Abstract
Introduction
The frequency of adverse events, such as cerebral ischemia, following traumatic brain injury (TBI) is often debated. Point-in-time monitoring modalities provide important information, but have limited temporal resolution.
Purpose
This study examines the frequency of an adverse event as a point prevalence at 24 and 72 h post-injury, compared with the cumulative burden measured as a frequency of the event over the full duration of monitoring.
Methods
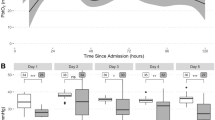
Reduced brain tissue oxygenation (PbtO2 < 10 mmHg) was the adverse event chosen for examination. Data from 100 consecutive children with severe TBI who received PbtO2 monitoring were retrospectively examined, with data from 87 children found suitable for analysis. Hourly recordings were used to identify episodes of PbtO2 less than 10 mmHg, at 24 and 72 h post-injury, and for the full duration of monitoring.
Results
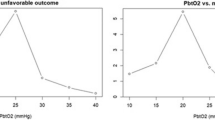
Reduced PbtO2 was more common early than late after injury. The point prevalence of reduced PbtO2 at the selected time points was relatively low (10 % of patients at 24 h and no patients at the 72-h mark post-injury). The cumulative burden of these events over the full duration of monitoring was relatively high: 50 % of patients had episodes of PbtO2 less than 10 mmHg and 88 % had PbtO2 less than 20 mmHg.
Conclusion
Point-in-time monitoring in a dynamic condition like TBI may underestimate the overall frequency of adverse events, like reduced PbtO2, particularly when compared with continuous monitoring, which also has limitations, but provides a dynamic assessment over a longer time period.

Similar content being viewed by others
References
Kochanek PM, Clark RS, Ruppel RA, Dixon EC (2001) Cerebral resuscitation after traumatic brain injury and cardiopulmonary arrest in infants and children in the new millennium. Pediatr Clin North Am 48:661–681
Teasdale GM, Graham DI (1998) Craniocerebral trauma: protection and retrieval of the neuronal population after injury. Neurosurgery 43:723–737
Chestnut R, Marshall LF, Klauber MR, Blunt BA, Baldwin N, Eisenberg HM, Jane JA, Marmarou A, Foulkes MA (1993) The role of secondary brain injury in determining outcome from severe brain injury. J Trauma 34(2):216–222
Bruce DA, Langfitt TW, Miller JD, Schutz H, Vapalahti MP, Stanek A, Goldberg HI (1973) Regional cerebral blood flow, intracranial pressure, and brain metabolism in comatose patients. J Neurosurg 38:131–144
Miller JD (1985) Head injury and brain ischaemia: implications for therapy. Br J Anaesth 57:120–129
Barclay L, Zemcov A, Reichert W, Blass JP (1985) Cerebral blood flow decrements in chronic head injury syndrome. Biol Psychiatry 20:146–157
Graham DI, Adams JH (1971) Ischaemic brain damage in fatal head injuries. Lancet 6:265–266
Graham DI, Ford I, Adams JH, Doyle D, Teasdale GM, Lawrence AE, McLellan DR (1989) Ischaemic brain damage is still common in fatal non-missile head injury. J Neurol Neurosurg Psychiatry 52:346–350
Bouma GJ, Muizelaar JP, Choi SC, Newlon PG, Young HF (1991) Cerebral circulation and metabolism after severe traumatic brain injury: the elusive role of ischemia. J Neurosurg 75:685–693
Yundt KD, Diringer MN (1997) The use of hyperventilation and its impact on cerebral ischemia in the treatment of traumatic brain injury. Crit Care Clin 13:163–184
Vespa P, Bergsneider M, Hattori N, Wu HM, Huang SC, Martin NA, Glenn TC, McArthur DL, Hovda DA (2005) Metabolic crisis without brain ischemia is common after traumatic brain injury: a combined microdialysis and positron emission tomography study. J Cereb Blood Flow Metab 25:763–774
Hlatky R, Valadka AB, Robertson CS (2003) Intracranial hypertension and cerebral ischemia after severe traumatic brain injury. Neurosurg Focus 14(4):1–4, Article 2
Bouma GJ, Muizelaar JP, Stringer WA, Choi SC, Fatouros P, Young HF (1992) Ultra-early evaluation of regional cerebral blood flow in severely head-injured patients using xenon-enhanced computerized tomography. J Neurosurg 77:360–368
