Abstract
Introduction and hypothesis
Different techniques of mesh placement for cystocele repair are known. Our goal was to compare anatomical and functional outcomes of three different techniques of mesh placement over a 3-year follow-up.
Methods
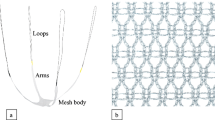
Between March 2003 and June 2004, 230 patients (stage 2–4 pelvic organ prolapse (POP)) were included in a prospective study. For cystocele repair, mesh was implanted either with two arms into the retropubic space (RP) or with two to four arms into the obturator foramen (TO), or fixed to the arcus tendineous fascia pelvis (FG).
Results
Patients' distribution is as follows: 142 TO, 32 RP, and 31 FG. Anatomical success (cystocele < stage 2 in the POP staging system) was clearly poorer after the retropubic free technique, with success rates of 69% (RP), 90.1% (TO), and 96.6% (FG) (p = 0.004). POP distress inventory (p < 0.005) and POP impact questionnaire scores were both significantly poorer after RP.
Conclusions
RP technique is less effective than TO and FG techniques.

Similar content being viewed by others
References
Benson J, Lucente V, McClellan E (1996) Vaginal versus abdominal reconstructive surgery for the treatment of pelvic support defects: a prospective randomized study with long-term outcome evaluation. Am J Obstet Gynecol 175:1418–1422
Julian TM (1996) The efficacy or Marlex mesh in the repair of severe, recurrent vaginal prolapse of the anterior midvaginal wall. Am J Obstet Gynecol 175:1472–1475
Hiltunen R, Nieminen K, Takala T, Heiskanen E, Merikari M, Niemi K, Heinonen PK (2007) Low-weight polypropylene mesh for anterior vaginal wall prolapse: a randomized controlled trial. Obstet Gynecol 110(2 Pt 2):455–462
Sivaslioglu AA, Unlubilgin E, Dolen I (2008) A randomized comparison of polypropylene mesh surgery with site-specific surgery in the treatment of cystocoele. Int Urogynecol J Pelvic Floor Dysfunct 19(4):467–471, Epub 2007 Sep 28
Nguyen JN, Burchette RJ (2008) Outcome after anterior vaginal prolapse repair: a randomized controlled trial. Obstet Gynecol 111(4):891–898
de Tayrac R, Devoldere G, Renaudie J, Villard P, Guilbaud O, Eglin G, French Ugytex Study Group (2007) Prolapse repair by vaginal route using a new protected low-weight polypropylene mesh: 1-year functional and anatomical outcome in a prospective multicentre study. Int Urogynecol J Pelvic Floor Dysfunct 18(3):251–256
de Tayrac R, Chauveaud-Lambling A, Fernandez D, Fernandez H (2003) Quality of life instruments for women with pelvic organ prolapse. J Gynecol Obstet Biol Reprod (Paris) 32:503–523
Barber MD, Kuchibhatla MN, Pieper CF, Bump RC (2001) Psychometric evaluation of 2 comprehensive condition-specific quality of life instruments for women with pelvic floor disorders. Am J Obstet Gynecol 185:1388–1395
Haab F, Richard F, Amarenci G, Coloby P, Arnould B, Benmedjahed K, Guillemin I, Grise P (2008) Comprehensive evaluation of bladder and urethral dysfunction symptoms: development and psychometric validation of the Urinary Symptom Profile (USP) questionnaire. Urology 71(4):646–656
de Tayrac R, Gervaise A, Chauveaud A, Fernandez H (2005) Tension-free polypropylene mesh for vaginal repair of anterior vaginal wall prolapse. J Reprod Med 50(2):75–80
Eglin G, Ska JM, Serres X (2003) Trans-obturator subvesical mesh. Tolerance and short-term results of 103 case continuous series. Gynecol Obstet Fertil 31:14–19
de Tayrac R, Picone O, Chauveaud-Lambling A, Fernandez H (2006) Two-year anatomical and functional assessment of transvaginal rectocele repair using a polypropylene mesh. Int Urogynecol J 17(2):100–105
Petros PE (2001) Vault Prolapse II: restoration of dynamic vaginal supports by infracoccygeal sacropexy, an axial day-case vaginal procedure. Int Urogynecol J Pelvic Floor Dysfunct 12:296–303
Moore RD, Beyer RD, Jacoby K, Freedman SJ, Mc Cammon KA, Gambla MT (2010) Prospective multicenter trial assessing type I, polypropylene mesh placed via transobturator route for the treatment of anterior vaginal prolapse with 2-year follow-up. Int Urogynecol J Pelvic Floor Dysfunct 21(5):545–552
