Abstract
Purpose
We are attempting to develop a navigation system for safe and effective peripancreatic lymphadenectomy in gastric cancer surgery. As a preliminary study, we examined whether or not the peripancreatic dissection line could be learned by a machine learning model (MLM).
Methods
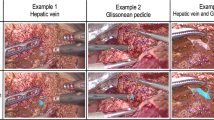
Among the 41 patients with gastric cancer who underwent radical gastrectomy between April 2019 and January 2020, we selected 6 in whom the pancreatic contour was relatively easy to trace. The pancreatic contour was annotated by a trainer surgeon in 1242 images captured from the video recordings. The MLM was trained using the annotated images from five of the six patients. The pancreatic contour was then segmented by the trained MLM using images from the remaining patient. The same procedure was repeated for all six combinations.
Results
The median maximum intersection over union of each image was 0.708, which was higher than the threshold (0.5). However, the pancreatic contour was misidentified in parts where fatty tissue or thin vessels overlaid the pancreas in some cases.
Conclusion
The contour of the pancreas could be traced relatively well using the trained MLM. Further investigations and training of the system are needed to develop a practical navigation system.





Similar content being viewed by others
References
Bray F, Ferlay J, Soerjomataram I, Siegel RL, Torre LA. Jemal a global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin. 2018;68:394–424.
Yuya S, Kazuyuki K, Mikito I, Keiji K, Hirofumi S, Sho O, et al. Intraoperative pancreatic injury gives rise to severe postoperative pancreatic fistula: results of a review of unedited videos of the laparoscopic surgical procedures. Int Surg. 2021;105:359–65.
He K, Gkioxari G, Dollar P. Girshick R Mask R-CNN. IEEE Trans Pattern Anal Mach Intell. 2020;42:386–97.
Lin T-Y, Maire M, Belongie S, Hays J, Perona P, Ramanan D, et al Microsoft COCO: common objects in context. Lecture Notes Comput Sci. 2014:740–55
Selvaraj MG, Vergara A, Ruiz H, Safari N, Elayabalan S, Ocimati W, et al AI-powered banana diseases and pest detection. Plant Methods. 2019; 15
Madad Zadeh S, Francois T, Calvet L, Chauvet P, Canis M, Bartoli A, et al. SurgAI: deep learning for computerized laparoscopic image understanding in gynaecology. Surg Endosc. 2020;34:5377–89.
Caicedo JC, Roth J, Goodman A, Becker T, Karhohs KW, Broisin M, et al. Evaluation of deep learning strategies for nucleus segmentation in fluorescence images. Cytometry A. 2019;95:952–65.
Ieiri S, Uemura M, Konishi K, Souzaki R, Nagao Y, Tsutsumi N, et al. Augmented reality navigation system for laparoscopic splenectomy in children based on preoperative CT image using optical tracking device. Pediatr Surg Int. 2012;28:341–6.
Kenngott HG, Neuhaus J, Muller-Stich BP, Wolf I, Vetter M, Meinzer HP, et al. Development of a navigation system for minimally invasive esophagectomy. Surg Endosc. 2008;22:1858–65.
Marescaux J, Rubino F, Arenas M, Mutter D. Soler L Augmented-reality-assisted laparoscopic adrenalectomy. JAMA. 2004;292:2214–5.
Okamoto T, Onda S, Matsumoto M, Gocho T, Futagawa Y, Fujioka S, et al. Utility of augmented reality system in hepatobiliary surgery. J Hepatobiliary Pancreat Sci. 2013;20:249–53.
Onda S, Okamoto T, Kanehira M, Suzuki F, Ito R, Fujioka S, et al. Identification of inferior pancreaticoduodenal artery during pancreaticoduodenectomy using augmented reality-based navigation system. J Hepatobiliary Pancreat Sci. 2014;21:281–7.
Wengert C, Bossard L, Haberling A, Baur C, Szekely G. Cattin PC endoscopic navigation for minimally invasive suturing. Med Image Comput Comput Assist Interv. 2007;10:620–7.
Ortmaier T, Groger M, Boehm DH, Falk V. Hirzinger G motion estimation in beating heart surgery. IEEE Trans Biomed Eng. 2005;52:1729–40.
Mountney P, Lo B, Thiemjarus S, Stoyanov D. Zhong-Yang G A probabilistic framework for tracking deformable soft tissue in minimally invasive surgery. Med Image Comput Comput Assist Interv. 2007;10:34–41.
Mylonas GP, Stoyanov D, Deligianni F, Darzi A. Yang GZ Gaze-contingent soft tissue deformation tracking for minimally invasive robotic surgery. Med Image Comput Comput Assist Interv. 2005;8:843–50.
Stoyanov D. Yang GZ Soft tissue deformation tracking for robotic assisted minimally invasive surgery. Conf Proc IEEE Eng Med Biol Soc. 2009;2009:254–7.
Acknowledgements
We would like to thank Enago (https://www.enago.jp/) for the English language editing.
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Sato, Y., Sese, J., Matsuyama, T. et al. Preliminary study for developing a navigation system for gastric cancer surgery using artificial intelligence. Surg Today 52, 1753–1758 (2022). https://doi.org/10.1007/s00595-022-02508-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00595-022-02508-5