Abstract
Objectives
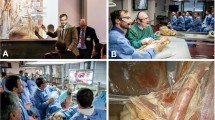
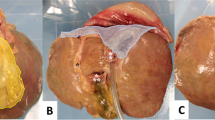
The purpose of this study was to evaluate the feedback of participants upon laparoscopic liver surgery (LLS) course on Thiel-embalmed human bodies.
Methods
From 2010 to 2017, ten LLS masterclasses have been organized by the Department of Hepatobiliary Surgery at Ghent University Hospital. A 23-question anonymous survey was electronically sent to 119 participants between November 2017 and January 2018, exploring their characteristics and asking for evaluation of the course. The obstacles for implementing LLS in their centers have been assessed.
Results
Sixty-four surgeons (53.8%) responded to the survey; 42 (65.6%) were employed at a university hospital; and 39 (60.9%) were in the first decade of their practice as a consultant surgeon. Forty-three (67.2%) surgeons reported an increased percentage of LLS cases afterward. Training on Thiel cadavers was considered superior (49.2%) to other training options including proctoring in the operating room (34.9%), virtual reality (6.3%), video training (4.8%) and practicing on pigs (4.8%). Obstacles identified contained inadequate training, patient’s referral pattern, financial issues, lack of dedicated surgical team and time constrains.
Conclusions
This survey revealed that a structured short-time program incorporating interactive discussion, live operations and hands-on training on human bodies under proctorship may enhance efficient training in laparoscopic liver surgery. In a step forward for upcoming courses, the importance of team building has to be addressed.

Similar content being viewed by others
References
Ciria R, Cherqui D, Geller DA et al (2016) Comparative short-term benefits of laparoscopic liver resection: 9000 cases and climbing. Ann Surg 263(4):761–777
Tomassini F, Scuderi V, Colman R et al (2016) The single surgeon learning curve of laparoscopic liver resection: a continuous evolving process through stepwise difficulties. Medicine (Baltimore) 95(43):5138
Berardi G, Van Cleven S, Fretland AA et al (2017) Evolution of laparoscopic liver surgery from innovation to implementation to mastery: perioperative and oncologic outcomes of 2,238 patients from 4 European specialized centers. J Am Coll Surg 225:639–649
Wakabayashi G, Cherqui D, Geller DA et al (2015) Recommendations for laparoscopic liver resection: a report from the second international consensus conference held in Morioka. Ann Surg 261:619–629
Abu Hilal M, Aldrighetti L, Dagher I et al (2018) The Southampton consensus guidelines for laparoscopic liver surgery: from indication to implementation. Ann Surg 268(1):11–18
Jrearz R, Govindarajan A, Jayaraman S (2017) A survey of current practices and barriers to expanding laparoscopic HPB surgery in Canada. HPB (Oxford) 19(1):42–46
Vigano L, Laurent A, Tayar C et al (2009) The learning curve in laparoscopic liver resection: improved feasibility and reproducibility. Ann Surg 250(5):772–782
Hasegawa Y, Nitta H, Takahara T et al (2017) Safely extending the indications of laparoscopic liver resection: when should we start laparoscopic major hepatectomy? Surg Endosc 31:309–316
Halls MC, Alseidi A, Berardi G et al (2019) A comparison of the learning curves of laparoscopic liver surgeons in differing stages of the IDEAL paradigm of surgical innovation: standing on the shoulders of pioneers. Ann Surg 269(2):221–228
Strickland A, Fairhurst K, Lauder C et al (2011) Development of an ex vivo simulated training model for laparoscopic liver resection. Surg Endosc 25(5):1677–1682
Xiao J, Cui Z, Fu M et al (2016) An ex vivo liver training model continuously perfused to simulate bleeding for suture skills involved in laparoscopic liver resection: development and validity. Surg Endosc 30(10):4553–4561
Komorowski AL, Mituś JW, Sanchez Hurtado MA et al (2015) Porcine model in the laparoscopic liver surgery training. Pol Przegl Chir 87(8):425–428
