Abstract
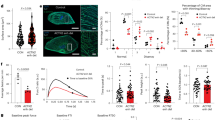
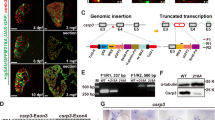
Connexin43 (Cx43) exits as hemichannels in the inner mitochondrial membrane. We examined how mitochondrial Cx43 and mitochondrial KATP channels affect the occurrence of triggered arrhythmias. To generate cardiac-specific Cx43-deficient (cCx43−/−) mice, Cx43flox/flox mice were crossed with α-MHC (Myh6)-cre+/− mice. The resulting offspring, Cx43flox/flox/Myh6-cre+/− mice (cCx43−/− mice) and their littermates (cCx43+/+ mice), were used. Trabeculae were dissected from the right ventricles of mouse hearts. Cardiomyocytes were enzymatically isolated from the ventricles of mouse hearts. Force was measured with a strain gauge in trabeculae (22°C). To assess arrhythmia susceptibility, the minimal extracellular Ca2+ concentration ([Ca2+]o,min), at which arrhythmias were induced by electrical stimulation, was determined in trabeculae. ROS production was estimated with 2′,7′-dichlorofluorescein (DCF), mitochondrial membrane potential with tetramethylrhodamine methyl ester (TMRM), and Ca2+ spark frequency with fluo-4 and confocal microscopy in cardiomyocytes. ROS production within the mitochondria was estimated with MitoSoxRed and mitochondrial Ca2+ with rhod-2 in trabeculae. Diazoxide was used to activate mitochondrial KATP. Most of cCx43−/− mice died suddenly within 8 weeks. Cx43 was present in the inner mitochondrial membrane in cCx43+/+ mice but not in cCx43−/− mice. In cCx43−/− mice, the [Ca2+]o,min was lower, and Ca2+ spark frequency, the slope of DCF fluorescence intensity, MitoSoxRed fluorescence, and rhod-2 fluorescence were higher. TMRM fluorescence was more decreased in cCx43−/− mice. Most of these changes were suppressed by diazoxide. In addition, in cCx43−/− mice, antioxidant peptide SS-31 and N-acetyl-L-cysteine increased the [Ca2+]o,min. These results suggest that Cx43 deficiency activates Ca2+ leak from the SR, probably due to depolarization of mitochondrial membrane potential, an increase in mitochondrial Ca2+, and an increase in ROS production, thereby causing triggered arrhythmias, and that Cx43 hemichannel deficiency may be compensated by activation of mitochondrial KATP channels in mouse hearts.






Similar content being viewed by others
Data availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Akar FG, Aon MA, Tomaselli GF, O’Rourke B (2005) The mitochondrial origin of postischemic arrhythmias. J Clin Invest 115:3527–3535. https://doi.org/10.1172/JCI25371
Andersson DC, Fauconnier J, Yamada T, Lacampagne A, Zhang SJ, Katz A, Westerblad H (2011) Mitochondrial production of reactive oxygen species contributes to the β-adrenergic stimulation of mouse cardiomyocytes. J Physiol 589:1791–1801. https://doi.org/10.1113/jphysiol.2010.202838
Boengler K, Ruiz-Meana M, Gent S, Ungefug E, Soetkamp D, Miro-Casas E, Cabestrero A, Fernandez-Sanz C, Semenzato M, Di Lisa F, Rohrbach S, Garcia-Dorado D, Heusch G, Schulz R (2012) Mitochondrial connexin 43 impacts on respiratory complex I activity and mitochondrial oxygen consumption. J Cell Mol Med 16:1649–1655. https://doi.org/10.1111/j.1582-4934.2011.01516.x
