Abstract
Purposes
Due to the morphological diversity of deformities, technical difficulties, improperly designed components, and so on, THA remains a challenging task in dysplastic hips, especially in highly dislocated hips. The purpose of this study was to comprehensively evaluate the clinical outcomes of robot-assisted THA in patients with DDH through a large cohort study, including the precision of acetabular cup positioning, indicators of inflammatory response, indicators of muscle damage, and complications.
Methods
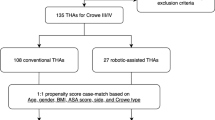
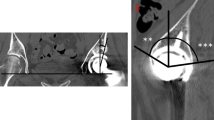
We retrospectively analyzed patients with DDH who underwent THA in our prospectively constructed joint registry between August 2018 and August 2022. Finally, 147 manual THAs and 147 robotic-assisted THAs were included in the final analysis. Patient demographics, indicators of inflammation, indicators of muscle damage, operative time, Harris hip scores (HHS), and forgotten joint score (FJS) were recorded for analysis. The precision of the positioning of the acetabular component was assessed with plain radiographs.
Results
In the Crowe II/III groups, the reconstructed center of rotation (COR) in the robotic-assisted group was closer to the anatomical COR with less variation than the manual group (absolute horizontal distances of COR 3.5 ± 2.8 vs. 5.4 ± 4.9 mm, p < 0.05; absolute vertical distances of COR 6.4 ± 4.1 vs. 11.7 ± 8.2 mm, p = 0.001). For all Crowe subtypes, the robotic-assisted THA significantly increased the proportion of acetabular cups located in the safety zone within 5° (all p < 0.05). Interleukin-6 and creatine kinase levels were slightly lower and significantly different in the robotic-assisted group at three days postoperatively (all p < 0.05).
Conclusions
Compared to the manual technique, the robot-assisted technique improved the precision and reproducibility of acetabular component positioning, particularly in DDH patients with Crowe types II/III. The robotic-assisted technique did not increase operative time, bleeding, complications, or revision rates, and had a slighter early inflammatory response and muscle damage.



Similar content being viewed by others
Data availability
All data generated or analyzed during this study are included in this published article.
References
Chai W, Xu C, Guo RW, Kong XP, Fu J, Tang PF, Chen JY (2022) Does robotic-assisted computer navigation improve acetabular cup positioning in total hip arthroplasty for Crowe III/IV hip dysplasia? A propensity score case-match analysis. Int Orthop 46:769–777. https://doi.org/10.1007/s00264-021-05232-w
Lloyd-Roberts GC (1955) Osteoarthritis of the hip; a study of the clinical pathology. J Bone Joint Surg (Br) 37-b:8–47. https://doi.org/10.1302/0301-620x.37b1.8
Harris WH (1986) Etiology of osteoarthritis of the hip. Clin Orthop Relat Res Dec (213):20–33
Greber EM, Pelt CE, Gililland JM, Anderson MB, Erickson JA, Peters CL (2017) Challenges in total hip arthroplasty in the setting of developmental dysplasia of the hip. J Arthroplast 32:S38–s44. https://doi.org/10.1016/j.arth.2017.02.024
Argenson JN, Ryembault E, Flecher X, Brassart N, Parratte S, Aubaniac JM (2005) Three-dimensional anatomy of the hip in osteoarthritis after developmental dysplasia. J Bone Joint Surg (Br) 87:1192–1196. https://doi.org/10.1302/0301-620x.87b9.15928
Argenson JN, Flecher X, Parratte S, Aubaniac JM (2007) Anatomy of the dysplastic hip and consequences for total hip arthroplasty. Clin Orthop Relat Res 465:40–45. https://doi.org/10.1097/BLO.0b013e3181576052
Sanchez-Sotelo J, Berry DJ, Trousdale RT, Cabanela ME (2002) Surgical treatment of developmental dysplasia of the hip in adults: II. Arthroplasty options. J Am Acad Orthop Surg 10:334–344. https://doi.org/10.5435/00124635-200209000-00005