Teh SH, Hunter JG, Sheppard BC (2007) A suitable animal model for laparoscopic hepatic resection training. Surg Endosc 21:1738–1744
Udomsawaengsup S, Pattana-arun J, Tansatit T et al (2005) Minimally invasive surgery training in soft cadaver (MIST-SC). J Med Assoc Thail 88:189–194
White SA, Satchidanand RY, French JJ et al (2014) A cadaver lab training facility to facilitate laparoscopic liver resection. Surg Laparosc Endosc Percutaneous Tech 24:357–360
Nobuoka D, Yagi T, Kondo Y et al (2017) The utility of cadaver-based surgical training in hepatobiliary and pancreatic surgery. J Hepato Biliary Pancreat Sci 24:A338
Bates R (2004) A critical analysis of evaluation practice: the Kirkpatrick model and the principle of beneficence. Eval Program Plan 27:341–347
Cai XJ, Li ZY, Zhang YL et al (2014) Laparoscopic liver resection and the learning curve: a 14-year, single-center experience. Surg Endosc 28:1334–1341
Nomi T, Fuks D, Kawaguchi Y et al (2015) Learning curve for laparoscopic major hepatectomy. Br J Surg 102:796–804
Chang YJ, Mittal VK (2009) Hepato-pancreato-biliary training in general surgery residency: is it enough for the real world? Am J Surg 197(3):291–295
Subhas G, Mittal VK (2011) Training minimal invasive approaches in hepatopancreatobilliary fellowship: the current status. HPB (Oxford) 13(3):149–152
Beyer-Berjot L, Palter V, Grantcharov T et al (2014) Advanced training in laparoscopic abdominal surgery (Atlas): a systematic review. Surgery 156(3):676–688
Eisma R, Wilkinson T (2014) From “Silent Teachers” to models. PLoS Biol 12(10):e1001971
Giger U, Fresard I, Hafliger A et al (2008) Laparoscopic training on Thiel human cadavers: a model to teach advanced laparoscopic procedures. Surg Endosc 22:901–906
Supe A, Dalvi A, Prabhu R et al (2005) Cadaver as a model for laparoscopic training. Indian J Gastroenterol 24:111–113
Willaert W, Tozzi F, Van Herzeele I et al (2018) Systematic review of surgical training on reperfused human cadavers. Acta Chir Belg 13:1–11
Balta JY, Cronin M, Cryan JF et al (2015) Human preservation techniques in anatomy: a 21st century medical education perspective. Clin Anat 28(6):725–734
Chevallier C, Willaert W, Kawa E et al (2014) Postmortem circulation: a new model for testing endovascular devices and training clinicians in their use. Clin Anat 27(4):556–562
Wolff KD, Fichter A, Braun C, Bauer F et al (2014) Flap raising on pulsatile perfused cadaveric tissue: a novel method for surgical teaching and exercise. J Craniomaxillofac Surg 42(7):1423–1427
Aboud ET, Krisht AF, O’Keeffe T et al (2011) Novel simulation for training trauma surgeons. J Trauma 71:1484–1490
Monbailliu T, Troisi RI, Willaert W (2018) Postgraduates’ experience with laparoscopic training on reperfused Thiel embalmed human livers. Oral communication, 19th Belgian Surgical Week, Ostend-Belgium, 3–5 May 2018
Acknowledgements
The authors would like to thank the experts from UK, Italy, France, Norway, South Korea, Germany, Japan and the Netherlands who have contributed with their passion and dedication to the success of the courses. The department of HPB Surgery of the Ghent University Hospital received restricted grant from Medtronic for the masterclasses (Reference No. KW/1791/HHB/006/013). The company played no role in design and conduct of the study; in the collection, management and interpretation of data; or in the preparation of the manuscript.
Funding
Nil.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declared that they have no conflict of interest.
Ethical approval
The study was approved by the local Ethics Committee (IRB Approval No. B670201836650).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Rashidian, N., Willaert, W., Giglio, M.C. et al. Laparoscopic Liver Surgery Training Course on Thiel-Embalmed Human Cadavers: Program Evaluation, Trainer’s Long-Term Feedback and Steps Forward. World J Surg 43, 2902–2908 (2019). https://doi.org/10.1007/s00268-019-05103-x
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-019-05103-x