Coles JP, Fryer TD, Smielewski P, Chatfield DA, Steiner LA, Johnston AJ, Downey SPMJ, Williams GB, Aigbirhio F, Hutchinson PJ, Rice K, Carpenter TA, Clark JC, Pickard JD, Menon DK (2004) Incidence and mechanisms of cerebral ischemia in early clinical head injury. J Cereb Blood Flow Metab 24:202–211
Sharples PM, Stuart AG, Mathews DSF, Aynsley-Green A, Eyre JA (1995) Cerebral blood flow and metabolism in children with severe head injury. Part I: relation to age, Glasgow coma score, outcome, intracranial pressure, and time after injury. J Neurol Neurosurg Psychiatr 58:145–152
Vigue B, Ract C, Benayed M, Zlotine N, Leblanc PE, Samii K, Bissonnette B (1999) Early SjvO2 monitoring in patients with severe brain trauma. Intensive Care Med 25:445–451
Narotam PK, Morrison JF, Nathoo N (2009) Brain tissue oxygen monitoring in traumatic brain injury and major trauma: outcome analysis of a brain tissue oxygen-directed therapy. J Neurosurg 111:672–682
Adelson PD, Srinivas R, Chang Y, Bell M, Kochanek PM (2011) Cerebrovascular response in children following severe traumatic brain injury. Childs Nerv Syst 27:1465–1476
Valadka AB, Furuya Y, Hlatky R, Robertson CS (2000) Global and regional techniques for monitoring cerebral oxidative metabolism after severe traumatic brain injury. Neurosurg Focus 9(5):1–3
Stocchetti N, Paparella A, Bridelli F, Bacchi M, Piazza P, Zuccoli P (1994) Cerebral venous oxygen saturation studied with bilateral samples in the internal jugular veins. Neurosurgery 34:38–43
Figaji AA (2010) Practical aspects of bedside cerebral hemodynamics monitoring in pediatric TBI. Childs Nerv Syst 26(4):431–439
Adelson PD, Bratton SL, Carney NA, Chestnut RM, du Coudray HE, Goldstein B, Kochanek PM, Miller HC, Partington MD, Selden NR, Warden CR, Wright DW, American Association for Surgery of Trauma, Child Neurology Society, International Society for Pediatric Neurosurgery, International Trauma Anesthesia and Critical Care Society, Society of Critical Care Medicine, World Federation of Pediatric Intensive and Critical Care Societies (2003) Guidelines for the acute medical management of severe traumatic brain injury in infants, children, and adolescents. Chapter 1: introduction. Pediatr Crit Care Med 4(3 Suppl):S2–S4
Adelson PD, Bratton SL, Carney NA, Chestnut RM, du Coudray HE, Goldstein B, Kochanek PM, Miller HC, Partington MD, Selden NR, Warden CR, Wright DW, American Association for Surgery of Trauma, Child Neurology Society, International Society for Pediatric Neurosurgery, International Trauma Anesthesia and Critical Care Society, Society of Critical Care Medicine, World Federation of Pediatric Intensive and Critical Care Societies (2003) Guidelines for the acute medical management of severe traumatic brain injury in infants, children, and adolescents. Chapter 6: threshold for treatment of intracranial hypertension. Pediatr Crit Care Med 4(3 Suppl):S25–S27
Figaji AA, Zwane E, Thompson C, Fieggen AG, Argent AC, Le Roux PD, Peter JC (2009) Brain tissue oxygen tension monitoring in pediatric severe traumatic brain injury: part 1: relationship with outcome. Childs Nerv Syst 25(10):1325–1333
Van den Brink WA, Van Santbrink H, Steyerberg EW, Avezaat CJ, Suazo JAC, Hogesteeger C, Jansen W, Kloos LM, Vermeulen J, Maas AIR (2000) Brain oxygen tension in severe head injury. Neurosurgery 46:868–876
Figaji AA, Fieggen AG, Argent AC, Le Roux PD, Peter JC (2008) Does adherence to treatment targets in children with severe traumatic brain injury avoid brain hypoxia? A brain tissue oxygenation study. Neurosurgery 63:83–91
Kiening KL, Unterberg AW, Bardt TF, Schneider G-H, Lanksch WR (1996) Monitoring of cerebral oxygenation in patients with severe head injuries: brain tissue PO2 versus jugular vein oxygen saturation. J Neurosurg 85:751–757
Dings J, Meixensberger J, Jager A, Roosen K (1998) Clinical experience with 118 brain tissue oxygen partial pressure catheter probes. Neurosurgery 43:1082–1095
