and DNA protection. Aβ is similarly multifunctional, and is proposed to regulate learning and memory, angiogenesis, neurogenesis, repair leaks in the blood–brain barrier, promote recovery from injury, and act as an antimicrobial peptide and tumour suppressor. This review will discuss potential physiological roles of tau and Aβ, highlighting how changes to these functions may contribute to pathology, as well as the implications for therapeutic development. We propose that a balanced consideration of both the physiological and pathological roles of tau and Aβ will be essential for the design of safe and effective therapeutics.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Alzheimer’s disease (AD) is a terminal neurodegenerative disorder associated with severe progressive dementia [155]. The disease is characterised by key neuropathological hallmarks of chronic inflammation, synapse loss, neuronal death and the diagnostic accumulation of insoluble protein aggregates, intracellular neurofibrillary tangles (NFTs), and extracellular amyloid plaques [28, 155, 258]. The disease begins as a primary disorder of short-term memory, learning, and spatial navigation, due to early degeneration of the temporal lobe [174]. In the end stages, however, the spread of pathology throughout the brain results in multimodal deficits, including loss of verbal and motor control [174]. Unfortunately, AD is a common disorder, affecting over 50 million individuals worldwide and representing 60–80% of all dementia cases [5]. Whilst there is evidence that dementia incidence may be declining in the population, potentially attributable to better management of modifiable risk factors, it is not yet known whether this trend will counteract the impact of a shift towards an ageing population [57, 229]. As the population ages, and the risk of developing dementia increases, AD cases are currently set to triple by the year 2050, representing a tremendous global, socio-economic challenge [5]. As existing treatments only target symptoms and do not slow (let alone halt or reverse) the progression of the disease, the need to develop a disease-modifying therapeutic has never been more urgent [155].
Since the identification of microtubule-associated protein tau (MAPT) and amyloid beta (Aβ) as the components of NFTs and extracellular plaques, respectively, research has primarily focused on the toxic roles these proteins play in AD pathogenesis [136, 171, 241]. Accumulation of Aβ causes synapse damage [106, 132, 274] and can induce cognitive and electrophysiological deficits [270]. Similarly, whilst tau was discovered as a microtubule-associated protein (MAP) [276], attention has been drawn to the toxic effects of tau hyperphosphorylation and aggregation [9]. As such, therapeutic development has focused heavily on targeting these proteins through preventing their aggregation, inhibiting their production, or promoting their clearance [155]. Despite promising results in pre-clinical studies, no clinical trials have produced meaningful benefits for patients, with trials being halted due to adverse side effects such as liver toxicity, encephalitis, vasogenic oedema, and even exacerbation of cognitive decline [203, 286]. It is becoming increasingly apparent that the involvement of “pathological” proteins in AD is complex and nuanced [241]. There is mounting evidence that these proteins may serve a number of crucial physiological functions that could be disrupted in the development of AD pathology or by Aβ- or tau-lowering therapeutics.
In this review, we discuss the emerging evidence for key physiological roles of tau and Aβ. The toxic roles of these proteins have been extensively reviewed elsewhere [94, 155, 241], and thus, we aim to highlight possible loss of function phenotypes in disease, as well as identify potentially detrimental side effects of tau- (Table 1) or Aβ (Table 2)-lowering therapeutics if not appropriately targeted. This will be especially important when considering treatment of the adult nervous system, where the lack of developmental compensation may reveal phenotypes masked in constitutive knockouts. We propose that balancing the consideration of both physiological and pathological roles of tau and Aβ will be essential for the design of safe and effective AD therapeutics.
The origin of Aβ and tau
Aβ biogenesis
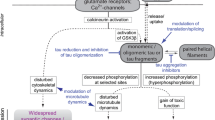
Amyloid precursor protein (APP) is encoded by the APP gene on chromosome 21 [84, 125, 257]. Aβ is produced by the sequential cleavage of APP by beta-site amyloid precursor protein cleaving enzyme 1 (BACE1) [265] and γ-secretase [55], which have recently been shown to form a multiprotease complex to maximise cleavage efficiency [151] (Fig. 1a). BACE1 cleaves APP at Asp1 or Glu11 of the Aβ sequence [265], after which the catalytic component of γ-secretase (presenilin) sequentially trims the resulting carboxy-terminal fragment at ε-, ζ-, and γ-cleavage sites, releasing the Aβ intracellular domain (AICD) and Aβ (between 37 and 49 amino acids in length) [292]. Mutations in presenilin, or environmental factors, consistently decrease the processivity of γ-secretase, resulting in fewer cuts per APP molecule and consequentially the release of longer Aβ peptides [42]. This amyloidogenic (or β) cleavage of APP is in direct competition with an alternative α-cleavage pathway, where α-secretase bisects APP in the middle of the putative Aβ protein, thus preventing Aβ production [70]. Under physiological conditions, Aβ1-40 (~ 90% of total Aβ) and Aβ1-42 (~ 5–10% of total Aβ) are the most abundant isoforms in humans [184]. Aβ1-40 is produced exclusively within the trans-Golgi network (TGN) and then packaged into secretory vesicles, whilst Aβ1-42 can be made in either the TGN or the endoplasmic reticulum [91]. Aβ monomers readily assemble to form higher order structures, from low-molecular-weight oligomers, to protofibrils and eventually to fibrils containing β-sheets (Fig. 1b), with longer isoforms of Aβ showing the greatest propensity to oligomerise and aggregate [34]. Increased production of Aβ1-42, at the expense of Aβ1-40 generation, is a common feature of both familial [42] and sporadic AD [101], with the increased aggregation of this peptide believed to be responsible for driving neurotoxicity [34].
a The two pathways through which APP can be cleaved. The non-amyloidogenic (α) pathway (left-hand side of diagram) involves the cleavage of APP by α-secretase, within the Aβ sequence, to form C-terminal fragment α (CTFα) and soluble APP α (sAPPα). γ-secretase then cleaves the resulting CTFα, releasing the Aβ intracellular domain (AICD) and the extracellular p3 fragment. The amyloidogenic (β) pathway (right-hand side of the diagram) involves the cleavage of APP by BACE1 to form CTFβ and sAPPβ. γ-secretase then cleaves the resulting CTFβ, releasing the AICD and Aβ. b Aβ monomers can assemble to form higher order structures, from oligomers, to protofibrils and eventually mature fibrils containing β-sheets which form the core component of amyloid plaques. Created with https://biorender.com/
Tau production
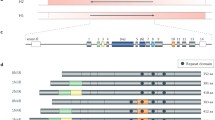
Tau is encoded by the MAPT (microtubule-associated protein tau) gene on chromosome 17 [189], which generates a total of 6 tau protein isoforms through alternative splicing of exons 2, 3, and 10 in the central nervous system (CNS) [94] (Fig. 2a). Inclusion of exon 10 produces tau with 4 microtubule-binding domains (4R), whilst omission of exon 10 excludes microtubule-binding domain R2 (3R). Similarly, tau can include (2 N or 1 N) or exclude (0 N) amino-terminal inserts through regulation of exons 2 and 3. In the peripheral nervous system (PNS), exons 4A, 6, and 8 can also be transcribed, resulting in the production of larger tau proteins [75]. Tau expression is developmentally regulated, with only 0N3R tau being expressed in the foetal brain, whilst all isoforms are expressed in adult humans [94]. However, adult mice and rats show almost exclusive expression of 4R tau [94]. In humans, there are two principle genetic haplotypes at the MAPT locus; H1, which is directly orientated (~ 75% of the Caucasian population), and H2, which has an inverted sequence (~ 25% of the Caucasian population) [269]. Interestingly, the H2 haplotype appears to be almost exclusively Caucasian in origin, with Central Asian populations having H2 allele frequencies of ~ 5% and African, East Asian, and Native American populations effectively lacking H2 expression [71]. Possession of the H1 versus H2 haplotype subtly alters the tau isoform expression profile [269]. Tau can undergo a vast array of post-translational modifications including phosphorylation, acetylation, ubiquitination, sumoylation, methylation, glycation, glycosylation, polyamination, nitration, isomerisation, and oxidation (reviewed in [94]). Tau monomers can aggregate to form oligomers and higher order fibrils (Fig. 2b). However, whilst Aβ can largely self-assemble, tau phosphorylation is believed to be important for its aggregation [9].
a Tau is encoded by the MAPT gene on chromosome 17. A total of 6 tau protein isoforms are generated via alternative splicing of exons 2, 3, and 10. Inclusion of exon 10 produces tau with 4 microtubule-binding (MTB) domains (4R), with omission of exon 10 producing tau with 3 MTB domains (3R). Tau can include (2 N or 1 N) or exclude (0 N) amino-terminal inserts through regulation of exons 2 and 3. Only 0N3R tau is expressed in the foetal human or mouse brain, with all 6 tau isoforms being expressed in adult humans. Adult mice and rats show almost exclusive expression of 4R tau. b Phosphorylated tau monomers can assemble to form oligomers, filaments (both straight and paired helical) and eventually tangles. N N-terminus, PRD proline-rich domain, MTB microtubule-binding domains, C C-terminus. Created with https://biorender.com/
Aβ and tau are expressed throughout the body
Tau and the key proteins required to produce Aβ [APP, BACE1, and components of γ-secretase (presenilin-1)] are expressed in a variety of tissues throughout the body (as reported by The Human Protein Atlas [262] (Fig. 3)). Whilst tau is predominantly found in brain and peripheral nerves, tau protein expression has been detected in diverse locations including salivary glands, breast tissue, cardiac myocytes, skeletal muscle, the pancreas, and kidneys [296]. Similarly, in addition to the brain, the key components of the Aβ-processing pathway [APP, BACE1, and presenilin-1 (PS1)] are co-expressed in the pancreas, appendix, gastrointestinal tract, and both male and female reproductive organs [297,298,299]. It is likely, therefore, that both Aβ and tau will serve functions beyond the CNS.
Aβ and tau are evolutionarily conserved
Both tau and Aβ show remarkable evolutionary conservation. An Aβ-like sequence has been reported in sea anemones, demonstrating that such peptides have been in existence from 540 to 630 million years ago [259]. The human Aβ sequence is over 95% homologous to that in other mammals, and over 90% in birds, reptiles, and amphibians [259]. Similarly, evidence of a MAPT-like gene has been found in lampreys, hagfish, and sharks, pinpointing an origin over 550 million years ago [247]. Such evolutionary conservation raises the possibility that these proteins are involved in key biological functions. Identifying these functions will provide a greater understanding of the pathogenesis of AD, as well as informing how Aβ- or tau-targeting treatments could impact physiology.
Regulation of microtubules: the primary physiological role of tau?
Tau binds to and regulates the structure of microtubules
Since the discovery of tau in 1975 [276], a plethora of research has focused on the role of tau at microtubules (reviewed in [10]). Microtubule deficits are common in AD and related disorders, with studies reporting axonal transport deficits [1], and defective microtubule assembly [115]. Tau binds tubulin via its microtubule-binding domains [141], with a single tau molecule crosslinking multiple tubulin dimers [6]. Original studies found that tau stabilises microtubules [62], reducing the frequency of catastrophes (sudden microtubule disintegration) [208]. Early studies found that tau reduces the concentration of tubulin required for polymerisation [276]. A mechanism for this process has recently been proposed, where conditions of macro-molecular crowding induce tau to form liquid-like drops [102]. Tubulin partitions into these drops, effectively raising its concentration to drive nucleation of microtubule formation [102]. Crucially, tau from AD post-mortem brain tissue fails to stimulate microtubule formation [115] and hyperphosphorylation of tau [115, 192], mutations within microtubule-binding sites [83], or C-terminal truncation [192], all greatly reduce tau’s microtubule-binding capacity. These findings have contributed to the established dogma that disease-associated hyperphosphorylation of tau promotes its dissociation from microtubules, reducing microtubule stability [9]. Whilst pseudo-phosphorylation of tau results in a fivefold decrease in the association rate of binding to microtubules, this surprisingly does not impact tau’s dissociation rate, raising the question of whether tau hyperphosphorylation occurs prior to, or following, microtubule detachment in disease [192]. In support of the latter hypothesis, inducing microtubule catastrophe via stathmin application results in unphosphorylated tau falling off the microtubule and subsequently being phosphorylated in the cytoplasm [181]. Thus, the role of microtubule-associated tau appears to be more complex than originally thought, with recent studies demonstrating its diverse, subtle, and sometimes contradictory functions.
Beyond microtubule stability: tau as a regulator of microtubule dynamics
Tau is preferentially expressed within the axon and there is agreement that tau concentration increases towards the distal, labile end [213]. As such, a role for regulating microtubule dynamics has been proposed. Indeed, tau knockdown in primary neurons results in a substantial drop in the labile microtubule mass with a corresponding increase in the stable domain [213]. Tau knockdown reduces neuronal outgrowth [150], impairs the repulsive response of the growth cone [22, 147], disrupts axonal extension [36], delays neuronal maturation [37, 54], and reduces microtubule density [96]. Tau also recruits end-binding proteins (EBs) to the stable microtubule bundle, preventing them from tracking to microtubule ends where they increase catastrophe frequency [217]. However, not all tau depletion studies report deficits in microtubule dynamics [261], with compensatory increases in other MAPs potentially masking relevant functions [164, 266]. Indeed, MAPT and MAP1B double knockouts have a high mortality rate, showing a synergistic disruption to growth cone dynamics, axonal elongation, and neuronal migration, resulting in defective axonal tract and neuronal layer formation [252]. Interestingly, an individual with frontotemporal dementia (FTD) was found to have a partial deletion of the MAPT gene, resulting in the production of truncated tau lacking the first microtubule-binding repeat [224]. This truncated tau exhibited dramatic reduction in microtubule-binding capability, but acquired the ability to sequester MAP1B, potentially mediating both loss-of-function and gain-of-function disruption to microtubule dynamics, similar to double knockout mice [224].
Tau regulates axonal transport
Many studies have sought to determine whether tau regulates axonal transport. Knockdown of 4R tau in human induced pluripotent stem cell (iPSC)-derived neurons increases the velocity of mitochondrial transport [15]. Additionally, young P301L knockin mice, which exhibit reduced tau-microtubule binding, show enhanced anterograde transport [1, 83]. It is hypothesised that tau may compete with motor proteins for tubulin-binding sites, and overexpression of tau has been reported to cause “traffic jams” [242] and induce kinesin dissociation from microtubules [61, 65, 233, 255]. Tau fibrils or oligomers can also inhibit axonal transport [124] and MAPT−/− neurons are resistant to Aβ-induced axonal transport deficits [268]. Recent work has demonstrated a potential mechanism for this under physiological conditions, with two studies describing “island” regions of concentrated tau protein along the axon [233, 255]. Upon reaching the island boundaries, kinesin-1 motor proteins dissociate instantaneously from the microtubules, whilst dynein slowly moves through [233, 255]. Such differential regulation of motor proteins could allow tau to regulate axonal transport and cargo delivery, processes that may be disrupted in disease. However, other studies report that neither tau knockout nor overexpression alters axonal transport dynamics [288]. A “kiss-and-hop” binding of tau to tubulin has been proposed as a mechanism, whereby tau remains associated with microtubules without clogging motor protein binding sites [118].
Tau protects microtubules from cleavage
An emerging role of tau is protecting microtubules from the microtubule-severing protein katanin [214, 233, 255, 287]. Recently described “tau islands” block katanin-tubulin binding, preventing breakdown of the microtubule lattice at these sites [233, 255]. Indeed, tau knockdown [214], or expression of pseudo-hyperphosphorylated tau [245], results in katanin-mediated cleavage, loss of microtubules, and reduced axon length in vitro. Tau depletion also increases neuronal branching [287], raising the hypothesis that the preferential expression of tau in the axon may maintain a non-branched structure, in contrast to highly branched dendrites, which show low tau expression [287]. Pathological tau mislocalisation may, therefore, render axonal microtubules vulnerable to inappropriate cleavage [233]. Interestingly, Aβ-induced tau mis-sorting permits recruitment of tubulin tyrosine ligase-like 6 (TTLL6) to dendritic microtubules, promoting spastin-mediated cleavage [289]. Tau location, therefore, appears vital for regulating its physiological versus pathological functions. Indeed, dendritic mis-sorting of tau also promotes aberrant clustering of Fyn, a key step in Aβ-mediated synaptotoxicity and spine collapse [116].
The future of therapeutics targeting microtubule (dys)function
Whilst microtubule-stabilising drugs, such as Taxol and Epothilone D, showed pre-clinical promise, replication of this success in humans is not yet forthcoming [286]. Forty five years of exploration of tau at the microtubule has transformed understanding from tau being a simple “stabiliser”, to reveal a diverse array of physiological and pathological functions [10]. With development of tau-targeting therapies becoming increasingly common, careful maintenance of physiological tau at the axon, whilst also preventing mis-sorting and pathological aggregation, will likely be crucial for therapeutic success. Interestingly, a recent study reported that Aβ-mediated dendritic simplification requires microtubule stabilisation by unphosphorylated dendritic tau [85]. This finding raises concerns that reducing tau phosphorylation, a common goal of tau-targeting treatments, may negatively impact neuronal connectivity in some circumstances, highlighting the complexity of untangling physiological from pathological modifications. Therefore, focus on other physiological functions of tau or Aβ may reveal more promising therapeutic targets.
Physiological roles at the synapse
Synapse loss is the strongest pathological correlate of cognitive decline in AD [56, 258], so protecting these vital structures is a key therapeutic goal. Tau and Aβ are prime suspects for causing synaptic damage, with toxic species reported to accumulate at synapses [132, 250], disrupt key synaptic machinery [293], induce spine collapse [274], and target synapses for microglia-mediated pruning [52, 106]. Whilst toxic tau and Aβ are undoubtedly involved in AD pathology, there is growing evidence that these proteins play key physiological roles at the synapse that could be lost, or hijacked, to contribute to disease. Potential loss-of-function at the synapse should be carefully considered when designing tau- or Aβ-targeting therapeutics to avoid exacerbating, or introducing new, synaptic pathology.