Boengler K, Lochnit G, Schulz R (2018) Mitochondria “THE” target of myocardial conditioning. Am J Physiol Heart Circ Physiol 315:H1215–H1231. https://doi.org/10.1152/ajpheart.00124.2018
Brandes R, Bers DM (2002) Simultaneous measurements of mitochondrial NADH and Ca2+ during increased work in intact rat heart trabeculae. Biophys J 83:587–604. https://doi.org/10.1016/S0006-3495(02)75194-1
Brown DA, Aon MA, Frasier CR, Sloan RC, Maloney AH, Anderson EJ, O’Rourke B (2010) Cardiac arrhythmias induced by glutathione oxidation can be inhibited by preventing mitochondrial depolarization. J Mol Cell Cardiol 48:673–679. https://doi.org/10.1016/j.yjmcc.2009.11.011
Chavez JD, Tang X, Campbell MD, Reyes G, Kramer PA, Stuppard R, Keller A, Zhang H, Rabinovitch PS, Marcinek DJ, Bruce JE (2020) Mitochondrial protein interaction landscape of SS-31. Proc Natl Acad Sci USA 117:15363–15373. https://doi.org/10.1073/pnas.2002250117
Chen F, Hadfield JM, Berzingi C, Hollander JM, Miller DB, Nichols CE, Finkel MS (2013) N-acetylcysteine reverses cardiac myocyte dysfunction in a rodent model of behavioral stress. J Appl Physiol 115:514–524. https://doi.org/10.1152/japplphysiol.01471.2012
Coetzee WA (2013) Multiplicity of effectors of the cardioprotective agent, diazoxide. Pharmacol Ther 140:167–175. https://doi.org/10.1016/j.pharmthera.2013.06.007
Cottet-Rousselle C, Ronot X, Leverve X, Mayol JF (2011) Cytometric assessment of mitochondria using fluorescent probes. Cytometry A 79:405–425. https://doi.org/10.1002/cyto.a.21061
Danik SB, Liu F, Zhang J, Suk HJ, Morley GE, Fishman GI, Gutstein DE (2004) Modulation of cardiac gap junction expression and arrhythmic susceptibility. Circ Res 95:1035–1041. https://doi.org/10.1161/01.RES.0000148664.33695.2a
De Vuyst E, Wang N, Decrock E, de Bock M, Vinken M, van Moorhem M, Lai C, Culot M, Rogiers V, Cecchelli R, Naus CC, Evans WH, Leybaert L (2009) Ca2+ regulation of connexin 43 hemichannels in C6 glioma and glial cells. Cell Calcium 46:176–187. https://doi.org/10.1016/j.ceca.2009.07.002
Guerrero PA, Schuessler RB, Davis LM, Beyer EC, Johnson CM, Yamada KA, Saffitz JE (1997) Slow ventricular conduction in mice heterozygous for a connexin43 null mutation. J Clin Invest 99:1991–1998. https://doi.org/10.1172/JCI119367
Heinzel FR, Luo Y, Li X, Boengler K, Buechert A, García-Dorado D, Di Lisa F, Schulz R, Heusch G (2005) Impairment of diazoxide-induced formation of reactive oxygen species and loss of cardioprotection in connexin 43 deficient mice. Circ Res 97:583–586. https://doi.org/10.1161/01.RES.0000181171.65293.65
Jin C, Wu J, Watanabe M, Okada T, Iesaki T (2012) Mitochondrial K+ channels are involved in ischemic postconditioning in rat hearts. J Physiol Sci 62:325–332. https://doi.org/10.1007/s12576-012-0206-y
Kawakami M, Okabe E (1998) Superoxide anion radical-triggered Ca2+ release from cardiac sarcoplasmic reticulum through ryanodine receptor Ca2+ channel. Mol Pharmacol 53:497–503. https://doi.org/10.1124/mol.53.3.497
Kim JC, Pérez-Hernández M, Alvarado FJ, Maurya SR, Montnach J, Yin Y, Zhang M, Lin X, Vasquez C, Heguy A, Liang FX, Woo SH, Morley GE, Rothenberg E, Lundby A, Valdivia HH, Cerrone M, Delmar M (2019) Disruption of Ca2+i homeostasis and connexin 43 hemichannel function in the right ventricle precedes overt arrhythmogenic cardiomyopathy in plakophilin-2-deficient mice. Circulation 140:1015–1030. https://doi.org/10.1161/CIRCULATIONAHA.119.039710
