Abstract
Summary
Premature osteoporosis and stunted growth are common complications of childhood chronic inflammatory disease. Presently, no treatment regimens are available for these defects in juvenile diseases. We identified the sequential Fc-OPG/hPTH treatment as an experimental therapy that improves the skeletal growth and prevents the bone loss in a mouse model overexpressing IL-6.
Introduction
Premature osteoporosis and stunted growth are common complications of childhood chronic inflammatory diseases and have a significant impact on patients’ quality of life. Presently, no treatment regimens are available for these defects in juvenile diseases. To test a new therapeutic approach, we used growing mice overexpressing the pro-inflammatory cytokine IL-6 (TG), which show a generalized bone loss and stunted growth.
Methods
Since TG mice present increased bone resorption and impaired bone formation, we tested a combined therapy with the antiresorptive modified osteoprotegerin, Fc-OPG, and the anabolic PTH. We injected TG mice with Fc-OPG once at the 4th day of life and with hPTH(1–34) everyday from the 16th to the 30th day of age.
Results
A complete prevention of growth and bone defects was observed in treated mice due to normalization of osteoclast and osteoblast parameters. Re-establishment of normal bone turnover was confirmed by RT-PCR analysis and by in vitro experiments that revealed the full rescue of osteoclast and osteoblast functions. The phenotypic recovery of TG mice was due to the sequential treatment, because TG mice treated with Fc-OPG or hPTH alone showed an increase of body weight, tibia length, and bone volume to intermediate levels between those observed in vehicle-treated WT and TG mice.
Conclusions
Our results identified the sequential Fc-OPG/hPTH treatment as an experimental therapy that improves the skeletal growth and prevents the bone loss in IL-6 overexpressing mice, thus providing the proof of principle for a therapeutic approach to correct these defects in juvenile inflammatory diseases.




Similar content being viewed by others
References
Cassidy JT, Hillman LS (1997) Abnormalities in skeletal growth in children with juvenile rheumatoid arthritis. Rheum Dis Clin N Am 23:499–522
Burnham JM, Leonard MB (2004) Bone disease in pediatric rheumatologic disorders. Curr Rheumatol Rep 6:70–78
Lee N, Radford-Smith G, Taaffe DR (2005) Bone loss in Crohn’s disease: exercise as a potential countermeasure. Inflamm Bowel Dis 11:1108–1118
van Hogezand RA, Hamdy NA (2006) Skeletal morbidity in inflammatory bowel disease. Scand J Gastroenterol Suppl 243:59–64
Baker-LePain JC, Nakamura MC, Lane NE (2011) Effects of inflammation on bone: an update. Curr Opin Rheumatol 23:389–395
Via MA, Gallagher EJ, Mechanick JI (2010) Bone physiology and therapeutics in chronic critical illness. Ann N Y Acad Sci 1211:85–94
Ansell BM, Bywaters EG (1956) Growth in Still’s disease. Ann Rheum Dis 15:295–319
Henderson CJ, Cawkwell GD, Specker BL, Sierra RI, Wilmott RW, Campaigne BN, Lovell DJ (1997) Predictors of total body bone mineral density in non-corticosteroid-treated prepubertal children with juvenile rheumatoid arthritis. Arthritis Rheum 40:1967–1975
McLean RR (2009) Proinflammatory cytokines and osteoporosis. Curr Osteoporos Rep 7:134–139
MacRae VE, Farquharson C, Ahmed SF (2006) The pathophysiology of the growth plate in juvenile idiopathic arthritis. Rheumatology (Oxford) 45:11–19
Lien G, Selvaag AM, Flato B, Haugen M, Vinje O, Sorskaar D, Dale K, Egeland T, Førre Ø (2005) A two-year prospective controlled study of bone mass and bone turnover in children with early juvenile idiopathic arthritis. Arthritis Rheum 52:833–840
De Benedetti F, Rucci N, Del Fattore A, Peruzzi B, Paro R, Longo M, Vivarelli M, Muratori F, Berni S, Ballanti P, Teti A (2006) Impaired skeletal development in interleukin-6 transgenic mice. A model for the impact of chronic inflammation in growing skeletal system. Arthritis and Rheumatism 54:3551–3563
De Benedetti F, Alonzi T, Moretta A, Lazzaro D, Costa P, Poli V, Martini A, Ciliberto G, Fattori E (1997) Interleukin 6 causes growth impairment in transgenic mice through a decrease in insulin-like growth factor-I. A model for stunted growth in children with chronic inflammation. J Clin Invest 15:643–650
Finkelstein JS, Wyland JJ, Lee H, Neer RM (2010) Effects of teriparatide, alendronate, or both in women with postmenopausal osteoporosis. J Clin Endocrinol Metab 95:1838–1845