Physiological concentrations of Aβ enhance LTP
Studies of synapse function often use long-term potentiation (LTP), an indicator of synapse strengthening, and long-term depression (LTD), an indicator of synaptic weakening, as electrophysiological correlates of learning and memory [14]. Pathological concentrations of Aβ applied to hippocampal slices disrupt LTP [270], but physiological concentrations may, in fact, be required for this process [210] (Fig. 4). A biphasic, or hormetic, role of soluble Aβ in regulating LTP has been proposed, whereby low (picomolar) concentrations of Aβ enhance LTP, whilst high (nanomolar) concentrations suppress LTP [92, 99, 185, 210, 211]. Such experiments highlight a potential role for endogenous Aβ in regulating memory formation. Indeed, the extracellular concentration of Aβ increases after neuronal stimulation [123, 253] and interstitial fluid Aβ concentration positively correlates with neuronal activity in human brain [29]. Interestingly, both APP knockout [53] and BACE1 knockout [139, 154, 272, 273] in vivo induce cognitive deficits and impair LTP. Wild-type mice given BACE1 inhibitors also show a dose-dependent suppression of LTP and impaired cognitive performance [74]. Treatment of wild-type slices with the anti-Aβ antibody 4G8 prevents LTP formation [185, 210] with LTP restored by application of picomolar oligomeric Aβ1-42 [210]. In vivo, hippocampal infusion of 4G8 [81, 185, 210] or siRNA to APP [185, 210] abolishes short-term memory in contextual fear conditioning [81, 185, 210] or the Morris Water Maze (MWM) [210]. Infusion of picomolar Aβ rescues this effect [81, 210], whilst Aβ-infusion into naive mice enhances reference and contextual fear memory [81, 210, 211]. A potential hormetic role of Aβ raises the possibility that physiological, learning-mediated Aβ production throughout life could eventually result in accumulation of Aβ to a toxic level, especially if clearance mechanisms fail. Indeed, in humans, brain regions in the default mode network that show high levels of neuronal activity in young adults closely correlate with regions most heavily burdened by amyloid in AD later in life [32].
Schematic representation of the hormetic responses to tau and Aß concentration. There is an optimal concentration of tau or Aβ for a number of physiological functions. Too little protein (or loss of function modifications) or too much protein (or gain of function modifications) can both disrupt normal function. Effectively rescuing loss of function or preventing gain of function to maintain optimal physiological conditions should be the ultimate goal of therapeutics. Created with https://biorender.com/
Tau in LTP, LTD, and memory
Like Aβ, tau expression and secretion also increases following neuronal activity [131, 207], and studies in MAPT−/− mice have sought to explore the role of tau in synaptic function. Phenotypes of MAPT−/− mice vary, with findings differing depending on the model used, genetic background [146], cleanliness of the animal unit [186], diet [164], and the age of the animals when studied. Some studies do not report cognitive or synaptic deficits in MAPT−/− mice [113, 146, 186, 254], and reports that there is compensatory upregulation of other MAPs highlight that developmental compensation could mask relevant effects [164]. Ma et al. found that 8-month old MAPT−/− mice had no cognitive deficits, but displayed significant MAP1A upregulation. At 19 months old, however, compensatory MAP levels fell, and extensive synapse loss and cognitive deficits became apparent [164]. A recent study showed that acute tau knockdown in adult mice using viral shRNA resulted in reduced spine density, loss of synaptic proteins, and significant spatial memory impairments in the absence of compensatory MAP upregulation [266]. Despite potential compensatory confounds, different groups have reported age-dependent cognitive deficits in MAPT−/− mice in contextual fear conditioning [3], Y-maze [146], MWM [164], and reversal learning tests [218]. Whilst one study found a severe LTP deficit in tau knockouts [3], LTD deficits are more commonly reported [128, 218]. Tau’s role in LTD appears to depend on its phosphorylation at serine 396 permitting AMPA receptor internalisation [218]. Crucially, a number of studies have reported human genetic cases of FTD [199, 294] or intellectual disability [172, 232, 263] in which tau levels are drastically reduced compared to age-matched controls. Reduced soluble tau has also been reported in normal ageing [187], Parkinson’s disease (PD) [145], and AD [137, 191] (potentially due to sequestration of tau into NFTs). Together, this raises the possibility that loss of normal tau function may be partly responsible for cognitive and synaptic deficits in disease. Tau-targeting therapeutics should, therefore, be carefully managed to avoid disrupting physiological tau at the synapse.
Regulating neuronal hyperexcitability: could tau and Aβ act at opposite ends of the spectrum?
A common feature of many neurodegenerative and neurodevelopmental disorders is the prevalence of seizures. Up to 22% of individuals with AD experience at least one seizure [178], whilst epilepsy is diagnosed in around 20% of individuals with autism spectrum disorder (ASD) [18]. Tau appears to be important for permitting seizure activity, and there is strong evidence that MAPT−/− mice [148], or mice treated with tau antisense oligonucleotides [59] are resistant to pentylenetetrazol-induced seizures. Crossing MAPT−/− mice with genetic models of epilepsy [105], AD [219] and ASD [249] can rescue hyperexcitability and spontaneous epileptiform activity. As such, a role for tau in promoting or regulating neuronal excitability seems likely. It has recently been shown that hyperexcitation increases tau translation [131] and that tau translocation to the nucleus regulates the expression of the glutamatergic transporter protein, VGLUT1 [234]. Interestingly, MAPT−/− neurons lack extrasynaptic NMDA currents that, whilst their physiological role is under debate, mediate excitotoxicity under a number of conditions [196]. Tau deficiency may also impact basal synaptic activity; one study reported that tau knockout neurons were hyperpolarised compared to wild-type cells [197], and a recent study found that tau knockout impaired basal neurotransmission in APP transgenic mice [209]. Lowering of tau levels could, therefore, be beneficial under conditions of hyperexcitability, but this must be carefully balanced against the risk of depressing normal neuronal activity.
When considering the impact of Aβ on neuronal excitability, there are seemingly contradictory findings, potentially explainable through the aforementioned hormetic role of Aβ (Fig. 4). Whilst low levels of Aβ can increase dendritic spine density [194], increase the number of docked vesicles [92], enhance glutamate release, promote excitotoxicity, and disrupt calcium homeostasis (particularly in early stages of disease) [7, 35, 225], Aβ production after synaptic activity could also act via negative feedback to prevent hyperactivity [123]. Indeed, Aβ can induce spine collapse and synapse loss [231, 274], increase the proportion of silent neurons [35], and disrupt neurotransmitter release via depletion of presynaptic PIP2 [99]. However, untangling the specific role of Aβ versus APP, alternative APP-processing products or BACE1 has proven difficult. Both APP−/− [243] and BACE1−/− [103, 112, 130] mice fail to produce Aβ and show hypersensitivity to spontaneous and induced seizures. BACE1, however, cleaves a variety of proteins important for normal neuronal function, including seizure protein 6 [206]. Notably, conditional BACE1 knockout in adult mice does not induce epileptiform activity [264], suggesting BACE1 or Aβ may play independent roles in the developing versus adult brain. To add further complexity, overexpression of APP, not Aβ, is responsible for hypersynchronous activity in some AD mouse models [26]. Therefore, clarification of the roles of Aβ, APP, and BACE1 will be essential to ensure balanced synaptic activity when therapeutically targeting amyloid dysregulation.
Neurogenesis, synaptogenesis, and structural plasticity
The formation of new neurons and synapses is an important process both throughout development and in the adult nervous system. Early studies found that low concentrations of Aβ promote the survival of primary neurons [278] and have a neurogenic effect on neural progenitor cells [158]. Aβ1-42 also stimulates neurogenesis of subventricular zone precursors in vivo, raising the hypothesis that the early overstimulation of neurogenesis in AD may result in depletion of the stem cell pool and a decline in basal neurogenesis later in life [238]. Despite showing neurogenic properties, Aβ is often considered an antagonist to the formation of new synapses. Indeed, high concentrations of oligomeric Aβ can induce spine collapse [7, 231, 274], and synapse loss has been found to correlate with increased intraneuronal APP [295], plaque-proximal extracellular Aβ [132, 295], and accumulation of intraneuronal Aβ [97, 253]. However, long exposure to picomolar Aβ has also been found to increase the spine density in slice cultures [194]. Similarly, APP knockout in hippocampal neurons reduces neuronal branching and synapse formation [239], and APP−/− mice show a profound loss of synaptic proteins [53, 228], although loss of sAPPα (a non-amyloidogenic product of APP cleavage) may be a key contributor to this phenotype (reviewed in [47]). BACE1 has also been shown to play a role in normal synapse development, with BACE1−/− mice showing a developmental hearing impairment caused by aberrant synaptic organisation in the cochlea [60]. Interestingly, adult wild-type mice treated with BACE1 inhibitors also show a reduction in dendritic spine density and formation [74], whilst BACE1 inhibitor treatment of APP/PS1 mice (which produce excess Aβ) slowed the rate of synapse loss around plaques [204]. Taken together, it once again seems likely that there is an optimal concentration of Aβ to maintain synapses, which must be considered when therapeutically targeting Aβ (Fig. 4).
Tau may also play a role in neuronal development and synaptogenesis. In vitro, stimulation of hippocampal neurons with brain-derived neurotrophic factor (BDNF) normally increases tau expression and spine growth, but tau-shRNA treatment significantly decreases baseline spine numbers and blocks the pro-synaptic response to BDNF [44]. In adult mice, tau-shRNA treatment reduced apical and basal dendrite density, supporting a role for tau in spine formation or maintenance [266]. In MAPT−/− mice, new-born granule neurons in the dentate gyrus fail to migrate normally [78, 227], show reduced dendritic length, and have disrupted postsynaptic density (PSD) and mossy fiber terminal formation [197]. Tau also mediates the pro-neurogenic effect of environmental enrichment on adult hippocampal neurogenesis and synaptic integration [197]. Other studies have reported impaired neurogenesis in MAPT−/− mice [107], potentially explaining the reduced brain weight reported in some strains [145, 146]. An anti-aggregant tau mouse model shows increased neurogenesis and hippocampal volume [120], whilst tauopathy models frequently show deficits in hippocampal neurogenesis [134], potentially highlighting tau aggregation as a loss-of-function mechanism in this context. Tau knockdown also delays neuronal maturation in primary neurons [54] and induces transcriptional repression of neuronal genes [11], indicative of a potential role of tau in promoting neuronal differentiation. Some studies, however, contradict these findings, reporting increased neurogenesis in tau-deficient animals [50]. Further exploration of the role of tau in adult neurogenesis, and whether this translates to humans, is, therefore, required.
Regulating behaviour
Tau, hyperactivity, anxiety, and sleep
In addition to cognitive deficits, MAPT−/− mice show evidence of hyperactivity, as measured by spontaneous locomotion in an open field test [23, 114], and substantially increased rearing behaviour [148]. MAPT−/− mice also spend significantly less time in the open arms of elevated Z-mazes and keep to the periphery of open field arenas, indicative of increased anxiety [86]. Tau may also help to regulate circadian behaviours, with MAPT−/− mice [41] or Drosophila [8], showing major abnormalities in the sleep–wake cycle, including increased wakefulness and disruption to normal circadian activities. Sleep disturbances are commonly reported in ageing and neurodegenerative disorders [281], so understanding how tau alterations impact sleep may be clinically relevant. Interestingly, tauopathy models often show disturbed sleep patterns [122] and hyperactivity [122, 205] phenotypes, raising the possibility that tau mutations could, for these behaviours, mimic the effect of tau depletion through loss of function.
Tau and the motor system
Another common feature of MAPT−/− mice is the appearance of FTD-P17-like motor dysfunction, suggesting that tau loss of function could be partly responsible for Parkinsonism in these individuals [145]. Notably, soluble tau levels in the substantia nigra of the brains of individuals with PD are 44% lower than those observed in age-matched controls, indicating that loss of normal tau may contribute to motor deficits [145]. In mouse studies, a number of groups have reported significant impairment in balance beam or rotarod performance in tau knockouts [114, 145, 146, 157, 164, 186], mice lacking 4R tau [93], and mice treated with tau-shRNA [266]. Additionally, changes in gait [146], reduced locomotion [145, 146], and muscle weakness [114] have been recorded, and many MAPT−/− models also show loss of dopaminergic neurons [145, 146, 164]. Interestingly, treatment of MAPT−/− mice with L-DOPA rescued motor phenotypes in some models [145, 146], but another study reported a dopamine-independent motor deficit [186]. A recent study postulated that the age-dependent motor deficits observed in their MAPT−/− model were due to hypomyelination and degeneration of the sciatic nerve (discussed below), raising further questions about the effect of tau loss of function in the peripheral versus central nervous systems [157]. Interestingly, motor deficits are common in tau-overexpressing transgenic mice [4, 77], and it has been reported that whilst modest overexpression of FTD-P17 mutant tau can improve motor performance in young animals, this progresses to severe paraparesis in later life [183]. In humans, the MAPT H1/H1 genotype is also associated with increased risk of neurodegenerative diseases affecting the motor system, such as corticobasal degeneration (CBD) and progressive supranuclear palsy (PSP) [108]. Taken together, it seems likely that, in addition to mutations potentially disrupting physiological roles of tau, changes in tau concentration may have a hormetic effect on motor function (Fig. 4). Whilst individuals with AD can develop motor symptoms [155], this is not considered the primary deficit, indicative that the location of tau changes within the brain (e.g., hippocampus versus substantia nigra or motor cortex) and peripheral nervous system is likely an important determinant of symptoms.
Regulation of myelination
Tau is important for normal myelination
Whilst many studies focus on neuronal damage, white matter hyperintensities (evidence of demyelination) are commonly reported in the early stages of AD and other tauopathies and correlate with tau burden [173]. A recent study describes human familial globular glial tauopathy, linked to MAPT mutations, that result in extensive tau deposits in oligodendrocytes [73]. Affected individuals show severe demyelination, defective myelin synthesis, and concomitant axonal damage [73]. Coiled bodies of tau in oligodendrocytes and demyelination are also common features of other primary tauopathies such as PSP and CBD [291]. Mouse models of tauopathy frequently demonstrate deficits in myelination, with evidence of filamentous tau inclusions developing in oligodendrocytes [149], resulting in defective myelination of the perforant path [117], spinal cord [149], and sciatic nerve [179]. Tauopathy-induced myelination deficits coincide with increased nerve conduction latency [117], cognitive decline [117], and motor impairments [179]. The mechanism by which tau pathology leads to deficits in myelination has yet to be fully elucidated, but there is evidence that this could represent a loss of normal tau function. Tau is found within oligodendrocytes and Schwann cells under physiological conditions and is upregulated during developmental myelination [159]. siRNA-mediated knockdown of tau impairs oligodendrocyte process outgrowth, reduces myelin basic protein (MBP) expression, and impairs contact with axons in myelinating co-cultures [230]. Oligodendrocyte process outgrowth depends on the recruitment of tau and tubulin to activated Fyn-kinase rafts, with disruption of tau-microtubule binding reducing oligodendrocyte process number and length [129]. Expression of an inducible, truncated tau (which retains the Fyn-binding domain but lacks microtubule-binding capability) in oligodendrocytes induced demyelination and gait abnormalities in mice [160]. MAPT−/− mice also show age-dependent degeneration of myelinated fibers, reduced nerve conduction, and progressive hypomyelination [157, 237], resulting in motor [157] and nociceptive [237] impairments. Tau knockdown also restricts recovery after sciatic nerve damage, with mice showing defective myelin debris clearance and severely impaired Schwann cell migration and differentiation [285]. Similarly, MAPT−/− mice showed a worse clinical outcome after experimental autoimmune encephalomyelitis (EAE) (a model of demyelinating disease) [277]. Taken together, it seems likely that tau plays a key role in forming, maintaining, and repairing myelin, potentially via the regulation of microtubule dynamics [129]. Tau hyperphosphorylation may disrupt this key function in disease, contributing to the commonly observed white matter pathology. Whether myelination deficits will become a problem for tau-targeting therapeutics remains to be seen, but caution may be required to ensure normal oligodendrocyte and Schwann cell function is maintained.
Aβ and its cleavage enzymes may regulate myelination
A recent study reports that low concentrations of Aβ oligomers can enhance oligodendrocyte survival in vitro [215]. Aβ peptides also induced translation of MBP, promoted oligodendrocyte differentiation, and improved remyelination in demyelinated cerebellar slices [215]. BACE1−/− mice show delayed myelination and reduced myelin thickness in the PNS and CNS [110, 280], as well as impaired remyelination of peripheral nerves after injury [109, 111]. However, BACE1−/− phenotypes may be Aβ-independent, relying instead on the cleavage of neuregulins [109], highlighting a potential off-target effect of lowering Aβ through BACE1 inhibition. Interestingly, BACE1, neuregulin-1, and Aβ expression increase during myelin repair following ischaemic stroke, suggesting a potential role in the myelin repair process [190]. However, oligomeric Aβ1-42 can also reduce oligodendrocyte number and induce motor deficits when injected intracerebroventricularly in mice [290]. Interestingly, a recent study has found that the secreted metalloprotease ADAMTS4, located exclusively in oligodendrocytes in adult mice, is responsible for the production of highly amyloidogenic, N-truncated, Aβ4-x peptides [271]. Further studies will, therefore, be required to elucidate the role of Aβ peptides and their cleavage enzymes in oligodendrocytes, and to determine whether Aβ-targeting therapies will be beneficial or detrimental in resolving white matter pathology in disease. Once again, it seems likely that a balance between preventing toxicity and maintaining physiological functions will be required.
Aβ regulates vasculature
Angiogenesis and Aβ: a question of balance?
There is mounting evidence that Aβ plays important roles in regulating vasculature. Studies in post-mortem human brains have found evidence for increased angiogenesis in AD [21, 58], with one study finding that vascular density in the hippocampus positively correlated with Aβ load [58]. Conversely, other studies have reported reduced vascularisation in AD brains [76]. Studies in AD mice found evidence for a dual-staged response to rising Aβ, with young animals showing increased vascular density compared to wild-type littermates, with reversal of the trend in old mice [21]. In vitro, Aβ can inhibit endothelial cell capillary formation in a dose-dependent manner and stimulates capillary degeneration at high concentrations [201]. At low concentrations, however, Aβ has been found to promote endothelial cell proliferation [27], induce formation of capillary-like structures [27], and increase vessel density in brain slice cultures [64]. In vivo studies using chick [27] or zebrafish embryos [40] and adult zebrafish retinas [51] find that Aβ peptides increase capillary density and induce formation of sprouting tip cells. BACE1−/− mice also show a significant reduction in retinal vascular density [38] and APP-deficient zebrafish, or zebrafish treated with a BACE1 inhibitor, have shorter hindbrain vessels with fewer cerebrovascular branches [163]. Crucially, application of human Aβ rescued the vascular phenotype in both APP-deficient and BACE1 inhibitor-treated zebrafish [163], highlighting a primary role of endogenous Aβ in maintaining normal capillary density.