Kennedy JG, Rogers WB, Soffe KE, Sullivan RJ, Griffen DG, Sheehan LJ (1998) Effect of acetabular component orientation on recurrent dislocation, pelvic osteolysis, polyethylene wear, and component migration. J Arthroplast 13:530–534. https://doi.org/10.1016/s0883-5403(98)90052-3
Kelley SS, Lachiewicz PF, Hickman JM, Paterno SM (1998) Relationship of femoral head and acetabular size to the prevalence of dislocation. Clin Orthop Relat Res 163–170. https://doi.org/10.1097/00003086-199810000-00017
Conroy JL, Whitehouse SL, Graves SE, Pratt NL, Ryan P, Crawford RW (2008) Risk factors for revision for early dislocation in total hip arthroplasty. J Arthroplast 23:867–872. https://doi.org/10.1016/j.arth.2007.07.009
Zhou Y, Shao H, Huang Y, Deng W, Yang D, Bian T (2021) Does robotic assisted technology improve the accuracy of acetabular component positioning in patients with DDH? J Orthop Surg (Hong Kong) 29:23094990211025325. https://doi.org/10.1177/23094990211025325
Hepinstall M, Mota F, Naylor B, Coden G, Muthusamy N, Salem HS, Mont MA (2021) Robotic-assisted total hip arthroplasty in patients who have developmental hip dysplasia. Surg Technol Int 39:338–347. https://doi.org/10.52198/21.STI.39.OS1454
Vigdorchik JM, Sharma AK, Aggarwal VK, Carroll KM, Jerabek SA (2020) The use of robotic-assisted total hip arthroplasty in developmental dysplasia of the hip. Arthroplast Today 6:770–776. https://doi.org/10.1016/j.artd.2020.07.022
Chai W, Xu C, Guo RW, Kong XP, Fu J, Tang PF, Chen JY (2022) Does robotic-assisted computer navigation improve acetabular cup positioning in total hip arthroplasty for Crowe III/IV hip dysplasia? A propensity score case-match analysis. Int Orthop https://doi.org/10.1007/s00264-021-05232-w
Ranawat CS, Dorr LD, Inglis AE (1980) Total hip arthroplasty in protrusio acetabuli of rheumatoid arthritis. J Bone Joint Surg Am 62:1059–1065
Kong X, Chai W, Chen J, Yan C, Shi L, Wang Y (2019) Intraoperative monitoring of the femoral and sciatic nerves in total hip arthroplasty with high-riding developmental dysplasia. Bone Joint J 101-b:1438–1446. https://doi.org/10.1302/0301-620x.101b11.Bjj-2019-0341.R2
Zhang S, Liu Y, Ma M, Cao Z, Kong X, Chai W (2023) Is robotic-assisted technology still accurate in total hip arthroplasty for fibrous-fused hips? J Arthroplast 38:129–134. https://doi.org/10.1016/j.arth.2022.07.023
Zhang S, Liu Y, Yang M, Ma M, Cao Z, Kong X, Chai W (2022) Robotic-assisted versus manual total hip arthroplasty in obese patients: a retrospective case-control study. J Orthop Surg Res 17:368. https://doi.org/10.1186/s13018-022-03263-6
Øvre S, Sandvik L, Madsen JE, Røise O (2005) Comparison of distribution, agreement and correlation between the original and modified Merle d'Aubigné-Postel Score and the Harris Hip Score after acetabular fracture treatment: moderate agreement, high ceiling effect and excellent correlation in 450 patients. Acta Orthop 76:796–802. https://doi.org/10.1080/17453670510045390
Gross JB (1983) Estimating allowable blood loss: corrected for dilution. Anesthesiology 58:277–280. https://doi.org/10.1097/00000542-198303000-00016
Domb BG, El Bitar YF, Sadik AY, Stake CE, Botser IB (2014) Comparison of robotic-assisted and conventional acetabular cup placement in THA: a matched-pair controlled study. Clin Orthop Relat Res 472:329–336. https://doi.org/10.1007/s11999-013-3253-7
Liaw CK, Yang RS, Hou SM, Wu TY, Fuh CS (2009) Measurement of the acetabular cup anteversion on simulated radiographs. J Arthroplast 24:468–474. https://doi.org/10.1016/j.arth.2007.10.029
Widmer KH (2004) A simplified method to determine acetabular cup anteversion from plain radiographs. J Arthroplast 19:387–390. https://doi.org/10.1016/j.arth.2003.10.016
Ranawat CS, Rao RR, Rodriguez JA, Bhende HS (2001) Correction of limb-length inequality during total hip arthroplasty. J Arthroplast 16:715–720. https://doi.org/10.1054/arth.2001.24442
