Abstract
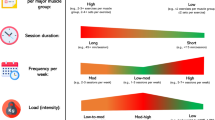
Athletes employ high-intensity training to promote their physical fitness. However, high-intensity training can harm the immune system, making athletes susceptible to URTI, and negatively affecting their performance in sports. In addition, the athlete’s diet should be paid more attention to as it is another issue influencing the immune system, especially during the URTI. The present study attempts to discuss the impact of different training intensities on athletes' immune system function, as well as the management of upper respiratory traction infections. An online search was done in web of science (WoS), Ovid, Scopus, and PubMed (MeSH) databases with the following combination of keywords: “Upper Respiratory Tract Infections”, “Exercise Training”, and “Athletes”. The results of our overview showed that regular and moderate-intensity training can reduce the relative risk of URTI, improve immune function and physical fitness. Moreover, we found that prolonged and high-intensity training can increase the relative risk of URTI, which leads to a decrease in aerobic performance, and also lessens physical fitness. Although high-intensity training can suppress the immune system, elite athletes should not stop training during the time of URTI. Based on the available evidence, it may be recommended to exercise during the URTI outbreak. Therefore, the first step in managing athletes’ URTI is to reduce exercise intensity (the open window hypothesis may actually increase the susceptibility to URTI), with the utilization of nutritional strategies as the second step. However, athletes with severe and major URTI symptoms (e.g., severe sore throat, fever, cough, myalgia, shortness of breath, general fatigue) should avoid training and must have active rest (i.e., low-intensity exercise), as well as protein supplementation and low-intensity resistance training. Third, athletes with mild and minor URTI symptoms (e.g., runny nose, sinus congestion, mild sore throat) can perform aerobic training and moderate-intensity training, and benefit from improved immune function according to the J-shaped model. Functional nutritional strategies include avoiding sudden dietary changes, receiving 50% of total daily calories from carbohydrates consumption: 30–90 g/h in competitions (depending on the intensity and duration of exercise), protein consumption: 1.3 to 1.8 g/kg bw/day, flavonoids intake, herbal supplements intake, probiotic supplementation intake, and taking vitamins C and D.

Similar content being viewed by others
Referencess
Gleeson M (2007) Immune function in sport and exercise. J Appl Physiol 103(2):693–699
Walsh NP, Gleeson M, Shephard RJ, Gleeson M, Woods JA, Bishop NC, Fleshner M, Green C, Pedersen BK, Hoffman-Goetz L, Rogers CJ, Northoff H, Abbasi A, Simon P (2011) Position 27 Exercise Regulates the Immune System statement. Part one: immune function and exercise. ExercImmunol Rev 17:6–63
Nieman DC, Nehlsen-Cannarella SL (1994) The immune response to exercise. Sem Hematol 31(2):166–179
Lowder T, Padgett DA, Woods JA (2005) Moderate exercise protects mice from death due to influenza virus. Brain Behav Immun 19(5):377–380
Brown AS, Davis JM, Murphy EA, Carmichael MD, Ghaffar A, Mayer EP (2004) Gender differences in viral infection after repeated exercise stress. Med Sci Sports Exerc 36(8):1290–1295
Wong CM, Lai HK, Ou CQ, Ho SY, Chan KP, Thach TQ, Peiris JSM (2008) Is exercise protective against influenza-associated mortality? PLoS ONE 3(5):e2108
Nieman DC, Henson DA, Gusewitch G, Warren BJ, Dotson RC, Butterworth DE, Nehlsen-Cannarella SL (1993) Physical activity and immune function in elderly women. Med Sci Sports Exerc 25(7):823–831
Nieman DC, Johanssen LM, Lee JW (1989) Infectious episodes in runners before and after a roadrace. J Sports Med Phys Fitness 29(3):289–296
Nieman DC, Johanssen LM, Lee JW, Arabatzis K (1990) Infectious episodes in runners before and after the Los Angeles Marathon. J Sports Med Phys Fitness 30(3):316–328
Asimakos A, Toumpanakis D, Karatza MH, Vasileiou S, Katsaounou P, Mastora Z, Vassilakopoulos T (2018) Immune cell response to strenuous resistive breathing: comparison with whole body exercise and the effects of antioxidants. Int J Chron Obstruct Pulmon Dis 13:529–545