Whilst low levels of Aβ seem important for maintaining physiological vascularisation, increasing levels of Aβ in early AD have been shown to promote pathological angiogenesis, resulting in excessive vascularisation and disturbance to normal blood flow [21, 58, 64]. Excessive cleavage of APP, or direct inhibitory action of Aβ, may overwhelm or inhibit the activity of γ-secretase, thus reducing its availability to cleave Notch proteins, known angiogenesis inhibitors [27, 64]. Indeed, γ-secretase inhibitor treatment increases angiogenesis and vascularisation in a range of model systems [40]. Lowering Aβ levels, through immunisation against Aβ [20] or BACE1 inhibition [64], restores normal vascular patterns in AD models. Indeed, a meta-analysis of clinical trials reports that people with AD receiving immunisations against Aβ1-42, show a significant reduction of endothelial cells and vascular density [20]. In another example of hormesis, either too little or too much Aβ may result in pathological alterations to capillary density (Fig. 4). Carefully controlling Aβ concentration will be important to restore and maintain physiological angiogenesis in AD.
Aβ as a “vascular plug”
Clinical trials targeting Aβ have unintentionally provided evidence for a further role of Aβ in the vascular system: repairing leaks in the blood–brain barrier (BBB) [30]. A side effect of a number of active or passive anti-Aβ immunotherapies has been the appearance of microhaemorrhages and brain oedema [203]. This pattern of pathology, visible by MRI, has been termed “Amyloid-Related Imaging Abnormalities” (ARIA) and has become synonymous with Aβ immunisation [240]. A meta-analysis of 14 Aβ-targeting clinical trials reported a fivefold increase in the incidence of ARIA in treated versus placebo AD groups, with many trials showing a dose-dependent effect and increased incidence in APOE4 carriers [203]. Aβ immunisation in AD mouse models [24] and aged mouse lemurs [121] can also induce ARIA-like cerebral microbleeds.
At present, it is not fully understood why removal of Aβ causes haemorrhages. Deposition of amyloid in blood vessels [cerebral amyloid angiopathy (CAA)] is a common feature of AD [166]. One possibility is that sudden removal of amyloid from blood vessels could compromise vascular integrity, as amyloid may have completely replaced the vessel wall in some instances (grade 2 CAA) [166]. Alternatively, a number of groups have proposed a relationship between Aβ and blood clotting. Platelets are the primary source of Aβ within the blood [43] and Aβ can induce aggregation of platelets [69]. It has been postulated that Aβ could play a physiological role as a vascular sealant, which could become overactivated with age and disease [30]. The expression of APP and Aβ rises in response to haemorrhagic damage, such as induction of microhaemorrhages [80] and chronic hypertension [33]. APP−/− or BACE−/− mice also show increased mortality after ischaemic injury, with severe deficits in reactive blood flow compared to wild-type controls [133]. Taken together, these findings add weight to the hypothesis that Aβ could serve a crucial role in vascular responses to injury, potentially explaining the appearance of ARIA after Aβ-immunotherapy. Conversely, high levels of Aβ can increase BBB permeability, potentially via reducing levels of tight junction proteins [127]. Interestingly, increasing BBB permeability promoted clearance of Aβ from the brain and improved cognition in a mouse model of AD, indicative of a physiological negative feedback mechanism [127]. Once again, this demonstrates the delicate balance between Aβ acting to support physiological versus pathological processes that must be considered to design safe, effective therapeutics.
Response to injury
Tau and Aβ increase after injury: a protective or pathological response?
Increasing evidence demonstrates that the levels of both tau and Aβ proteins increase following stroke [190], spinal cord injury (SCI) [195, 212] and traumatic brain injury (TBI) [282]. TBI promotes tau aggregation and spreading [67], with levels of tau pathology detected via PET correlating with poor long-term neuropsychiatric outcomes [251]. Whilst increases in tau often correlate with poorer outcome after injury [251], increased soluble Aβ has been shown to correlate with improved neurological status in individuals with a TBI [29]. Similarly, the formation of Aβ deposits in demyelinating lesions in people with multiple sclerosis (MS) has been proposed as a potentially protective response to axonal injury [89]. This raises the question of whether increases in tau and Aβ after injury serve to promote recovery, or whether they are involved in a detrimental pathological cascade.
Aβ may promote recovery after brain injury
Attempts to clarify the function of increased Aβ after injury have produced conflicting results and it is often difficult to separate specific effects of Aβ from functions of APP, which is known to be upregulated in axons after injury and may have protective functions [100]. Whilst some groups found that BACE1 knockout or inhibition improves recovery after sciatic nerve injury [72] or TBI [153], others report that BACE1−/− mice have impaired remyelination after sciatic nerve lesion [109, 111] and worse functional outcome after SCI [195] or TBI [168]. Interestingly, both BACE1−/− and APP−/− mice have an increased risk of mortality following cerebral ischaemia, indicating that this is likely a consequence of Aβ loss [133]. Mannix et al. found that following controlled cortical impact (CCI), functional outcome is worse in BACE1−/− mice compared to wild-type mice [168]. A follow-up study demonstrated that motor function (but not spatial memory or histopathology) could be improved by administration of Aβ1-40 to BACE1−/− mice after CCI, demonstrating a potential role for Aβ in recovery [167]. In the same study, administration of Aβ to injured wild-type animals worsened outcome, demonstrating a hormetic role for Aβ [167] (Fig. 4). Grant et al. also showed that peripheral administration of Aβ could reduce paralysis and demyelination in a mouse model of EAE, providing further evidence of a role for Aβ in promoting recovery after injury [89].
The effect of tau depends on the type of injury induced
Studies exploring the role of tau after injury have also been contradictory. MAPT−/− mice suffer worse functional outcome after sciatic nerve injury [285] and EAE [277], reminiscent of tau regulating physiological myelination (discussed earlier). Several studies, however, report that MAPT−/− mice are resistant to some functional and cognitive deficits after TBI, although this depends on whether the injury was repetitive [45] and whether short-term or long-term outcomes were measured [256]. A study by Bi et al. found that following experimental stroke, MAPT−/− mice were protected from neurological deficits and excitotoxic brain damage [19]. The authors suggested a mechanism for this effect whereby tau normally mediates excitotoxic Ras/ERK signalling by regulating SynGAP1 postsynaptic compartmentalisation [19]. Whilst further experiments are required in a range of injury models, it seems likely that the positive versus negative effects of targeting tau will depend largely on the type of damage induced and the normal recovery mechanisms required. An apparent role for tau in myelin repair may mean that individuals with AD who have a history of MS, for example, could be at risk of worse outcome after receiving tau-lowering therapies. Similarly, Aβ-lowering therapies may increase the risk of brain damage in individuals who go on to suffer a TBI, which may be a risk in individuals who frequently suffer falls [260]. Therefore, patient history could be key in assessing the risk for negative outcomes associated with comorbidities, prior to the administration of tau- or Aβ-targeting therapeutics.
Mitochondria and oxidative stress
Mitochondrial dysfunction is a key component of AD pathology
Mitochondrial dysfunction is an early and important pathogenic feature of AD [98], and both tau and Aβ have been shown to separately and synergistically affect mitochondrial function [66]. Whilst most studies have examined the pathological effects of tau and Aβ on mitochondria, there is some evidence that these proteins may also have physiological roles.
Aβ and tau deposition: cause of, or response to, oxidative damage?
Many studies have found an association between mitochondrial Aβ deposition and oxidative stress [66, 193]. However, the directionality of the observed events, i.e., whether Aβ accumulation is a cause of, or response to, oxidative stress, has proven difficult to ascertain. Somewhat counterintuitively, whilst oxidative stress is an early feature of AD, oxidative damage decreases alongside increased Aβ deposition during AD progression [193]. Notably, neurons containing an NFT show a 40–56% decrease in oxidised nucleosides compared to non-tangle-bearing neurons [193], leading to the proposal that Aβ and tau may have antioxidant properties [235]. Interestingly, a gene called saitohin, located in the intron downstream of exon 9 within the MAPT gene, interacts with peroxiredoxin 6, an antioxidant enzyme that protects cells from oxidative damage [79]. Whilst further research is required to explore the interaction of saitohin with tau, it seems likely that gene-level changes to MAPT may also impact the function of saitohin. Therefore, caution may be required when utilising tau- or Aβ-targeting therapies, to avoid potential exacerbation of oxidative damage.
Tau as a regulator of mitochondrial mobility and health?
Tau has also been proposed to regulate mitochondrial function. Sapir et al. found that tau knockdown reduced mitochondrial mobility and increased the number of abnormal mitochondria [227]. A recent study reports that tau localises to the outer mitochondrial membrane under physiological conditions, proposing a role for tau in regulating mitochondrial association, and calcium transfer, with the endoplasmic reticulum [48]. However, overexpression of tau can also impair mitochondrial transport [65] and mouse models of tauopathy demonstrate deficits in mitochondrial distribution [135]. These seemingly contradictory results require further exploration and it seems likely that tau expression levels, post-translational modifications, developmental stage, and potential compensation from other MAPs will all impact whether tau serves a physiological or pathological role at the mitochondria.
Aβ may function as an antimicrobial peptide
The antimicrobial protection/infection hypotheses of AD
In 2002, Robinson and Bishop proposed that Aβ is normally produced to “bind toxic solutes” with the formation of amyloid plaques being “an efficient means of presenting these toxins to phagocytes” [220]. Since then, a number of groups have built upon the idea of amyloidosis as an innate immune response and have proposed that increased Aβ deposition, caused by continuous activation of this pathway through recurrent, chronic infection, may lead to the development of AD [182].
Aβ rises after infection and is associated with pathogens in the CNS
A number of studies have shown that infection with a range of pathogens, including Herpes simplex virus-1 (HSV-1), Chlamydia pneumoniae and Borrelia burgdorferi, can increase production and deposition of Aβ in vitro and in vivo, where microbial DNA can be found associated with amyloid plaques (reviewed in [87]). Interestingly, a post-mortem study of individuals who had died from HIV/AIDS found that over half of them possessed extensive accumulation of Aβ in the brain, despite their young age (average age of death was 43 years old) [90]. Interestingly, treatment of HSV-1-infected cell cultures with the antiviral agent Acyclovir lowers intracellular Aβ accumulation and normalises BACE1 expression, leading to the proposal that antiviral therapies may be beneficial for the treatment of AD [162]. It is important to note, however, that human studies linking infections and AD are mostly correlational in nature. Whilst there is considerable evidence for a role of neuroinflammation in the progression of AD [106], it is possible that the increase in microbes in the AD brain is a response to rather than a cause of AD pathology. Breakdown of the BBB is common during neurodegenerative disease [248], and this could permit invasion of microbes circulating in the periphery, especially viruses, such as HSV, that are endemic in the population [283].
Aβ has antimicrobial activity
The increased expression of Aβ after infection is proposed to be an innate immune response, and there is evidence that Aβ can act as an antimicrobial peptide (AMP) (reviewed in [87]). Soscia et al. found that Aβ exhibits antimicrobial action of equal or greater potency than LL-37 (a human antimicrobial peptide) against eight common microbes [236]. Application of Aβ also decreases the infectivity of HSV-1 [162] in cell lines, and reduces the growth of Candida albicans, Gram-negative, and Gram-positive bacteria [138, 236] in culture. In vivo, Kumar et al. found that Aβ overexpression significantly increases survival in 5xFAD mice infected with S. Typhimurium, and in C. elegans infected with C. albicans and S. Typhimurium [138]. The authors suggest that Aβ acts as an AMP by agglutinating and trapping microbes via the binding of its heparin-binding domain to carbohydrates in microbe cell walls [138]. Alternatively, Aβ may form cation channels in cell membranes, inducing cell death via calcium dyshomeostasis [126]. Interestingly, APP−/− mice show a trend for increased mortality after infection [138] and a common side effect of Aβ-targeting therapies in clinical trials has been increased incidence of infections [87], although BBB disruption caused by removal of vascular amyloid could also explain this increased vulnerability [240].
Regulation of iron homeostasis
Iron homeostasis may be disrupted in neurodegenerative disorders
A number of groups have postulated that iron dyshomeostasis could contribute to AD and other neurodegenerative diseases [140], with iron accumulation resulting in cellular oxidative damage, dysfunction, and death via ferroptosis, an iron-dependent form of regulated necrosis [140]. It remains unknown whether iron dyshomeostasis is a cause, or consequence, of neurodegenerative pathology, but there is evidence that tau and APP may play physiological roles in regulating cellular iron transport.
Tau and APP play a role in physiological iron transport
Whilst the role of Aβ in regulating iron homeostasis is unclear, APP has been proposed to have iron-export ferroxidase activity and interacts with, and stabilises, a major iron transport protein, ferroportin [16, 63]. Indeed, APP−/− neurons retain more iron [63] and APP−/− mice show vulnerability to oxidative damage from dietary iron [63] and exhibit exaggerated age-dependent iron accumulation in the brain and liver [16]. Tau may also regulate iron transport, likely through mediating transport of APP to ferroportin [145]. Lei et al. found that MAPT−/− mice exhibit age-dependent iron accumulation associated with neurodegeneration, cognitive deficits, and parkinsonian-like motor deficits [145]. These deficits were rescued by treatment of aged MAPT−/− mice with the iron chelator clioquinol [144]. Interestingly, they also found that tau levels were reduced by ~ 40% in the substantia nigra of individuals with PD [145], and the authors hypothesise that loss of tau may contribute to the extensive iron accumulation reported in this brain region in PD. The same group reported that lithium-mediated reduction of tau in wild-type mice, or primary cortical neurons, results in iron accumulation in the brain and reduced cellular iron efflux [143]. Taken together, the effects of tau-lowering therapeutics on iron homeostasis should be carefully considered when targeting tau in AD. As iron chelation has been shown to be beneficial in a MAPT−/− mouse model [144], potentially detrimental side effects may be avoided by a combinatorial approach targeting both tau and iron dyshomeostasis.
The role of tau and Aβ in the nucleus
Tau is located at the nucleus and interacts with oligonucleotides
Whilst the majority of tau protein is located in the cytoplasm, there is clear evidence for nuclear association of tau in cell lines [156, 165, 234], primary neurons [11], and in mouse [267] and human [68, 216] brain tissue. Nuclear tau is mostly unphosphorylated [246] and is often localised to the nucleolar border, co-localising with constitutive heterochromatin [169] and ribosomal DNA (rDNA) [226]. In vitro, tau readily binds RNA [31] and DNA [39, 275]. Tau binds the minor groove of DNA, in a manner analogous to histones, via its proline-rich domain and microtubule-binding domain R2 [39, 275]. Tau’s ability to bind nucleic acids is disrupted by hyperphosphorylation [161], raising the possibility that such changes during disease may result in loss of function.
Tau protects DNA from damage
Neurons continuously face the harmful effects of oxidative stress and evidence points to a key role for tau in preventing DNA damage and promoting repair [267]. Cellular stress, induced by heat shock or reactive oxygen species (ROS), results in dephosphorylation of tau, translocation to the nucleus [246, 267] and increases the capacity for tau to bind DNA [246]. In vitro, tau protects DNA from thermal denaturation, DNAse digestion, and ROS-mediated damage [39, 275]. Hyperphosphorylation prevents tau from binding DNA, resulting in DNA breakage and deficient repair under experimental stress conditions [161]. Whilst primary neuronal cultures from wild-type mice are resistant to hyperthermic conditions, DNA breaks caused by extensive heat shock become evident in tau-deficient neurons, damage which can be rescued by overexpression of human tau targeted to the nucleus [246]. In vivo, MAPT−/− mice show increased DNA fragmentation under physiological conditions and are highly susceptible to DNA breakage after hyperthermic stress [267]. MAPT−/− mice also show delayed repair of double-strand breaks after heat shock which was especially evident in the CA1 hippocampal subfield [267]. Caution may, therefore, be required to ensure that tau-lowering therapies do not increase neuronal susceptibility to DNA damage.
Tau maintains chromosomal stability
Cells from individuals with MAPT mutations consistently show chromosomal aberrations, including breakages, gaps, aneuploidies, and translocations [222]. Interestingly, knocking out one or both copies of tau in murine splenocytes resulted in a marked increase in aneuploidy, indicating that MAPT mutations could induce dysfunction via loss of function, potentially through disruption of the mitotic spindle [88]. In MAPT−/− neurons, hallmarks of normal pericentromeric heterochromatin (clustering of H3K9me3 and HP1α) are also disrupted [165, 169], indicating a role for tau in maintaining nucleolar integrity. Pericentromeric chromatin was also found to be disrupted in AD post-mortem brain tissue, further supporting a role for tau loss of function in disease [169].
Tau as a regulator of transcription
In addition to maintaining genomic integrity, tau may also regulate transcription of genes involved in neuronal function. A recent paper reported that shRNA knockdown of tau in neurons greatly reduced both mRNA and protein levels of VGLUT1 [234]. Overexpressing wild-type tau, or forcing tau translocation to the nucleus, resulted in increased VGLUT1 transcription [234]. Remarkably, this effect was abolished when attempted with P301L-mutant tau, indicating a potential loss-of-function effect of this FTD-associated mutation. Tau has also been implicated in repressing transcription of a number of genes implicated in neuronal function [17], with tau depletion, resulting in upregulation of proteins such as BAF-57 (involved in neuron-specific gene repression) [11]. Additionally, tau knockdown alters rDNA transcription, although whether tau normally promotes [226] or represses [165] this process, and the implications for neuronal function, is still under debate. Overall, tau plays many roles at the nucleus and there is evidence for disruption of these functions in disease. Preserving the physiological functions of tau at the nucleus may, therefore, provide therapeutic benefit in tauopathies.
Aβ at the nucleus - a caution for tau-lowering therapeutics?
Whilst the APP-processing product AICD is frequently associated with the nucleus (reviewed in [47]), a nuclear role for Aβ has been less forthcoming. Exogenously applied, or transfected, Aβ can translocate to the nucleus in vitro and is found at the nucleus in adult wild-type or APP/PS1 mice [12]. Some studies have suggested that Aβ1-42 can regulate transcription, including upregulation of APP and insulin-like growth factor receptors [12, 13]. However, most studies focus on the pathological roles of Aβ in the nucleus including inducing DNA breaks [244] and increasing chromosome mis-segregation by disrupting physiological tau function [88]. The fact that Aβ induces DNA damage provides an interesting link between potential Aβ and tau pathology in disease. Perhaps, increasing Aβ-mediated DNA damage results in reactionary alterations to tau that become overwhelmed in time. With this in mind, tau-lowering therapeutics without additional targeting of Aβ may need to be carefully considered to prevent additional DNA damage resulting from the removal of physiological protection.