Liao Y, Day KH, Damon DN, Duling BR (2001) Endothelial cell-specific knockout of connexin 43 causes hypotension and bradycardia in mice. Proc Natl Acad Sci USA 98:9989–9994. https://doi.org/10.1073/pnas.171305298
Lu G, Haider HKh, Porollo A, Ashraf M (2010) Mitochondria-specific transgenic overexpression of connexin-43 simulates preconditioning-induced cytoprotection of stem cells. Cardiovasc Res 88:277–286. https://doi.org/10.1093/cvr/cvq293
Matejíková J, Kucharská J, Pintérová M, Pancza D, Ravingerová T (2009) Protection against ischemia-induced ventricular arrhythmias and myocardial dysfunction conferred by preconditioning in the rat heart: involvement of mitochondrial KATP channels and reactive oxygen species. Physiol Res 58:9–19. https://doi.org/10.33549/physiolres.931317
Miro-Casas E, Ruiz-Meana M, Agullo E, Stahlhofen S, Rodríguez-Sinovas A, Cabestrero A, Jorge I, Torre I, Vazquez J, Boengler K, Schulz R, Heusch G, Garcia-Dorado D (2009) Connexin43 in cardiomyocyte mitochondria contributes to mitochondrial potassium uptake. Cardiovasc Res 83:747–756. https://doi.org/10.1093/cvr/cvp157
Miura M, Wakayama Y, Endoh H, Nakano M, Sugai Y, Hirose M, ter Keurs HEDJ, Shimokawa H (2008) Spatial non-uniformity of excitation-contraction coupling can enhance arrhythmogenic delayed afterdepolarizations in rat cardiac muscle. Cardiovasc Res 80:55–61. https://doi.org/10.1093/cvr/cvn162
Miura M, Nagano T, Murai N, Taguchi Y, Handoh T, Satoh M, Miyata S, Miller L, Shindoh C, Stuyvers BD (2016) Effect of carbenoxolone on arrhythmogenesis in rat ventricular muscle. Circ J 80:76–84. https://doi.org/10.1253/circj.CJ-15-0401
Miura M, Taguchi Y, Handoh T, Hasegawa T, Takahashi Y, Morita N, Matsumoto A, Sato H, Shindoh C (2018) Regional increase in ROS within stretched region exacerbates arrhythmias in rat trabeculae with nonuniform contraction. Pflügers Arch 470:1349–1357. https://doi.org/10.1007/s00424-018-2152-x
Miura M, Hasegawa T, Matsumoto A, Nishiyama M, Someya Y, Satoh W, Kumasaka K, Shindoh C, Sato H (2021) Effect of transient elevation of glucose on contractile properties in non-diabetic rat cardiac muscle. Heart Vessels 36:568–576. https://doi.org/10.1007/s00380-020-01726-6
Monma Y, Shindo T, Eguchi K, Kurosawa R, Kagaya Y, Ikumi Y, Ichijo S, Nakata T, Miyata S, Matsumoto A, Sato H, Miura M, Kanai H, Shimokawa H (2021) Low-intensity pulsed ultrasound ameliorates cardiac diastolic dysfunction in mice: a possible novel therapy for heart failure with preserved left ventricular ejection fraction. Cardiovasc Res 117:1325–1338. https://doi.org/10.1093/cvr/cvaa221
Morley GE, Vaidya D, Samie FH, Lo C, Delmar M, Jalife J (1999) Characterization of conduction in the ventricles of normal and heterozygous Cx43 knockout mice using optical mapping. J Cardiovasc Electrophysiol 10:1361–1375. https://doi.org/10.1111/j.1540-8167.1999.tb00192.x
Mykytenko J, Reeves JG, Kin H, Wang NP, Zatta AJ, Jiang R, Guyton RA, Vinten-Johansen J, Zhao ZQ (2008) Persistent beneficial effect of postconditioning against infarct size: role of mitochondrial KATP channels during reperfusion. Basic Res Cardiol 103:472–484. https://doi.org/10.1007/s00395-008-0731-2