Nieminen K, Hiltunen R, Takala T, Heiskanen E, Merikari M, Niemi K, Heinonen PK (2010) Outcomes after anterior vaginal wall repair with mesh: a randomized, controlled trial with a 3 year follow-up. Am J Obstet Gynecol 203(3):235.e1–235.e8
Sentilhes L, Berthier A, Sergent F, Verspyck E, Descamps P, Marpeau L (2008) Sexual function in women before and after transvaginal mesh placement for pelvic organ prolapse. Int Urogynecol J 19:763–772
Dwyer PL, O’Reilly BA (2004) Transvaginal repair of anterior and posterior compartment prolapse with atrium polypropylene mesh. Br J Obstet Gynaecol 111:831–836
Milani R, Salvatore S, Soligo M, Pifarotti P, Meschia M, Cortese M (2005) Functional and anatomical outcome of anterior and posterior vaginal prolapse repair with prolene mesh. BJOG 112(1):107–111
Carey M, Slack M, Higgs P, Wynn-Williams M, Cornish A (2008) Vaginal surgery for pelvic organ prolapse using mesh and a vaginal support device. BJOG 115:391–397
Zargar MA, Emami M, Zargar K, Jamshidi M (2004) The results of grade IV cystocele repair using mesh. Urol J 1(4):263–267
de Tayrac R, Deffieux X, Gervaise A, Chauveaud-Lambling A, Fernandez H (2006) Long-term anatomical and functional assessment of trans-vaginal cystocele repair using a tension-free polypropylene mesh. Int Urogynecol J 17:483–488
Cervigni M, Natale F, La Penna C, Panei M, Mako A (2008) Transvaginal cystocele repair with polypropylene mesh using a tension-free technique. Int Urogynecol J 19:489–496
Milani AL, Heidema WM, van der Vloedt WS, Kluivers KB, Withagen MI, Vierhout ME (2008) Vaginal prolapse repair surgery augmented by ultralightweight titanium-coated polypropylene mesh. Eur J Obstet Gynecol Reprod Biol 138(2):232–238
Fatton B, Amblard J, Debodinance P, Cosson M, Jacquetin B (2007) Transvaginal repair of genital prolapse: preliminary results of a new tension-free vaginal mesh (prolift technique): a case series multicentric study. Int Urogynecol J 18:743–752
Altman D, Väyrynen T, Engh ME, Axelsen S, Falconer C, for the Nordic Transvaginal Mesh Group (2007) Short-term outcome after transvaginal mesh repair of pelvic organ prolapse. Int Urogynecol J 19:787–793
Gauruder-Burmester A, Koutouzidou P, Rohne J, Gronewold M, Tunn R (2007) Follow-up after polypropylene mesh repair of anterior and posterior compartments in patients with recurrent prolapse. Int Urogynecol J 18:1059–1064
Abdel-Fattah M, Ramsay I, West of Scotland Study Group (2008) Retrospective multicentre study of the new minimally invasive mesh repair devices for pelvic organ prolapse. BJOG 115:22–30
Bai SW, Jung HJ, Jeon MJ, Chung DJ, Kim SK, Kim JW (2007) Surgical repair of anterior wall vaginal defects. Int J Gynaecol Obstet 98:147–150
Amrute KV, Eisenberg ER, Rastinehad AR, Kushner L, Badlani GH (2007) Analysis of outcomes of single polypropylene mesh in total pelvic floor reconstruction. Neurourol Urodyn 26:53–58
Acknowledgments
We thank all the other investigators of the French Ugytex Study Group for their participation to the study: Jean-Louis Bénifla and Fabien Demaria (Rothschild Hospital, Paris), Jérome Blanchot and Pierre-Louis Broux (La Sagesse Private Hospital, Rennes), Michel Cosson and Jean-Philippe Lucot (Jeanne De Flandre University Hospital, Lille), Patrick Delporte (Public Hospital, Dunkerque), Hervé Fernandez (Antoine Béclere University Hospital, Clamart), Christine Frayret (Public Hospital, Chartres), François Hacquin (Santa Maria Private Hospital, Nice), Kazeem-Marc Maaliki (Franche Comté Private Hospital, Besançon), Loïc Marpeau and Fabrice Sergent (University Hospital, Rouen), and Olivier Guilbaud (Public Hospital, Chartres, France).
Funding
This study was funded by Sofradim-Covidien.
Conflicts of interest
None.
Author information
Authors and Affiliations
Consortia
Corresponding author
Additional information
For the list of investigators comprising the French Ugytex Study Group, please refer to Acknowledgments.
Rights and permissions
About this article
Cite this article
Mourtialon, P., Letouzey, V., Eglin, G. et al. Cystocele repair by vaginal route: comparison of three different surgical techniques of mesh placement. Int Urogynecol J 23, 699–706 (2012). https://doi.org/10.1007/s00192-011-1650-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-011-1650-6