Aβ and tau may function as tumour suppressors
Do individuals with AD have reduced incidence of cancer?
An increasing number of studies have reported a striking inverse association between AD and many types of cancer (reviewed in [30]), with one study reporting that the risk of developing cancer was 50% lower in individuals with AD [188]. This effect is not thought to be simply due to individuals with cancer dying earlier in life, as there is no such inverse correlation with other age-related disorders such as vascular dementia [221]. Of note, a recent paper by Rossi et al. showed that individuals with FTD possessing an MAPT mutation have an increased risk of developing cancer [223]. Together, such findings warrant exploration of whether tau and Aβ could function physiologically as tumour suppressors.
Aβ can act as a tumour suppressor
Aβ has been proposed to act as a tumour suppressor under a number of experimental conditions [30]. Studies demonstrate that Aβ can suppress tumour growth [201] and inhibit cancer cell proliferation [202], with Aβ dimers/trimers being stronger tumour inhibitors than pentadecamers [202]. AD transgenic mice overexpressing Aβ also demonstrate reduced growth rate of implanted glioma tumours, with the authors proposing that high levels of Aβ could inhibit neoangiogenesis within the tumour mass [200]. Brothers et al. suggest that Aβ could also indirectly suppress tumour formation through intercepting oncogenic viruses, or via scavenging free metal ions, restricting availability of micronutrients required for cell proliferation [30]. It is worth noting that the majority of studies investigating Aβ as a potential tumour suppressor have used supraphysiological concentrations in their models. Therefore, it is difficult to discern whether Aβ has a role in tumour suppression at physiological concentrations in humans. A recent study found significantly decreased BACE1 expression in invasive ductal carcinoma, indicating that reduced levels of Aβ could potentially increase the proliferation rate of this aggressive tumour [284]. Counterintuitively, increased levels of APP have been found in a number of cancers, with worse outcomes associated with higher APP levels (reviewed in [198]). Further research is, therefore, required to elucidate the contribution of Aβ and its processing pathways to cancer pathogenesis and the potential impacts of Aβ-targeting therapies on cancer risk.
Loss of tau function may increase tumour incidence
As microtubules are crucial components of the mitotic spindle and regulate the cell cycle [82], it seems plausible that tau could play a role in tumourigenesis. Gargini et al. showed that tau expression levels vary in different cancer types and high tau expression levels correlate with increased patient survival [82]. Another study found that MAPT knockdown enhanced cell growth and invasion and suggested that tau may be a tumour-suppressive protein in clear cell renal cell carcinoma [95]. The finding that MAPT mutations increase the risk of developing cancer suggests that tau mutations may result in loss of a tumour-suppressive function [223]. On the other hand, increased MAPT expression correlates with poor prognosis and taxane (a microtubule-stabilising drug) resistance in gastric cancer [180]. It appears that tau may have different effects depending on the cancer type being studied, highlighting the heterogeneous nature of cancer and the need for further research. As with Aβ, any potential for increased risk of cancer must be carefully assessed when designing tau-targeting therapeutics for AD.
Glucose metabolism
Dysregulation of insulin signalling in AD
Diabetes is a well-established risk factor for developing AD [152]. Insulin receptors are densely expressed in the hippocampus, frontal cortex, and entorhinal cortex [49], with insulin playing key roles in a number of crucial CNS processes such as synaptogenesis, synaptic remodelling [46], and regulation of memory [175]. The link between impaired insulin signalling and cognitive decline has been demonstrated in humans and animal models [25, 49]. Indeed, impaired brain glucose metabolism is an early characteristic of AD, with one study reporting that up to 81% of individuals with AD had either type 2 diabetes or impaired fasting glucose, an indicator of prediabetes [119]. Whilst direct connections between glucose metabolism, tau, and Aβ have been made, it is important to highlight that the association between AD and diabetes could be, at least in part, due to diabetes-related blood vessel damage given the strong epidemiological links between many vascular risk factors and AD [152, 176].
Tau regulates normal glucose metabolism
Marciniak et al. reported that MAPT−/− mice exhibit insulin resistance in the hippocampus, suggesting that tau plays a normal role in the cellular response to insulin, a function that may be lost in AD [170]. The authors propose a mechanism, whereby tau normally interacts with PTEN, a phosphatase that inhibits insulin signalling, reducing its activity [170]. Tau is expressed in the pancreas [296], and MAPT−/− mice have been shown to develop pancreatic β cell dysfunction and glucose intolerance [279]. A recent imaging study in humans found that Aβ affected tau-glucose metabolism associations [2]. This study reported that during normal ageing, small increases in tau are associated with increased glucose metabolism, but large accumulations of hyperphosphorylated tau associated with Aβ deposition correlated instead with hypometabolism, suggestive of a hormetic function for tau (Fig. 4), or Aβ-mediated dysregulation of normal tau function [2]. Interestingly, data from genome-wide association studies have shown that the MAPT H1 haplotype is associated with increased glucose intolerance in humans [170]. Taken together, tau likely plays a role in the regulation of homeostatic glucose metabolism. How this changes during disease, for example by loss of function caused by Aβ accumulation, or the potential effects of tau-targeting therapies on insulin signalling, requires further exploration.
Aβ-processing enzymes regulate insulin signalling
Whilst Aβ has been proposed to dysregulate insulin signalling [25], there is mounting evidence that its cleavage enzyme, BACE1, which is strongly expressed in the pancreas [298], plays crucial physiological roles in glucose homeostasis. Indeed, BACE1−/− mice show impaired insulin expression in the pancreas [104] and siRNA-mediated BACE1 knockdown significantly reduces insulin mRNA and protein in insulinoma cells [104]. However, another study reports that BACE1−/− mice have enhanced insulin sensitivity [177]. Notably, hyperglycaemia increases BACE1-mediated production of Aβ [142], indicative of a potentially vicious cycle between amyloid and glucose dysregulation. This also highlights the likely contribution of diseases such as diabetes mellitus to AD development and emphasises the potential of nutritional intervention strategies as a means of treating and preventing AD.
Conclusion
From molecular interactions with DNA to influencing complex behaviour, the physiological roles of tau (Fig. 5) and Aβ (Fig. 6) are multifaceted, dynamic, and at times, contradictory. This review emphasises the complexity of untangling physiology from pathology, as well as the wide-reaching implications, for both the brain and body, that can be induced by subtle protein alterations. Whilst the range of functions which we discuss are diverse, common themes emerge:
-
The functions of tau and Aβ are influenced by their location. Shifts within the cell, expression in different cells or locations within the body, can alter the roles that these proteins play, whether they are beneficial or harmful, and how therapeutic treatments will influence function.
-
Different isoforms, aggregation status, and post-translational modifications can dramatically alter the function of tau and Aβ.
-
The concentrations of tau and Aβ are crucial for regulating physiological versus pathological function. This “hormetic nature”, where too much or too little protein causes functional deficits, raises the likelihood of a “therapeutic sweet spot” where the physiologically optimal concentrations lie, outside of which may result in damage (Fig. 4).
-
AD is likely a combination of both gain- and loss-of-function phenotypes. Physiological responses can become hijacked to become toxic, detrimental functions can appear, or normal functions can be lost during disease-related changes.
-
Contradictory findings are common in the literature. The potential for developmental compensation in constitutive knockouts, as well as experimental differences in factors such as age, sex, and environment, will all impact outcome. Future studies testing multiple timepoints, acute versus constitutive knockdown, different genetic backgrounds, mixed-sex cohorts, and increasing comparisons between animal and human tissue will greatly clarify genuine phenotypes from experimental artefacts.
A schematic representation of the suggested physiological roles of tau in the brain and body. Created with https://biorender.com/
A schematic representation of the suggested physiological roles of Aβ in the brain and body. Created with https://biorender.com/
With the above in mind, a meticulous approach to therapeutic development is crucial. Therapies must balance potentially detrimental effects of targeting tau (Table 1) and Aβ (Table 2) with the benefits of disrupting pathology. Targeting treatments early in the disease cascade, considering the individual’s medical history (such as previous injury and comorbidities), engaging with modifiable lifestyle risk factors and the use of combinatorial therapies will likely be important to obtain the best outcome for individuals. By understanding the functions of tau and Aβ in health, we can gain greater insight into their contribution to disease. Such research will be vital for the development of safe and effective therapeutic strategies.
Abbreviations
- Aβ:
-
Amyloid beta
- AD:
-
Alzheimer’s disease
- AICD:
-
Aβ intracellular domain
- AMP:
-
Antimicrobial peptide
- APP:
-
Amyloid precursor protein
- ARIA:
-
Amyloid-related imaging abnormalities
- ASD:
-
Autism spectrum disorder
- BACE1:
-
Beta-site amyloid precursor protein cleaving enzyme 1
- BBB:
-
Blood–brain barrier
- BDNF:
-
Brain-derived neurotrophic factor
- CAA:
-
Cerebral amyloid angiopathy
- CBD:
-
Corticobasal degeneration
- CCI:
-
Controlled cortical impact
- CNS:
-
Central nervous system
- CSF:
-
Cerebrospinal fluid
- EAE:
-
Experimental autoimmune encephalomyelitis
- FTD:
-
Frontotemporal dementia
- FTD-P17:
-
Frontotemporal dementia with parkinsonism 17
- HSV:
-
Herpes simplex virus
- iPSC:
-
Induced pluripotent stem cell
- LTD:
-
Long-term depression
- LTP:
-
Long-term potentiation
- MAP:
-
Microtubule-associated protein
- MAPT:
-
Microtubule-associated protein tau
- MBP:
-
Myelin basic protein
- MS:
-
Multiple sclerosis
- MWM:
-
Morris Water Maze
- NFTs:
-
Neurofibrillary tangles
- PD:
-
Parkinson’s disease
- PNS:
-
Peripheral nervous system
- PSD:
-
Postsynaptic density
- PS1:
-
Presenilin-1
- PSP:
-
Progressive supranuclear palsy
- rDNA:
-
Ribosomal DNA
- ROS:
-
Reactive oxygen species
- SCI:
-
Spinal cord injury
- TBI:
-
Traumatic brain injury
- TGN:
-
Trans-Golgi network
- TTLL6:
-
Tubulin tyrosine ligase-like 6
- 3R:
-
Tau with 3 microtubule-binding domains
- 4R:
-
Tau with 4 microtubule-binding domains
References
Adalbert R, Milde S, Durrant C, Ando K, Stygelbout V, Yilmaz Z et al (2018) Interaction between a MAPT variant causing frontotemporal dementia and mutant APP affects axonal transport. Neurobiol Aging 68:68–75. https://doi.org/10.1016/j.neurobiolaging.2018.03.033
Adams JN, Lockhart SN, Li L, Jagust WJ (2019) Relationships between tau and glucose metabolism reflect alzheimer’s disease pathology in cognitively normal older adults. Cereb Cortex N Y NY 29:1997–2009. https://doi.org/10.1093/cercor/bhy078
Ahmed T, Van der Jeugd A, Blum D, Galas M-C, D’Hooge R, Buee L et al (2014) Cognition and hippocampal synaptic plasticity in mice with a homozygous tau deletion. Neurobiol Aging 35:2474–2478. https://doi.org/10.1016/j.neurobiolaging.2014.05.005
Allen B, Ingram E, Takao M, Smith MJ, Jakes R, Virdee K et al (2002) Abundant tau filaments and nonapoptotic neurodegeneration in transgenic mice expressing human p301s tau protein. J Neurosci 22:9340–9351. https://doi.org/10.1523/JNEUROSCI.22-21-09340.2002
Alzheimer’s Association (2019) 2019 Alzheimer’s disease facts and figures. Alzheimers Dement 15:321–387. https://doi.org/10.1016/j.jalz.2019.01.010
Amos LA (2004) Microtubule structure and its stabilisation. Org Biomol Chem 2:2153–2160. https://doi.org/10.1039/B403634D
Arbel-Ornath M, Hudry E, Boivin JR, Hashimoto T, Takeda S, Kuchibhotla KV et al (2017) Soluble oligomeric amyloid-β induces calcium dyshomeostasis that precedes synapse loss in the living mouse brain. Mol Neurodegener 12:27. https://doi.org/10.1186/s13024-017-0169-9
Arnes M, Alaniz ME, Karam CS, Cho JD, Lopez G, Javitch JA et al (2019) Role of tau protein in remodeling of circadian neuronal circuits and sleep. Front Aging Neurosci 11:320. https://doi.org/10.3389/fnagi.2019.00320
Ballatore C, Lee VM-Y, Trojanowski JQ (2007) Tau-mediated neurodegeneration in Alzheimer’s disease and related disorders. Nat Rev Neurosci 8:663–672. https://doi.org/10.1038/nrn2194
Barbier P, Zejneli O, Martinho M, Lasorsa A, Belle V, Smet-Nocca C et al (2019) Role of tau as a microtubule-associated protein: structural and functional aspects. Front Aging Neurosci. https://doi.org/10.3389/fnagi.2019.00204
de Barreda EG, Dawson HN, Vitek MP, Avila J (2010) Tau deficiency leads to the upregulation of BAF-57, a protein involved in neuron-specific gene repression. FEBS Lett 584:2265–2270. https://doi.org/10.1016/j.febslet.2010.03.032
Barucker C, Harmeier A, Weiske J, Fauler B, Albring KF, Prokop S et al (2014) Nuclear translocation uncovers the amyloid peptide Aβ42 as a regulator of gene transcription. J Biol Chem 289:20182–20191. https://doi.org/10.1074/jbc.M114.564690
Barucker C, Sommer A, Beckmann G, Eravci M, Harmeier A, Schipke CG et al (2015) Alzheimer amyloid peptide aβ42 regulates gene expression of transcription and growth factors. J Alzheimers Dis JAD 44:613–624. https://doi.org/10.3233/JAD-141902
Bear MF, Malenka RC (1994) Synaptic plasticity: LTP and LTD. Curr Opin Neurobiol 4:389–399. https://doi.org/10.1016/0959-4388(94)90101-5
Beevers JE, Lai MC, Collins E, Booth HDE, Zambon F, Parkkinen L et al (2017) MAPT genetic variation and neuronal maturity alter isoform expression affecting axonal transport in ipsc-derived dopamine neurons. Stem Cell Rep 9:587–599. https://doi.org/10.1016/j.stemcr.2017.06.005
Belaidi AA, Gunn AP, Wong BX, Ayton S, Appukuttan AT, Roberts BR et al (2018) Marked age-related changes in brain iron homeostasis in amyloid protein precursor knockout mice. Neurother J Am Soc Exp Neurother 15:1055–1062. https://doi.org/10.1007/s13311-018-0656-x
Benhelli-Mokrani H, Mansuroglu Z, Chauderlier A, Albaud B, Gentien D, Sommer S et al (2018) Genome-wide identification of genic and intergenic neuronal DNA regions bound by Tau protein under physiological and stress conditions. Nucleic Acids Res 46:11405–11422. https://doi.org/10.1093/nar/gky929
Besag FM (2017) Epilepsy in patients with autism: links, risks and treatment challenges. Neuropsychiatr Dis Treat 14:1–10. https://doi.org/10.2147/NDT.S120509
Bi M, Gladbach A, van Eersel J, Ittner A, Przybyla M, van Hummel A et al (2017) Tau exacerbates excitotoxic brain damage in an animal model of stroke. Nat Commun 8:473. https://doi.org/10.1038/s41467-017-00618-0
Biron KE, Dickstein DL, Gopaul R, Fenninger F, Jefferies WA (2013) Cessation of neoangiogenesis in alzheimer’s disease follows amyloid-beta immunization. Sci Rep 3:1354. https://doi.org/10.1038/srep01354