Nieman DC, Nehlsen-Cannarella SL, Markoff PA, Balk-Lamberton AJ, Yang H, Chritton DBW, Arabatzis K (1990) The effects of moderate exercise training on natural killer cells and acute upper respiratory tract infections. Int J Sports Med 11(06):467–473
Schouten WJ, Verschuur R, Kemper HCG (1988) Physical activity and upper respiratory tract infections in a normal population of young men and women: the Amsterdam growth and health study. Int J Sports Med 9(06):451–455
Cramer SR, Nieman DC, Lee JW (1991) The effects of moderate exercise training on psychological well-being and mood state in women. J Psychosom Res 35(4–5):437–449
Pyne DB, Baker MS, Fricker PA, Mcdonald WA, Telford RD, Weidemann MJ (1995) Effects of an intensive 12-wk training program by elite swimmers on neutrophil oxidative activity. Med Sci Sports Exer 27(4):536–542
Mackinnon LT, Ginn EM, Seymour GJ (1993) Temporal relationship between decreased salivary IgA and upper respiratory tract infection in elite athletes. Aust J Sci Med Sport 25(4):94–99
Lee DJ, Meehan RT, Robinson C, Mabry TR, Smith ML (1992) Immune responsiveness and risk of illness in US Air Force Academy cadets during basic cadet training. Aviat Space Environ Med 63(6):517–523
Matthews CE, Ockene IS, Freedson PS, Rosal MC, Merriam PA, Hebert JR (2002) Moderate to vigorous physical activity and risk of upper-respiratory tract infection. Med Sci Sports Exer 34(8):1242–1248
Łagowska K, Bajerska J (2021) Probiotic supplementation and respiratory infection and immune function in athletes: systematic review and meta-analysis of randomized controlled trials. J Athl Train 56(11):1213–1223
Umeda M, Tominaga T, Kozuma K, Kitazawa H, Furushima D, Hibi M, Yamada H (2021) Preventive effects of tea and tea catechins against influenza and acute upper respiratory tract infections: A systematic review and meta-analysis. Eur J Nutr 34:1–14
Kim TK, Lim HR, Byun JS (2022) Vitamin C supplementation reduces the odds of developing a common cold in Republic of Korea Army recruits: randomised controlled trial. BMJ Mil Health 168(2):117–123
Kostka TOMASZ, Berthouze SE, Lacour J, Bonnefoy MARC (2000) The symptomatology of upper respiratory tract infections and exercise in elderly people. Med Sci Sports Exerc 32(1):46–51
Weidner TG, Cranston TRACY, Schurr TERRY, Kaminsky LA (1998) The effect of exercise training on the severity and duration of a viral upper respiratory illness. Med Sci Sports Exer 30(11):1578–1583
Weidner BL, Gotsch AR, Delnevo CD, Newman JB, McDonald B (1998) Worker health and safety training: assessing impact among responders. Am J Ind Med 33(3):241–246
Moreira A, Delgado L, Moreira P, Haahtela T (2009) Does exercise increase the risk of upper respiratory tract infections? Br Med Bull 90(1):111–131
Fricker PA, Pyne DB, Saunders PU, Cox AJ, Gleeson M, Telford RD (2005) Influence of training loads on patterns of illness in elite distance runners. Clin J Sport Med 15(4):246–252
Ekblom B, Ekblom Ö, Malm C (2006) Infectious episodes before and after a marathon race. Scand J Med Sci Sports 16(4):287–293
Malm C (2006) Susceptibility to infections in elite athletes: the S-curve. Scand J Med Sci Sports 16(1):4–6
Shirvani H, Rostamkhani F (2020) Exercise considerations during coronavirus disease 2019 (COVID-19) Outbreak: A narrative review. J Military Med 22(2):161–168
Nieman DC (2000) Is infection risk linked to exercise workload? Med Sci Sports Exer 32(7):S406–S411
Klentrou P, Cieslak T, MacNeil M, Vintinner A, Plyley M (2002) Effect of moderate exercise on salivary immunoglobulin A and infection risk in humans. Eur J Appl Physiol 87:153–158
Gleeson MAREE, McDONALD WA, Pyne DB, Cripps AW, Francis JL, Fricker PA, Clancy RL (1999) Salivary IgA levels and infection risk in elite swimmers. Med Sci Sports Exerc 31(1):67–73
Rico-González M, Clemente FM, Oliveira R, Bustamante-Hernández N, Pino-Ortega J (2021) Part I: relationship among training load management, salivary immunoglobulin A, and upper respiratory tract infection in team sport: A systematic review. Healthcare 9(4):366
Cicchella A, Stefanelli C, Massaro M (2021) Upper respiratory tract infections in sport and the immune system response: a review. Biology 10(5):362
