Abstract
Introduction
It is estimated that by 2030, 38% of the world population will be overweight, and another 20% will be people with obesity. Intragastric balloons (IGBs) are an option in conjunction with lifestyle modification for the treatment of obesity. We sought to investigate the effects of IGB therapy on hemoglobin A1c (A1c), systolic and diastolic blood pressure (SBP, DBP), total cholesterol (TC), high-density lipoprotein (HDL), low-density lipoprotein (LDL), and triglycerides (TGs).
Methods
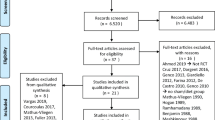
PubMed, Embase, and Google Scholar were queried through November 2021 to identify studies that evaluated the effects of IGB therapy on selected variables at 6 months. A total of 17 studies and 1198 patients met inclusion criteria. Results were pooled using a random-effects model.
Results
At 6-month post-IGB insertion, patients had a significant reduction in A1c (mean difference (MD): − 0.62, 95% confidence interval (CI): − 0.884 to − 0.355, p < 0.001), SBP (MD: − 8.39, 95% CI: − 11.39 to − 5.386, p < 0.001), DBP (MD: − 5.807, 95% CI: − 8.852 to − 2.76, p < 0.001), TC (MD: − 9.189, 95% CI: − 15.763 to − 2.616, p = 0.006), LDL (MD: − 5.20, 95% CI: − 9.05 to − 1.35, p = 0.008), and TGs (MD: − 25.35, 95% CI: − 40.30 to − 10.10, p = 0.001). There was no significant difference in HDL (MD: 1.245, 95% CI: − 0.11 to 2.60, p = 0.071).
Conclusions
Our meta-analysis suggests that IGB therapy is associated with improvements in insulin resistance, blood pressure, and dyslipidemia at 6 months. The results of this analysis suggest that IGB placement can be a viable treatment option to improve important metabolic parameters beyond weight loss alone.
Graphical Abstract



Similar content being viewed by others
References
“Adult obesity facts.” Centers for Disease Control and Prevention, Centers for Disease Control and Prevention, 30 Sept. 2021. https://www.cdc.gov/obesity/data/adult.html. Accessed 11/1/2021
Obesity and overweight. World Health Organization. https://www.who.int/news-room/fact-sheets/detail/obesity-and-overweight. Published April 1, 2020. Accessed June 23, 2020.
Sjöström L. Review of the key results from the Swedish Obese Subjects (SOS) trial – a prospective controlled intervention study of bariatric surgery. J Intern Med. 2013;273(3):219–34. https://doi.org/10.1111/joim.12012.
Ponce J, Woodman G, Swain J, et al. The REDUCE pivotal trial: a prospective, randomized controlled pivotal trial of a dual intragastric balloon for the treatment of obesity. Surg Obes Relat Dis. 2015;11(4):874–81. https://doi.org/10.1016/j.soard.2014.12.006.
Kotinda APST, de Moura DTH, Ribeiro IB, et al. Efficacy of intragastric balloons for weight loss in overweight and obese adults: a systematic review and meta-analysis of randomized controlled trials. Obes Surg. 2020;30(7):2743–53. https://doi.org/10.1007/s11695-020-04558-5.
Gómez V, Woodman G, Abu Dayyeh BK. Delayed gastric emptying as a proposed mechanism of action during intragastric balloon therapy: Results of a prospective study. Obesity (Silver Spring). 2016;24(9):1849–53. https://doi.org/10.1002/oby.21555.
Chandan S, Mohan BP, Khan SR, et al. Efficacy and safety of intragastric balloon (IGB) in non-alcoholic fatty liver disease (NAFLD): a comprehensive review and meta-analysis. Obes Surg. 2021;31(3):1271–9. https://doi.org/10.1007/s11695-020-05084-0.
Loo JH, Lim YH, Seah HL, et al. Intragastric balloon as bridging therapy prior to bariatric surgery for patients with severe obesity (BMI ≥ 50 kg/m2): a systematic review and meta-analysis. Obes Surg. 2022;32(2):489–502. https://doi.org/10.1007/s11695-021-05772-5.
Rebecca Voelker MSJ. Deaths reported after intragastric balloon surgery. JAMA. 2017;318(11):996. https://doi.org/10.1001/jama.2017.12984.
Omalu BI, Ives DG, Buhari AM, et al. Death rates and causes of death after bariatric surgery for Pennsylvania residents, 1995 to 2004. Arch Surg. 2007;142(10):923–8; discussion 929. https://doi.org/10.1001/archsurg.142.10.923.
Murad MH, Sultan S, Haffar S, et al. Methodological quality and synthesis of case series and case reports. BMJ Evid Based Med. 2018;23(2):60–3. https://doi.org/10.1136/bmjebm-2017-110853.
“EAG/A1C conversion calculator.” EAG/A1C conversion calculator, American Diabetes Association. https://professional.diabetes.org/diapro/glucose_calc. Accessed 11/1/2021
Balk EM, Earley A, Patel K, et al. Empirical assessment of within-arm correlation imputation in trials of continuous outcomes [Internet]. Rockville (MD): Agency for Healthcare Research and Quality (US); 2012 Nov. Report No.: 12(13)-EHC141-EF.