Biron KE, Dickstein DL, Gopaul R, Jefferies WA (2011) Amyloid triggers extensive cerebral angiogenesis causing blood brain barrier permeability and hypervascularity in Alzheimer’s disease. PLoS ONE 6:e23789. https://doi.org/10.1371/journal.pone.0023789
Biswas S, Kalil K (2018) The microtubule-associated protein tau mediates the organization of microtubules and their dynamic exploration of actin-rich lamellipodia and filopodia of cortical growth cones. J Neurosci 38:291–307. https://doi.org/10.1523/JNEUROSCI.2281-17.2017
Biundo F, Prete DD, Zhang H, Arancio O, D’Adamio L (2018) A role for tau in learning, memory and synaptic plasticity. Sci Rep 8:1–13. https://doi.org/10.1038/s41598-018-21596-3
Blockx I, Einstein S, Guns P-J, Van Audekerke J, Guglielmetti C, Zago W et al (2016) Monitoring blood-brain barrier integrity following amyloid-β immunotherapy using gadolinium-enhanced mri in a pdapp mouse model. J Alzheimers Dis JAD 54:723–735. https://doi.org/10.3233/JAD-160023
Bomfim TR, Forny-Germano L, Sathler LB, Brito-Moreira J, Houzel J-C, Decker H et al (2012) An anti-diabetes agent protects the mouse brain from defective insulin signaling caused by Alzheimer’s disease–associated Aβ oligomers. J Clin Invest 122:1339–1353. https://doi.org/10.1172/JCI57256
Born HA, Kim J-Y, Savjani RR, Das P, Dabaghian YA, Guo Q et al (2014) Genetic suppression of transgenic APP rescues Hypersynchronous network activity in a mouse model of Alzeimer’s disease. J Neurosci Off J Soc Neurosci 34:3826–3840. https://doi.org/10.1523/JNEUROSCI.5171-13.2014
Boscolo E, Folin M, Nico B, Grandi C, Mangieri D, Longo V et al (2007) β amyloid angiogenic activity in vitro and in vivo. Int J Mol Med 19:581–587. https://doi.org/10.3892/ijmm.19.4.581
Braak H, Braak E (1991) Neuropathological stageing of Alzheimer-related changes. Acta Neuropathol (Berl) 82:239–259. https://doi.org/10.1007/BF00308809
Brody DL, Magnoni S, Schwetye KE, Spinner ML, Esparza TJ, Stocchetti N et al (2008) Amyloid-beta dynamics correlate with neurological status in the injured human brain. Science 321:1221–1224. https://doi.org/10.1126/science.1161591
Brothers HM, Gosztyla ML, Robinson SR (2018) The physiological roles of amyloid-β peptide hint at new ways to treat Alzheimer’s Disease. Front Aging Neurosci. https://doi.org/10.3389/fnagi.2018.00118
Bryan JB, Nagle BW, Doenges KH (1975) Inhibition of tubulin assembly by RNA and other polyanions: evidence for a required protein. Proc Natl Acad Sci USA 72:3570–3574
Buckner RL, Snyder AZ, Shannon BJ, LaRossa G, Sachs R, Fotenos AF et al (2005) Molecular, structural, and functional characterization of Alzheimer’s disease: evidence for a relationship between default activity, amyloid, and memory. J Neurosci Off J Soc Neurosci 25:7709–7717. https://doi.org/10.1523/JNEUROSCI.2177-05.2005
Bueche CZ, Hawkes C, Garz C, Vielhaber S, Attems J, Knight RT et al (2014) Hypertension drives parenchymal β-amyloid accumulation in the brain parenchyma. Ann Clin Transl Neurol 1:124–129. https://doi.org/10.1002/acn3.27
Burdick D, Soreghan B, Kwon M, Kosmoski J, Knauer M, Henschen A et al (1992) Assembly and aggregation properties of synthetic Alzheimer’s A4/beta amyloid peptide analogs. J Biol Chem 267:546–554
Busche MA, Chen X, Henning HA, Reichwald J, Staufenbiel M, Sakmann B et al (2012) Critical role of soluble amyloid-β for early hippocampal hyperactivity in a mouse model of Alzheimer’s disease. Proc Natl Acad Sci 109:8740–8745. https://doi.org/10.1073/pnas.1206171109
Caceres A, Kosik KS (1990) Inhibition of neurite polarity by tau antisense oligonucleotides in primary cerebellar neurons. Nature 343:461–463. https://doi.org/10.1038/343461a0
Caceres A, Potrebic S, Kosik KS (1991) The effect of tau antisense oligonucleotides on neurite formation of cultured cerebellar macroneurons. J Neurosci Off J Soc Neurosci 11:1515–1523
Cai J, Qi X, Kociok N, Skosyrski S, Emilio A, Ruan Q et al (2012) β-Secretase (BACE1) inhibition causes retinal pathology by vascular dysregulation and accumulation of age pigment. EMBO Mol Med 4:980–991. https://doi.org/10.1002/emmm.201101084
Camero S, Benítez MJ, Barrantes A, Ayuso JM, Cuadros R, Avila J et al (2014) Tau protein provides DNA with thermodynamic and structural features which are similar to those found in histone-DNA complex. J Alzheimers Dis JAD 39:649–660. https://doi.org/10.3233/JAD-131415
Cameron DJ, Galvin C, Alkam T, Sidhu H, Ellison J, Luna S et al (2012) Alzheimer’s-related peptide amyloid-β plays a conserved role in angiogenesis. PLoS ONE 7:e39598. https://doi.org/10.1371/journal.pone.0039598
Cantero JL, Hita-Yañez E, Moreno-Lopez B, Portillo F, Rubio A, Avila J (2010) Tau protein role in sleep-wake cycle. J Alzheimers Dis JAD 21:411–421. https://doi.org/10.3233/JAD-2010-100285
Chávez-Gutiérrez L, Bammens L, Benilova I, Vandersteen A, Benurwar M, Borgers M et al (2012) The mechanism of γ-Secretase dysfunction in familial Alzheimer disease. EMBO J 31:2261–2274. https://doi.org/10.1038/emboj.2012.79
Chen M, Inestrosa NC, Ross GS, Fernandez HL (1995) Platelets are the primary source of amyloid beta-peptide in human blood. Biochem Biophys Res Commun 213:96–103. https://doi.org/10.1006/bbrc.1995.2103
Chen Q, Zhou Z, Zhang L, Wang Y, Zhang Y, Zhong M et al (2012) Tau protein is involved in morphological plasticity in hippocampal neurons in response to BDNF. Neurochem Int 60:233–242. https://doi.org/10.1016/j.neuint.2011.12.013
Cheng JS, Craft R, Yu G-Q, Ho K, Wang X, Mohan G et al (2014) Tau reduction diminishes spatial learning and memory deficits after mild repetitive traumatic brain injury in mice. PLoS ONE 9:e115765. https://doi.org/10.1371/journal.pone.0115765
Chiu S-L, Chen C-M, Cline HT (2008) Insulin receptor signaling regulates synapse number, dendritic plasticity, and circuit function in vivo. Neuron 58:708–719. https://doi.org/10.1016/j.neuron.2008.04.014
Chow VW, Mattson MP, Wong PC, Gleichmann M (2010) An overview of APP processing enzymes and products. Neuromolecular Med 12:1–12. https://doi.org/10.1007/s12017-009-8104-z
Cieri D, Vicario M, Vallese F, D’Orsi B, Berto P, Grinzato A et al (2018) Tau localises within mitochondrial sub-compartments and its caspase cleavage affects ER-mitochondria interactions and cellular Ca2+ handling. Biochim Biophys Acta BBA 1864:3247–3256. https://doi.org/10.1016/j.bbadis.2018.07.011
Craft S, Baker LD, Montine TJ, Minoshima S, Watson GS, Claxton A et al (2012) Intranasal insulin therapy for alzheimer disease and amnestic mild cognitive impairment. Arch Neurol 69:29–38. https://doi.org/10.1001/archneurol.2011.233
Criado-Marrero M, Sabbagh JJ, Jones MR, Chaput D, Dickey CA, Blair LJ (2020) Hippocampal neurogenesis is enhanced in adult tau deficient mice. Cells. https://doi.org/10.3390/cells9010210
Cunvong K, Huffmire D, Ethell DW, Cameron DJ (2013) Amyloid-β increases capillary bed density in the adult zebrafish retina. Invest Ophthalmol Vis Sci 54:1516–1521. https://doi.org/10.1167/iovs.12-10821
Davies C, Spires-Jones TL (2018) Complementing tau: new data show that the complement system is involved in degeneration in tauopathies. Neuron 100:1267–1269. https://doi.org/10.1016/j.neuron.2018.12.003
Dawson GR, Seabrook GR, Zheng H, Smith DW, Graham S, O’Dowd G et al (1999) Age-related cognitive deficits, impaired long-term potentiation and reduction in synaptic marker density in mice lacking the beta-amyloid precursor protein. Neuroscience 90:1–13. https://doi.org/10.1016/s0306-4522(98)00410-2
Dawson HN, Ferreira A, Eyster MV, Ghoshal N, Binder LI, Vitek MP (2001) Inhibition of neuronal maturation in primary hippocampal neurons from tau deficient mice. J Cell Sci 114:1179–1187
De Strooper B, Annaert W, Cupers P, Saftig P, Craessaerts K, Mumm JS et al (1999) A presenilin-1-dependent gamma-secretase-like protease mediates release of Notch intracellular domain. Nature 398:518–522. https://doi.org/10.1038/19083
DeKosky ST, Scheff SW (1990) Synapse loss in frontal cortex biopsies in Alzheimer’s disease: correlation with cognitive severity. Ann Neurol 27:457–464
Derby CA, Katz MJ, Lipton RB, Hall CB (2017) Trends in dementia incidence in a birth cohort analysis of the Einstein Aging Study. JAMA Neurol 74:1345–1351. https://doi.org/10.1001/jamaneurol.2017.1964
Desai BS, Schneider JA, Li J-L, Carvey PM, Hendey B (2009) Evidence of angiogenic vessels in Alzheimer’s disease. J Neural Transm Vienna Austria 116:587–597. https://doi.org/10.1007/s00702-009-0226-9
DeVos SL, Goncharoff DK, Chen G, Kebodeaux CS, Yamada K, Stewart FR et al (2013) Antisense reduction of tau in adult mice protects against seizures. J Neurosci 33:12887–12897. https://doi.org/10.1523/JNEUROSCI.2107-13.2013
Dierich M, Hartmann S, Dietrich N, Moeser P, Brede F, Johnson Chacko L et al (2019) β-Secretase BACE1 is required for normal cochlear function. J Neurosci 39:9013–9027. https://doi.org/10.1523/JNEUROSCI.0028-19.2019
Dixit R, Ross JL, Goldman YE, Holzbaur ELF (2008) Differential regulation of dynein and kinesin motor proteins by tau. Science 319:1086–1089. https://doi.org/10.1126/science.1152993
Drechsel DN, Hyman AA, Cobb MH, Kirschner MW (1992) Modulation of the dynamic instability of tubulin assembly by the microtubule-associated protein tau. Mol Biol Cell 3:1141–1154
Duce JA, Tsatsanis A, Cater MA, James SA, Robb E, Wikhe K et al (2010) Iron-export ferroxidase activity of β-amyloid precursor protein is inhibited by zinc in Alzheimer’s disease. Cell 142:857–867. https://doi.org/10.1016/j.cell.2010.08.014
Durrant CS, Ruscher K, Sheppard O, Coleman MP, Özen I (2020) Beta secretase 1-dependent amyloid precursor protein processing promotes excessive vascular sprouting through NOTCH3 signalling. Cell Death Dis 11:1–15. https://doi.org/10.1038/s41419-020-2288-4
Ebneth A, Godemann R, Stamer K, Illenberger S, Trinczek B, Mandelkow E-M et al (1998) Overexpression of tau protein inhibits kinesin-dependent trafficking of vesicles, mitochondria, and endoplasmic reticulum: implications for Alzheimer’s Disease. J Cell Biol 143:777–794
Eckert A, Schmitt K, Götz J (2011) Mitochondrial dysfunction the beginning of the end in Alzheimer’s disease? Separate and synergistic modes of tau and amyloid-β toxicity. Alzheimers Res Ther 3:15. https://doi.org/10.1186/alzrt74
Edwards G, Zhao J, Dash PK, Soto C, Moreno-Gonzalez I (2019) Traumatic brain injury induces tau aggregation and spreading. J Neurotrauma 37:80–92. https://doi.org/10.1089/neu.2018.6348
Eftekharzadeh B, Daigle JG, Kapinos LE, Coyne A, Schiantarelli J, Carlomagno Y et al (2018) Tau protein disrupts nucleocytoplasmic transport in Alzheimer’s disease. Neuron 99:925–940.e7. https://doi.org/10.1016/j.neuron.2018.07.039
Elaskalani O, Khan I, Morici M, Matthysen C, Sabale M, Martins RN et al (2018) Oligomeric and fibrillar amyloid beta 42 induce platelet aggregation partially through GPVI. Platelets 29:415–420. https://doi.org/10.1080/09537104.2017.1401057
Esch FS, Keim PS, Beattie EC, Blacher RW, Culwell AR, Oltersdorf T et al (1990) Cleavage of amyloid beta peptide during constitutive processing of its precursor. Science 248:1122–1124. https://doi.org/10.1126/science.2111583
Evans W, Fung HC, Steele J, Eerola J, Tienari P, Pittman A et al (2004) The tau H2 haplotype is almost exclusively Caucasian in origin. Neurosci Lett 369:183–185. https://doi.org/10.1016/j.neulet.2004.05.119
Farah MH, Pan BH, Hoffman PN, Ferraris D, Tsukamoto T, Nguyen T et al (2011) Reduced BACE1 activity enhances clearance of myelin debris and regeneration of axons in the injured peripheral nervous system. J Neurosci 31:5744–5754. https://doi.org/10.1523/JNEUROSCI.6810-10.2011
Ferrer I, Andrés-Benito P, Zelaya MV, Aguirre MEE, Carmona M, Ausín K et al (2020) Familial globular glial tauopathy linked to MAPT mutations: molecular neuropathology and seeding capacity of a prototypical mixed neuronal and glial tauopathy. Acta Neuropathol (Berl) 139:735–771. https://doi.org/10.1007/s00401-019-02122-9
Filser S, Ovsepian SV, Masana M, Blazquez-Llorca L, Brandt Elvang A, Volbracht C et al (2015) Pharmacological inhibition of BACE1 impairs synaptic plasticity and cognitive functions. Biol Psychiatry 77:729–739. https://doi.org/10.1016/j.biopsych.2014.10.013
Fischer I, Baas PW (2020) Resurrecting the mysteries of big tau. Trends Neurosci 43:493–504. https://doi.org/10.1016/j.tins.2020.04.007
Fischer VW, Siddiqi A, Yusufaly Y (1990) Altered angioarchitecture in selected areas of brains with Alzheimer’s disease. Acta Neuropathol (Berl) 79:672–679. https://doi.org/10.1007/bf00294246
Frank S, Clavaguera F, Tolnay M (2007) Tauopathy models and human neuropathology: similarities and differences. Acta Neuropathol (Berl) 115:39–53. https://doi.org/10.1007/s00401-007-0291-9
Fuster-Matanzo A, de Barreda EG, Dawson HN, Vitek MP, Avila J, Hernández F (2009) Function of tau protein in adult newborn neurons. FEBS Lett 583:3063–3068. https://doi.org/10.1016/j.febslet.2009.08.017
Gao L, Tse S-W, Conrad C, Andreadis A (2005) Saitohin, which is nested in the tau locus and confers allele-specific susceptibility to several neurodegenerative diseases, interacts with peroxiredoxin 6. J Biol Chem 280:39268–39272. https://doi.org/10.1074/jbc.M506116200
Garcia-Alloza M, Gregory J, Kuchibhotla KV, Fine S, Wei Y, Ayata C et al (2011) Cerebrovascular lesions induce transient β-amyloid deposition. Brain J Neurol 134:3697–3707. https://doi.org/10.1093/brain/awr300
Garcia-Osta A, Alberini CM (2009) Amyloid beta mediates memory formation. Learn Mem 16:267–272. https://doi.org/10.1101/lm.1310209
Gargini R, Segura-Collar B, Sánchez-Gómez P (2019) Novel functions of the neurodegenerative-related gene tau in cancer. Front Aging Neurosci. https://doi.org/10.3389/fnagi.2019.00231
Gilley J, Seereeram A, Ando K, Mosely S, Andrews S, Kerschensteiner M et al (2012) Age-dependent axonal transport and locomotor changes and tau hypophosphorylation in a “P301L” tau knockin mouse. Neurobiol Aging 33:621.e1–621.e15. https://doi.org/10.1016/j.neurobiolaging.2011.02.014
Goldgaber D, Lerman MI, McBride OW, Saffiotti U, Gajdusek DC (1987) Characterization and chromosomal localization of a cDNA encoding brain amyloid of Alzheimer’s disease. Science 235:877–880. https://doi.org/10.1126/science.3810169
Golovyashkina N, Penazzi L, Ballatore C, Smith AB, Bakota L, Brandt R (2015) Region-specific dendritic simplification induced by Aβ, mediated by tau via dysregulation of microtubule dynamics: a mechanistic distinct event from other neurodegenerative processes. Mol Neurodegener 10:60. https://doi.org/10.1186/s13024-015-0049-0
Gonçalves RA, Wijesekara N, Fraser PE, De Felice FG (2020) Behavioral Abnormalities in Knockout and Humanized Tau Mice. Front Endocrinol. https://doi.org/10.3389/fendo.2020.00124
Gosztyla ML, Brothers HM, Robinson SR (2018) Alzheimer’s amyloid-β is an antimicrobial peptide: a review of the evidence. J Alzheimers Dis JAD 62:1495–1506. https://doi.org/10.3233/JAD-171133
Granic A, Padmanabhan J, Norden M, Potter H (2010) Alzheimer Aβ peptide induces chromosome mis-segregation and aneuploidy, including trisomy 21: requirement for tau and APP. Mol Biol Cell 21:511–520. https://doi.org/10.1091/mbc.E09-10-0850
Grant JL, Ghosn EEB, Axtell RC, Herges K, Kuipers HF, Woodling NS et al (2012) Reversal of paralysis and reduced inflammation from peripheral administration of β-amyloid in TH1 and TH17 versions of experimental autoimmune encephalomyelitis. Sci Transl Med 4:145ra105. https://doi.org/10.1126/scitranslmed.3004145
Green DA, Masliah E, Vinters HV, Beizai P, Moore DJ, Achim CL (2005) Brain deposition of beta-amyloid is a common pathologic feature in HIV positive patients. AIDS Lond Engl 19:407–411. https://doi.org/10.1097/01.aids.0000161770.06158.5c
Greenfield JP, Tsai J, Gouras GK, Hai B, Thinakaran G, Checler F et al (1999) Endoplasmic reticulum and trans-Golgi network generate distinct populations of Alzheimer β-amyloid peptides. Proc Natl Acad Sci 96:742–747. https://doi.org/10.1073/pnas.96.2.742
Gulisano W, Melone M, Ripoli C, Tropea MR, Puma DDL, Giunta S et al (2019) Neuromodulatory action of picomolar extracellular aβ42 oligomers on presynaptic and postsynaptic mechanisms underlying synaptic function and memory. J Neurosci 39:5986–6000. https://doi.org/10.1523/JNEUROSCI.0163-19.2019