Drummond LR, Campos HO, Drummond FR, de Oliveira GM, Fernandes JGRP, Amorim RP, Coimbra CC (2022) Acute and chronic effects of physical exercise on IgA and IgG levels and susceptibility to upper respiratory tract infections: a systematic review and meta-analysis. PflügersArchiv-Eur J Physiol 474(12):1221–1248
Peters EM, Bateman ED (1983) Ultramarathon running and upper respiratory tract infections-an epidemiological survey. S Afr Med J 64(16):582–584
Nieman DC (1997) Risk of upper respiratory tract infection in athletes: an epidemiologic and immunologic perspective. J Athl Train 32(4):344
Gleeson M, Hall ST, McDonald WA, Flanagan AJ, Clancy RL (1999) Salivary IgA subclasses and infection risk in elite swimmers. Immunol Cell Biol 77(4):351–355
Linde GA, Granström M, Orvell C (1987) Immunoglobulin class and immunoglobulin G subclass enzyme-linked immunosorbent assays compared with microneutralization assay for serodiagnosis of mumps infection and determination of immunity. J Clin Microbiol 25(9):1653–1658
Bury T, Marechal R, Mahieu P, Pirnay F (1998) Immunological status of competitive football players during the training season. Int J Sports Med 19(05):364–368
Foster CARL (1998) Monitoring training in athletes with reference to overtraining syndrome. Med Sci Sports Exer 30(7):1164–1168
Illing JW, Miller FJ, Gardner DE (1980) Decreased resistance to infection in exercised mice exposed to NO2 and O3. J Toxicol Environ Health Part A 6(4):843–851
Shephard RJ, Shek PN, DiNubile NA (1999) Exercise, immunity, and susceptibility to infection: a j-shaped relationship? Phys Sports Med 27(6):47–71
Gleeson M, Pyne DB (2016) Respiratory inflammation and infections in high-performance athletes. Immunol Cell Biol 94(2):124–131
Walsh NP, Oliver SJ (2016) Exercise, immune function and respiratory infection: An update on the influence of training and environmental stress. Immunol Cell Biol 94(2):132–139
Couto M, Silva D, Delgado L, Moreira A (2013) Exercise and airway injury in athletes. Acta Med Port 26(1):56–60
Nieman DC, Wentz LM (2019) The compelling link between physical activity and the body’s defense system. J Sport Health Sci 8(3):201–217
Bruunsgaard HELLE, Hartkopp ANDREAS, Mohr THOMAS, Konradsen HELLE, Heron IVER, Mordhorst CH, Pedersen BK (1997) In vivo cell-mediated immunity and vaccination response following prolonged, intense exercise. Med Sci Sports Exerc 29(9):1176–1181
Sabzevari Rad R, Noodeh FA, Moradi A (2021) Strategies to prevent the harmful effects of environmental pollutants on the athletes’ respiratory performance: A review. J Milit Health Promotion 1(4):224–236
Douglas DJ (1978) Upper respiratory infections in the conditioned athlete. Med Sci Sports Exerc 10:55
Shephard RJ, Kavanagh T, Mertens DJ, Qureshi S, Clark M (1995) Personal health benefits of Masters athletics competition. Br J Sports Med 29(1):35–40
Heath GW, Ford ES, Craven TE, Macera CA, Jackson KL, Pate RR (1991) Exercise and the incidence of upper respiratory tract infections. Med Sci Sports Exer 23(2):152–157
Peters EM (1997) Exercise, immunology and upper respiratory tract infections. Int J Sports Med 18(S1):S69–S77
Österback L, Qvarnberg Y (1987) A Prospective Study of Respiratory Infections in 12-Year-Old Children Actively Engaged in Sports. Acta Pædiatrica 76(6):944–949
Buddgett RG (1989) Illness and injury in international oarsmen. Clinical Sports Medicine 1:57–61
Linde F (1987) Running and upper respiratory tract infections. Scand J sports Sci 9:21–23
Strauss RH, Lanese RR, Leizman DJ (1988) Illness and absence among wrestlers, swimmers, and gymnasts at a large university. Am J Sports Med 16(6):653–655
Berglund B, Hemmingson P (1990) Infectious disease in elite cross-country skiers: a one-year incidence study. Clin Sports Med 2(1):19–23
Linenger JM, Flinn S, Thomas B, Johnson CW (1993) Musculoskeletal and medical morbidity associated with rigorous physical training. Clin J Sport Med 3(4):229–234
Seyfried PL, Tobin RS, Brown NE, Ness PF (1985) A prospective study of swimming-related illness. I. Swimming-associated health risk. Am J Public Health 75(9):1068–1070
Grimby G (1962) Exercise in man during pyrogen-induced fever. Scand J Clin Lab Invest 14:1–112
Friman G, Wesslén L (2000) Infections and exercise in high-performance athletes. Immunol Cell Biol 78(5):510–522
Gleeson M, Nieman DC, Pedersen BK (2004) Exercise, nutrition and immune function. J Sports Sci 22(1):115–125