Recker RR, Armas L (2011) The effect of antiresorptives on bone quality. Clin Orthop Relat Res 469:2207–2214
Mosekilde L, Tørring O, Rejnmark L (2011) Emerging anabolic treatments in osteoporosis. Curr Drug Saf 6:62–74
Rejnmark L, Mosekilde L (2011) New and emerging antiresorptive treatments in osteoporosis. Curr Drug Saf 6:75–88
Lacey DL, Timms E, Tan HL, Kelley MJ, Dunstan CR, Burgess T, Elliott R, Colombero A, Elliott G, Scully S, Hsu H, Sullivan J, Hawkins N, Davy E, Capparelli C, Eli A, Qian YX, Kaufman S, Sarosi I, Shalhoub V, Senaldi G, Guo J, Delaney J, Boyle WJ (1998) Osteoprotegerin ligand is a cytokine that regulates osteoclast differentiation and activation. Cell 17:165–176
Cummings SR, San Martin J, McClung MR, Siris ES, Eastell R, Reid IR, Delmas P, Zoog HB, Austin M, Wang A, Kutilek S, Adami S, Zanchetta J, Libanati C, Siddhanti S, Christiansen C (2009) Denosumab for prevention of fractures in postmenopausal women with osteoporosis. N Engl J Med 20:756–765
Kostenuik PJ, Nguyen HQ, McCabe J, Warmington KS, Kurahara C, Sun N, Chen C, Li L, Cattley RC, Van G, Scully S, Elliott R, Grisanti M, Morony S, Tan HL, Asuncion F, Li X, Ominsky MS, Stolina M, Dwyer D, Dougall WC, Hawkins N, Boyle WJ, Simonet WS, Sullivan JK (2009) Denosumab, a fully human monoclonal antibody to RANKL, inhibits bone resorption and increases BMD in knock-in mice that express chimeric (murine/human) RANKL. J Bone Miner Res 24:182–195
Simonet WS, Lacey DL, Dunstan CR, Kelley M, Chang MS, Lüthy R, Nguyen HQ, Wooden S, Bennett L, Boone T, Shimamoto G, DeRose M, Elliott R, Colombero A, Tan HL, Trail G, Sullivan J, Davy E, Bucay N, Renshaw-Gegg L, Hughes TM, Hill D, Pattison W, Campbell P, Sander S, Van G, Tarpley J, Derby P, Lee R, Boyle WJ (1997) Osteoprotegerin: a novel secreted protein involved in the regulation of bone density. Cell 18:309–319
Morony S, Capparelli C, Lee R, Shimamoto G, Boone T, Lacey DL, Dunstan CR (1999) A chimeric form of osteoprotegerin inhibits hypercalcemia and bone resorption induced by IL-1beta, TNF-alpha, PTH, PTHrP, and 1, 25(OH)2D3. J Bone Miner Res 14:1478–1485
Capparelli C, Morony S, Warmington K, Adamu S, Lacey D, Dunstan CR, Stouch B, Martin S, Kostenuik PJ (2003) Sustained antiresorptive effects after a single treatment with human recombinant osteoprotegerin (OPG): a pharmacodynamic and pharmacokinetic analysis in rats. J Bone Miner Res 5:852–858
Bilezikian JP, Rubin MR, Finkelstein JS (2005) Parathyroid hormone as an anabolic therapy for women and men. J Endocrinol Invest 28:41–49
Reeve J, Meunier PJ, Parsons JA, Bernat M, Bijvoet OL, Courpron P, Edouard C, Klenerman L, Neer RM, Renier JC, Slovik D, Vismans FJ, Potts JT Jr (1980) Anabolic effect of human parathyroid hormone fragment on trabecular bone in involutional osteoporosis: a multicentre trial. Br Med J 7:1340–1344
Cusano NE, Bilezikian JP (2011) Combination antiresorptive and osteoanabolic therapy for osteoporosis: we are not there yet. Curr Med Res Opin 27:1705–1707
Bilezikian JP (2008) Combination anabolic and antiresorptive therapy for osteoporosis: opening the anabolic window. Curr Osteoporos Rep 6:24–30
Black DM, Greenspan SL, Ensrud KE, Palermo L, McGowan JA, Lang TF, Garnero P, Bouxsein ML, Bilezikian JP, Rosen CJ (2003) The effects of parathyroid hormone and alendronate alone or in combination in postmenopausal osteoporosis. N Engl J Med 25:1207–1215
Lewiecki EM (2011) New targets for intervention in the treatment of postmenopausal osteoporosis. Nat Rev Rheumatol 7:631–638
Bachrach LK (2007) Consensus and controversy regarding osteoporosis in the pediatric population. Endocr Pract 13:513–520
Parfitt AM, Drezner MK, Glorieux FH, Kanis JA, Malluche H, Meunier PJ, Ott SM, Recker RR (1987) Bone histomorphometry: standardization of nomenclature, symbols, and units: report of the ASBMR Histomorphometry Nomenclature Committee. J Bone Miner Res 2:595–610
Benedetti D, De Benedetti F, Meazza C, Oliveri M, Pignatti P, Vivarelli M, Alonzi T, Fattori E, Garrone S, Barreca A, Martini A (2001) Effect of IL-6 on IGF binding protein-3: a study in IL-6 transgenic mice and in patients with systemic juvenile idiopathic arthritis. Endocrinology 142:4818–4826
Hoshino K, Hanyu T, Arai K, Takahashi HE (2001) Mineral density and histomorphometric assessment of bone changes in the proximal tibia early after induction of type II collagen-induced arthritis in growing and mature rats. J Bone Miner Metab 19:76–83