Paggio A, Checchetto V, Campo A, Menabò R, Di Marco G, Di Lisa F, Szabo I, Rizzuto R, De Stefani D (2019) Identification of an ATP-sensitive potassium channel in mitochondria. Nature 572:609–613. https://doi.org/10.1038/s41586-019-1498-3
Peng TI, Jou MJ (2010) Oxidative stress caused by mitochondrial calcium overload. Ann N Y Acad Sci 1201:183–188. https://doi.org/10.1111/j.1749-6632.2010.05634.x
Pinz I, Zhu M, Mende U, Ingwall JS (2011) An improved isolation procedure for adult mouse cardiomyocyte. Cell Biochem Biophys 61:93–101. https://doi.org/10.1007/s12013-011-9165-9
Rodriguez-Sinovas A, Boengler K, Cabestrero A, Gres P, Morente M, Ruiz-Meana M, Konietzka I, Miró E, Totzeck A, Heusch G, Schulz R, Garcia-Dorado D (2006) Translocation of connexin 43 to the inner mitochondrial membrane of cardiomyocytes through the heat shock protein 90-dependent TOM pathway and its importance for cardioprotection. Circ Res 99:93–101. https://doi.org/10.1161/01.RES.0000230315.56904.de
Rottlaender D, Boengler K, Wolny M, Michels G, Endres-Becker J, Motloch LJ, Schwaiger A, Buechert A, Schulz R, Heusch G, Hoppe UC (2010) Connexin 43 acts as a cytoprotective mediator of signal transduction by stimulating mitochondrial KATP channels in mouse cardiomyocytes. J Clin Invest 120:1441–1453. https://doi.org/10.1172/JCI40927
Ruiz-Meana M, Rodríguez-Sinovas A, Cabestrero A, Boengler K, Heusch G, Garcia-Dorado D (2008) Mitochondrial connexin43 as a new player in the pathophysiology of myocardial ischaemia-reperfusion injury. Cardiovasc Res 77:325–333. https://doi.org/10.1093/cvr/cvm062
Sáez JC, Schalper KA, Retamal MA, Orellana JA, Shoji KF, Bennett MV (2010) Cell membrane permeabilization via connexin hemichannels in living and dying cells. Exp Cell Res 316:2377–2389. https://doi.org/10.1016/j.yexcr.2010.05.026
Sato H, Nagano T, Satoh W, Kumasaka K, Shindoh C, Miura M (2022) Roles of stretch-activated channels and NADPH oxidase 2 in the induction of twitch contraction by muscle stretching in rat ventricular muscle. Pflügers Arch 474:355–363. https://doi.org/10.1007/s00424-021-02657-5
Schulz R, Görge PM, Görbe A, Ferdinandy P, Lampe PD, Leybaert L (2015) Connexin 43 is an emerging therapeutic target in ischemia/reperfusion injury, cardioprotection and neuroprotection. Pharmacol Ther 153:90–106. https://doi.org/10.1016/j.pharmthera.2015.06.005
Schwanke U, Konietzka I, Duschin A, Li X, Schulz R, Heusch G (2002) No ischemic preconditioning in heterozygous connexin43-deficient mice. Am J Physiol Heart Circ Physiol 283:H1740–H1742. https://doi.org/10.1152/ajpheart.00442.2002
Soetkamp D, Nguyen TT, Menazza S, Hirschhäuser C, Hendgen-Cotta UB, Rassaf T, Schlüter KD, Boengler K, Murphy E, Schulz R (2014) S-nitrosation of mitochondrial connexin 43 regulates mitochondrial function. Basic Res Cardiol 109:433. https://doi.org/10.1007/s00395-014-0433-x
Sovari AA, Rutledge CA, Jeong EM, Dolmatova E, Arasu D, Liu H, Vahdani N, Gu L, Zandieh S, Xiao L, Bonini MG, Duffy HS, Dudley SC Jr (2013) Mitochondria oxidative stress, connexin43 remodeling, and sudden arrhythmic death. Circ Arrhythm Electrophysiol 6:623–631. https://doi.org/10.1161/CIRCEP.112.976787