Chan AO, Chow WS, Lam KF, et al. The effect of intragastric balloon placement on weight loss and type 2 diabetes control. Aliment Pharmacol Ther. 2008;28(1):162–4. https://doi.org/10.1111/j.1365-2036.2008.03687.x.
Mariani S, Fiore D, Persichetti A, et al. Circulating SIRT1 increases after intragastric balloon fat loss in obese patients. Obes Surg. 2016;26(6):1215–20. https://doi.org/10.1007/s11695-015-1859-4.
Takihata M, Nakamura A, Aoki K, et al. Comparison of intragastric balloon therapy and intensive lifestyle modification therapy with respect to weight reduction and abdominal fat distribution in super-obese Japanese patients. Obes Res Clin Pract. 2014;8(4):e331-8. https://doi.org/10.1016/j.orcp.2013.07.002.
Bazerbachi F, Vargas EJ, Rizk M, et al. Intragastric balloon placement induces significant metabolic and histologic improvement in patients with nonalcoholic steatohepatitis. Clin Gastroenterol Hepatol. 2021;19(1):146-154.e4. https://doi.org/10.1016/j.cgh.2020.04.068.
Crea N, Pata G, Della Casa D, et al. Improvement of metabolic syndrome following intragastric balloon: 1 year follow-up analysis. Obes Surg. 2009;19(8):1084–8. https://doi.org/10.1007/s11695-009-9879-6.
Donadio F, Sburlati LF, Masserini B, et al. Metabolic parameters after BioEnterics intragastric balloon placement in obese patients. J Endocrinol Invest. 2009;32(2):165–8. https://doi.org/10.1007/BF03345708.
Forlano R, Ippolito AM, Iacobellis A, et al. Effect of the BioEnterics intragastric balloon on weight, insulin resistance, and liver steatosis in obese patients. Gastrointest Endosc. 2010;71(6):927–33. https://doi.org/10.1016/j.gie.2009.06.036.
Koc F, Kayaoglu HA, Celik A, et al. Effect of weight loss induced by intragastric balloon therapy on cardiac function in morbidly obese individuals: a pilot study. Med Princ Pract. 2015;24(5):432–5. https://doi.org/10.1159/000431177.
Mafort TT, Madeira E, Madeira M, et al. Six-month intragastric balloon treatment for obesity improves lung function, body composition, and metabolic syndrome. Obes Surg. 2014;24(2):232–40. https://doi.org/10.1007/s11695-013-1061-5.
Mirošević G, Nikolić M, Kruljac I, et al. Decrease in insulin resistance has a key role in improvement of metabolic profile during intragastric balloon treatment. Endocrine. 2014;45(2):331–4. https://doi.org/10.1007/s12020-013-0069-x.
Mui WL, Ng EK, Tsung BY, et al. Impact on obesity-related illnesses and quality of life following intragastric balloon. Obes Surg. 2010;20(8):1128–32. https://doi.org/10.1007/s11695-008-9766-6.
Nikolic M, Mirosevic G, Ljubicic N, et al. Obesity treatment using a Bioenterics intragastric balloon (BIB)–preliminary Croatian results. Obes Surg. 2011;21(8):1305–10. https://doi.org/10.1007/s11695-010-0101-7.
Sekino Y, Imajo K, Sakai E, et al. Time-course of changes of visceral fat area, liver volume and liver fat area during intragastric balloon therapy in Japanese super-obese patients. Intern Med. 2011;50(21):2449–55. https://doi.org/10.2169/internalmedicine.50.5672.
Stimac D, Majanović SK, Turk T, et al. Intragastric balloon treatment for obesity: results of a large single center prospective study. Obes Surg. 2011;21(5):551–5. https://doi.org/10.1007/s11695-010-0310-0.
Vargas EJ, Pesta CM, Bali A, et al. Single fluid-filled intragastric balloon safe and effective for inducing weight loss in a real-world population. Clin Gastroenterol Hepatol. 2018;16(7):1073-1080.e1. https://doi.org/10.1016/j.cgh.2018.01.046.
Agnihotri A, Xie A, Bartalos C, et al. Real-world safety and efficacy of fluid-filled dual intragastric balloon for weight loss. Clin Gastroenterol Hepatol. 2018;16(7):1081-1088.e1. https://doi.org/10.1016/j.cgh.2018.02.026.
Al Kahtani K, Khan MQ, Helmy A, et al. Bio-enteric intragastric balloon in obese patients: a retrospective analysis of King Faisal Specialist Hospital experience. Obes Surg. 2010;20(9):1219–26. https://doi.org/10.1007/s11695-008-9654-0.