Suzuki M, Umeda T, Nakaji S, Shimoyama T, Mashiko T, Sugawara K (2004) Effect of incorporating low intensity exercise into the recovery period after a rugby match. Br J Sports Med 38(4):436–440
Beisel WR, Sawyer WD, Ryll ED, Crozier D (1967) Metabolic effects of intracellular infections in man. Ann Intern Med 67(4):744–779
Gade J, Beck AM, Andersen HE, Christensen B, Rønholt F, Klausen TW, Astrup A (2019) Protein supplementation combined with low-intensity resistance training in geriatric medical patients during and after hospitalisation: a randomised, double-blind, multicentre trial. Br J Nutr 122(9):1006–1020
Nieman DC, Pedersen BK (1999) Exercise and immune function: recent developments. Sports Med 27:73–80
Miles MP, Kraemer WJ, Grove DS, Leach SK, Dohi K, Bush JA, Mastro AM (2002) Effects of resistance training on resting immune parameters in women. Eur J Appl Physiol 87:506–508
Peake J, Wilson G, Mackinnon L, Coombes JS (2005) Carbohydrate supplementation and alterations in neutrophils, and plasma cortisol and myoglobin concentration after intense exercise. Eur J Appl Physiol 93:672–678
Dorneles GP, Haddad DO, Fagundes VO, Vargas BK, Kloecker A, Romão PR, Peres A (2016) High intensity interval exercise decreases IL-8 and enhances the immunomodulatory cytokine interleukin-10 in lean and overweight–obese individuals. Cytokine 77:1–9
Spruit MA, Singh SJ, Garvey C, ZuWallack R, Nici L, Rochester C, Wouters EF (2013) An official American Thoracic Society/European Respiratory Society statement: key concepts and advances in pulmonary rehabilitation. Am J Respir Crit Care Med 188(8):e13–e64
Mertz KH, Reitelseder S, Bechshoeft R, Bulow J, Højfeldt G, Jensen M, Holm L (2021) The effect of daily protein supplementation, with or without resistance training for 1 year, on muscle size, strength, and function in healthy older adults: A randomized controlled trial. Am J Clin Nutr 113(4):790–800
Chapman S, Chung HC, Rawcliffe AJ, Izard R, Smith L, Roberts JD (2021) Does protein supplementation support adaptations to arduous concurrent exercise training? a systematic review and meta-analysis with military based applications. Nutrients 13(5):1416
Strasser B, Geiger D, Schauer M, Gostner JM, Gatterer H, Burtscher M, Fuchs D (2016) Probiotic supplements beneficially affect tryptophan–kynurenine metabolism and reduce the incidence of upper respiratory tract infections in trained athletes: A randomized, double-blinded, placebo-controlled trial. Nutrients 8(11):752
Somerville VS, Braakhuis AJ, Hopkins WG (2016) Effect of flavonoids on upper respiratory tract infections and immune function: a systematic review and meta-analysis. Adv Nutr 7(3):488–497
Witard OC, Turner JE, Jackman SR, Kies AK, Jeukendrup AE, Bosch JA, Tipton KD (2014) High dietary protein restores overreaching induced impairments in leukocyte trafficking and reduces the incidence of upper respiratory tract infection in elite cyclists. Brain Behav Immun 39:211–219
Kawanishi N, Kato K, Takahashi M, Mizokami T, Otsuka Y, Imaizumi A, Suzuki K (2013) Curcumin attenuates oxidative stress following downhill running-induced muscle damage. Biochem Biophys Res Commun 441(3):573–578
Ruhee RT, Ma S, Suzuki K (2020) Protective effects of sulforaphane on exercise-induced organ damage via inducing antioxidant defense responses. Antioxidants 9(2):136
Koch AJ (2010) Immune response to exercise. Braz J Biomotricity 4(2):92–103
Funding
No funds were received in support of this work.
Author information
Authors and Affiliations
Contributions
This article was written only by Reza Sabzevari Rad and no author participated in writing it.
Corresponding author
Ethics declarations
Conflict of interest
The author declare no conflict of interest.
Ethical approval
This article does not contain any studies with human participants performed by any of the author.
Informed consent
As the study is an article review, there is no informed consent.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Sabzevari Rad, R. The impact of different training intensities on athletes' immune system function and the management of upper respiratory traction infections: a narrative review. Sport Sci Health 20, 415–426 (2024). https://doi.org/10.1007/s11332-023-01110-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11332-023-01110-7