Sunamura S, Satoh K, Kurosawa R, Ohtsuki T, Kikuchi N, Elias-Al-Mamun M, Shimizu T, Ikeda S, Suzuki K, Satoh T, Omura J, Nogi M, Numano K, Siddique MAH, Miyata S, Miura M, Shimokawa H (2018) Different roles of myocardial ROCK1 and ROCK2 in cardiac dysfunction and postcapillary pulmonary hypertension in mice. Proc Natl Acad Sci USA 115:E7129-7138. https://doi.org/10.1073/pnas.1721298115
Szeto HH (2014) First-in-class cardiolipin-protective compound as a therapeutic agent to restore mitochondrial bioenergetics. Br J Pharmacol 171:2029–2050. https://doi.org/10.1111/bph.12461
Ter Keurs HEDJ, Boyden PA (2007) Calcium and arrhythmogenesis. Physiol Rev 87:457–506. https://doi.org/10.1152/physrev.00011.2006
Van Kempen MJ, Fromaget C, Gros D, Moorman AF, Lamers WH (1991) Spatial distribution of connexin43, the major cardiac gap junction protein, in the developing and adult rat heart. Circ Res 68:1638–1651. https://doi.org/10.1161/01.res.68.6.1638
Thimm J, Mechler A, Lin H, Rhee S, Lal R (2005) Calcium-dependent open/closed conformations and interfacial energy maps of reconstituted hemichannels. J Biol Chem 280:10646–10654. https://doi.org/10.1074/jbc.M412749200
Wagner S, Ruff HM, Weber SL, Bellmann S, Sowa T, Schulte T, Anderson ME, Grandi E, Bers DM, Backs J, Belardinelli L, Maier LS (2011) Reactive oxygen species-activated Ca/calmodulin kinase IIδ is required for late INa augmentation leading to cellular Na and Ca overload. Circ Res 108:555–565. https://doi.org/10.1161/CIRCRESAHA.110.221911
Zhang YM, Miura M, ter Keurs HEDJ (1996) Triggered propagated contractions in rat cardiac trabeculae. Inhibition by octanol and heptanol. Circ Res 79:1077–1085. https://doi.org/10.1161/01.res.79.6.1077
Zima AV, Blatter LA (2006) Redox regulation of cardiac calcium channels and transporters. Cardiovasc Res 71:310–321. https://doi.org/10.1016/j.cardiores.2006.02.019
Funding
This work was supported by Grant-in-Aid for Scientific Research (C) from Japan Society for the Promotion of Science (H. Sato, No. 19K17548; M. Miura, No. 19K07298, No 22K06839).
Author information
Authors and Affiliations
Contributions
MM and HS conceived the idea and designed the animal experiments; MN, NM, WS, TH, YS, TO, and SK conducted animal and laboratory experiments and analyzed the data; MM, CS, and HS interpreted results and experiments; MM and HS prepared figures; MM and HS have drafted the manuscript.
Corresponding author
Ethics declarations
Ethical approval
All animal procedures were approved by the Ethics Review Board of Tohoku University (approval reference number: 2017MdLM0-102, 2020 MdLM0-041).
Consent for publication
All authors have read the manuscript and gave explicit consent to submit. All authors are completely satisfied with its publication.
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Sato, H., Nishiyama, M., Morita, N. et al. Mitochondrial connexin43 and mitochondrial KATP channels modulate triggered arrhythmias in mouse ventricular muscle. Pflugers Arch - Eur J Physiol 475, 477–488 (2023). https://doi.org/10.1007/s00424-023-02789-w
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00424-023-02789-w