Gumucio A, Lannfelt L, Nilsson LN (2013) Lack of exon 10 in the murine tau gene results in mild sensorimotor defects with aging. BMC Neurosci 14:148. https://doi.org/10.1186/1471-2202-14-148
Guo T, Noble W, Hanger DP (2017) Roles of tau protein in health and disease. Acta Neuropathol (Berl) 133:665–704. https://doi.org/10.1007/s00401-017-1707-9
Han X, Sekino Y, Babasaki T, Goto K, Inoue S, Hayashi T et al (2020) Microtubule-associated protein tau (MAPT) is a promising independent prognostic marker and tumor suppressive protein in clear cell renal cell carcinoma. Urol Oncol 38:605.e9–605.e17. https://doi.org/10.1016/j.urolonc.2020.02.010
Harada A, Oguchi K, Okabe S, Kuno J, Terada S, Ohshima T et al (1994) Altered microtubule organization in small-calibre axons of mice lacking tau protein. Nature 369:488–491. https://doi.org/10.1038/369488a0
Harwell CS, Coleman MP (2016) Synaptophysin depletion and intraneuronal Aβ in organotypic hippocampal slice cultures from huAPP transgenic mice. Mol Neurodegener 11:44. https://doi.org/10.1186/s13024-016-0110-7
Hauptmann S, Keil U, Scherping I, Bonert A, Eckert A, Müller WE (2006) Mitochondrial dysfunction in sporadic and genetic Alzheimer’s disease. Exp Gerontol 41:668–673. https://doi.org/10.1016/j.exger.2006.03.012
He Y, Wei M, Wu Y, Qin H, Li W, Ma X et al (2019) Amyloid β oligomers suppress excitatory transmitter release via presynaptic depletion of phosphatidylinositol-4,5-bisphosphate. Nat Commun 10:1193. https://doi.org/10.1038/s41467-019-09114-z
Hefter D, Draguhn A (2017) APP as a protective factor in acute neuronal insults. Front Mol Neurosci. https://doi.org/10.3389/fnmol.2017.00022
Hellström-Lindahl E, Viitanen M, Marutle A (2009) Comparison of Aβ levels in the brain of familial and sporadic Alzheimer’s disease. Neurochem Int 55:243–252. https://doi.org/10.1016/j.neuint.2009.03.007
Hernández-Vega A, Braun M, Scharrel L, Jahnel M, Wegmann S et al (2017) Local nucleation of microtubule bundles through tubulin concentration into a condensed tau phase. Cell Rep 20:2304–2312. https://doi.org/10.1016/j.celrep.2017.08.042
Hitt BD, Jaramillo TC, Chetkovich DM, Vassar R (2010) BACE1-/- mice exhibit seizure activity that does not correlate with sodium channel level or axonal localization. Mol Neurodegener 5:31. https://doi.org/10.1186/1750-1326-5-31
Hoffmeister A, Tuennemann J, Sommerer I, Mössner J, Rittger A, Schleinitz D et al (2013) Genetic and biochemical evidence for a functional role of BACE1 in the regulation of insulin mRNA expression. Obesity 21:E626–E633. https://doi.org/10.1002/oby.20482
Holth JK, Bomben VC, Reed JG, Inoue T, Younkin L, Younkin SG et al (2013) Tau loss attenuates neuronal network hyperexcitability in mouse and Drosophila genetic models of epilepsy. J Neurosci Off J Soc Neurosci 33:1651–1659. https://doi.org/10.1523/JNEUROSCI.3191-12.2013
Hong S, Beja-Glasser VF, Nfonoyim BM, Frouin A, Li S, Ramakrishnan S et al (2016) Complement and microglia mediate early synapse loss in Alzheimer mouse models. Science 352:712–716. https://doi.org/10.1126/science.aad8373
Hong X-P, Peng C-X, Wei W, Tian Q, Liu Y-H, Yao X-Q et al (2010) Essential role of tau phosphorylation in adult hippocampal neurogenesis. Hippocampus 20:1339–1349. https://doi.org/10.1002/hipo.20712
Houlden H, Baker M, Morris HR, MacDonald N, Pickering-Brown S et al (2001) Corticobasal degeneration and progressive supranuclear palsy share a common tau haplotype. Neurology 56:1702–1706. https://doi.org/10.1212/wnl.56.12.1702
Hu X, He W, Diaconu C, Tang X, Kidd GJ, Macklin WB et al (2008) Genetic deletion of BACE1 in mice affects remyelination of sciatic nerves. FASEB J 22:2970–2980. https://doi.org/10.1096/fj.08-106666
Hu X, Hicks CW, He W, Wong P, Macklin WB, Trapp BD et al (2006) Bace1 modulates myelination in the central and peripheral nervous system. Nat Neurosci 9:1520–1525. https://doi.org/10.1038/nn1797
Hu X, Hu J, Dai L, Trapp B, Yan R (2015) Axonal and schwann cell BACE1 is equally required for remyelination of peripheral nerves. J Neurosci 35:3806–3814. https://doi.org/10.1523/JNEUROSCI.5207-14.2015
Hu X, Zhou X, He W, Yang J, Xiong W, Wong P et al (2010) BACE1 deficiency causes altered neuronal activity and neurodegeneration. J Neurosci 30:8819–8829. https://doi.org/10.1523/JNEUROSCI.1334-10.2010
van Hummel A, Bi M, Ippati S, van der Hoven J, Volkerling A, Lee WS et al (2016) No overt deficits in aged tau-deficient C57Bl/6. Mapttm1(EGFP)Kit GFP knockin mice. PLoS ONE 11:e0163236. https://doi.org/10.1371/journal.pone.0163236
Ikegami S, Harada A, Hirokawa N (2000) Muscle weakness, hyperactivity, and impairment in fear conditioning in tau-deficient mice. Neurosci Lett 279:129–132. https://doi.org/10.1016/s0304-3940(99)00964-7
Iqbal K, Grundke-Iqbal I, Zaidi T, Merz PA, Wen GY, Shaikh SS et al (1986) Defective brain microtubule assembly in Alzheimer’s disease. Lancet Lond Engl 2:421–426. https://doi.org/10.1016/s0140-6736(86)92134-3
Ittner LM, Ke YD, Delerue F, Bi M, Gladbach A, van Eersel J et al (2010) Dendritic function of tau mediates amyloid-beta toxicity in Alzheimer’s disease mouse models. Cell 142:387–397. https://doi.org/10.1016/j.cell.2010.06.036
Jackson J, Bianco G, Rosa AO, Cowan K, Bond P, Anichtchik O et al (2018) White matter tauopathy: transient functional loss and novel myelin remodeling. Glia 66:813–827. https://doi.org/10.1002/glia.23286
Janning D, Igaev M, Sündermann F, Brühmann J, Beutel O, Heinisch JJ et al (2014) Single-molecule tracking of tau reveals fast kiss-and-hop interaction with microtubules in living neurons. Mol Biol Cell 25:3541–3551. https://doi.org/10.1091/mbc.E14-06-1099
Janson J, Laedtke T, Parisi JE, O’Brien P, Petersen RC, Butler PC (2004) Increased risk of type 2 diabetes in Alzheimer disease. Diabetes 53:474–481. https://doi.org/10.2337/diabetes.53.2.474
Joseph M, Anglada-Huguet M, Paesler K, Mandelkow E, Mandelkow E-M (2017) Anti-aggregant tau mutant promotes neurogenesis. Mol Neurodegener 12:88. https://doi.org/10.1186/s13024-017-0230-8
Joseph-Mathurin N, Dorieux O, Trouche SG, Boutajangout A, Kraska A, Fontès P et al (2013) Amyloid beta immunization worsens iron deposits in the choroid plexus and cerebral microbleeds. Neurobiol Aging 34:2613–2622. https://doi.org/10.1016/j.neurobiolaging.2013.05.013
Jul P, Volbracht C, de Jong IEM, Helboe L, Elvang AB, Pedersen JT (2016) Hyperactivity with agitative-like behavior in a mouse tauopathy model. J Alzheimers Dis JAD 49:783–795. https://doi.org/10.3233/JAD-150292
Kamenetz F, Tomita T, Hsieh H, Seabrook G, Borchelt D, Iwatsubo T et al (2003) APP processing and synaptic function. Neuron 37:925–937. https://doi.org/10.1016/s0896-6273(03)00124-7
Kanaan NM, Morfini GA, LaPointe NE, Pigino GF, Patterson KR, Song Y et al (2011) Pathogenic forms of tau inhibit kinesin-dependent axonal transport through a mechanism involving activation of axonal phosphotransferases. J Neurosci Off J Soc Neurosci 31:9858–9868. https://doi.org/10.1523/JNEUROSCI.0560-11.2011
Kang J, Lemaire HG, Unterbeck A, Salbaum JM, Masters CL, Grzeschik KH et al (1987) The precursor of Alzheimer’s disease amyloid A4 protein resembles a cell-surface receptor. Nature 325:733–736. https://doi.org/10.1038/325733a0
Kawahara M (2010) Neurotoxicity of β-amyloid protein: oligomerization, channel formation, and calcium dyshomeostasis. Curr Pharm Des 16:2779–2789. https://doi.org/10.2174/138161210793176545
Keaney J, Walsh DM, O’Malley T, Hudson N, Crosbie DE, Loftus T et al (2015) Autoregulated paracellular clearance of amyloid-β across the blood-brain barrier. Sci Adv 1:e1500472. https://doi.org/10.1126/sciadv.1500472
Kimura T, Whitcomb DJ, Jo J, Regan P, Piers T, Heo S et al (2014) Microtubule-associated protein tau is essential for long-term depression in the hippocampus. Philos Trans R Soc Lond B Biol Sci 369:20130144. https://doi.org/10.1098/rstb.2013.0144
Klein C, Kramer E-M, Cardine A-M, Schraven B, Brandt R, Trotter J (2002) Process outgrowth of oligodendrocytes is promoted by interaction of fyn kinase with the cytoskeletal protein tau. J Neurosci Off J Soc Neurosci 22:698–707
Kobayashi D, Zeller M, Cole T, Buttini M, McConlogue L, Sinha S et al (2008) BACE1 gene deletion: impact on behavioral function in a model of Alzheimer’s disease. Neurobiol Aging 29:861–873. https://doi.org/10.1016/j.neurobiolaging.2007.01.002
Kobayashi S, Tanaka T, Soeda Y, Takashima A (2019) Enhanced tau protein translation by hyper-excitation. Front Aging Neurosci 11:322. https://doi.org/10.3389/fnagi.2019.00322
Koffie RM, Meyer-Luehmann M, Hashimoto T, Adams KW, Mielke ML, Garcia-Alloza M et al (2009) Oligomeric amyloid associates with postsynaptic densities and correlates with excitatory synapse loss near senile plaques. Proc Natl Acad Sci 106:4012–4017. https://doi.org/10.1073/pnas.0811698106
Koike MA, Lin AJ, Pham J, Nguyen E, Yeh JJ, Rahimian R et al (2012) APP knockout mice experience acute mortality as the result of ischemia. PLoS ONE 7:e42665. https://doi.org/10.1371/journal.pone.0042665
Komuro Y, Xu G, Bhaskar K, Lamb BT (2015) Human tau expression reduces adult neurogenesis in a mouse model of tauopathy. Neurobiol Aging 36:2034–2042. https://doi.org/10.1016/j.neurobiolaging.2015.03.002
Kopeikina KJ, Carlson GA, Pitstick R, Ludvigson AE, Peters A, Luebke JI et al (2011) Tau accumulation causes mitochondrial distribution deficits in neurons in a mouse model of tauopathy and in human Alzheimer’s disease brain. Am J Pathol 179:2071–2082. https://doi.org/10.1016/j.ajpath.2011.07.004
Kosik KS, Joachim CL, Selkoe DJ (1986) Microtubule-associated protein tau (tau) is a major antigenic component of paired helical filaments in Alzheimer disease. Proc Natl Acad Sci USA 83:4044–4048
Ksiezak-Reding H, Binder LI, Yen SH (1988) Immunochemical and biochemical characterization of tau proteins in normal and Alzheimer’s disease brains with Alz 50 and Tau-1. J Biol Chem 263:7948–7953
Kumar DKV, Choi SH, Washicosky KJ, Eimer WA, Tucker S, Ghofrani J et al (2016) Amyloid-β peptide protects against microbial infection in mouse and worm models of Alzheimer’s disease. Sci Transl Med 8:34072. https://doi.org/10.1126/scitranslmed.aaf1059
Laird FM, Cai H, Savonenko AV, Farah MH, He K, Melnikova T et al (2005) BACE1, a major determinant of selective vulnerability of the brain to amyloid-β amyloidogenesis, is essential for cognitive, emotional, and synaptic functions. J Neurosci 25:11693–11709. https://doi.org/10.1523/JNEUROSCI.2766-05.2005
Lane DJR, Ayton S, Bush AI (2018) Iron and Alzheimer’s disease: an update on emerging mechanisms. J Alzheimers Dis JAD 64:S379–S395. https://doi.org/10.3233/JAD-179944
Lee G, Neve RL, Kosik KS (1989) The microtubule binding domain of tau protein. Neuron 2:1615–1624. https://doi.org/10.1016/0896-6273(89)90050-0
Lee HJ, Ryu JM, Jung YH, Lee S-J, Kim JY, Lee SH et al (2016) High glucose upregulates BACE1-mediated Aβ production through ROS-dependent HIF-1α and LXRα/ABCA1-regulated lipid raft reorganization in SK-N-MC cells. Sci Rep. https://doi.org/10.1038/srep36746
Lei P, Ayton S, Appukuttan AT, Moon S, Duce JA, Volitakis I et al (2017) Lithium suppression of tau induces brain iron accumulation and neurodegeneration. Mol Psychiatry 22:396–406. https://doi.org/10.1038/mp.2016.96
Lei P, Ayton S, Appukuttan AT, Volitakis I, Adlard PA et al (2015) Clioquinol rescues Parkinsonism and dementia phenotypes of the tau knockout mouse. Neurobiol Dis 81:168–175. https://doi.org/10.1016/j.nbd.2015.03.015
Lei P, Ayton S, Finkelstein DI, Spoerri L, Ciccotosto GD, Wright DK et al (2012) Tau deficiency induces parkinsonism with dementia by impairing APP-mediated iron export. Nat Med 18:291–295. https://doi.org/10.1038/nm.2613
Lei P, Ayton S, Moon S, Zhang Q, Volitakis I, Finkelstein DI et al (2014) Motor and cognitive deficits in aged tau knockout mice in two background strains. Mol Neurodegener 9:29. https://doi.org/10.1186/1750-1326-9-29
Li L, Fothergill T, Hutchins BI, Dent EW, Kalil K (2014) Wnt5a evokes cortical axon outgrowth and repulsive guidance by tau mediated reorganization of dynamic microtubules. Dev Neurobiol 74:797–817. https://doi.org/10.1002/dneu.22102
Li Z, Hall AM, Kelinske M, Roberson ED (2014) Seizure resistance without parkinsonism in aged mice after tau reduction. Neurobiol Aging 35:2617–2624. https://doi.org/10.1016/j.neurobiolaging.2014.05.001
Lin W-L, Zehr C, Lewis J, Hutton M, Yen S-H, Dickson DW (2005) Progressive white matter pathology in the spinal cord of transgenic mice expressing mutant (P301L) human tau. J Neurocytol 34:397–410. https://doi.org/10.1007/s11068-006-8726-0
Liu CA, Lee G, Jay DG (1999) Tau is required for neurite outgrowth and growth cone motility of chick sensory neurons. Cell Motil 43:232–242. https://doi.org/10.1002/(SICI)1097-0169(1999)43:3<232:AID-CM6>3.0.CO;2-7
Liu L, Ding L, Rovere M, Wolfe MS, Selkoe DJ (2019) A cellular complex of BACE1 and γ-secretase sequentially generates Aβ from its full-length precursor. J Cell Biol 218:644–663. https://doi.org/10.1083/jcb.201806205
Livingston G, Sommerlad A, Orgeta V, Costafreda SG, Huntley J, Ames D et al (2017) Dementia prevention, intervention, and care. The Lancet 390:2673–2734. https://doi.org/10.1016/S0140-6736(17)31363-6
Loane DJ, Pocivavsek A, Moussa CE-H, Thompson R, Matsuoka Y et al (2009) Amyloid precursor protein secretases as therapeutic targets for traumatic brain injury. Nat Med 15:377–379. https://doi.org/10.1038/nm.1940
Lombardo S, Chiacchiaretta M, Tarr A, Kim W, Cao T, Sigal G et al (2019) BACE1 partial deletion induces synaptic plasticity deficit in adult mice. Sci Rep. https://doi.org/10.1038/s41598-019-56329-7
Long JM, Holtzman DM (2019) Alzheimer disease: an update on pathobiology and treatment strategies. Cell 179:312–339. https://doi.org/10.1016/j.cell.2019.09.001
Loomis PA, Howard TH, Castleberry RP, Binder LI (1990) Identification of nuclear tau isoforms in human neuroblastoma cells. Proc Natl Acad Sci USA 87:8422–8426
Lopes S, Lopes A, Pinto V, Guimarães MR, Sardinha VM, Duarte-Silva S et al (2016) Absence of tau triggers age-dependent sciatic nerve morphofunctional deficits and motor impairment. Aging Cell 15:208–216. https://doi.org/10.1111/acel.12391
López-Toledano MA, Shelanski ML (2004) Neurogenic effect of beta-amyloid peptide in the development of neural stem cells. J Neurosci Off J Soc Neurosci 24:5439–5444. https://doi.org/10.1523/JNEUROSCI.0974-04.2004
LoPresti P (2002) Regulation and differential expression of tau mRNA isoforms as oligodendrocytes mature in vivo: implications for myelination. Glia 37:250–257. https://doi.org/10.1002/glia.10035
LoPresti P (2015) Inducible expression of a truncated form of tau in oligodendrocytes elicits gait abnormalities and a decrease in myelin: implications for selective CNS degenerative diseases. Neurochem Res 40:2188–2199. https://doi.org/10.1007/s11064-015-1707-x
Lu Y, He H-J, Zhou J, Miao J-Y, Lu J, He Y-G et al (2013) Hyperphosphorylation results in tau dysfunction in DNA folding and protection. J Alzheimers Dis 37:551–563. https://doi.org/10.3233/JAD-130602
Lukiw WJ, Cui JG, Yuan LY, Bhattacharjee PS, Corkern M, Clement C et al (2010) Acyclovir or Aβ42 peptides attenuate HSV-1-induced miRNA-146a levels in human primary brain cells. NeuroReport 21:922–927. https://doi.org/10.1097/WNR.0b013e32833da51a
Luna S, Cameron DJ, Ethell DW (2013) Amyloid-β and APP deficiencies cause severe cerebrovascular defects: important work for an old villain. PLoS ONE 8:e75052. https://doi.org/10.1371/journal.pone.0075052
Ma Q-L, Zuo X, Yang F, Ubeda OJ, Gant DJ, Alaverdyan M et al (2014) Loss of MAP function leads to hippocampal synapse loss and deficits in the morris water maze with aging. J Neurosci 34:7124–7136. https://doi.org/10.1523/JNEUROSCI.3439-13.2014
Maina MB, Bailey LJ, Wagih S, Biasetti L, Pollack SJ, Quinn JP et al (2018) The involvement of tau in nucleolar transcription and the stress response. Acta Neuropathol Commun 6:70. https://doi.org/10.1186/s40478-018-0565-6