Siebenhofer A, Winterholer S, Jeitler K, et al. Long-term effects of weight-reducing drugs in people with hypertension. Cochrane Database Syst Rev. 2021;1(1):CD007654. Published 2021 Jan 17. https://doi.org/10.1002/14651858.CD007654.pub5
Blood pressure lowering treatment trialists’ collaboration. Pharmacological blood pressure lowering for primary and secondary prevention of cardiovascular disease across different levels of blood pressure: an individual participant-level data meta-analysis [published correction appears in Lancet. 2021;397(10288):1884]. Lancet. 2021;397(10285):1625–1636. https://doi.org/10.1016/S0140-6736(21)00590-0
Capristo E, Maione A, Lucisano G, et al. Effects of weight loss medications on mortality and cardiovascular events: a systematic review of randomized controlled trials in adults with overweight and obesity. Nutr Metab Cardiovasc Dis. 2021;31(9):2587–95. https://doi.org/10.1016/j.numecd.2021.05.023.
Prospective Studies Collaboration, Lewington S, Whitlock G, et al. Blood cholesterol and vascular mortality by age, sex, and blood pressure: a meta-analysis of individual data from 61 prospective studies with 55,000 vascular deaths [published correction appears in Lancet. 2008;372(9635):292]. Lancet. 2007;370(9602):1829–1839. https://doi.org/10.1016/S0140-6736(07)61778-4
Monami M, Candido R, Pintaudi B, et al. Improvement of glycemic control in type 2 diabetes: a systematic review and meta-analysis of randomized controlled trials. Nutr Metab Cardiovasc Dis. 2021;31(9):2539–46. https://doi.org/10.1016/j.numecd.2021.05.010.
Tsapas A, Avgerinos I, Karagiannis T, et al. Comparative effectiveness of glucose-lowering drugs for type 2 diabetes: a systematic review and network meta-analysis. Ann Intern Med. 2020;173(4):278–86. https://doi.org/10.7326/M20-0864.
Maiorino MI, Longo M, Scappaticcio L, et al. Improvement of glycemic control and reduction of major cardiovascular events in 18 cardiovascular outcome trials: an updated meta-regression. Cardiovasc Diabetol. 2021;20(1):210. Published 2021 Oct 18. https://doi.org/10.1186/s12933-021-01401-8.
Cavero-Redondo I, Peleteiro B, Álvarez-Bueno C, et al. Glycated haemoglobin A1c as a risk factor of cardiovascular outcomes and all-cause mortality in diabetic and non-diabetic populations: a systematic review and meta-analysis. BMJ Open. 2017;7(7):e015949. Published 2017 Jul 31. https://doi.org/10.1136/bmjopen-2017-015949.
Fralick M, Colacci M, Odutayo A, et al. Lowering of hemoglobin A1C and risk of cardiovascular outcomes and all-cause mortality, a meta-regression analysis. J Diabetes Complicat. 2020;34(11):107704. https://doi.org/10.1016/j.jdiacomp.2020.107704.
Sherifali D, Nerenberg K, Pullenayegum E, et al. The effect of oral antidiabetic agents on A1C levels: a systematic review and meta-analysis. Diabetes Care. 2010;33(8):1859–64. https://doi.org/10.2337/dc09-1727.
Popov VB, Ou A, Schulman AR, et al. The impact of intragastric balloons on obesity-related co-morbidities: a systematic review and meta-analysis. Am J Gastroenterol. 2017;112(3):429–39. https://doi.org/10.1038/ajg.2016.530.
de Freitas Júnior JR, Ribeiro IB, de Moura DTH, et al. Effects of intragastric balloon placement in metabolic dysfunction-associated fatty liver disease: A systematic review and meta-analysis. World J Hepatol. 2021;13(7):815–29. https://doi.org/10.4254/wjh.v13.i7.815.
Rucker G, Schwarzer G, Carpenter JR, et al. Undue reliance on I(2) in assessing heterogeneity may mislead. BMC Med Res Methodol. 2008;8:79.
Machytka E, Klvana P, Hanuskova I, et al. Use of pharmacotherapy for long-term maintenance of weight loss following explantation of intragastric balloon (BIB). Gut. 2007;57:A290.
Farina MG, Baratta R, Nigro A, et al. Intragastric balloon in association with lifestyle and/or pharmacotherapy in the long-term management of obesity. Obes Surg. 2012r;22(4):565–71. https://doi.org/10.1007/s11695-011-0514-y.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. For this type of study, formal consent is not required.
Informed Consent
Informed consent does not apply.
Conflict of Interest
Sunil Amin is a consultant for Boston Scientific and MicroTech. However, no grant or outside funding was used for this project. The other authors (RHS, SV, SK, MP, SB) declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Key Points
• IGB led to significant improvements in A1c, SBP, DBP, TC, LDL, and TG.
• IGB should be considered with lifestyle changes and pharmacotherapy for patients.
• Long-term data is limited preventing conclusive decisions on the effectiveness of IGB.
Supplementary Information
ESM 1
(PDF 88.3 kb)
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Shah, R.H., Vedantam, S., Kumar, S. et al. Intragastric Balloon Significantly Improves Metabolic Parameters at 6 Months: a Meta-Analysis. OBES SURG 33, 725–732 (2023). https://doi.org/10.1007/s11695-022-06437-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-022-06437-7