Lewinnek GE, Lewis JL, Tarr R, Compere CL, Zimmerman JR (1978) Dislocations after total hip-replacement arthroplasties. J Bone Joint Surg Am 60:217–220
Callanan MC, Jarrett B, Bragdon CR, Zurakowski D, Rubash HE, Freiberg AA, Malchau H (2011) The John Charnley Award: risk factors for cup malpositioning: quality improvement through a joint registry at a tertiary hospital. Clin Orthop Relat Res 469:319–329. https://doi.org/10.1007/s11999-010-1487-1
Reina N, Putman S, Desmarchelier R, Sari Ali E, Chiron P, Ollivier M, Jenny JY, Waast D, Mabit C, de Thomasson E, Schwartz C, Oger P, Gayet LE, Migaud H, Ramdane N, Fessy MH (2017) Can a target zone safer than Lewinnek's safe zone be defined to prevent instability of total hip arthroplasties? Case-control study of 56 dislocated THA and 93 matched controls. Orthop Traumatol Surg Res 103:657–661. https://doi.org/10.1016/j.otsr.2017.05.015
Gwam CU, Mistry JB, Mohamed NS, Thomas M, Bigart KC, Mont MA, Delanois RE (2017) Current epidemiology of revision total hip arthroplasty in the United States: national inpatient sample 2009 to 2013. J Arthroplast 32:2088–2092. https://doi.org/10.1016/j.arth.2017.02.046
Biedermann R, Tonin A, Krismer M, Rachbauer F, Eibl G, Stöckl B (2005) Reducing the risk of dislocation after total hip arthroplasty: the effect of orientation of the acetabular component. J Bone Joint Surg (Br) 87:762–769. https://doi.org/10.1302/0301-620x.87b6.14745
Coulomb R, Cascales V, Haignere V, Bauzou F, Kouyoumdjian P (2023) Does acetabular robotic-assisted total hip arthroplasty with femoral navigation improve clinical outcomes at 1-year post-operative? A case-matched propensity score study comparing 98 robotic-assisted versus 98 manual implantation hip arthroplasties. Orthop Traumatol Surg Res 109:103477. https://doi.org/10.1016/j.otsr.2022.103477
Grammatopoulos G, Alvand A, Monk AP, Mellon S, Pandit H, Rees J, Gill HS, Murray DW (2016) Surgeons’ accuracy in achieving their desired acetabular component orientation. J Bone Joint Surg Am 98:e72. https://doi.org/10.2106/jbjs.15.01080
Bosker BH, Verheyen CC, Horstmann WG, Tulp NJ (2007) Poor accuracy of freehand cup positioning during total hip arthroplasty. Arch Orthop Trauma Surg 127:375–379. https://doi.org/10.1007/s00402-007-0294-y
Ando W, Takao M, Hamada H, Uemura K, Sugano N (2021) Comparison of the accuracy of the cup position and orientation in total hip arthroplasty for osteoarthritis secondary to developmental dysplasia of the hip between the Mako robotic arm-assisted system and computed tomography-based navigation. Int Orthop 45:1719–1725. https://doi.org/10.1007/s00264-021-05015-3
Little NJ, Busch CA, Gallagher JA, Rorabeck CH, Bourne RB (2009) Acetabular polyethylene wear and acetabular inclination and femoral offset. Clin Orthop Relat Res 467:2895–2900. https://doi.org/10.1007/s11999-009-0845-3
Dapuzzo MR, Sierra RJ (2012) Acetabular considerations during total hip arthroplasty for hip dysplasia. Orthop Clin North Am 43:369–375. https://doi.org/10.1016/j.ocl.2012.05.012
Bhaskar D, Rajpura A, Board T (2017) Current concepts in acetabular positioning in total hip arthroplasty. Indian J Orthop 51:386–396. https://doi.org/10.4103/ortho.IJOrtho_144_17
Parvizi J, Sharkey PF, Bissett GA, Rothman RH, Hozack WJ (2003) Surgical treatment of limb-length discrepancy following total hip arthroplasty. J Bone Joint Surg Am 85:2310–2317. https://doi.org/10.2106/00004623-200312000-00007
Abolghasemian M, Samiezadeh S, Jafari D, Bougherara H, Gross AE, Ghazavi MT (2013) Displacement of the hip center of rotation after arthroplasty of Crowe III and IV dysplasia: a radiological and biomechanical study. J Arthroplast 28:1031–1035. https://doi.org/10.1016/j.arth.2012.07.042
Bicanic G, Delimar D, Delimar M, Pecina M (2009) Influence of the acetabular cup position on hip load during arthroplasty in hip dysplasia. Int Orthop 33:397–402. https://doi.org/10.1007/s00264-008-0683-z