Mann DMA, Davidson YS, Robinson AC, Allen N, Hashimoto T, Richardson A et al (2018) Patterns and severity of vascular amyloid in Alzheimer’s disease associated with duplications and missense mutations in APP gene, Down syndrome and sporadic Alzheimer’s disease. Acta Neuropathol (Berl) 136:569–587. https://doi.org/10.1007/s00401-018-1866-3
Mannix RC, Zhang J, Berglass J, Qui J, Whalen MJ (2013) Beneficial effect of amyloid beta after controlled cortical impact. Brain Inj 27:743–748. https://doi.org/10.3109/02699052.2013.771797
Mannix RC, Zhang J, Park J, Lee C, Whalen MJ (2011) Detrimental effect of genetic inhibition of B-site APP-cleaving enzyme 1 on functional outcome after controlled cortical impact in young adult mice. J Neurotrauma 28:1855–1861. https://doi.org/10.1089/neu.2011.1759
Mansuroglu Z, Benhelli-Mokrani H, Marcato V, Sultan A, Violet M, Chauderlier A et al (2016) Loss of Tau protein affects the structure, transcription and repair of neuronal pericentromeric heterochromatin. Sci Rep 6:33047. https://doi.org/10.1038/srep33047
Marciniak E, Leboucher A, Caron E, Ahmed T, Tailleux A, Dumont J et al (2017) Tau deletion promotes brain insulin resistance. J Exp Med 214:2257–2269. https://doi.org/10.1084/jem.20161731
Masters CL, Simms G, Weinman NA, Multhaup G, McDonald BL, Beyreuther K (1985) Amyloid plaque core protein in Alzheimer disease and Down syndrome. Proc Natl Acad Sci USA 82:4245–4249. https://doi.org/10.1073/pnas.82.12.4245
Mazzon G, Menichelli A, Fabretto A, Cattaruzza T, Manganotti P (2018) A new MAPT deletion in a case of speech apraxia leading to corticobasal syndrome. Neurocase 24:140–144. https://doi.org/10.1080/13554794.2018.1492729
McAleese KE, Firbank M, Dey M, Colloby SJ, Walker L, Johnson M et al (2015) Cortical tau load is associated with white matter hyperintensities. Acta Neuropathol Commun. https://doi.org/10.1186/s40478-015-0240-0
McKhann GM, Knopman DS, Chertkow H, Hyman BT, Jack CR, Kawas CH et al (2011) The diagnosis of dementia due to Alzheimer’s disease: Recommendations from the National Institute on Aging-Alzheimer’s Association workgroups on diagnostic guidelines for Alzheimer’s disease. Alzheimers Dement J Alzheimers Assoc 7:263–269. https://doi.org/10.1016/j.jalz.2011.03.005
McNay EC, Ong CT, McCrimmon RJ, Cresswell J, Bogan JS, Sherwin RS (2010) Hippocampal memory processes are modulated by insulin and high-fat-induced insulin resistance. Neurobiol Learn Mem 93:546–553. https://doi.org/10.1016/j.nlm.2010.02.002
Meakin PJ, Coull BM, Tuharska Z, McCaffery C, Akoumianakis I, Antoniades C et al (2020) Elevated circulating amyloid concentrations in obesity and diabetes promote vascular dysfunction. J Clin Invest. https://doi.org/10.1172/JCI122237
Meakin PJ, Harper AJ, Hamilton DL, Gallagher J, McNeilly AD, Burgess LA et al (2012) Reduction in BACE1 decreases body weight, protects against diet-induced obesity and enhances insulin sensitivity in mice. Biochem J 441:285–296. https://doi.org/10.1042/BJ20110512
Mendez M, Lim G (2003) Seizures in elderly patients with dementia: epidemiology and management. Drugs Aging 20:791–803. https://doi.org/10.2165/00002512-200320110-00001
Merchán-Rubira J, Sebastián-Serrano Á, Díaz-Hernández M, Avila J, Hernández F (2019) Peripheral nervous system effects in the PS19 tau transgenic mouse model of tauopathy. Neurosci Lett 698:204–208. https://doi.org/10.1016/j.neulet.2019.01.031
Mimori K, Sadanaga N, Yoshikawa Y, Ishikawa K, Hashimoto M, Tanaka F et al (2006) Reduced tau expression in gastric cancer can identify candidates for successful Paclitaxel treatment. Br J Cancer 94:1894–1897. https://doi.org/10.1038/sj.bjc.6603182
Miyasaka T, Sato S, Tatebayashi Y, Takashima A (2010) Microtubule destruction induces tau liberation and its subsequent phosphorylation. FEBS Lett 584:3227–3232. https://doi.org/10.1016/j.febslet.2010.06.014
Moir RD, Lathe R, Tanzi RE (2018) The antimicrobial protection hypothesis of Alzheimer’s disease. Alzheimers Dement 14:1602–1614. https://doi.org/10.1016/j.jalz.2018.06.3040
Morgan D, Munireddy S, Alamed J, DeLeon J, Diamond DM, Bickford P et al (2008) Apparent behavioral benefits of tau overexpression in P301L tau transgenic mice. J Alzheimers Dis JAD 15:605–614
Mori H, Takio K, Ogawara M, Selkoe DJ (1992) Mass spectrometry of purified amyloid beta protein in Alzheimer’s disease. J Biol Chem 267:17082–17086
Morley JE, Farr SA, Banks WA, Johnson SN, Yamada KA, Xu L (2010) A physiological role for amyloid-beta protein:enhancement of learning and memory. J Alzheimers Dis JAD 19:441–449. https://doi.org/10.3233/JAD-2009-1230
Morris M, Hamto P, Adame A, Devidze N, Masliah E, Mucke L (2013) Age-appropriate cognition and subtle dopamine-independent motor deficits in aged tau knockout mice. Neurobiol Aging 34:1523–1529. https://doi.org/10.1016/j.neurobiolaging.2012.12.003
Mukaetova-Ladinska EB, Harrington CR, Roth M, Wischik CM (1996) Alterations in tau protein metabolism during normal aging. Dement Basel Switz 7:95–103. https://doi.org/10.1159/000106861
Musicco M, Adorni F, Di Santo S, Prinelli F, Pettenati C, Caltagirone C et al (2013) Inverse occurrence of cancer and Alzheimer disease: a population-based incidence study. Neurology 81:322–328. https://doi.org/10.1212/WNL.0b013e31829c5ec1
Neve RL, Harris P, Kosik KS, Kurnit DM, Donlon TA (1986) Identification of cDNA clones for the human microtubule-associated protein tau and chromosomal localization of the genes for tau and microtubule-associated protein 2. Mol Brain Res 1:271–280. https://doi.org/10.1016/0169-328X(86)90033-1
Nguyen T-VV, Hayes M, Zbesko JC, Frye JB, Congrove NR, Belichenko NP et al (2018) Alzheimer’s associated amyloid and tau deposition co-localizes with a homeostatic myelin repair pathway in two mouse models of post-stroke mixed dementia. Acta Neuropathol Commun 6:100. https://doi.org/10.1186/s40478-018-0603-4
Nieto A, de Garcini EM, Avila J (1989) Altered levels of microtubule proteins in brains of Alzheimer’s disease patients. Acta Neuropathol (Berl) 78:47–51. https://doi.org/10.1007/BF00687401
Niewidok B, Igaev M, Sündermann F, Janning D, Bakota L, Brandt R (2016) Presence of a carboxy-terminal pseudorepeat and disease-like pseudohyperphosphorylation critically influence tau’s interaction with microtubules in axon-like processes. Mol Biol Cell 27:3537–3549. https://doi.org/10.1091/mbc.E16-06-0402
Nunomura A, Perry G, Aliev G, Hirai K, Takeda A, Balraj EK et al (2001) Oxidative damage is the earliest event in Alzheimer disease. J Neuropathol Exp Neurol 60:759–767. https://doi.org/10.1093/jnen/60.8.759
Ortiz-Sanz C, Gaminde-Blasco A, Valero J, Bakota L, Brandt R, Zugaza JL et al (2020) Early effects of Aβ oligomers on dendritic spine dynamics and arborization in hippocampal neurons. Front Synaptic Neurosci. https://doi.org/10.3389/fnsyn.2020.00002
Pajoohesh-Ganji A, Burns MP, Pal-Ghosh S, Tadvalkar G, Hokenbury NG, Stepp MA et al (2014) Inhibition of amyloid precursor protein secretases reduces recovery after spinal cord injury. Brain Res 1560:73–82. https://doi.org/10.1016/j.brainres.2014.02.049
Pallas-Bazarra N, Draffin J, Cuadros R, Antonio Esteban J, Avila J (2019) Tau is required for the function of extrasynaptic NMDA receptors. Sci Rep. https://doi.org/10.1038/s41598-019-45547-8
Pallas-Bazarra N, Jurado-Arjona J, Navarrete M, Esteban JA, Hernández F, Ávila J et al (2016) Novel function of tau in regulating the effects of external stimuli on adult hippocampal neurogenesis. EMBO J 35:1417–1436. https://doi.org/10.15252/embj.201593518
Pandey P, Sliker B, Peters HL, Tuli A, Herskovitz J, Smits K et al (2016) Amyloid precursor protein and amyloid precursor-like protein 2 in cancer. Oncotarget 7:19430–19444. https://doi.org/10.18632/oncotarget.7103
Papegaey A, Eddarkaoui S, Deramecourt V, Fernandez-Gomez F-J, Pantano P, Obriot H et al (2016) Reduced tau protein expression is associated with frontotemporal degeneration with progranulin mutation. Acta Neuropathol Commun. https://doi.org/10.1186/s40478-016-0345-0
Paris D, Ganey N, Banasiak M, Laporte V, Patel N, Mullan M et al (2010) Impaired orthotopic glioma growth and vascularization in transgenic mouse models of Alzheimer’s disease. J Neurosci Off J Soc Neurosci 30:11251–11258. https://doi.org/10.1523/JNEUROSCI.2586-10.2010
Paris D, Townsend K, Quadros A, Humphrey J, Sun J, Brem S et al (2004) Inhibition of angiogenesis by Abeta peptides. Angiogenesis 7:75–85. https://doi.org/10.1023/B:AGEN.0000037335.17717.bf
Pavliukeviciene B, Zentelyte A, Jankunec M, Valiuliene G, Talaikis M, Navakauskiene R et al (2019) Amyloid β oligomers inhibit growth of human cancer cells. PLoS ONE. https://doi.org/10.1371/journal.pone.0221563
Penninkilampi R, Brothers HM, Eslick GD (2017) Safety and Efficacy of Anti-Amyloid-β Immunotherapy in Alzheimer’s Disease: A Systematic Review and Meta-Analysis. J Neuroimmune Pharmacol Off J Soc NeuroImmune Pharmacol 12:194–203. https://doi.org/10.1007/s11481-016-9722-5
Peters F, Salihoglu H, Rodrigues E, Herzog E, Blume T, Filser S et al (2018) BACE1 inhibition more effectively suppresses initiation than progression of β-amyloid pathology. Acta Neuropathol (Berl) 135:695–710. https://doi.org/10.1007/s00401-017-1804-9
Pickett EK, Herrmann AG, McQueen J, Abt K, Dando O, Tulloch J et al (2019) Amyloid beta and tau cooperate to cause reversible behavioral and transcriptional deficits in a model of Alzheimer’s disease. Cell Rep 29:3592–3604.e5. https://doi.org/10.1016/j.celrep.2019.11.044
Pigoni M, Wanngren J, Kuhn P-H, Munro KM, Gunnersen JM, Takeshima H et al (2016) Seizure protein 6 and its homolog seizure 6-like protein are physiological substrates of BACE1 in neurons. Mol Neurodegener 11:67. https://doi.org/10.1186/s13024-016-0134-z
Pooler AM, Phillips EC, Lau DHW, Noble W, Hanger DP (2013) Physiological release of endogenous tau is stimulated by neuronal activity. EMBO Rep 14:389–394. https://doi.org/10.1038/embor.2013.15
Prezel E, Elie A, Delaroche J, Stoppin-Mellet V, Bosc C, Serre L et al (2018) Tau can switch microtubule network organizations: from random networks to dynamic and stable bundles. Mol Biol Cell 29:154–165. https://doi.org/10.1091/mbc.E17-06-0429
Puzzo D, Argyrousi EK, Staniszewski A, Zhang H, Calcagno E, Zuccarello E et al (2020) Tau is not necessary for amyloid-beta-induced synaptic and memory impairments. J Clin Invest. https://doi.org/10.1172/JCI137040
Puzzo D, Privitera L, Fa M, Staniszewski A, Hashimoto G, Aziz F et al (2011) Endogenous amyloid-β is necessary for hippocampal synaptic plasticity and memory. Ann Neurol 69:819–830. https://doi.org/10.1002/ana.22313
Puzzo D, Privitera L, Leznik E, Fà M, Staniszewski A, Palmeri A et al (2008) Picomolar amyloid-beta positively modulates synaptic plasticity and memory in hippocampus. J Neurosci Off J Soc Neurosci 28:14537–14545. https://doi.org/10.1523/JNEUROSCI.2692-08.2008
Qi Z, Wang G, Xia P, Hou T, Zhou H, Wang T et al (2016) Effects of microtubule-associated protein tau expression on neural stem cell migration after spinal cord injury. Neural Regen Res 11:332–337. https://doi.org/10.4103/1673-5374.177744
Qiang L, Sun X, Austin TO, Muralidharan H, Jean DC, Liu M et al (2018) Tau does not stabilize axonal microtubules but rather enables them to have long labile domains. Curr Biol CB 28:2181–2189.e4. https://doi.org/10.1016/j.cub.2018.05.045
Qiang L, Yu W, Andreadis A, Luo M, Baas PW (2006) Tau protects microtubules in the axon from severing by katanin. J Neurosci 26:3120–3129. https://doi.org/10.1523/JNEUROSCI.5392-05.2006
Quintela-López T, Ortiz-Sanz C, Serrano-Regal MP, Gaminde-Blasco A, Valero J, Baleriola J et al (2019) Aβ oligomers promote oligodendrocyte differentiation and maturation via integrin β1 and Fyn kinase signaling. Cell Death Dis 10:1–16. https://doi.org/10.1038/s41419-019-1636-8
Rady RM, Zinkowski RP, Binder LI (1995) Presence of tau in isolated nuclei from human brain. Neurobiol Aging 16:479–486. https://doi.org/10.1016/0197-4580(95)00023-8
Ramirez-Rios S, Denarier E, Prezel E, Vinit A, Stoppin-Mellet V, Devred F et al (2016) Tau antagonizes end-binding protein tracking at microtubule ends through a phosphorylation-dependent mechanism. Mol Biol Cell 27:2924–2934. https://doi.org/10.1091/mbc.E16-01-0029
Regan P, Piers T, Yi J-H, Kim D-H, Huh S, Park SJ et al (2015) Tau phosphorylation at serine 396 residue is required for hippocampal LTD. J Neurosci Off J Soc Neurosci 35:4804–4812. https://doi.org/10.1523/JNEUROSCI.2842-14.2015
Roberson ED, Scearce-Levie K, Palop JJ, Yan F, Cheng IH, Wu T et al (2007) Reducing endogenous tau ameliorates amyloid beta-induced deficits in an Alzheimer’s disease mouse model. Science 316:750–754. https://doi.org/10.1126/science.1141736
Robinson SR, Bishop GM (2002) Aβ as a bioflocculant: implications for the amyloid hypothesis of Alzheimer’s disease. Neurobiol Aging 23:1051–1072. https://doi.org/10.1016/S0197-4580(01)00342-6
Roe CM, Fitzpatrick AL, Xiong C, Sieh W, Kuller L, Miller JP et al (2010) Cancer linked to Alzheimer disease but not vascular dementia. Neurology 74:106–112. https://doi.org/10.1212/WNL.0b013e3181c91873
Rossi G, Conconi D, Panzeri E, Redaelli S, Piccoli E, Paoletta L et al (2013) Mutations in MAPT gene cause chromosome instability and introduce copy number variations widely in the genome. J Alzheimers Dis JAD 33:969–982. https://doi.org/10.3233/JAD-2012-121633
Rossi G, Redaelli V, Contiero P, Fabiano S, Tagliabue G, Perego P et al (2018) Tau mutations serve as a novel risk factor for cancer. Cancer Res 78:3731–3739. https://doi.org/10.1158/0008-5472.CAN-17-3175
Rovelet-Lecrux A, Lecourtois M, Thomas-Anterion C, Ber IL, Brice A, Frebourg T et al (2009) Partial deletion of the MAPT gene: A novel mechanism of FTDP-17. Hum Mutat 30:E591–E602. https://doi.org/10.1002/humu.20979
Russell CL, Semerdjieva S, Empson RM, Austen BM, Beesley PW, Alifragis P (2012) Amyloid-β Acts as a regulator of neurotransmitter release disrupting the interaction between synaptophysin and VAMP2. PLoS ONE 7:e43201. https://doi.org/10.1371/journal.pone.0043201
Samra EB, Buhagiar-Labarchède G, Machon C, Guitton J, Onclercq-Delic R et al (2017) A role for Tau protein in maintaining ribosomal DNA stability and cytidine deaminase-deficient cell survival. Nat Commun 8:1–14. https://doi.org/10.1038/s41467-017-00633-1
Sapir T, Frotscher M, Levy T, Mandelkow E-M, Reiner O (2012) Tau’s role in the developing brain: implications for intellectual disability. Hum Mol Genet 21:1681–1692. https://doi.org/10.1093/hmg/ddr603
Seabrook GR, Smith DW, Bowery BJ, Easter A, Reynolds T, Fitzjohn SM et al (1999) Mechanisms contributing to the deficits in hippocampal synaptic plasticity in mice lacking amyloid precursor protein. Neuropharmacology 38:349–359. https://doi.org/10.1016/s0028-3908(98)00204-4
Seblova D, Quiroga ML, Fors S, Johnell K, Lövdén M, de Leon AP et al (2018) Thirty-year trends in dementia: a nationwide population study of Swedish inpatient records. Clin Epidemiol 10:1679–1693. https://doi.org/10.2147/CLEP.S178955
Seiberlich V, Bauer NG, Schwarz L, Ffrench-Constant C, Goldbaum O, Richter-Landsberg C (2015) Downregulation of the microtubule associated protein tau impairs process outgrowth and myelin basic protein mRNA transport in oligodendrocytes. Glia 63:1621–1635. https://doi.org/10.1002/glia.22832
Shankar GM, Bloodgood BL, Townsend M, Walsh DM, Selkoe DJ, Sabatini BL (2007) Natural oligomers of the Alzheimer amyloid-β protein induce reversible synapse loss by modulating an NMDA-type glutamate receptor-dependent signaling pathway. J Neurosci 27:2866–2875. https://doi.org/10.1523/JNEUROSCI.4970-06.2007
Shaw-Smith C, Pittman AM, Willatt L, Martin H, Rickman L, Gribble S et al (2006) Microdeletion encompassing MAPT at chromosome 17q21.3 is associated with developmental delay and learning disability. Nat Genet 38:1032–1037. https://doi.org/10.1038/ng1858