Kitamura H, Kawata H, Takahashi F, Higuchi Y, Furuichi T, Ohkawa H (1995) Bone marrow neutrophilia and suppressed bone turnover in human interleukin-6 transgenic mice: a cellular relationship among hematopoietic cells, osteoblasts, and osteoclasts mediated by stromal cells in bone marrow. Am J Pathol 147:1682–1692
Sims NA, Jenkins BJ, Quinn JM, Nakamura A, Glatt M, Gillespie MT, Ernst M, Martin TJ (2004) Glycoprotein 130 regulates bone turnover and bone size by distinct downstream signaling pathways. J Clin Invest 113:379–389
Vahle JL, Sato M, Long GG, Young JK, Francis PC, Engelhardt JA, Westmore MS, Linda Y, Nold JB (2002) Skeletal changes in rats given daily subcutaneous injections of recombinant human parathyroid hormone (1–34) for 2 years and relevance to human safety. Toxicol Pathol 30:312–321
Samadfam R, Xia Q, Goltzman D (2007) Pretreatment with anticatabolic agents blunts but does not eliminate the skeletal anabolic response to parathyroid hormone in oophorectomized mice. Endocrinology 148:2778–2787
Pierroz DD, Bonnet N, Baldock PA, Ominsky MS, Stolina M, Kostenuik PJ, Ferrari SL (2010) Are osteoclasts needed for the bone anabolic response to parathyroid hormone? A study of intermittent parathyroid hormone with denosumab or alendronate in knock-in mice expressing humanized RANKL. J Biol Chem 3(285):28164–28173
Letocha AD, Cintas HL, Troendle JF, Reynolds JC, Cann CE, Chernoff EJ, Hill SC, Gerber LH, Marini JC (2005) Controlled trial of pamidronate in children with types III and IV osteogenesis imperfecta confirms vertebral gains but not short-term functional improvement. J Bone Miner Res 20:977–986
Speiser PW, Clarson CL, Eugster EA, Kemp SF, Radovick S, Rogol AD, Wilson TA, Pharmacy LWPES, Committee T (2005) Bisphosphonate treatment of pediatric bone disease. Pediatr Endocrinol Rev 3:87–96
Jayaraman M, Karikumar K, Verma A, Modi KD (2011) Alendronate therapy in polyostotic fibrous dysplasia presenting with pathologic fracture. Am J Orthop 40:48–50
Acknowledgments
We thank Dr. Rita Di Massimo for excellent assistance in the editing of the manuscript. ADF has been supported by a fellowship funded by AMGEN through European Calcified Tissue Society (ECTS).
Conflicts of interest
None.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Online Resource 1
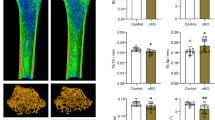
Analysis of somatic growth. (a) Body weight of male and female wild-type and of NSE/hIL6 mice. (b) Histomorphometric analysis of bone volume/total volume (BV/TV), trabecular number (Tb.N), trabecular thickness (Tb.Th) and trabecular separation (Tb.Sp) performed on the tibia proximal spongiosa. # p < 0.05 vs. wild-type mice. (PDF 20 kb)
Online Resource 2
Analysis of somatic growth. (a) Longitudinal growth assessed by measuring the animal length on radiographs and (b) histomorphometric analysis of hypertrophic zone width of 30-days-old wild-type and NSE/hIL6 mice treated with vehicle, Fc-OPG 0.25 mg/kg, vehicle/hPTH(1-34) or Fc-OPG/hPTH(1-34). # p < 0.01; *p < 0.05. (PDF 13 kb)
Online Resource 3
RNA Expression analysis. RNA was extracted from whole femurs and reverse transcribed, then cDNA was subjected to comparative real time PCR using primer pairs and conditions specific for rankl, opg, igf1, igfbp3 and igfbp5. Values are normalized vs. the housekeeping gene gapdh. *p < 0.05 vs. WT mice treated with vehicle. (PDF 15 kb)
Online Resource 4
Analysis of somatic growth. Body weight of wild-type and of NSE/hIL6 mice treated with vehicle or with different doses of Fc-OPG. *p < 0.05. (PDF 14 kb)
Online Resource 5
Analysis of osteoclast parameters in 16-days-old mice. (a) Histomorphometric analysis of osteoclast number/bone surface (Oc.N/BS) performed on TRAcP histochemically stained sections of proximal tibias. (b) Bone marrows were flushed off, subjected to Ficoll/Histopaque separation of mononuclear cells which were fixed after 3 h. Quantification of osteoclast mononuclear TRAcP-positive precursors was performed. # p < 0.01; *p < 0.05. (PDF 13 kb)
Rights and permissions
About this article
Cite this article
Del Fattore, A., Cappariello, A., Capulli, M. et al. An experimental therapy to improve skeletal growth and prevent bone loss in a mouse model overexpressing IL-6. Osteoporos Int 25, 681–692 (2014). https://doi.org/10.1007/s00198-013-2479-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-013-2479-2