Rosenthal G, Hemphill JC, Sorani M, Martin C, Morabito D, Obrist WD, Manley GT (2008) Brain tissue oxygen tension is more indicative of oxygen diffusion than oxygen delivery and metabolism in patients with traumatic brain injury. Crit Care Med 36(6):1917–1924
Van Santbrink H, Maas AI, Avezaat CJ (1996) Continuous monitoring of partial pressure of brain tissue oxygen in patients with severe head injury. Neurosurgery 38(1):21–31
Obrist WD, Thompson HK Jr, King CH, Wang HS (1967) Determination of regional cerebral blood flow by inhalation of 133-xenon. Circ Res 20:124–135
Robertson CS, Narayan RK, Gokaslan ZL, Pahwa R, Grossman RG, Caram P Jr, Allen E (1989) Cerebral arteriovenous oxygen difference as an estimate of cerebral blood flow in comatose patients. J Neurosurg 70:222–230
Figaji AA, Zwane E, Thompson C, Fieggen AG, Argent AC, Le Roux PD, Peter JC (2009) Brain tissue oxygen tension monitoring in pediatric severe traumatic brain injury: part 2: relationship with clinical, physiological, and treatment factors. Childs Nerv Syst 25(10):1335–1343
Scheufler KM, Lehnert A, Rohrborn HJ, Nadstawek J, Thees C (2004) Individual value of brain tissue oxygen pressure, microvascular oxygen saturation, cytochrome redox level, and energy metabolites in detecting critically reduced cerebral energy state during acute changes in global cerebral perfusion. J Neurosurg Anesthesiol 16:210–219
Imberti R, Bellinzona G, Langer M (2002) Cerebral tissue PO2 and SjvO2 changes during moderate hyperventilation in patients with severe traumatic brain injury. J Neurosurg 96:97–102
Robertson CS, Valadka AB, Hannay JH, Contant CF, Gopinath SP, Cormio M, Uzura M, Grossman RG (1999) Prevention of secondary ischemic insults after severe head injury. Crit Care Med 27(10):2086–2095
Stiefel MF, Spiotta A, Gracias VH, Garuffe AM, Guillamondegui O, Maloney-Wilensky E, Bloom S, Grady MS, LeRoux PD (2005) Reduced mortality rate in patients with severe traumatic brain injury treated with brain tissue oxygen monitoring. J Neurosurg 103(5):805–811
Adamides AA, Cooper DJ, Rosenfeldt FL, Bailey MJ, Pratt N, Tippett N, Vallance S, Rosenfeld JV (2009) Focal cerebral oxygenation and neurological outcome with or without brain tissue oxygen-guided therapy in patients with traumatic brain injury. Acta Neurochir (Wien) 151(11):1399–1409
McCarthy MC, Moncrief H, Sands JM, Market RJ, Hall LC, Wenker IC, Anderson HL, Ekeh AP, Walusimbi MS, Woods RJ, Saxe JM, Tchorz KM (2009) Neurological outcomes with cerebral oxygenation monitoring in traumatic brain injury. Surgery 146(4):585–590
Martini RP, Deem S, Yanez ND, Chestnut RM, Weiss NS, Daniel S, Souter M, Treggiari MM (2009) Management guided by brain tissue oxygen monitoring and outcome following severe traumatic brain injury. J Neurosurg 111(4):644–649
Meixensberger J, Jaeger M, Väth A, Dings J, Kunze E, Roosen K (2003) Brain tissue oxygen guided treatment supplementing ICP/CPP therapy after traumatic brain injury. J Neurol Neurosurg Psychiatr 74(6):760–764
Graham DI, Adams JH, Doyle D (1978) Ischaemic brain damage in fatal non-missile head injuries. J Neurol Sci 39:213–234
Schroder M, Muizelaar JP, Kuta A, Choi S (1996) Thresholds for cerebral ischemia after severe head injury: relationship with late CT findings and outcome. J Neurotrauma 13:17–23
Valadka AB, Goodman JC, Gopinath SP, Uzura M, Robertson CS (1998) Comparison of brain tissue oxygen tension to microdialysis-based measures of cerebral ischemia in fatally head-injuried humans. J Neurotrauma 15:509–519
Chestnut RM, Marshall SB, Piek J, Blunt BA, Klauber MR, Marshall LF (1993) Early and late systemic hypotension as a frequent and fundamental source of cerebral ischemia following severe injury in the Traumatic Coma Data Bank. Acta Neurochir Suppl (Wien) 59:121–125
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Padayachy, L.C., Rohlwink, U., Zwane, E. et al. The frequency of cerebral ischemia/hypoxia in pediatric severe traumatic brain injury. Childs Nerv Syst 28, 1911–1918 (2012). https://doi.org/10.1007/s00381-012-1837-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-012-1837-2