Siahaan V, Krattenmacher J, Hyman AA, Diez S, Hernández-Vega A et al (2019) Kinetically distinct phases of tau on microtubules regulate kinesin motors and severing enzymes. Nat Cell Biol 21:1086–1092. https://doi.org/10.1038/s41556-019-0374-6
Siano G, Varisco M, Caiazza MC, Quercioli V, Mainardi M, Ippolito C et al (2019) Tau modulates VGluT1 expression. J Mol Biol 431:873–884. https://doi.org/10.1016/j.jmb.2019.01.023
Smith MA, Casadesus G, Joseph JA, Perry G (2002) Amyloid-beta and tau serve antioxidant functions in the aging and Alzheimer brain. Free Radic Biol Med 33:1194–1199. https://doi.org/10.1016/s0891-5849(02)01021-3
Soscia SJ, Kirby JE, Washicosky KJ, Tucker SM, Ingelsson M, Hyman B et al (2010) The Alzheimer’s disease-associated amyloid β-protein is an antimicrobial peptide. PLoS ONE. https://doi.org/10.1371/journal.pone.0009505
Sotiropoulos I, Lopes AT, Pinto V, Lopes S, Carlos S, Duarte-Silva S et al (2014) Selective impact of Tau loss on nociceptive primary afferents and pain sensation. Exp Neurol 261:486–493. https://doi.org/10.1016/j.expneurol.2014.07.008
Sotthibundhu A, Li Q-X, Thangnipon W, Coulson EJ (2009) Abeta(1–42) stimulates adult SVZ neurogenesis through the p75 neurotrophin receptor. Neurobiol Aging 30:1975–1985. https://doi.org/10.1016/j.neurobiolaging.2008.02.004
Southam KA, Stennard F, Pavez C, Small DH (2019) Knockout of Amyloid β Protein Precursor (APP) expression alters synaptogenesis, neurite branching and axonal morphology of hippocampal neurons. Neurochem Res 44:1346–1355. https://doi.org/10.1007/s11064-018-2512-0
Sperling R, Salloway S, Brooks DJ, Tampieri D, Barakos J, Fox NC et al (2012) Amyloid-related imaging abnormalities in patients with Alzheimer’s disease treated with bapineuzumab: a retrospective analysis. Lancet Neurol 11:241–249. https://doi.org/10.1016/S1474-4422(12)70015-7
Spires-Jones TL, Attems J, Thal DR (2017) Interactions of pathological proteins in neurodegenerative diseases. Acta Neuropathol (Berl) 134:187–205. https://doi.org/10.1007/s00401-017-1709-7
Stamer K, Vogel R, Thies E, Mandelkow E, Mandelkow E-M (2002) Tau blocks traffic of organelles, neurofilaments, and APP vesicles in neurons and enhances oxidative stress. J Cell Biol 156:1051–1063. https://doi.org/10.1083/jcb.200108057
Steinbach JP, Müller U, Leist M, Li ZW, Nicotera P, Aguzzi A (1998) Hypersensitivity to seizures in beta-amyloid precursor protein deficient mice. Cell Death Differ 5:858–866. https://doi.org/10.1038/sj.cdd.4400391
Suberbielle E, Sanchez PE, Kravitz AV, Wang X, Ho K, Eilertson K et al (2013) Physiological brain activity causes DNA double strand breaks in neurons — exacerbation by amyloid-β. Nat Neurosci 16:613–621. https://doi.org/10.1038/nn.3356
Sudo H, Baas PW (2011) Strategies for diminishing katanin-based loss of microtubules in tauopathic neurodegenerative diseases. Hum Mol Genet 20:763–778. https://doi.org/10.1093/hmg/ddq521
Sultan A, Nesslany F, Violet M, Bégard S, Loyens A, Talahari S et al (2011) Nuclear tau, a key player in neuronal DNA protection. J Biol Chem 286:4566–4575. https://doi.org/10.1074/jbc.M110.199976
Sündermann F, Fernandez M-P, Morgan RO (2016) An evolutionary roadmap to the microtubule-associated protein MAP Tau. BMC Genom. https://doi.org/10.1186/s12864-016-2590-9
Sweeney MD, Sagare AP, Zlokovic BV (2018) Blood–brain barrier breakdown in Alzheimer’s disease and other neurodegenerative disorders. Nat Rev Neurol 14:133–150. https://doi.org/10.1038/nrneurol.2017.188
Tai C, Chang C-W, Yu G-Q, Lopez I, Yu X, Wang X et al (2020) Tau reduction prevents key features of autism in mouse models. Neuron. https://doi.org/10.1016/j.neuron.2020.01.038
Tai H-C, Serrano-Pozo A, Hashimoto T, Frosch MP, Spires-Jones TL, Hyman BT (2012) The synaptic accumulation of hyperphosphorylated tau oligomers in alzheimer disease is associated with dysfunction of the ubiquitin-proteasome system. Am J Pathol 181:1426–1435. https://doi.org/10.1016/j.ajpath.2012.06.033
Takahata K, Kimura Y, Sahara N, Koga S, Shimada H, Ichise M et al (2019) PET-detectable tau pathology correlates with long-term neuropsychiatric outcomes in patients with traumatic brain injury. Brain J Neurol 142:3265–3279. https://doi.org/10.1093/brain/awz238
Takei Y, Teng J, Harada A, Hirokawa N (2000) Defects in axonal elongation and neuronal migration in mice with disrupted tau and map1b genes. J Cell Biol 150:989–1000. https://doi.org/10.1083/jcb.150.5.989
Tampellini D, Rahman N, Gallo EF, Huang Z, Dumont M, Capetillo-Zarate E et al (2009) Synaptic activity reduces intraneuronal Abeta, promotes APP transport to synapses, and protects against Abeta-related synaptic alterations. J Neurosci Off J Soc Neurosci 29:9704–9713. https://doi.org/10.1523/JNEUROSCI.2292-09.2009
Tan DCS, Yao S, Ittner A, Bertz J, Ke YD, Ittner LM et al (2018) Generation of a new tau knockout (tau Δex1) line using CRISPR/Cas9 genome editing in mice. J Alzheimers Dis 62:571–578. https://doi.org/10.3233/JAD-171058
Tan R, Lam AJ, Tan T, Han J, Nowakowski DW, Vershinin M et al (2019) Microtubules gate tau condensation to spatially regulate microtubule functions. Nat Cell Biol 21:1078–1085. https://doi.org/10.1038/s41556-019-0375-5
Tan XL, Zheng P, Wright DK, Sun M, Brady RD, Liu S et al (2020) The genetic ablation of tau improves long-term, but not short-term, functional outcomes after experimental traumatic brain injury in mice. Brain Inj 34:131–139. https://doi.org/10.1080/02699052.2019.1667539
Tanzi RE, Gusella JF, Watkins PC, Bruns GA, St George-Hyslop P, Van Keuren ML et al (1987) Amyloid beta protein gene: cDNA, mRNA distribution, and genetic linkage near the Alzheimer locus. Science 235:880–884. https://doi.org/10.1126/science.2949367
Terry RD, Masliah E, Salmon DP, Butters N, DeTeresa R, Hill R et al (1991) Physical basis of cognitive alterations in Alzheimer’s disease: synapse loss is the major correlate of cognitive impairment. Ann Neurol 30:572–580. https://doi.org/10.1002/ana.410300410
Tharp WG, Sarkar IN (2013) Origins of amyloid-β. BMC Genomics 14:290. https://doi.org/10.1186/1471-2164-14-290
Thompson HJ, McCormick WC, Kagan SH (2006) Traumatic brain injury in older adults: epidemiology, outcomes, and future implications. J Am Geriatr Soc 54:1590–1595. https://doi.org/10.1111/j.1532-5415.2006.00894.x
Tint I, Slaughter T, Fischer I, Black MM (1998) Acute inactivation of tau has no effect on dynamics of microtubules in growing axons of cultured sympathetic neurons. J Neurosci Off J Soc Neurosci 18:8660–8673
Uhlén M, Fagerberg L, Hallström BM, Lindskog C, Oksvold P, Mardinoglu A et al (2015) Tissue-based map of the human proteome. Science. https://doi.org/10.1126/science.1260419
Varela MC, Krepischi-Santos ACV, Paz JA, Knijnenburg J, Szuhai K, Rosenberg C et al (2006) A 17q21.31 microdeletion encompassing the MAPT gene in a mentally impaired patient. Cytogenet Genome Res 114:89–92. https://doi.org/10.1159/000091934
Vassar R (2019) Implications for BACE1 inhibitor clinical trials: adult conditional BACE1 knockout mice exhibit axonal organization defects in the hippocampus. J Prev Alzheimers Dis 6:78–84. https://doi.org/10.14283/jpad.2019.3
Vassar R, Bennett BD, Babu-Khan S, Kahn S, Mendiaz EA, Denis P et al (1999) Beta-secretase cleavage of Alzheimer’s amyloid precursor protein by the transmembrane aspartic protease BACE. Science 286:735–741. https://doi.org/10.1126/science.286.5440.735
Velazquez R, Ferreira E, Tran A, Turner EC, Belfiore R, Branca C et al (2018) Acute tau knockdown in the hippocampus of adult mice causes learning and memory deficits. Aging Cell 17:e12775. https://doi.org/10.1111/acel.12775
Violet M, Delattre L, Tardivel M, Sultan A, Chauderlier A, Caillierez R et al (2014) A major role for Tau in neuronal DNA and RNA protection in vivo under physiological and hyperthermic conditions. Front Cell Neurosci 8:84. https://doi.org/10.3389/fncel.2014.00084
Vossel KA, Zhang K, Brodbeck J, Daub AC, Sharma P, Finkbeiner S et al (2010) Tau reduction prevents Abeta-induced defects in axonal transport. Science 330:198. https://doi.org/10.1126/science.1194653
Wade-Martins R (2012) The MAPT locus—a genetic paradigm in disease susceptibility. Nat Rev Neurol 8:477–478. https://doi.org/10.1038/nrneurol.2012.169
Walsh DM, Klyubin I, Fadeeva JV, Cullen WK, Anwyl R, Wolfe MS et al (2002) Naturally secreted oligomers of amyloid beta protein potently inhibit hippocampal long-term potentiation in vivo. Nature 416:535–539. https://doi.org/10.1038/416535a
Walter S, Jumpertz T, Hüttenrauch M, Ogorek I, Gerber H, Storck SE et al (2019) The metalloprotease ADAMTS4 generates N-truncated Aβ4-x species and marks oligodendrocytes as a source of amyloidogenic peptides in Alzheimer’s disease. Acta Neuropathol (Berl) 137:239–257. https://doi.org/10.1007/s00401-018-1929-5
Wang H, Megill A, Wong PC, Kirkwood A, Lee H-K (2014) Postsynaptic target specific synaptic dysfunctions in the CA3 Area of BACE1 knockout mice. PLoS ONE 9:e92279. https://doi.org/10.1371/journal.pone.0092279
Wang H, Song L, Laird F, Wong PC, Lee H-K (2008) BACE1 knock-outs display deficits in activity-dependent potentiation of synaptic transmission at mossy fiber to ca3 synapses in the hippocampus. J Neurosci 28:8677–8681. https://doi.org/10.1523/JNEUROSCI.2440-08.2008
Wei W, Nguyen LN, Kessels HW, Hagiwara H, Sisodia S, Malinow R (2010) Amyloid beta from axons and dendrites reduces local spine number and plasticity. Nat Neurosci 13:190–196. https://doi.org/10.1038/nn.2476
Wei Y, Qu M-H, Wang X-S, Chen L, Wang D-L, Liu Y et al (2008) Binding to the minor groove of the double-strand, tau protein prevents DNA from damage by peroxidation. PLoS ONE. https://doi.org/10.1371/journal.pone.0002600
Weingarten MD, Lockwood AH, Hwo SY, Kirschner MW (1975) A protein factor essential for microtubule assembly. Proc Natl Acad Sci USA 72:1858–1862
Weinger JG, Davies P, Acker CM, Brosnan CF, Tsiperson V, Bayewitz A et al (2012) Mice devoid of Tau have increased susceptibility to neuronal damage in myelin oligodendrocyte glycoprotein-induced experimental autoimmune encephalomyelitis. J Neuropathol Exp Neurol 71:422–433. https://doi.org/10.1097/NEN.0b013e3182540d2e
Whitson JS, Selkoe DJ, Cotman CW (1989) Amyloid beta protein enhances the survival of hippocampal neurons in vitro. Science 243:1488–1490. https://doi.org/10.1126/science.2928783
Wijesekara N, Gonçalves RA, Ahrens R, De Felice FG, Fraser PE (2018) Tau ablation in mice leads to pancreatic β cell dysfunction and glucose intolerance. FASEB J 32:3166–3173. https://doi.org/10.1096/fj.201701352
Willem M, Garratt AN, Novak B, Citron M, Kaufmann S, Rittger A et al (2006) Control of peripheral nerve myelination by the ß-secretase BACE1. Science 314:664–666. https://doi.org/10.1126/science.1132341
Wu Y-H, Swaab DF (2007) Disturbance and strategies for reactivation of the circadian rhythm system in aging and Alzheimer’s disease. Sleep Med 8:623–636. https://doi.org/10.1016/j.sleep.2006.11.010
Wu Z, Wang Z-H, Liu X, Zhang Z, Gu X, Yu SP et al (2020) Traumatic brain injury triggers APP and Tau cleavage by delta-secretase, mediating Alzheimer’s disease pathology. Prog Neurobiol 185:101730. https://doi.org/10.1016/j.pneurobio.2019.101730
Xu F, Schillinger JA, Sternberg MR, Johnson RE, Lee FK, Nahmias AJ et al (2002) Seroprevalence and coinfection with herpes simplex virus type 1 and type 2 in the United States, 1988–1994. J Infect Dis 185:1019–1024. https://doi.org/10.1086/340041
Yaghoobi H, Azizi H, Banitalebi-Dehkordi M, Mohammad Rezaei F, Arsang-Jnag S, Taheri M et al (2019) Beta-secretase 1 (BACE1) is down-regulated in invasive ductal carcinoma of breast. Rep Biochem Mol Biol 8:200–207
Yi S, Liu Q, Wang X, Qian T, Wang H, Zha G et al (2019) Tau modulates Schwann cell proliferation, migration and differentiation following peripheral nerve injury. J Cell Sci. https://doi.org/10.1242/jcs.222059
Yiannopoulou KG, Papageorgiou SG (2020) Current and future treatments in Alzheimer disease: an update. J Cent Nerv Syst Dis. https://doi.org/10.1177/1179573520907397
Yu W, Qiang L, Solowska JM, Karabay A, Korulu S, Baas PW (2008) The microtubule-severing proteins spastin and katanin participate differently in the formation of axonal branches. Mol Biol Cell 19:1485–1498. https://doi.org/10.1091/mbc.e07-09-0878
Yuan A, Kumar A, Peterhoff C, Duff K, Nixon RA (2008) Axonal transport rates in vivo are unaffected by tau deletion or overexpression in mice. J Neurosci 28:1682–1687. https://doi.org/10.1523/JNEUROSCI.5242-07.2008
Zempel H, Luedtke J, Kumar Y, Biernat J, Dawson H, Mandelkow E et al (2013) Amyloid-beta oligomers induce synaptic damage via Tau-dependent microtubule severing by TTLL6 and spastin. Embo J 32:2920–2937. https://doi.org/10.1038/emboj.2013.207
Zhang M, Zhang J, Zhang W, Yao Z (2018) Demyelination takes place prior to neuronal damage following intracerebroventricular injection of amyloid beta oligomer. Neuropsychiatry 8:1770–1785. https://doi.org/10.4172/Neuropsychiatry.1000519
Zhang Y, Walter R, Ng P, Luong PN, Dutt S, Heuer H et al (2016) Progression of microstructural degeneration in progressive supranuclear palsy and corticobasal syndrome: a longitudinal diffusion tensor imaging study. PLoS ONE. https://doi.org/10.1371/journal.pone.0157218
Zhao G, Cui M-Z, Mao G, Dong Y, Tan J, Sun L et al (2005) gamma-Cleavage is dependent on zeta-cleavage during the proteolytic processing of amyloid precursor protein within its transmembrane domain. J Biol Chem 280:37689–37697. https://doi.org/10.1074/jbc.M507993200
Zhou L, McInnes J, Wierda K, Holt M, Herrmann AG, Jackson RJ et al (2017) Tau association with synaptic vesicles causes presynaptic dysfunction. Nat Commun 8:15295. https://doi.org/10.1038/ncomms15295
Zhukareva V, Sundarraj S, Mann D, Sjogren M, Blenow K, Clark CM et al (2003) Selective reduction of soluble tau proteins in sporadic and familial frontotemporal dementias: an international follow-up study. Acta Neuropathol (Berl) 105:469–476. https://doi.org/10.1007/s00401-002-0668-8
Zou C, Montagna E, Shi Y, Peters F, Blazquez-Llorca L, Shi S et al (2015) Intraneuronal APP and extracellular Aβ independently cause dendritic spine pathology in transgenic mouse models of Alzheimer’s disease. Acta Neuropathol (Berl) 129:909–920. https://doi.org/10.1007/s00401-015-1421-4
Tissue expression of MAPT-Summary-The Human Protein Atlas. https://www.proteinatlas.org/ENSG00000186868-MAPT/tissue. Accessed 23 Jun 2020.
Tissue expression of APP-Summary-The Human Protein Atlas. https://www.proteinatlas.org/ENSG00000142192-APP/tissue. Accessed 23 Jun 2020.
Tissue expression of BACE1-Summary-The Human Protein Atlas. https://www.proteinatlas.org/ENSG00000186318-BACE1/tissue. Accessed 23 Jun 2020.
Tissue expression of PSEN1-Summary-The Human Protein Atlas. https://www.proteinatlas.org/ENSG00000080815-PSEN1/tissue. Accessed 23 Jun 2020.
Acknowledgements
Sarah Kent is a Translational Neuroscience PhD student funded by Wellcome (108890/Z/15/Z). Tara Spires-Jones receives funding from the European Research Council (ERC) under the European Union’s Horizon 2020 research and innovation programme (Grant agreement No. 681181), the UK Dementia Research Institute which receives its funding from DRI Ltd, funded by the UK Medical Research Council, Alzheimer’s Society, and Alzheimer’s Research UK, and industrial collaborative partners (none of whom had any influence over the current paper). Claire Durrant is funded by ARUK Race Against Dementia-Dyson fellowship (RADF2019A-001).
Author information
Authors and Affiliations
Contributions
SAK wrote and edited the manuscript and designed the figures. TLS-J wrote and edited the manuscript. CSD planned, wrote and edited the manuscript, and designed the figures.
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Kent, S.A., Spires-Jones, T.L. & Durrant, C.S. The physiological roles of tau and Aβ: implications for Alzheimer’s disease pathology and therapeutics. Acta Neuropathol 140, 417–447 (2020). https://doi.org/10.1007/s00401-020-02196-w
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00401-020-02196-w