Traina F, De Fine M, Biondi F, Tassinari E, Galvani A, Toni A (2009) The influence of the centre of rotation on implant survival using a modular stem hip prosthesis. Int Orthop 33:1513–1518. https://doi.org/10.1007/s00264-008-0710-0
Watts CD, Martin JR, Fehring KA, Griffin WL (2018) Inferomedial hip center decreases failure rates in cementless total hip arthroplasty for Crowe II and III hip dysplasia. J Arthroplast 33:2177–2181. https://doi.org/10.1016/j.arth.2018.02.039
Hayashi S, Hashimoto S, Kuroda Y, Nakano N, Matsumoto T, Ishida K, Shibanuma N, Kuroda R (2021) Robotic-arm assisted THA can achieve precise cup positioning in developmental dysplasia of the hip : a case control study. Bone Joint Res 10:629–638. https://doi.org/10.1302/2046-3758.1010.Bjr-2021-0095.R1
Sato K, Sato A, Okuda N, Masaaki M, Koga H (2023) A propensity score-matched comparison between Mako robotic arm-assisted system and conventional technique in total hip arthroplasty for patients with osteoarthritis secondary to developmental dysplasia of the hip. Arch Orthop Trauma Surg 143:2755–2761. https://doi.org/10.1007/s00402-022-04524-z
Morrell AT, Layon DR, Scott MJ, Kates SL, Golladay GJ, Patel NK (2021) Enhanced recovery after primary total hip and knee arthroplasty: a systematic review. J Bone Joint Surg Am 103:1938–1947. https://doi.org/10.2106/jbjs.20.02169
Poehling-Monaghan KL, Taunton MJ, Kamath AF, Trousdale RT, Sierra RJ, Pagnano MW (2017) No correlation between serum markers and early functional outcome after contemporary THA. Clin Orthop Relat Res 475:452–462. https://doi.org/10.1007/s11999-016-4904-2
Guo R, Chen JY, Zhang G, Zhou Y, Chen J, Chai W (2019) Calculation method to predict postoperative limb length in patients undergoing THA following developmental dysplasia of hips. BMC Musculoskelet Disord 20:513. https://doi.org/10.1186/s12891-019-2903-7
Kort N, Stirling P, Pilot P, Müller JH (2021) Clinical and surgical outcomes of robot-assisted versus conventional total hip arthroplasty: a systematic overview of meta-analyses. EFORT Open Rev 6:1157–1165. https://doi.org/10.1302/2058-5241.6.200121
Kumar V, Patel S, Baburaj V, Rajnish RK, Aggarwal S (2023) Does robotic-assisted surgery improve outcomes of total hip arthroplasty compared to manual technique? A systematic review and meta-analysis. Postgrad Med J 99:375–383. https://doi.org/10.1136/postgradmedj-2021-141135
Funding
National Natural Science Foundation of China Joint Key Program (U22A20355)
Author information
Authors and Affiliations
Contributions
Shuai Zhang and Mingyang Ma: primarily responsible for all computational analyses in the article and the drafting of the manuscript. Shuai Zhang and Mingyang Ma are the co-first authors of this article. Yonggang Zhou, Jiying Chen, and Wei Chai: primarily responsible for oversight of the research project, including all data acquisition and analysis, and manuscript preparation and approval. Yonggang Zhou, Jiying Chen, and Wei Chai contributed to this work equally, and both of them were co-corresponding author. Xiangpeng Kong: revised the manuscript and helped perform the analysis with constructive discussions. All authors have read and approved the final submitted manuscript.
Corresponding authors
Ethics declarations
Consent for publication
All the authors agreed to the publication.
Informed consent
This study was approved by the ethics committee of hospital and was carried out in accordance with the Declaration of Helsinki of the World Medical Association. All enrolled patients provided written informed consent.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Zhang, S., Ma, M., Kong, X. et al. Robotic-assisted total hip arthroplasty in patients with developmental dysplasia of the hip. International Orthopaedics (SICOT) 48, 1189–1199 (2024). https://doi.org/10.1007/s00264-024-06115-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-024-06115-6